Pelvic Exenteration Reconstruction Techniques
*Rivas V Armando
1Department of Surgical Oncology, Central Military Hospital of El Salvador, Central America
Submission: January 10, 2017; Published: January 20, 2017
*Corresponding author: Armando Antonio Rivas Valencia, UNAM Centro Médico Nacional Siglo 21, Department of Surgical Oncology, Central Military Hospital, El Salvador, Central America, Phone: +503 25340649; Email: clinica@cirugiaoncologia.com; www.cirugiaoncologia.com
How to cite this article: Rivas V A. Pelvic Exenteration Reconstruction Techniques. Canc Therapy & Oncol Int J. 2017; 2(5): 555600. DOI:10.19080/CTOIJ.2017.02.555600
Abstract
We are currently using two Surgical Techniques for Pelvic Reconstruction at Central Military Hospital in El Salvador. We achieved excellent results after the completion of Vaginectomy, Radical Hysterectomy and Pelvic Exenteration. These Surgical procedures are: I) Laparoscopic Vaginal Diverticulization of a minimum remaining of vagina for the formation of a neovagina. When a Radical Hysterectomy (Pyver IV type) was performed and the vagina was resected almost completely, we proceed to place a resin marble to pull the vaginal remnant using two thick sterile strings located by laparoscopy at the preperitoneal space using two mini graspers and then the strings are externalized and tied to a device for adjusting the tension of the strings gradually. The progressive traction on the vaginal mucosa remnant gives rise to the formation of a extra peritoneal diverticulum which functions as a neovagina. II) The formation of a new pelvic diaphragm from a defunctionalized segment of sigmoid colon after pelvic exenteration. A segment of sigmoid colon preserving its vascularity is defunctionalized and it is open longitudinally at its antimesenteric border. The intestinal mucosa is removed by hydro dissection and the open segment of sigmoid colon is applied to the pelvic cavity. Thus a viable new pelvic diaphragm is created which has muscle and serous layer. This has reduced substantially the risk of perineal dehiscence.
Keywords: Pelvic reconstruction; Laparoscopic vaginal diverticulization; Reconstruction of pelvic diaphragm
Abbreviations: LVD: Laparoscopic Vaginal Diverticulization; RPD: Reconstruction of Pelvic Diaphragm.
Introduction
Radical surgery in advanced cancers of the pelvis poses great technical difficulties not only in the resection of the tumor but also in the reconstructive process. This type of "salvage surgery" can compromise the quality of life of the patients. This article describes two procedures that reduce reconstructive surgical complications and improve the patient's quality of life.
Laparoscopic Vaginal Diverticulization (LVD)
This technique uses the property of the mucous membrane in which when subjected to constant pressure tends to form a diverticulum. The mucous layer has a good blood supply and can resist pressure without suffering necrosis. It responds adapting to the pressure and grows forming a diverticulum. This can be seen in diverticular colon disease. The colon diverticulum consists only of mucous and serous layers. To remove the vagina completely a perineal approach is performed for the distal sectioning of the vagina which is removed in continuity with the uterus. The mucous tissue is closed at the level of the introitus. 6 to 8 weeks after surgery we perform this procedure to form a neovagina. We use a resin marble of 3 centimeters in diameter with two convergent drillings as shown in (Figure 1).
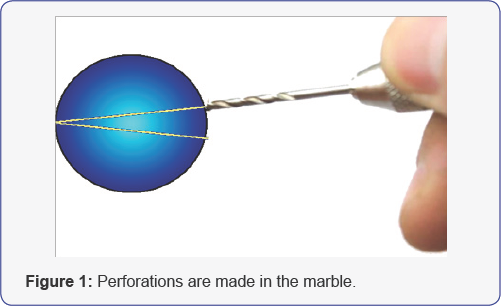
Then a silk thread number 1 is placed. This is to exert traction of the marble to form the diverticulum of the vaginal mucous tissue (Figure 2). The procedure is completely laparoscopic. The camera is placed through the umbilicus and two mini graspers are introduced on both sides [1]. Under laparoscopic view the silk thread that holds the marble is inserted through the vaginal remnant with a needle. The silk thread is entered into the abdominal cavity. Care must be taken not to injure the bladder or the rectum. Once the silk thread endings are within the abdominal cavity the needle is removed.

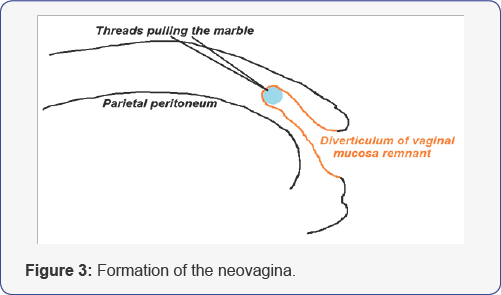
The two mini graspers that have been introduced laterally are reinserted into the preperitoneal space to the point where the silk threads of the marble were introduced. Pulling the end of each silk thread with the mini grasper the threads are extracted through the preperitoneal space until they are exteriorized through the lateral incisions.. The ends of the silk threads are attached to a plastic structure that permits to increase the tension gradually. The tension of the silk threads is increased every day generating the formation of the extra peritoneal vaginal diverticulum (Figure 3). Thus a neovagina is generated without using other tissue of the patient. The result is very aesthetic and functional. A vaginal dilator is used to finish the process of vaginal diverticulization.
Reconstruction of pelvic diaphragm (RPD)
This surgical technique reduces the risk of perineal evisceration after pelvic exenteration in which most of the pelvic diaphragm has been removed. It is also used when there is a large defect in the pelvic diaphragm that may cause a pelvic floor hernia. We have used this procedure in cases of advanced prostate, bladder, rectum or uterine cancers. Normally we perform pelvic exenteration in highly selected patients who have a persistent tumor after radical radiotherapy and chemotherapy. The tumor should have less than 10 cm diameter and should not be fixed to the pelvic walls. Patients are explained of the consequences of this procedure and undergo psychological evaluation to determine if they are suitable candidates for this type of surgery.
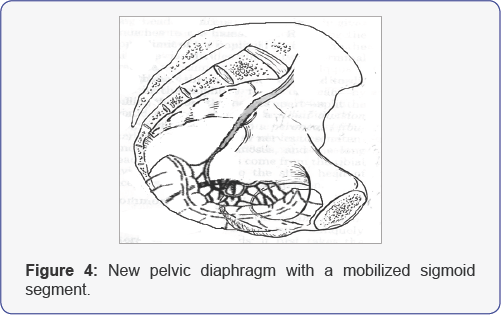
After performing the pelvic exenteration a segment of sigmoid colon is mobilized preserving its irrigation with the marginal vessels and the upper hemorrhoidal vessels [2-4]. The mobilized sigmoid segment is opened longitudinally along its antimesenteric border. Then using hydro dissection the entire mucosa is removed. The denuded mucosa surface is placed down and fixed to the pelvic walls so that a new pelvic diaphragm is formed containing muscular and serosal layers. The muscular layer supports the visceral contents of the pelvic cavity (Figure 4). This reduces the risk of perineal dehiscence.
Conclusion
Radical surgical procedures such as Pyver IV hysterectomy, vaginectomy and pelvic exenteration are considered "salvage surgery" because aesthetics and functionality become secondary priorities. With these procedures the only goal is to save the patient's life. But the development of new reconstructive techniques as the ones described above will help to improve the quality of life of our patients.
References
- FTJ Ferenschild, M Vermaas, C Verhoef, AC Ansink, WJ Kirkels, et al. (2009) Total exenteration for Primary and Recurrent Malignancies. World J Surg 33(7): 1502-1508.
- Orr JW, Shingleton HM, Hatch KD, Taylor PT, Partridge EE, et al. (1983) Gastrointestinal complications associated with exenteration. Am J Obstet Gynecol 145(3): 325-332.
- Lopez MJ, Luna-Perez P (2004) Composite exenteration: Is it worthwhile? Ann Surg Oncol 11(1): 27-33.
- Kecmanovic DM, Pavlov MJ, Kovacevic PA, Sepetkovski AV, Ceranic MS, et al. (2003) Management of advanced pelvic cancer by exenteration. Eur J Surg Oncol 29(9): 743-746.






























