Congenital Primary Right Lung Agenesis in A Child – MDCT Imaging Features
M Krishna Kumar1*, H Kalyana2 and S Yogaraj3
1Professor & HOD Department of Radiodiagnosis, Velammal Medical College & Research Institute, Anuppanadi, velammal village, Tuticorin ring road, Tamilnadu, India
2Senior Resident, Department of Radiodiagnosis, Velammal Medical College & Research Institute, Tamilnadu, India
3Department of Radiology, Rehman Medical Institute, Pakistan
Submission: September 4, 2019; Published: September 13, 2019
*Corresponding author: M Krishna Kumar, Professor & HOD Department of Radiodiagnosis, Velammal Medical College & Research Institute, Anuppanadi, velammal village, Tuticorin ring road, Tamilnadu, India
How to cite this article: M Krishna Kumar, H Kalyana, S Yogaraj. Congenital Primary Right Lung Agenesis in A Child – MDCT Imaging Features. Curr Trends Clin Med Imaging. 2019; 2(5): 555619. DOI: 10.19080/CTCMI.2019.02.555619
Summary
Pulmonary agenesis is a very uncommon congenital abnormality that represents the unsuccessful growth of the primitive lung bud. The cause may be a primary embryogenic defect or secondary to situations that restrict fetal lung growth. In the great majority of the cases, the diagnosis is usually made at or soon after birth, but some cases go unnoticed up to adulthood. It is generally associated with other congenital defects and must be suspected in the presence of a total radio-opaque hemithorax. In this article, we present a case of 8 years old female child with congenital pulmonary Agenesis who remained asymptomatic until childhood.
Keywords: Congenital Primary Pulmonary Agenesis, Pulmonary Hypoplasia, Pulmonary Aplasia, Pulmonary Artery Agenesis
Intrоductiоn
Lung agenesis is a rare developmental anomaly which affects both lungs. Long term survival with unilateral lung agenesis is possible in the absence of associated severe anomalies. However, the condition is frequently associated with other congenital abnormalities, particularly esophageal atresia and the VACTERL syndrome (vertebral, anal, cardiac, tracheo-esophageal, renal and radial and limb anomalies) [1]. The prevelance of this condition has been noted to be 0.0034 - 0.0097%. There appears to be no sexual predilection for this condition. Most cases present in the neonatal period with cyanosis, tachypnea, dyspnea, stridor or feeding difficulties. The condition is often associated with fetal distress at birth. Yet, it may also be asymptomatic and manifest itself in adulthood. The cause may be a primary embryogenic defect or secondary to situations that restrict fetal lung growth [2]. Left-sided agenesis (70% of cases) is more frequent than right-sided. Right-sided defects have a poorer prognosis due to often coexisting cardiac anomalies or greater mediastinal shift and pressure on other structures [3]. We herewith report an 8 years old female child with right congenital Primary Pulmonary Agenesis and describe the MDCT imaging features.
CaseReport
An 8 years old female child presented with complaints of dyspnea and left chest pain to the hospital for further investigations. General physical examination was non-contributory. Chest examination revealed absent air entry on right side, mediastinal shift to right side with hyper-resonance on left side. Cardiac examination revealed apex beat palpable in the right 4th intercostal space. Clinical examination of the abdomen revealed no abnormalities.
i. Routine biochemical and arterial blood gas analyses were unremarkable. Electrocardiographic assessment demonstrated a normal sinus rhythm pattern.
ii. The patient also had a cardiology consult to rule out any vascular, cardiac anomalies or effect of the agenesis on cardiac function.
iii. Echocardiography was suggestive of dextroposed heart with normal intracardiac connections.
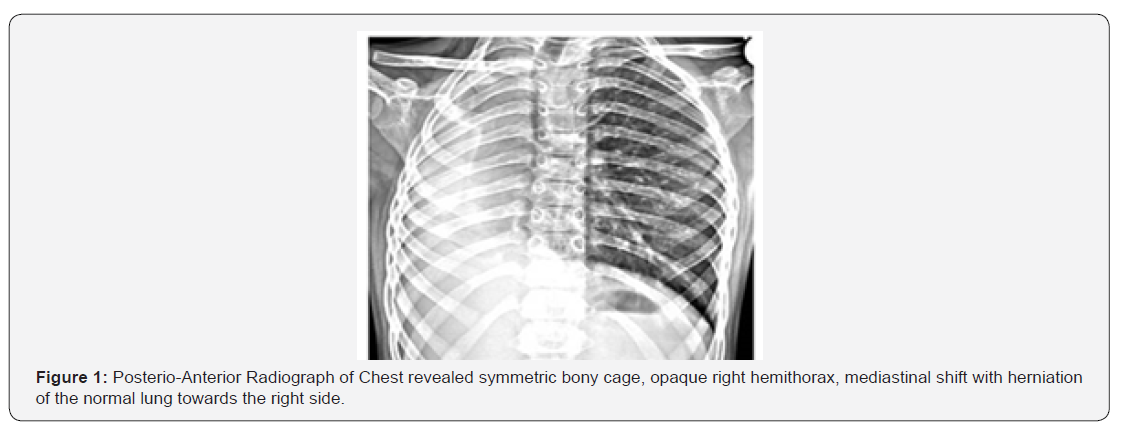
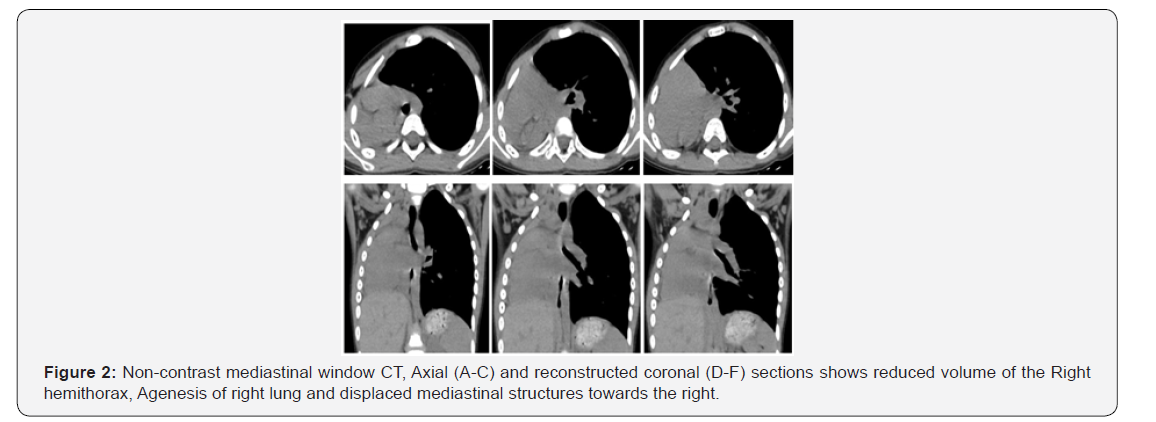
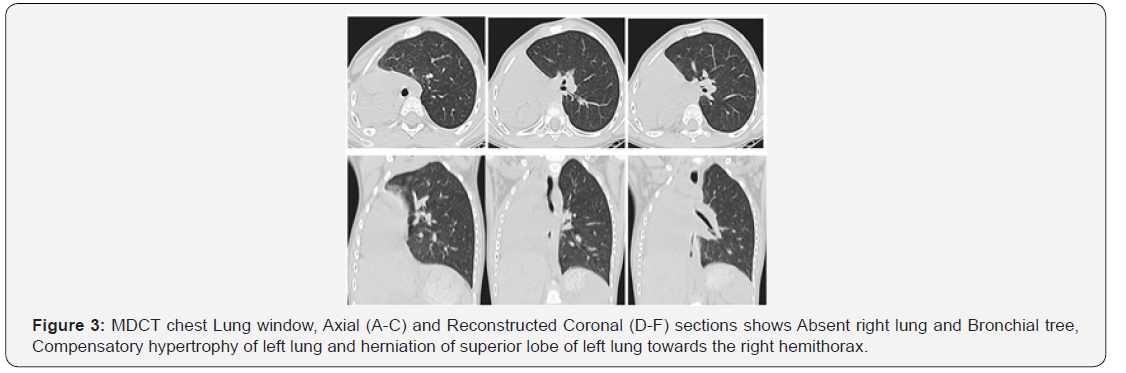
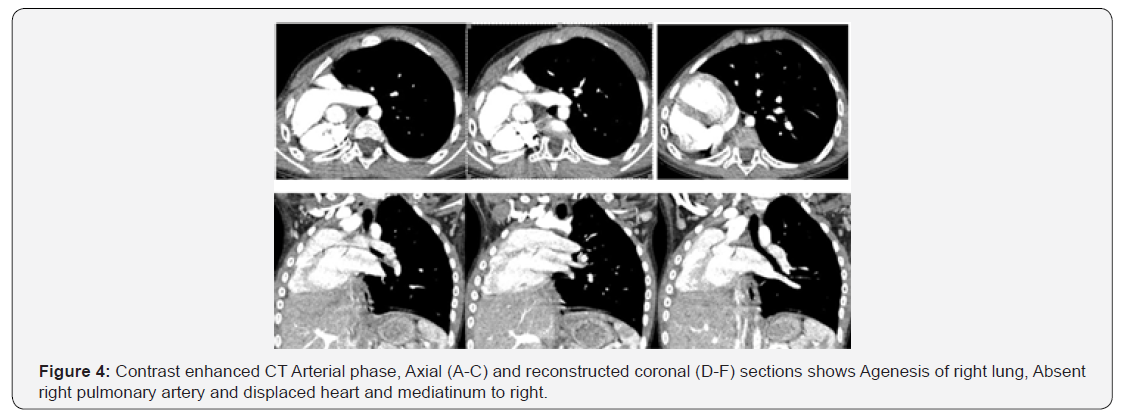
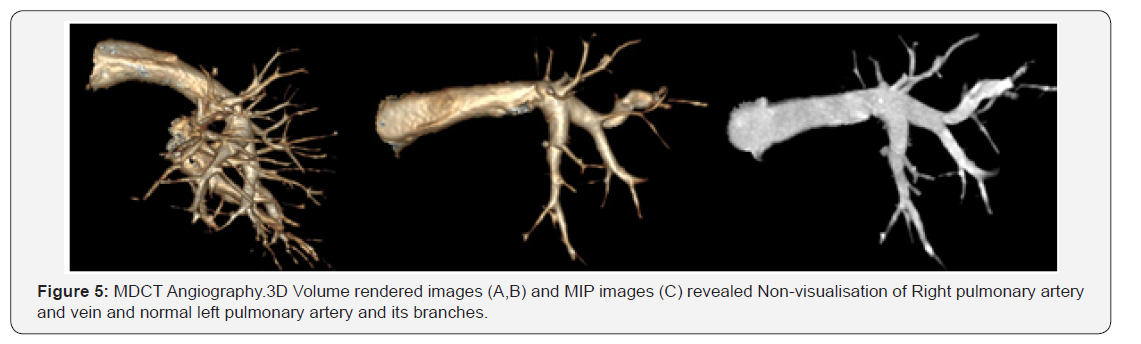
Radiograph of chest revealed symmetric bony cage, opaque right hemithorax, mediastinal shift with herniation of the normal lung towards the right side (Figure 1). Ultrasonography done revealed absence of right lung tissue and shifting of heart towards the affected side. To exclude the diagnosis of a pulmonary thrombo-embolic event, the patient underwent further evaluation with contrast-enhanced MDCT scanning (General Electric (GE) Light Speed Multi Slice CT Scanner) of the thorax with dynamic bolus injection of contrast (100 ml Omnipaque 350 mg/mL, 4.5 mL/s). Multidetector Computed Tomography (MDCT) scan revealed that the volume of the right hemithorax was reduced, Agenesis of right lung and bronchial tree with the mediastinal structures displaced towards the right .There was compensatory hypertrophy of left lung, while the superior lobe of the left lung was partially displaced towards the right hemithorax (Figures 2-4). MDCT Angiography revealed complete agenesis of right lung with non-visualization of right pulmonary artery and vein (Figure 5). On Bronchoscopy the patient had agenesis of the Right bronchial tree and no endobronchial lesions of left lung. Based on these findings a diagnosis of Congenital Primary Right Lung Agenesis was made.
Discussion
Pulmonary Agenesis is a rare congenital anomaly characterized by complete absence of the bronchus, lung parenchyma, and pulmonary vasculature on that side. Unilateral lung agenesis has a birth prevalence of approximately 1 in 15,000 [4]. Normally the lung develops as a diverticulm from foregut in the 4th week of intrauterine life. Pulmonary agenesis results due to failure of the bronchial analogue to divide equally between the two lung buds, leading to normal development of one side, while failure of other side to develop either completely (agenesis/ aplasia) or partially (dysplasia or hypoplasia) [5].
Genetic, teratogenic and mechanical factors have been implicated in the etiology of pulmonary agenesis [6,7]. A history of recurrent chest infections during the first year of life is the usual history elicited; however, the patient may be completely asymptomatic and diagnosed accidentally from the radiograph or detected during autopsy [8]. Associated congenital malformations of the cardiovascular, skeletal, gastrointestinal, or genitourinary systems are present in half of the cases and may modify clinical presentation, course and outcome of patients with pulmonary agenesis [9]. Schneider classified pulmonary agenesis into three groups, which were later modified by Boyden in 1955 [8].
Type 1 (Agenesis) - There is a complete absence of lung and bronchus and there is no vascular supply to the affected side.
Type 2 (Aplasia) - There is a rudimentary bronchus with the complete absence of pulmonary parenchyma.
Group I: No bifurcation of trachea;
Group II: Only rudimentary main bronchus;
Group III: Incomplete development after division of main bronchus; and
Group IV: Incomplete development of subsegmental bronchi and small segment of the corresponding lobe.
Functionally, unilateral lung agenesis and lung aplasia are similar. Pathologically sole lung is larger than normal in pulmonary agenesis, and this enlargement is true hypertrophy and not emphysema [11]. Patients presenting late usually have readily detectable flattening and reduced movement of the chest wall on the affected side, with reduced air entry on auscultation. Breath sounds from the herniated, hypertrophied lungs may be heard on the side of agenesis except in the axilla and base Chest wall deformity can be quite pronounced, with an associated secondary scoliosis [11]. Diagnosis of Pulmonary Agenesis has been made on chest skiagram, bronchoscopy, bronchography and angiography. With the advent of CT scan, these invasive procedures which entail significant risk have become unnecessary [12].
As might be expected, Chest radiographs in patients with unilateral absence of a lung show loss of aeration and marked volume loss on the affected side. Volume loss is shown as elevation of the ipsilateral hemidiaphragm, shift of the mediastinum toward the abnormal side, and anterior herniation of the contralateral lung. There is usually characteristic wedge-shaped opacity in the inferior and lateral aspect of the affected hemithorax. This opacity is due to herniation of heart and mediastinum into the lower thorax and proliferation of fat to partially compensate for the absence of lung tissue. The obvious Differential diagnoses are acquired total lung collapse or prior pneumonectomy [13]. Other conditions to consider in the differential include hyperlucent and hypoplastic lung syndromes, obstructive lung lesions mainly cancer, diaphragmatic hernia, adenomatoid cystic malformations and sequestrations and the Scimitar syndrome [14]. Pulmonary Angiography shows absence of ipsilateral pulmonary artery. Bronchoscopy demonstrates underdeveloped bronchus in agenesis. Other investigations e.g. echocardiogram, ultrasound abdomen etc. are required depending upon the presence of associated congenital abnormality [15]. The MDCT allows high‑resolution isotropic imaging and is the ideal modality for diagnosing right lung agenesis and for diagnosing simultaneously any associated tracheobronchial anomaly. MDCT can very speedily acquire volumetric data sets, allowing for 2D, multiplanar, maximum intensity projection and volume rendering technique reconstructions, and has the capability to image both airway and vascular abnormalities. The characteristic MDCT findings include opaque hemithorax, Agenesis of lung with mediastinal shift towards the affected side and bony cage symmetry (Figures 2-4). Similar findings were seen in our case and a diagnosis of primary right lung Agenesis was made. However, no etiological diagnosis could be confirmed as genetic mutation analysis was not affordable in our case.
No treatment is required in asymptomatic cases. Treatment is necessary for chest infections. Patients having stumps (hypoplastic bud) may require surgical removal if postural drainage and antibiotics fail to resolve the infection. Corrective surgery of associated congenital anomalies, wherever feasible, may be undertaken [16]. Several methods have been proposed to reduce vascular compression and intrinsic stenosis such as mediastinal stabilization by an expansion prosthesis, aortopexy, aortic grafting and resection, detour of the left pulmonary artery and slide tracheoplasty [4]. Overall, prognosis depends on two factors. Firstly, the severity of associated congenital anomalies and secondly, involvement of the normal lung in any disease process. While bilateral Pulmonary agenesis is incompatible with life, 50% of those with even unilateral lung agenesis die within 5 years of life [17]. Right lung Agenesis carries a poorer prognosis because of the larger shift of the heart and mediastinum with a consequent distortion of the great vessels, especially aortic arch resulting in extrinsic compression over the trachea anteriorly [18,19]. In our case the child is surviving beyond 5 years of life.
Conclusion
Pulmonary Agenesis is an uncommon pathology. Clinical findings of recurrent respiratory infections and radiologic evidence of opaque hemithorax, bony symmetry and herination of normal lung to the affected side, along with associated congenital anomalies are suggestive of Pulmonary Agenesis. No treatment is required in asymptomatic cases. Management is mainly supportive, correcting associated malformations, prevention and treatment of repeated respiratory tract infections. MDCT imaging not only guides us to a proper diagnosis but also can identify the etiology, level of airway narrowing and associated congenital anomalies , thus helping in proper patient care.
References
- BS Clements (2008) Congenital malformations of lungs and airways.in. LM Taussig, LI Landau (Ed.), Paediatric respiratory medicine, 2 (Philadelphia: Laura De Young,) pp1108-1110.
- Mardini MK, & Nyhan WL (1985) Agenesis of the lung: report of four patients with unusual anomalies. Chest 87: 522–527.
- Fokstuen Siv, Schinzel Albert (2000) Unilateral lobar pulmonary agenesis in sibs. J Med Genet 37: 557-559.
- Chou AK, Huang SC, Chen SJ, Huang PM, Wang JK, et al. (2007) Unilateral lung agenesis – Detrimental roles of surrounding vessels. Pediatr Pulmonol 42: 242‑24
- Skandalakis JE, GraySW, Symbas P (1994) The trachea and the lungs: Embryology for Surgeons. (2nd ), Williams and Wilkins, Baltimore, MD, USA.
- Say B, Carpenter NJ, Giacoia G, Jegathesan S (1980) Agenesis of the lung associated with a chromosome abnormality (46, XX,2p+). J Med Genet 17: 477-478.
- Roque AS, Burton EM, Boedy RF, Falls G, Bhatia JS (1997) Unilateral pulmonary agenesis without mediastinal displacement. South Med J 90: 335-337.
- Kisku KH, Panigrahi MK, Sudhakar R, Nagarajan A, Ravikumar R, et al. (2008) Agenesis of lung - a report of two cases. Lung India 25: 28-30.
- Razaque MA, Singh S, Singh T (1980) Pulmonary agenesis. Indian J Chest Dis Allied Sci 22: 174-178.
- Unilateral pulmonary hypoplasia-a case report. (2007) Lung India; 24: 69-71.
- TM Krummel, Congenital malformations of the lower respiratory tract. E.L.Kendig(Ed.), Kendig’s Disorders of The Respiratory Tract in Children. 6(Philadelphia: WB Saunders Company, 1998) 307-308.
- Bhagat R, Panchal N, Shah A (1992) Pulmonary Aplasia: A CT appearance. Ind Pediatr 29:1410-1412.
- DM Hansel, DA Lynch, HP Mc Adams, AA Bankier (2010) Imaging of diseases of the chest. (Mosby, Philadelphia,)1073.
- Berrocal Teresa, Madrid Carmen, Novo Susana, Gutieurez Julia, Arjonilla Antonia, et al. (2003) Congenital anomolies of the tracheobronchial tree, lung, and mediastinum: embryology, radiology, and pathology. Radiographics 24: e17.
- ML Gupta, SR Sharma, S Singh, (2011) Congenital anomalies of the respiratory system, Behera D(Ed.), NCCP text book of respiratory medicine (NewDelhi: Jaypee brothers medical publishers,) 870.
- Chopra K, Sethi GR, Kumar A, et al. (1988) Pulmonary agenesis. Indian Pediatr 25: 678-682.
- Krivchenya DU, Rudenko EO, Lysak SV, Dubrovin AG, Khursin VN, et al. (2007) Lung aplasia: anatomy, history, diagnosis and surgical management. Eur J Pediatr Surg 17: 244-250.
- Newman B, Gondor M MR (1997) evaluation of right pulmonary agenesis and vascular airway compression in pediatric patients. AJR Am J Roentgenol 168: 55‑5
- Pierron C, Sigal‑Cinqualbre A, Lambert V, Le Bret E (2011) Left pulmonary artery sling with right lung aplasia. J Pediatr Surg 46: 2190‑219






























