Functional Cancer Staging in Black Africans- An Initial Experience with Whole Body Diffusion MRI
G Asafu Adjaye Frimpong1*, E Aboagye2, KC Gyasi-Sarpong2 and KEK Aboah3
1Spectra Health Imaging and Interventional Radiology Centre, Kumasi-Ghana
2Department of Radiology, Kwame Nkrumah University of Science and Technology, Kumasi-Ghana
3Department of Surgery, Kwame Nkrumah university of Science and Technology, Kumasi-Ghana
Submission: August 24, 2019; Published: September 10, 2019
*Corresponding author: George Asafu Adjaye Frimpong, Spectra Health Imaging and Interventional Radiology Centre, Post Office Box KS 5431, Kumasi-GhanaKrálové 05, Sokolská 585, Czechia
How to cite this article: G Asafu Adjaye Frimpong, E Aboagye, KC Gyasi-Sarpong, KEK Aboah. Functional Cancer Staging in Black Africans- An Initial 0074 Experience with Whole Body Diffusion MRI. Curr Trends Clin Med Imaging. 2019; 2(5): 555618. DOI: 10.19080/CTCMI.2019.02.555618
Summary
Purpose: To report on our initial experience with whole body diffusion weighted MRI for cancer staging in oncological patients of black African origin.
Patients and Methods:
Results:The study involved 34 known oncological patients who were referred for cancer staging with whole body diffusion weighted MRI (WB-DW-MRI) at our center within the period of the study. WB-DW-MRI was performed on a 1.5T clinical scanner recently installed in our center. Scans were performed using 6 Channel body phase array coils together with 16 Channel Head/Neck Coil. Patients were examined in supine position and four stations of axial free breathing diffusion weighted imaging (DWI).
Results: Majority of our study population were males, recording a mean age of 60.2 years. The lesions indicated for WB-DW-MRI included prostate cancer, breast cancer, uterine cancer, gastric cancer, non-Hodgkins lymphoma, Burkitt’s lymphoma, rectal cancer and lung cancer. Prostate cancer was the most common lesion (n=25, 73.5%). Visceral and/or bony metastasis was evident in 12 out of the 34 cases reported, majority of which were prostate cancer cases.
Conclusion: Whole body diffusion weighted MRI has proven to be effective in assessing visceral, nodal and bony metastasis in various types of malignancies in a black African population. Based on this experience, we reinforce the recommendation that WB-DW-MRI should be integrated into routine clinical practice.
Keywords: Whole Body Diffusion, Diffusion Weighted Imaging, MRI, Prostate Cancer, Breast Cancer, Bony and Visceral Metastasis
Intrоductiоn
With the emergence of validated clinical indications for patients with known or suspected malignancy, the demand for imaging in oncology care is increasing. Imaging modalities such as positron emission tomography (PET), computed tomography (CT), magnetic resonance imaging (MRI), bone scintigraphy (BS) and ultrasound are employed in establishing early diagnosis and performing appropriate monitoring of patients with regards to visceral and bony metastasis, common in the brain, liver and lungs [1,2]. Also, in an era where novel surgical and interventional techniques are utilized for the management of cancers, proven imaging techniques are needed for accurate tumor staging and precise evaluation of the metastatic burden in order to plan appropriate therapeutic management of patients with malignancy [3-5].
Bone scintigraphy (BS) and CT scan have been utilized in detection and therapeutic response assessments but are not very effective in evaluating therapeutic response in bone disease, which is the most common disease sites in breast, multiple myeloma and prostate cancer [6]. For instance, BS is limited in the assessment of multiple myeloma when there is an insufficient osteoblastic reaction to the presence of an active disease. Even in the presence of osteoblastic reaction, BS usually provides misleading information when utilized in the assessment of therapeutic effectiveness. Also, increased BS uptake in number and extent of lesions can create confusion between progression and response, in therapy response settings [6]. Whole body imaging tools such as PET-CT and whole-body diffusion weighted MRI (WB-DW-MRI) have thus emerged as a viable alternative assessment tool.
uptake in number and extent of lesions can create confusion between progression and response, in therapy response settings [6]. Whole body imaging tools such as PET-CT and whole-body diffusion weighted MRI (WB-DW-MRI) have thus emerged as a viable alternative assessment tool.
Whole body diffusion weighted MRI (WB-DW-MRI) with its inherent advantages including lack of ionizing radiation, no use of contrast, time saving and relatively lower cost, is a practical technique that may fulfill this role [10,11]. WB-DWMRI, introduced by Takahara et al. [12] is able to suppress background body signal, thus allowing assessment of metastasis of various malignancies without motion artifact, and threedimensional (3D) images can be obtained using reformatting techniques such as maximum-intensity projection (MIP) and multi-planar reformatted (MPR). Furthermore, the apparent diffusion coefficient (ADC) map obtained from diffusion weighted MRI reflects cellular density, tumor morphology, nuclear-tocytoplasm ratio and integrity of cell membrane, regardless of cancer type and location [13,14]. WB-DW-MRI has thus emerged as a powerful tool, capable of evaluating both bone and soft tissue disease, and showing both cell viability and tissue cellularity, thus increasing confidence in the detection, characterization and monitoring of treatment response in metastatic lesion [6]. It has proven to be efficacious for overcoming the limitations of CT and BS for detection and therapeutic response assessments in patients with bone marrow tumors [15] Consequently, WBDW- MRI is progressively proposed by clinicians as an efficient examination for an expanding range of indications [16] In this study, we report on our initial experience with WB-DW-MRI for cancer staging in a black African population, providing additional evidence that whole body diffusion weighted MRI has an important role in the staging of different types of tumors and it is a viable alternative to positron emission tomography computed tomography (PET-CT) for cancer staging.
Methods
Within the period of October 2018 to February 2019, 34 known oncological cases were referred from various health facilities for cancer staging with whole body diffusion weighted MRI scan at our center. Ethical approval for the study was obtained from the Committee on Human Research, Publications and Ethics (CHRPE/AP/306118). Also, written informed consent was obtained from the participants before their inclusion into the study. WB-DW-MRI was performed on a 1.5T clinical scanner (Magnetom Essenza Siemens Healthineers, Erlangen German) recently installed in our center. Scans were performed using 6 Channel body phase array coils together with 16 Channel Head/ Neck Coil.
Patients were examined in supine position and four stations of axial free breathing DWI with Short Tau inversion Recovery (STIR) fat suppression obtained using the scan parameters as follows Echo time (TE) 93ms; Repetition time (TR) 9000 MS; Inversion time (TI) 160 ms, B values 50 and 900 s/mm2, Read out bandwidth 1628 Hz/Pixel, 6 Averages, Field of View (FOV) 400 MM, Slice thickness 5 mm, Image matrix 128x128, Voxel size 1.6x1.6x5.0 mm. Acquisition time per station 7.30 min. The protocol also included four stations of Coronal T2 Fat Sat free breathing with the following parameters: TR 2000 ms; TE 93ms; Image matrix 256x256, Voxel size 1.5x1.5x5mm with SPAIR Fat suppression mode. After the completion of the last acquisition, four stations including Head/Neck, Thorax, Abdomen and Pelvis were then composed inline. No contrast media was administered, and total duration of each examination was about 50 to 55 minutes.
Metastasis Reporting and Data System for Prostate (MET-RADS-P)
Despite the wider applicability of whole-body MRI (WBMRI), especially in assessing bone and soft tissue metastases, its use has been limited by inconsistencies in how the procedure is performed and interpreted. There was therefore the need for a standardized approach that ensures uniformity in acquisition, interpretation and reporting. This led to the formulation of Metastasis Reporting and Data System (MET-RADS-P), which provides the field of WB-MRI with minimum standards of image acquisition, interpretation and reporting [17,18].
MET-RADS-P criteria was employed in assessing bone metastasis in this study. It enables assessment of 14 predefined regions of the body including seven skeletal regions, primary disease, visceral, five nodal and other sites at baseline and follow-up assessment, making use of a 1.5 cm diameter threshold for all measured lesions. Each region was assigned a response assessment on a scale of 1-5 (1, indicating a higher likelihood of a patient responding, up to 5, indicating a higher likelihood of disease progression). In addition, MET-RADS-P utilizes a scoring system that allowed accounting for heterogeneity of responses in different regions. The final response assessment involved assessing the status of the bones, primary disease, viscera and nodes separately [17,18]. In assessing soft tissue metastases, RECIST criteria as described by Eisenhauer et al. [18] was employed.
Results
Thirty-four known oncological patients with a mean age of 60.2 years, underwent whole body diffusion weighted MRI scan at our center within the period of the study. The lesions indicated for WB-DW-MRI included prostate cancer, breast cancer, uterine cancer, gastric cancer, non-Hodgkins lymphoma, Burkitt’s lymphoma, rectal cancer and lung cancer. Prostate cancer was the most common lesion, representing 25 out of the 34 cases. Visceral and/or bony metastasis was evident in 12 out of the 34 cases reported.
Discussion
Whole body diffusion weighted MRI (WB-DW-MRI), which combines anatomical T1 and T2 images with functional information using diffusion sequences, is an attractive modality for tumor detection and oncological staging owing to lack of radiation, high spatial resolution and soft tissue contrast [10,11,19,20]. The utilization of whole body MRI (WB-MRI) has been hindered in the past due to limitations such as limited availability and forbidding acquisition times.16 However, recent technological advancements incorporating multi-channel whole body scanners, has led to high sensitivity in the detection of organ metastases, especially for tumors frequently metastasizing to the bone, liver or the brain [21,22].
In addition, the use of diffusion weighted imaging (DWI) has transformed WB-MRI, providing functional information which enables “at-a-glance” assessment of the whole body, thus improving readers’ performance and reducing interpretation time [20,23] The rationale for the use of WB-DW-MRI in oncology is to enable tumor detection and precise staging, which are crucial for assessing prognosis and planning effective treatment. This study to the best of our knowledge is the first to report on whole body diffusion weighted MRI cancer staging in oncological patients of black African origin. The main focus of the procedure was to find evidence of visceral/and or bony metastasis in already diagnosed tumor cases involving the prostate, gastric, uterine, rectum, lung and breast as well as stage lymphomas.
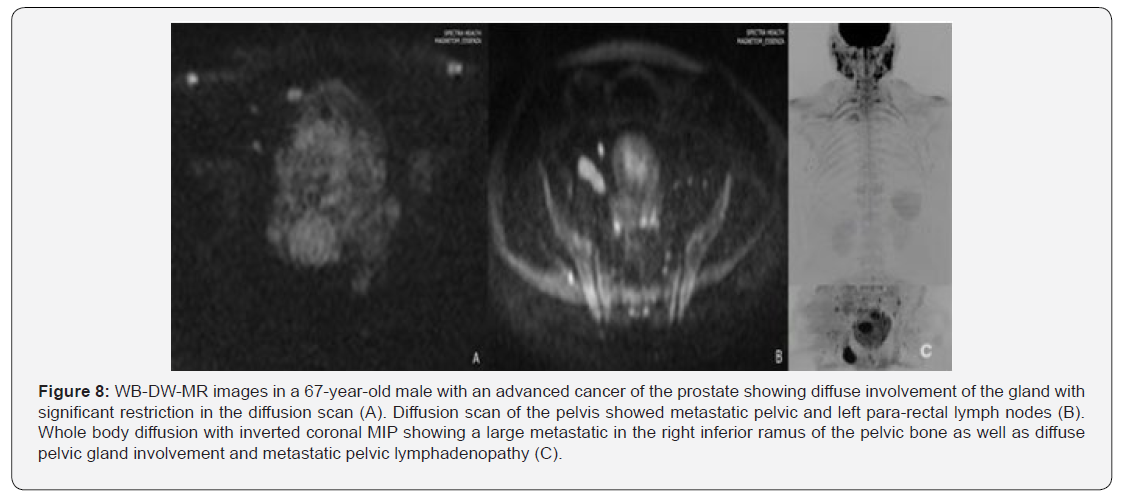
Majority of the cancer staging with WB-DW-MRI in this study involved prostate cancer patients, and metastases was evident in 6 out of the 25 cases (Figures 1-3). In most of these cases of prostate cancer, there was an early spread to bones and regional nodes. A meta-analysis from 27 studies have shown that, on per patient basis, WB-DW-MRI is superior to PET-CT and bone scintigraphy (BS) in the detection and staging of prostate cancer [24] The presence of metastasis in prostate cancer imaging in this study was crucial for the patients, assisting in defining the advanced disease state and the absence or presence of metastasis outside the true pelvis was highly prognostic, thus affecting subsequent therapy choices.

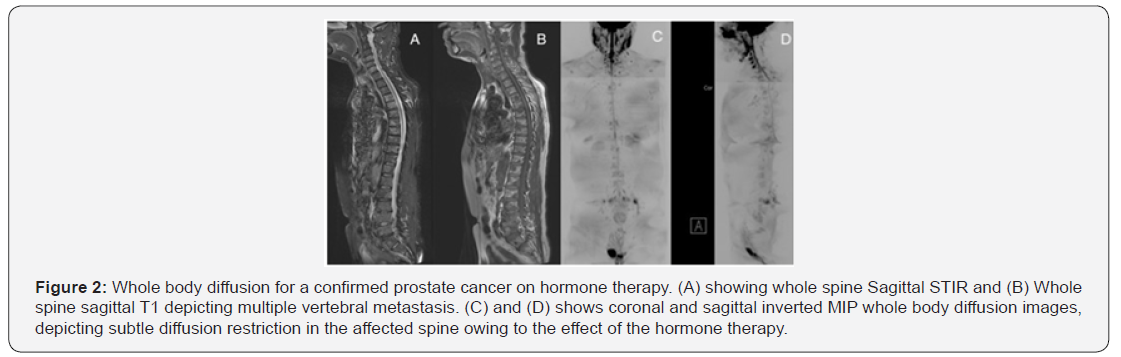
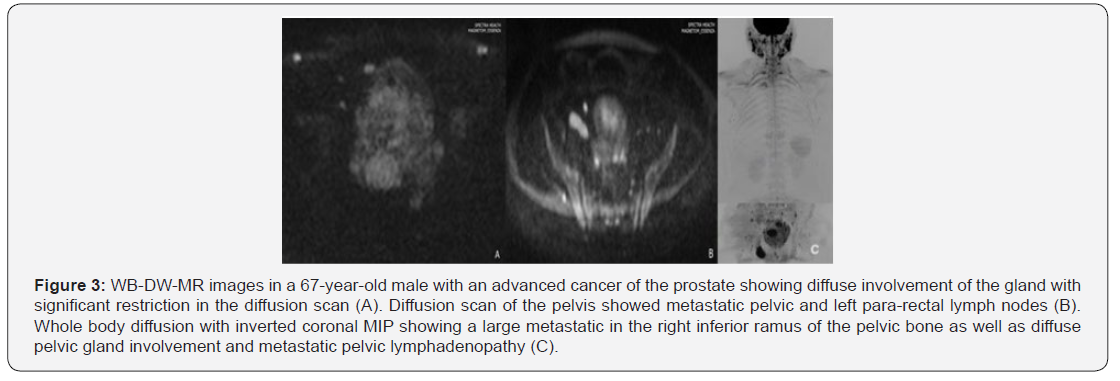
Also, the use of MET-RADS-P reporting template enabled us to characterize the metastatic bone disease response into 5 categories (1 Response: highly likely; 2 Response: likely; 3 stable; 4 progression: likely; 5 progression: highly likely), which was considered helpful compared to the limited clinically groups of progression and no-progression, eventually overcoming the limitations of BS and CT scans. In the reported prostate cancer cases, WB-DW-MRI was successful in establishing metastasis to the pelvic bone, pelvic lymph node and lumbosacral spine as depicted in (Figures 1-3). Extensive metastasis was recorded in the breast cancer cases reported in this study. The bone is recognized as the most common metastatic site in breast cancer cases, with axial and proximal appendicular skeleton been the most affected sites [25] In the current study, WB-DW-MRI for the breast cancer case established metastasis involving the lung, liver and axial skeleton (vertebral, pelvis and ribs) (Figure 4).
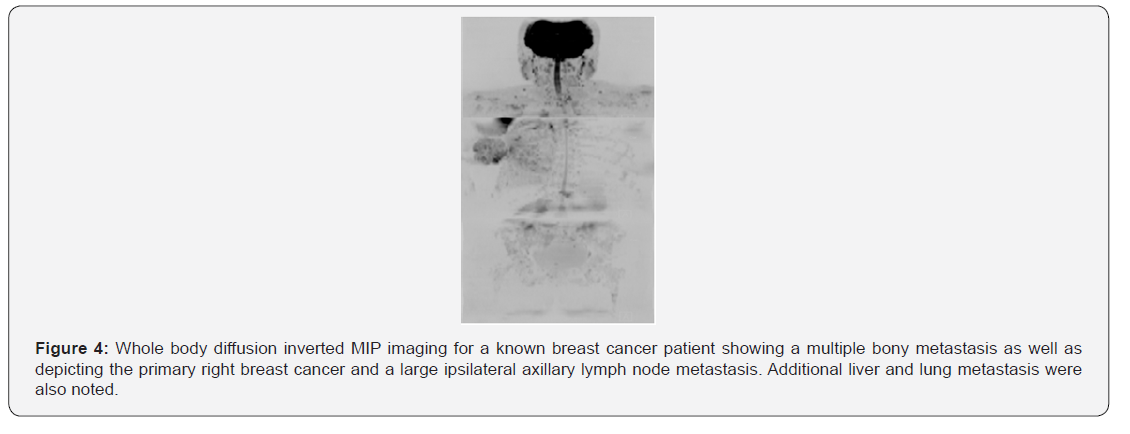
The main focus of performing WB-DW-MRI in this advanced case was to assess clinical response, evaluate post-therapeutic changes and complications, and search for hypercellular lesions for the purpose of disease staging. Moreover, it is essential to establish an early diagnosis and adopt appropriate monitoring strategies in breast cancer cases, as research has shown that about 10% of the patients will have secondary neoplastic involvement of multiple organ Schmidt et al. [26] in their study of breast cancer patients compared the diagnostic accuracy of WB-MRI and PET-CT for the detection of tumor recurrence. WB-MRI was found to be highly sensitive in detecting distant metastatic disease, as confirmed in our study, while PET-CT was more sensitive in detecting lymph node involvement [27].
Also, a meta-analysis conducted by Yang et al. [28] which involved 145 studies in various types of malignancies, including breast cancer, showed that WB-MRI and PET-CT have comparable diagnostic performance, and were found to be superior to CT and BS in terms of specificity and sensitivity to detect bone metastases. The current study demonstrates that WB-DW-MRI showed high specificity and sensitivity in detecting both visceral and bony metastases as depicted in Figure 4, thus serving as a “one-time” approach to staging the advanced case of breast cancer. This was in line with the recommendation by the UK’s National Institute for Health and Care Excellence that the progression of bone metastasis in patients with advanced breast cancer must be evaluated by MRI rather than PET-CT or BS [29].
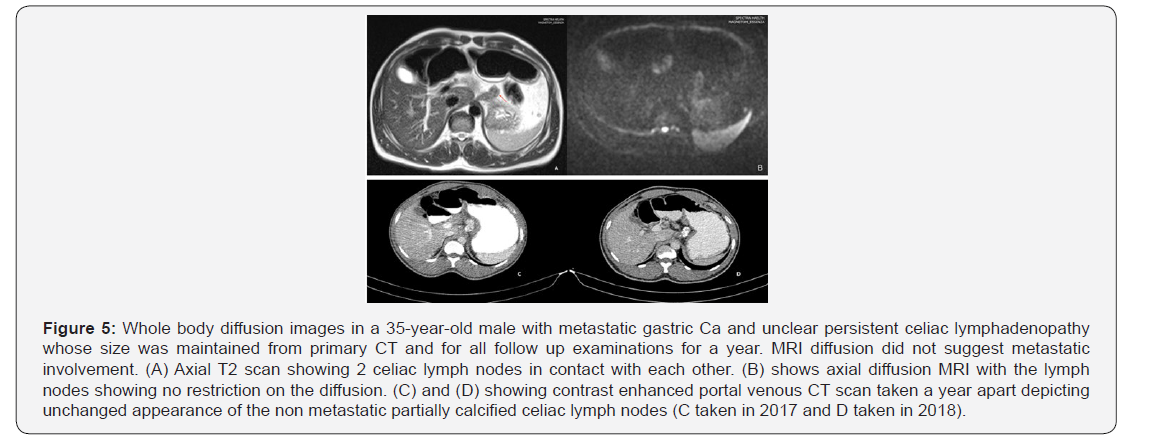
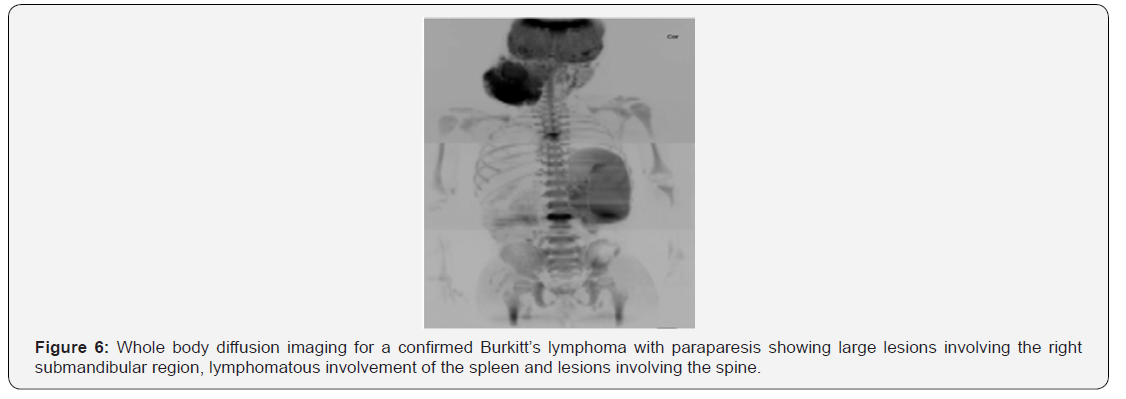
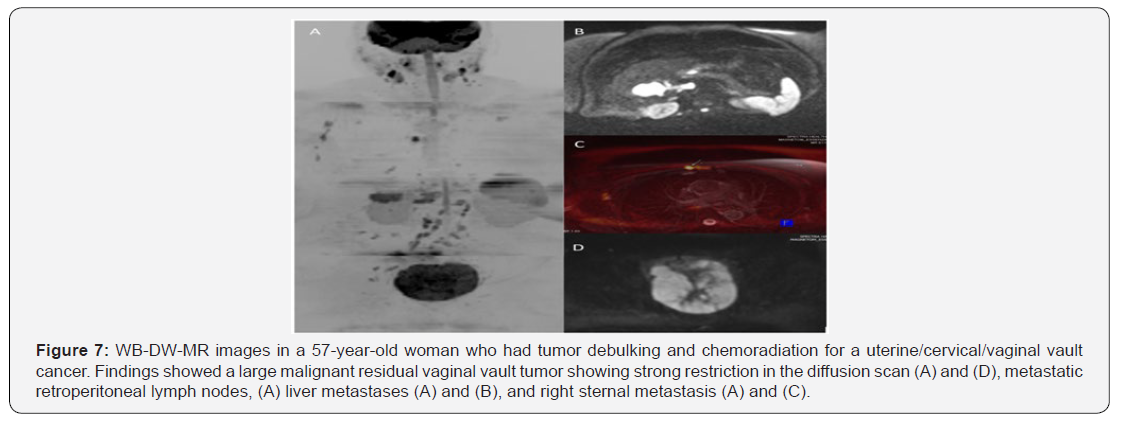
WB-DW-MRI also proved useful in the staging of cases involving gastric cancer (Figure 5), uterine cancer (Figure 5), non-Hodgkin’s lymphoma (Figure 3) and Burkitt’s lymphoma (Figure 6). In all these cases, WB-DW-MRI enabled overall assessment of the disease by providing accurate information on nodal and distant metastasis, thus rendering crucial information for assessing prognosis, risk stratification and planning effective treatment. Worthy of note was the presence of lung metastasis in both gastric cancer (Figure 5) and uterine cancer (Figures 7 & 8) and hepatic metastasis in uterine cancer. This demonstrates the utility of WB-DW-MRI in the detection of secondary visceral involvement, and this may even be detected before they appear in other sequences [2].
In summary, WB-DW-MRI allows more accurate tumor characterization and detection of both visceral and bony metastasis, as evident in the cases presented in this study. Bony metastases as shown in this study are detectable in patients with advanced stages of prostate, breast and uterine tumors. WBMRI with diffusion imaging provide clear categorization of the treatment response of bone metastases due to the calculation of the ADC value, as against BS and PET/CT which are able to identify only disease progression [30,31]. Various studies have thus demonstrated its superiority to BS for the detection of bone metastasis and was better than PET-CT on a per-patient basis [24,32]. However, several studies comparing the diagnostic accuracy of WB-DW-MRI and PET-CT have reported no significant difference, with some concluding that they are complementary techniques [24,28,33]. Moreover, in the performance of WBDW- MRI, one needs to be aware of inherent pitfalls such as false negatives in the presence of cystic metastasis, tumor necrosis and imaging areas close to the heart [33].
Conclusion
Whole body diffusion weighted MRI is a proven technology in cancer staging. It is currently the preferred imaging modality for multiple myeloma and bony metastasis, and it compares very well with PET-CT for all other indications. In breast and prostate cancer cases, which constituted majority of the reported cases in this study, WB-DW-MRI proved useful in assessing visceral, nodal and bony metastasis. Based on our experience with WBDW- MRI for cancer staging in a black African population, we reinforce the recommendation that it should be integrated into routine clinical practice.
References
- Glimelius B, Oliveira J (2009) ESMO Guidelines Working Group Rectal cancer: ESMO clinical recommendations for diagnosis, treatment and follow-up. Ann of Oncol 20(suppl_4): iv54-iv56.
- Godinho MV, Lopes FP, Costa FM (2018) Whole-body magnetic resonance imaging for the assessment of metastatic breast cancer. Cancer Manag Res 10: 6743-6756.
- O’shaughnessy J, Miles D, Vukelja S, Moiseyenko, V, Ayoub, et al. (2002) Superior survival with capecitabine plus docetaxel combination therapy in anthracycline-pretreated patients with advanced breast cancer: phase III trial results. J Clin Oncol. 20(12): 2812-2823.
- Vlastos G, Smith DL, Singletary SE, Mirza NQ, Tuttle TM, et al. (2004) Long-term survival after an aggressive surgical approach in patients with breast cancer hepatic metastases. Annals of Surgical Oncology 11(9): 869-874.
- Mack MG, Straub R, Eichler K, Söllner O, Lehnert T, et al. (2004) Breast cancer metastases in liver: laser-induced interstitial thermotherapy—local tumor control rate and survival data. Radiology 233(2): 400-409.
- Petralia G, Padhani AR (2018) Whole-Body Magnetic Resonance Imaging in Oncology: Uses and Indications. Magn Reson Imaging Clin 26(4): 495-507.
- Sironi S, Buda A, Picchio M, Perego P, Moreni R, et.al. (2006) Lymph node metastasis in patients with clinical early-stage cervical cancer: detection with integrated FDG PET/CT. Radiology 238(1): 272-299.
- Cheson BD, Fisher RI, Barrington SF, Cavalli F, Schwartz LH, et al. (2014) Recommendations for initial evaluation, staging, and response assessment of Hodgkin and non-Hodgkin lymphoma: the Lugano classification. J Clin Oncol 32(27): 3059-3068.
- Branstetter IV BF, Blodgett TM, Zimmer LA, Snyderman CH, Johnson JT, et al. (2005) Head and neck malignancy: is PET/CT more accurate than PET or CT alone? Radiology 235(2): 580-586.
- Cai W, Kassarjian A, Bredella MA, Harris GJ, Yoshida H, et al. (2009) Tumor burden in patients with neurofibromatosis types 1 and 2 and schwannomatosis: determination on whole-body MR images. Radiology 250(3): 665-673.
- Darge K, Jaramillo D, Siegel MJ (2008) Whole-body MRI in children: current status and future applications. Eur J Radiol. 68(2): 289-298.
- Takahara T, Imai Y, Yamashita T, Yasuda S, Nasu S, et al. (2004) Diffusion weighted whole body imaging with background body signal suppression (DWIBS): technical improvement using free breathing, STIR and high-resolution 3D display. Matrix 160(160): 160.
- Castillo M, Smith JK, Kwock L, Wilber K et al. (2001) Apparent diffusion coefficients in the evaluation of high-grade cerebral gliomas. Am J Neuroradiol 22(1): 60-64.
- Nonomura Y, Yasumoto M, Yoshimura R, Haraguchi K, Ito S, et al. (2001) Relationship between bone marrow cellularity and apparent diffusion coefficient. J Magn Reson Imaging 13(5): 757-760.
- Koh DM, Blackledge M, Padhani AR, Takahara T, Kwee TC et.al. (2012) Whole-body diffusion-weighted MRI: tips, tricks, and pitfalls. Am J Roentgenol 199(2): 252-262.
- Pasoglou V, Michoux N, Larbi A, Van Nieuwenhove S, Lecouvet F (2018) Whole Body MRI and oncology: recent major advances. Br J Radiol 91(1090): 20170664.
- Turkbey B, Choyke PL (2016) Prostate cancer: Birth of a standard: MET-RADS-P for metastatic prostate cancer. Nat Rev Urol 13(10): 568-570.
- Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, et.al. (2009) New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 45(2): 228-247.
- Lecouvet FE (2016) Whole-body MR imaging: musculoskeletal applications. Radiology 279(2): 345-365.
- Schlemmer HP, Schäfer J, Pfannenberg C, Radny P, Korchidi S, et al. (2005) Fast whole-body assessment of metastatic disease using a novel magnetic resonance imaging system: initial experiences. Invest Radiol 40(2): 64-71.
- Schmidt GP, Baur-Melnyk A, Herzog P, Schmid R, Tilling R, et al. (2005) High-resolution whole-body magnetic resonance image tumor staging with the use of parallel imaging versus dual-modality positron emission tomography–computed tomography: experience on a 32-channel system. Invest Radiol 40(12): 743-753.
- Wu LM, Gu HY, Zheng J, Xu X, Lin LH, et al (2011) Diagnostic value of whole‐body magnetic resonance imaging for bone metastases: a systematic review and meta‐analysis. J Magn Reson Imaging 34(1): 128-135.
- Shen G, Deng H, Hu S, Jia Z (2014) Comparison of choline-PET/CT, MRI, SPECT, and bone scintigraphy in the diagnosis of bone metastases in patients with prostate cancer: a meta-analysis. Skeletal Radiol 43(11): 1503-1513.
- Woolf DK, Padhani AR, Makris A (2014) Assessing response to treatment of bone metastases from breast cancer: what should be the standard of care? Ann Oncol 26(6): 1048-1057.
- Lee SC, Jain PA, Jethwa SC, Tripathy D, Yamashita MW (2014) Radiologist’s role in breast cancer staging: providing key information for clinicians. Radiographics 34(2): 330-342.
- Schmidt GP, Schmid R, Hahn K, Reiser MF (2004) Whole-body MRI and PET/CT in tumor diagnosis. Radiologe 44(11): 1079-1087.
- Yang HL, Liu T, Wang XM, Xu Y, Deng SM (2011) Diagnosis of bone metastases: a meta-analysis comparing 18FDG PET, CT, MRI and bone scintigraphy. Euro Radiol 21(12): 2604-2617.
- Mayor S (2009) NICE updates guidance on early and advanced breast cancer. Br Med J 338.
- Padhani AR, Lecouvet FE, Tunariu N, Koh DM, De Keyzer F, et al. (2017) Rationale for modernising imaging in advanced prostate cancer. Eur Urol Focus 3(2-3): 223-239.
- Lecouvet FE, Talbot JN, Messiou C, Bourguet P, Liu Y, et al. (2014) Monitoring the response of bone metastases to treatment with Magnetic Resonance Imaging and nuclear medicine techniques: a review and position statement by the European Organisation for Research and Treatment of Cancer imaging group. Eur J Cancer 50(15): 2519-2531.
- Lecouvet FE, El Mouedden J, Collette L, Coche E, Danse E, et al. (2012) Can whole-body magnetic resonance imaging with diffusion-weighted imaging replace Tc 99m bone scanning and computed tomography for single-step detection of metastases in patients with high-risk prostate cancer? Eur Urol 62(1): 68-75.
- Conde-Moreno AJ, Herrando-Parreño G, Muelas-Soria R, Ferrer-Robolleda J, Broseta-Torres R, et al. (2017) Whole-body diffusion-weighted magnetic resonance imaging (WB-DW-MRI) vs choline-positron emission tomography-computed tomography (choline-PET/CT) for selecting treatments in recurrent prostate cancer. Clin Transl Oncol 19(5): 553-561.
- Kapur A, Jain N, Kapur A, Mahajan G (2017) Is Whole Body–Diffusion MRI an Alternative to PET-CT! A Review of Literature. Clin Oncol 2: 1285.






























