Ear Discharge as a Symptom of a Malignant Tumor of a Temporal Bone
Dědková J1*, Chrobok V2 and Bělobrádek Z1
1Department of Radiology, Faculty Hospital, Faculty of Medicine, Hradec Králové, Charles University in Prague, Czechia
2Department of Otorhinolaryngology and Head and Neck Surgery, Faculty Hospital, Faculty of Medicine, Hradec Králové, Charles University in Prague, Czechia
Submission: August 24, 2019; Published: September 04, 2019
*Corresponding author: Jana Dědková, Department of Radiology, Faculty Hospital, Faculty of Medicine, Charles University in Prague, Hradec Králové 05, Sokolská 585, Czechia
How to cite this article: Rhabdomyosarcoma (RMS) is a highly malignant mesenchymal tumor that originates from a skeletal muscle. Curr Trends Clin Med Imaging. 2019; 2(5): 555617. DOI: 10.19080/CTCMI.2019.02.555617
Summary
We report a case of 5-year-old boy with one-week lasting pain and a discharge of the right ear. Symptoms persisted without improvement despite antibiotic treatment. The otoscopic finding was a polypous mass obturing an external auditory canal which was accompanied by a sanguinolent discharge. The boy’s head was examined by high resolution computer tomography (HRCT) and magnetic resonance imaging (MRI) with finding of a soft tissue mass filling the external auditory canal, a middle ear, mastoid and its air cell system and large bone destruction in the area of the mesotympanon, protympanon, apex of pyramid and carotic canal on the right side. The final diagnosis of rhabdomyosarcoma was established by histological examination of a sample obtained from polyp mass in external auditory canal. The aim of this article is to call attention to a possibility of rare but serious cause of the ear discharge.
Keywords: Magnetic Resonance Imaging (MRI), Otitis, Computer Tomography (CT), Rhabdomyosarcoma
Intrоductiоn
Rhabdomyosarcoma (RMS) is a highly malignant mesenchymal tumor that originates from a skeletal muscle. It appears most often in children; it affects mostly head and neck region and it represents 40 % of all the RMS cases. Rarely it affects the temporal bone, according to the literature 8 to 10% of all RSM of the head and neck region [1-3]. With microscopic examination we can classify RMS according to its histopathology to four subtypes: embryonal, alveolar, botryoid and pleomorfic. In the head and neck region, embryonal type occurs most often. The etiology of RMS is unknown. Most of the cases occur sporadically without any known predisposition or a risk factor [4].
Diagnosis of the temporal bone RMS is difficult, clinically it’s manifested as a middle ear infection or a polyp in the ear canal. Among clinical symptoms belong pain, bloody discharge from the ear, hearing impairment and facial nerve paralysis. Impairment of cranial nerves is a signal for infiltration of the tumor into cranial base and intracranially [1,2,5]. The development of the illness is often fatal, Jaffe et kol. in the 1932 states 0% survival after 2 years from the diagnosis [1]. Only after introduction of new medical procedures (chemotherapy, radiotherapy) the prognosis of the disease has distinctively improved. At the present day the literature states 41 - 81 % of 5-year survival. Prognosis of the disease depends on tumor expansion and infiltration extra temporally and intracranially and on the presence of metastases [1,5-7].

The traditional imaging approach for diagnosing underlying cause for post cholecystectomy pain has involved ultrasound and/or Computed Tomography (CT) followed by direct cholangiography, whereas manometry of the sphincter of Oddi and biliary scintigraphy have been reserved for cases of biliary dyskinesia. Because of its capability to provide non-invasive high-quality visualization of the biliary tract, MRCP has been advocated as a reliable imaging tool for assessing patients with post cholecystectomy pain or suspected PCS and for guiding management decisions. The present study was carried out to find the incidence and risk factors for post cholecystectomy pain in patients undergoing cholecystectomy. This paper illustrates the rationale for using MRCP, together with the main MRCP biliary findings and diagnostic pitfalls.
Case History
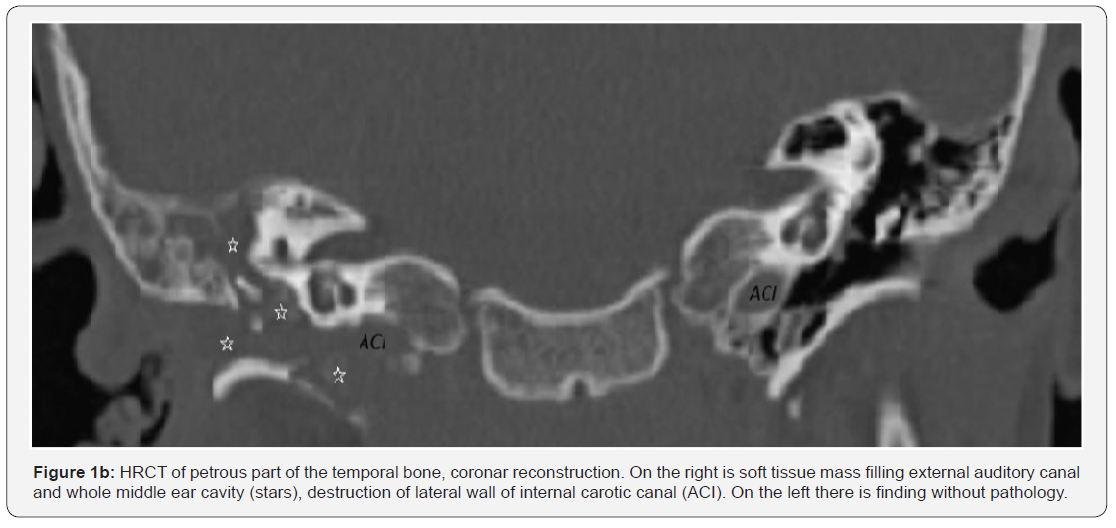
5-year-old boy was sent to a local hospital for one-week lasting ear pain and discharge from the right ear. The discharge from the ear hasn’t improved even after antibiotic therapy with erythromycin. The clinical symptoms worsened. An HRCT examination was performed in the local hospital described a soft tissue mass filling the eardrum cavity, pneumatic system of the mastoid process and the ear canal. Not only an extensive destruction of protympanic, hypotympanic and partly mesotympanic bony part was occurred, but partly was also destruction of a mastoid processes, septum, apex of the petrous pyramid and the carotid sinuses wall (Figures 1a & 1b). The boy was hospitalized in a pediatric department of the Otolaryngology clinic, College Hospital Hradec Králové. The overall status was normal with no alteration of the consciousness, temperature was slightly higher 37,5°C. In a local finding the right outer ear canal was completely filled with a polypous mass and sanguinolent discharge. An otomicroscopic examination of the right ear was performed in general anesthesia. Heavily bleeding polypous mass filling the outer ear canal was found and a sample from the outer ear canal and the tympanic cavity was taken.

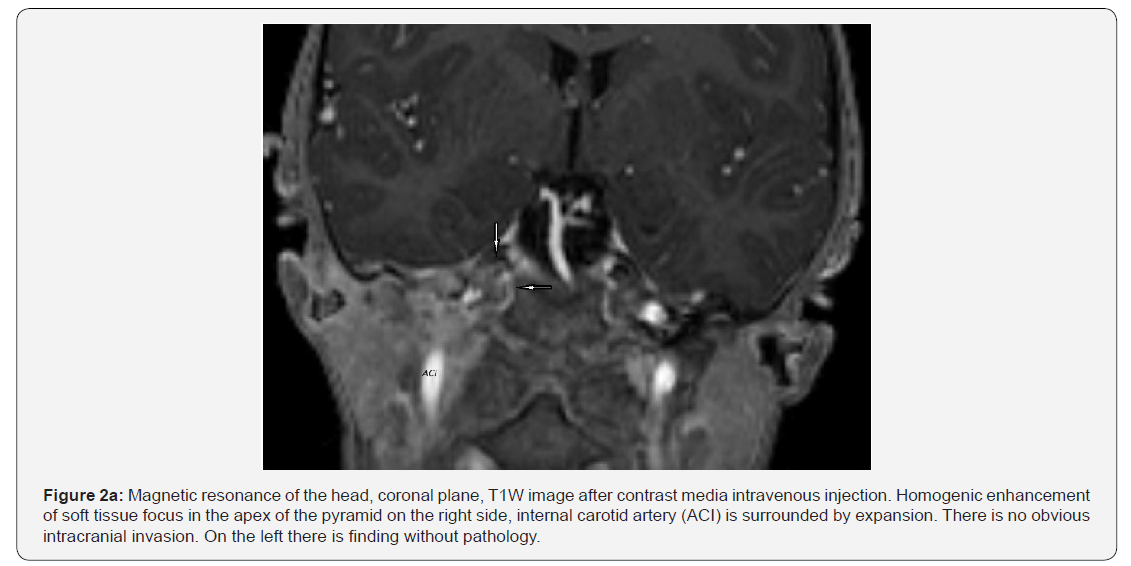
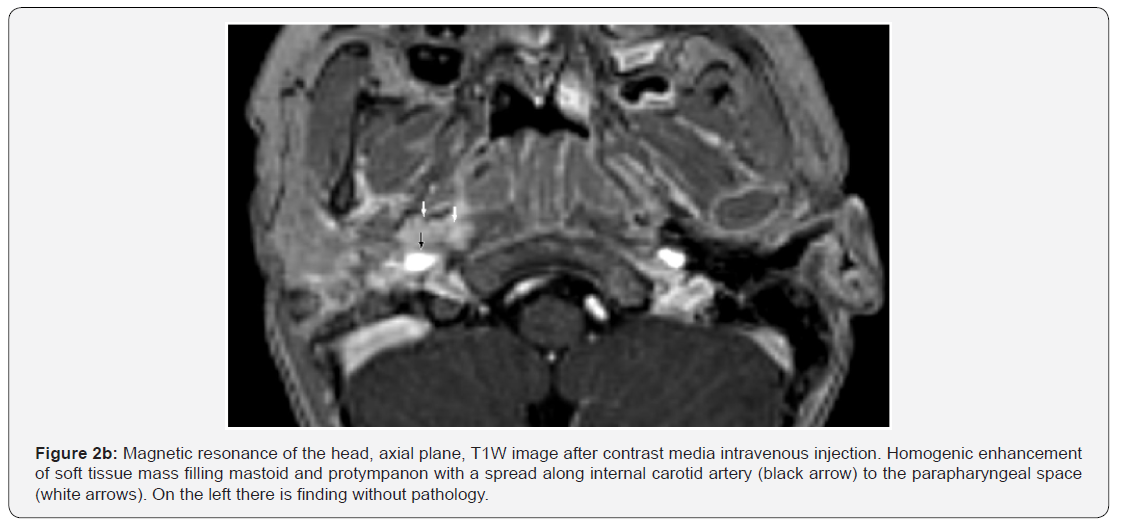
Afterwards an MRI examination was indicated to get more detailed image of the right tympanic bone alteration. The MRI examination (Figures 2a & 2b) shown us homogenic T1 hypointense and T2 hyperintense mass with a distinctive increase of T1 signal after intravenous application of paramagnetic contrast dye. The mass was filling the tympanic cavity, laterally further to the outer ear canal and mastoid process, the apex of pyramid and ventrally and inferiorly spreading along the internal carotid artery into the parapharyngeal space. Four regional lymphatic nodes were enlarged: 15 to 20 mm. Radiologist suspected otitis with mastoiditis and didn’t exclude tumorous etiology in the differential diagnosis. Histologic examination of the sample proved malignant tumor - embryonal rhabdomyosarcoma (RMS).
Discussion
Rhabdomyosarcoma of a temporal bone is localized in the tympanic cavity. The probable places of origin are a tensor tympani muscle and an ear canal. It is an aggressive tumor that grows fast and destroys a bony tissue. The tumor infiltrates the outer ear canal where it creates a polypous granulation tissue. Then it spreads into the mastoid process and destroys the Fallopian canal wall. That leads to the paralysis of a facial nerve [1,3,5]. When the tumor infiltrates the inner ear and inner ear canal, then hearing impairment, damage of cranial nerves in that area (nn.VII, VIII) and damage of the pyramidal apex (n.V, Gradenigo syndrome) can occur. If the tumor keeps on growing, it expands intracranially into the middle cranial fossa via tegmen tympani and into the posterior cranial fossa via inner ear canal. It can also penetrate mediocaudally into the parapharyngeal space and infratemporal area. It can infiltrate distant places via hematogenic or lymphogenic metastases. Most often it metastasizes into lungs; other tissues that can be affected are brain, skeleton and liver [1,2,3,7,8].
We can distinguish three clinical phases of the illness (3).
i. phase: the tumor is restricted only to the middle ear, clinical symptoms are similar to the middle ear inflammation
ii. phase: the tumor infiltrates infra temporally, the clinical features are ear pain, hearing impairment or paralysis of n. VII
iii. phase: the tumor infiltrates extra temporally: into parapharyngeal space, into infratemporal area or intracranially, most often into the middle cranial fossa. The damage of V and VI cranial nerves is a signature of the infiltration into the cranial fossa. The III. phase is the most commonly found diagnosed.
Clinical findings and modern imagining techniques (CT and MRI) contribute to the diagnosis of the temporal bone RMS. Computed topography (CT) applied with high resolution technique (HRCT) enables submilimetric image of small bony structures of the temporal bone. The CT of RMS shows a soft tissue mass without calcifications an with an aggressive destruction of the skeleton. Magnetic resonance (MR) combines three-dimensional resolution and high soft tissue contrast in high quality. MR displays homogenic expansion, in T1 sequence typically isointense with a muscular tissue and distinctively hyperintense in T2 sequences. After intravenous application of the contrast media, an opacification of the expansion appears. On DWI (Diffusion Weighted Imaging) sequences there is no restriction of diffusion [9,10]. Differential diagnosis of RMS on CT and MR is difficult, both imagining examinations are highly sensitive, but the specificity is low. Knowledge of medical history and clinical data can significantly help to establish more accurate diagnosis and etiology of displayed pathological changes of the temporal bone. In the differential diagnosis of the temporal bone RMS we include benign illnesses such as otititis or cholesteatoma and malignant illnesses such as sarcomas, histiocitosis, lymfoma and spino cellular carcinoma. Final diagnosis must be always determined by a pathologist based on histological examination [10].
At the present day the treatment used is chemotherapy, radiotherapy and surgical resection. The literature doesn’t state any definite and unified procedure; however, it agrees that the combination of individual therapeutic modalities improves the prognosis of this serious illness [1,3,5,7].
Conclusion
We presented a rare case history of the temporal bone rhabdomyosarcoma. The tumor hence to the direction of infiltration, most likely came out from the outer ear canal and the mastoid process. Extra temporally it expanded alongside inner carotid into the parapharyngeal area. According to the enlarged lymphatic nodes we can anticipate tumorous infiltration of regional lymphatic nodes. It was a III. clinical phase of the illness. We should suspect this serious illness when the clinical symptoms of otitis don’t react to the antibiotic treatment or when appearance of a polyp in an outer ear canal with an aggressive destruction of skeleton and soft tissue mass in a temporal bone on MRI and CT. At the present day the best results in the treatment of RMS bring an early diagnosis and the use of multimodal therapy.
References
- Sbeity S, Abela A, Arcand P, Quintal M, Saliba I (2007) Temporal bone rhabdomyosarcoma in children. Inter J Pediatr Otorhinolaryngolog 7: 807-814.
- Vegari S, A Hemati A, Baybordi H, Davarimajd L, Chatrbahr G (2012) Embryonal Rhabdomyosarcoma in Mastoid and Middle ear in a 3-Year-Old Girl: A Rare Case Report. Case report in Otolaryngology: 871235.
- Castillo M, Pillsbury HC (1993) Rhabdomyosarcoma of the Middle ear: Imaging features in two children. AJNR 14: 730-733.
- Kraus DH, Saenz NC, Gollamudi S, Heller G, Moustakis M, et al. (1997) Pediatric rhabdomyosarcoma of the head and neck. Am J Surg 174(5): 556-560.
- Durve DV, Kanegaonkar RG, Albert D, Levitt G (2004) Pediatric rhabdomyosarcoma of the ear and the temporal bone. Clin. Otolaryngol. Allied Sci 29(1): 32-37.
- Canalis RF, Gussen R (1980) Temporal Bone Findings in Rhabdomyosarcoma with Predominantly Petrous Involvement. Arch Otolaryngol Head Neck Surg 106(5): 290-293.
- Parham DM, Ellison DA (2006) Rhabdomyosarcomas in adults and children: Archives of Pathology and Laboratory Medicine 130 (10): 1454–1465.
- Schiavetto RR, Haber DM, Cancian LC, Maniglia CP, Drimel F (2009) Rhabdomyosacoma. Int Arch Otorhinolaryngol 13(3): 326-330.
- Yousem DM, Lexa FJ, Bilaniuk LT, Zimmermann LT (1990) Rhabdomyosarcomas in the Head and Neck: MR Imaging Evaluation. Radiology 177: 683-688.
- Lee JH, Lee MS, Lee BH, Choe DH, Do YS, et al. (1996) Rhabdomyosarcoma of the Head and Neck in Adults: MR and CT Findings. AJNR Am J Neuroradiol 17: 1923-1928.






























