Myocardial Contraction Fraction Performance in Left Ventricular Hypertrophy
Nisha Arenja1* and Sebastian J Buss2,3
1Department of Cardiology, Solothurner Spitäler AG, Switzerland
2Department of Cardiology, Angiology and Pneumology, University of Heidelberg, Germany
3Das Radiologische Zentrum - Radiology Center Sinsheim-Eberbach-Erbach-Walldorf-Heidelberg; Germany
Submission: October 29, 2019; Published: November 08, 2019
*Corresponding author:Nisha Arenja, Department of Cardiology, Solothurner Spitäler AG, Kantonsspital Olten, Baslerstrasse 150, 4600 Olten, Switzerland
How to cite this article:Nisha Arenja, Sebastian J Buss. Myocardial Contraction Fraction Performance in Left Ventricular Hypertrophy. Curr Trends Clin Med Imaging. 2019; 2(5): 555622. DOI: 10.19080/CTCMI.2019.02.555622
Abstract
Left ventricular hypertrophy (LVH) is a frequently diagnosed cardiac condition, which may result from physiological adaptation as well as from chronic pressure overload in various etiologies. Its differentiation has important prognostic implications for the patient. However, in clinical practice the identification of the underlying cause of disease is challenging. Myocardial contraction fraction (MCF) as an easily available parameter has the ability to offer additional diagnostic and prognostic information on LVH. The goal of this mini review is to provide a comprehensive overview of MCF performance in LVH assessed by cardiac magnetic resonance (CMR).
Keywords: Myocardial contraction fraction, Left ventricular hypertrophy, Cardiac magnetic resonance, Cardiac amyloidosis
Intrоductiоn
Left ventricular hypertrophy (LVH) is a common condition and associated with a poor cardiovascular prognosis [1,2]. Various etiologies cause LVH and their differentiation has prognostic implications for the patients. Physiological adaptation to chronic pressure overload in conditions such as aortic stenosis or arterial hypertension (AH) present the most common cause of LVH. In addition, genetically determined hypertrophic cardiomyopathy (HCM) as well as infiltrative myocardial disease, such as cardiac amyloidosis (CA), may also result in apparent LVH. In clinical practice, the non-invasive measurement of LVH assessed by two-dimensional (2D) M-mode echocardiography leads to the diagnosis of LVH. However, the echocardiographic differentiation of the underlying disease is not perennially feasible by echocardiography alone and patients are referred to cardiac magnetic resonance (CMR) for further diagnostic evaluation. CMR is the modality of choice for the quantitative assessment of ventricular mass and myocardial tissue characterization using Late gadolinium enhancement (LGE) images as well as T1 mapping with calculation of extracellular volume (ECV) [3]. Both techniques have been introduced for identification of myocardial fibrosis. Different pattern of fibrosis have been reported according to the underlying etiology [4-6]. However, the assessment of LGE as well as ECV requires the injection of contrast agents, which holds the risk of gadolinium-associated nephrogenic systemic fibrosis in patients with severe renal dysfunction. Especially, patients with CA suffer from renal failure and application of gadolinium-based contrast agents is often limited. Furthermore, tissue characterization may not represent enough information on functional abnormalities in LVH, especially subtle regional or global dysfunction for disease detection. Therefore, additional parameter for characterization of LVH are desirable. The goal of this mini review is to provide a comprehensive overview of myocardial contraction fraction (MCF) diagnostic and prognostic performance in LVH assessed by CMR.
Discussion
Introduction of myocardial contraction fraction (MCF)
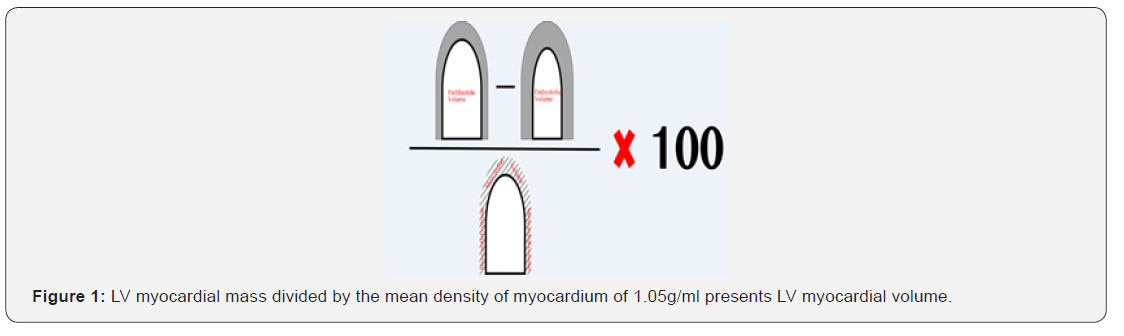
MCF is an easily available quantitative marker, dictated from standard cine CMR images, without the need for contrast agents or specific post-processing software. MCF is a simple imaging parameter, reflecting the relationship between stroke volume (SV) and left ventricle (LV) mass. It is calculated by dividing LV SV (LV enddiastolic volume - LV endsystolic volume) by LV myocardial volume and multiplicated by 100. LV myocardial mass divided by the mean density of myocardium of 1.05g/ml presents LV myocardial volume (Figure 1).
MCF reference values are defined in a large cohort of an age- and gender-matched healthy population [7]. The normal MCF mean values are higher in women (155 ± 18.7 %) than in men (126.6 ± 21.2%). These data consistent with Framingham Heart Study data [8]. Furthermore, the study demonstrated an association of higher MCF values with cardiovascular events.
MCF measured by different modalities
The first description of MCF exists from King et. al. and introduces MCF as a novel marker for investigating myocardial performance in LVH [9]. The estimation of MCF, as a ratio of SV to myocardial volume, is performed by freehand contours and 3D echocardiographic LV reconstruction algorithms. Echocardiography measurements of LV mass by M-mode or 2D echocardiography based on geometric assumptions has been hampered by poor accuracy, especially when compared to CMR as the accepted gold [10]. Major advantage of CMR is accuracy and reproducibility by using 3D approach. Even 3D echocardiography shows only limited performance compared to CMR, suffering from substantial variability and underestimation [11]. CMR is considered the reference standard for LV mass measurements [12,13]. Therefore, MCF derived from CMR images may present a more accurate and reproducible parameter than from 3D echocardiography.
Diagnostic performance of MCF in LVH
In a recent published study, we could demonstrate that MCF has a good diagnostic accuracy to identify LVH and discriminate heart failure patients with CA from patients with other forms of LVH [7]. Therefore, we analyzed CMR images of a heterogenous study population consisted of patients with CA, HCM, hypertensive heart disease (HHD). The diagnostic accuracy of MCF was compared to that of left ventricular ejection fraction (LVEF) and mass index. The results demonstrated a significant reduction of MCF values in LVH. Thereby, MCF performed better than LVEF in discriminating LVH from controls. In addition, MCF outperformed standard functional marker, such as LVEF and LV mass index, in discrimination of LVH etiologies. A cut-off value for MCF < 50% was identified for patients with high probability for CA. Similar to our analysis, a study by King et al presented lower values of MCF in patients with LVH compared with normal subjects [9]. The echocardiographic MCF measurements was performed in a heterogeneous group with various pathologies and controls. The authors concluded that MCF may be useful in assessing differences in myocardial performance in other patients with LVH. In both studies the decrease in MCF indicated an abnormal LV function, although LVEF remained normal even in advanced stages because the progressive reduction in ventricular capacitance. Therefore, measurement of LVEF alone may not give a complete representation of the complex cardiac dysfunction especially in LVH.
Prognostic performance of MCF amyloidosis
After identification of MCF as a discriminator for CA, the prognostic value of MCF was studied in a separate population of systemic immunoglobulin light chain (AL) amyloidosis [14]. Seventy-four subjects with biopsy-proven AL amyloidosis and LGE pattern characteristic for CA were analyzed. The median follow-up was 41 months. The results showed a reduced transplant-free survival and higher rates of death in AL patients with lower MCF values. In addition, the determination of MCF could further risk stratify subjects with AL amyloidosis. Related results were achieved in an additional study by Tendler et al. [15]. The authors proved the prognostic value of MCF in CA in standard 2D echocardiography and concluded the superiority of MCF to LVEF in predicting overall survival among patients with AL amyloidosis. The same method for MCF calculation was utilized by Rubin et al. in 30 subjects with wild-type or mutant ATTR from the THAOS registry. The recent published data could also demonstrate superiority of MCF to LVEF in predicting mortality [16]. These few investigations existing are indicating that MCF is a relevant prognostic marker in CA.
Conclusion
MCF calculated by CMR has a good diagnostic accuracy compared with LV mass and it presents a great prognostic marker in patients with CA. MCF is easily determined from standard cine CMR images, without the need for specific sequences, contrast agents or post-processing software. MCF remains as a routinely available clinical marker with a strong potential. However, further studies of MCF performance are required before it becomes part of clinical routine in the evaluation of LVH.
References
- Levy D, Salomon M, D'Agostino RB, Belanger AJ, Kannel WB (1994) Prognostic implications of baseline electrocardiographic features and their serial changes in subjects with left ventricular hypertrophy. Circulation 90(4): 1786-1793.
- Okin PM, Devereux RB, Jern S, Kjeldsen SE, Julius S, et al. (2004) Regression of electrocardiographic left ventricular hypertrophy during antihypertensive treatment and the prediction of major cardiovascular events. JAMA 292(19): 2343-2349.
- Moon JC, Messroghli DR, Kellman P, Piechnik SK, Robson MD, et al. (2013) Myocardial T1 mapping and extracellular volume quantification: a Society for Cardiovascular Magnetic Resonance (SCMR) and CMR Working Group of the European Society of Cardiology consensus statement. J Cardiovasc Magn Reson 15: 92.
- Maceira AM, Joshi J, Prasad SK, Moon JC, Perugini E, et al. (2005) Cardiovascular magnetic resonance in cardiac amyloidosis. Circulation 111(2): 186-193.
- Mahrholdt H, Wagner A, Judd RM, Sechtem U, Kim RJ (2005) Delayed enhancement cardiovascular magnetic resonance assessment of non-ischaemic cardiomyopathies. Eur Heart J 26(15): 1461-1474.
- Maron MS (2009) The current and emerging role of cardiovascular magnetic resonance imaging in hypertrophic cardiomyopathy. J Cardiovasc Transl Res 2(4): 415-425.
- Arenja N, Fritz T, Andre F, Riffel JH, Aus dem Siepen F, et al. (2017) Myocardial contraction fraction derived from cardiovascular magnetic resonance cine images-reference values and performance in patients with heart failure and left ventricular hypertrophy. Eur Heart J Cardiovasc Imaging 18(12): 1414-1422.
- Chuang ML, Gona P, Salton CJ, Yeon SB, Kissinger KV, et al. (2012) Usefulness of the left ventricular myocardial contraction fraction in healthy men and women to predict cardiovascular morbidity and mortality. Am J Cardiol 109(10): 1454-1458.
- King DL, El-Khoury Coffin L, Maurer MS (2002) Myocardial contraction fraction: a volumetric index of myocardial shortening by freehand three-dimensional echocardiography. J Am Coll Cardiol 40(2): 325-329.
- Armstrong AC, Gidding S, Gjesdal O, Wu C, Bluemke DA, et al. (2012) LV mass assessed by echocardiography and CMR, cardiovascular outcomes, and medical practice. JACC Cardiovasc Imaging 5(8): 837-848.
- Kusunose K, Kwon DH, Motoki H, Flamm SD, Marwick TH (2013) Comparison of three-dimensional echocardiographic findings to those of magnetic resonance imaging for determination of left ventricular mass in patients with ischemic and non-ischemic cardiomyopathy. Am J Cardiol 112(4): 604-611.
- Watzinger N, Maier R, Reiter U, Reiter G, Fuernau G, et al. (2005) Clinical applications of cardiovascular magnetic resonance. Curr Pharm Des 11(4): 457-475.
- Lyne JC, Pennell DJ (2005) Cardiovascular magnetic resonance in the quantitative assessment of left ventricular mass, volumes and contractile function. Coron Artery Dis 16(6): 337-343.
- Arenja N, Andre F, Riffel JH, Siepen FAD, Hegenbart U, et al. (2019) Prognostic value of novel imaging parameters derived from standard cardiovascular magnetic resonance in high risk patients with systemic light chain amyloidosis. J Cardiovasc Magn Reson 21(1): 53.
- Tendler A, Helmke S, Teruya S, Alvarez J, Maurer MS (2015) The myocardial contraction fraction is superior to ejection fraction in predicting survival in patients with AL cardiac amyloidosis. Amyloid 22(1): 61-66.
- Rubin J, Steidley DE, Carlsson M, Ong ML, Maurer MS (2018) Myocardial Contraction Fraction by M-Mode Echocardiography is Superior to Ejection Fraction in Predicting Mortality in Transthyretin Amyloidosis. J Card Fail 24(8): 504-511.






























