Clinical Challenges in Image Guided Radiation Therapy (Igrt) For Gynaecological Malignancies
Pushpa Naga CH* and Umesh Mahantshetty
Department of Radiation Oncology, Tata Memorial Hospital, Centre, Homi Bhabha National Institute (HBNI), Mumbai, India
Submission:April 08, 2019; Published:May 22, 2019
*Corresponding author: Pushpa Naga CH, Department of Radiation Oncology, Homi Bhabha Block,Tata Memorial Hospital, Dr Ernest Borges Street, Mumbai 400012, India
How to cite this article: Pushpa N CH, Umesh M. Clinical Challenges in Image Guided Radiation Therapy (Igrt) For Gynaecological Malignancies. Curr Trends Clin Med Imaging. 2019; 2(5): 555608. DOI: 10.19080/CTCMI.2019.02.555608
Keywоrds
Keywords: Gynaecological cancer, Radiation therapy, IGRT, Challengess
Opinion
Traditionally, the pelvic treatment fields for gynaecological cancer were designed based on bony landmarks using two-dimensional planning. However, with the advances in radiation oncology, clinical usage of high-end technology machines delivering static/fixed-beam, dynamic, rotational intensity modulated radiotherapy (IMRT) and arc therapy is increasing rapidly. Given the steep dose gradients of these highly conformal treatment delivery techniques, precise and reproducible target positioning is essential. Accuracy is even more important in treatment of cervical cancer with intact uterus which requires simultaneous irradiation of the cervix, entire uterus, vagina, parametrium, and draining lymph nodal region. As independent movement of these volumes along with day-to-day variation in bladder & rectal filling and bowel movements presents an additional challenge. Also, tumour regression during the course of treatment can add to the uncertainty of dose delivery. All these issues necessitate the need for image-guidance during treatment delivery which enables the clinicians to visualize the target volume and its relation to surrounding organs. Image-guided radiation therapy (IGRT) has become the state-of-the-art technology for most of the sites [1,2]. Similarly, for gynaecological malignancies a variety of IGRT tools have been integrated in the modern radiotherapy practice. The most widely practiced ones are based on imaging using electronic portal devices (EPIDs) or kV volumetric imaging devices. In both cases bony anatomy is used to verify patient position changes. Although bony shift is compatible with the position of the lymph nodes, movement of cervix is totally unrelated to the bony anatomy. Moreover, uterus move independently from the mentioned both cervix and lymph nodal target volumes. Thus, even when the patient is positioned in accordance with soft-tissue image- guidance localization of the cervical lesion, the same shift is applied to all irradiated volumes, which is not always correct (Figure 1).
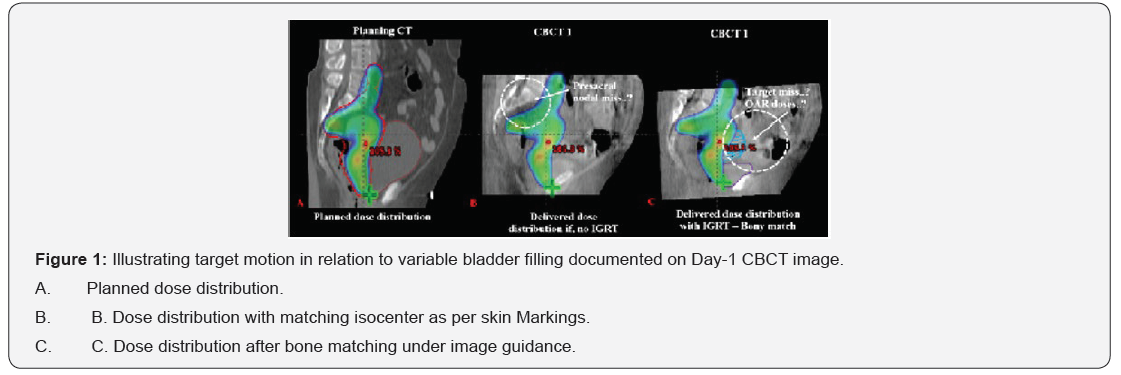
Current clinical practice involves the use of ‘populationbased’ margins which is based on typical bony anatomy variations in human populations. However, such an approach not only fails to account for individual variations, but also fails to consider the independent movement of the various target volumes. Larger PTV margins to encounter the above problem results in increased doses to organ at risk (OAR), especially bowel while smaller margins would result in geographical miss of the target volume. Hence adopting strict reproducible bladder filling and rectum emptying protocol along with verifications performed on a ‘plan-of-the-day’ strategy may overcome this problem by establishing PTV margins that are sufficiently large to encompass the target volumes without geographical miss but small enough to minimize OAR doses.
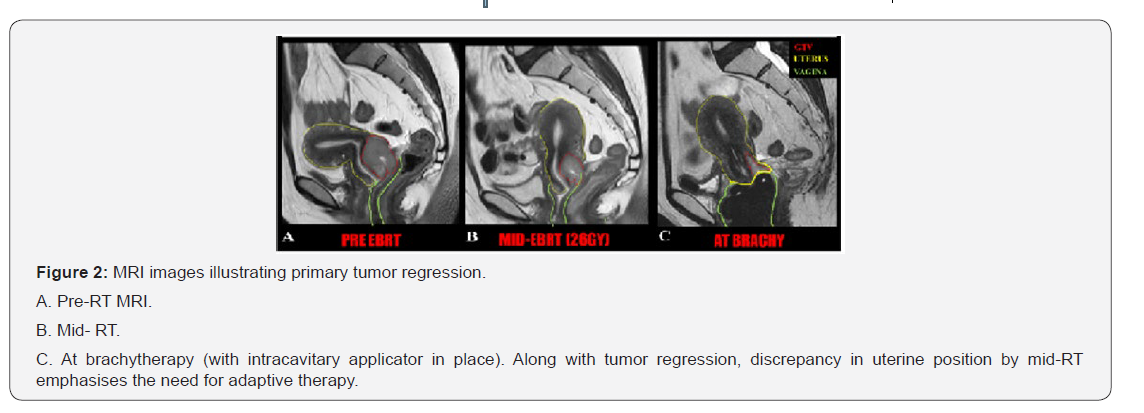
Primary tumor regression during pelvic radiotherapy resulting in varied dose deposition to adjacent normal structures is another contributing factor (Figure 2). Preliminary reports quantifying the tumor regression reveals, nearly 50-75% regression during course of EBRT followed by additional 10- 15% during brachytherapy sessions [3]. One of the ways that could be explored to resolve this issue is by real-time adaptive radiotherapy (ART). The added complexity of the adaptive processes and given the demands on time and resources, replanning at mid-RT can be a logical recommended approach. But the poorer soft tissue visualization with available daily volumetric imaging, makes difficult to quantify tumor regression. Hence decision regarding re-planning needs to be considered under strict IGRT protocol with serial documentation of target and OAR deformation and their doses.
Conclusion
In conclusion, use of IGRT in gynecological malignancies is not without its challenges. Imaging and biology related uncertainties are not corrected by IGRT; therefore, the promise of IGRT to be able to reduce PTV margins needs to be overlooked. Nevertheless, current image-guidance methods have introduced new considerations to the treatment delivery process. Optimal imaging protocols and vigilant correction strategies can extend the capabilities of IGRT in achieving comprehensive continual improvement in patient care and clinical outcomes.
References
- Intensity Modulated Radiation Therapy Collaborative Working Group (2001) Intensity-modulated radiotherapy: Current status and issues of interest. Int J Radiat Oncol Biol Phys 51: 880–914.
- Dawson LA, Jaffray DA (2007) Advances in image-guided radiation therapy. J Clin Oncol 25: 938–946.
- Dimopoulos JC, Schirl G, Baldinger A (2009) MRI assessment of cervical cancer for adaptive radiotherapy. Strahlenther Onkol 185: 282–287.






























