Calcified Nodules with Metastatic Dissemination to Multiple Organs and Systems: A Rare and Surprising Presentation of Primary Lung Adenocarcinoma
José Vitor Rassi Garcia1, Anderson Costa Lino Costa2, Francisco Barbosa de Araújo Neto3
1Department of Radiology, Hospital Heliópolis, São Paulo-SP, Brazil
2Department of Pathology, Hospital Heliópolis, São Paulo-SP Brazil
3Department of Radiology, Medical School of the University of São Paulo and Department of Radiology of the Hospital Heliópolis, São Paulo-SP, Brazil
Submission: February 28, 2019; Published: March 14, 2019
*Corresponding author: José Vitor Rassi Garcia, Radiologist, Department of Radiology of the Hospital Heliopolis, São Paulo-SP, Brazil
How to cite this article: José V R G, Anderson C L, Francisco B d A N. Calcified Nodules with Metastatic Dissemination to Multiple Organs and Systems: A Rare and Surprising Presentation of Primary Lung Adenocarcinoma . Curr Trends Clin Med Imaging. 2019; 2(5): 555603. DOI: 10.19080/CTCMI.2019.02.555603
Abstract
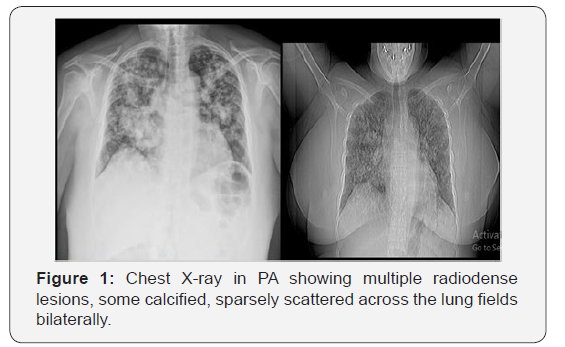
With increased use of computed tomography of the chest as a crucial diagnostic method, more lung injury began to be achieved in the early stages. One of the most important findings is the pulmonary nodules. Calcified pulmonary nodules are a group with a relatively narrow differential of diagnoses and will be discussed in this article. We report the case of a 46-year-old woman without prior disease who was evaluated in our emergency room with shortness of breath, cough and chest pain, both started two months ago. It progressed with progressive worsening of the condition in the last week. She denied weight loss, denied a fever, and denied drug abuse during that time. In the emergency room, the patient underwent chest radiography and chest tomography. Chest x-ray showed multiple radiodense lesions, some calcified, spread bilaterally over the lung fields. Chest tomography demonstrated multiple nodules and solid lung masses, most with calcifications, both of unknown etiology.
The initial diagnostic hypotheses were pulmonary tuberculosis, pulmonary neoplasia and pneumoconiosis. The initial support measures were performed, and the patient was admitted to our hospital for diagnostic investigation and treatment. During hospitalization, the patient was diagnosed with primary lung adenocarcinoma with calcified lesions and calcified metastatic lesions to organs and systems. Although common, it is of paramount importance to diagnose calcified pulmonary nodules and generally seek its etiology and cause, since these nodules can represent benign and or malignant lesions, having different conducts in the therapeutic approach.
Keywords:Tomography, Calcified Nodules, Primary Lung Cancer, Adenocarcinoma, Neoplasm Metastasis
Intrоductiоn
With the increase of computed tomography as a crucial diagnose method, more pulmonary lesions started to be caught up at initial stages. One of the most important findings are pulmonary nodules. There are a lot of variations that might be considered to its evaluation, such as size, morphology and distribution. When it comes to morphology, there are three possible variations, solid pulmonary nodules, partly solid pulmonary nodules and ground glass pulmonary nodules. All of them can be calcified or not, and that´s an important characteristic to guide the diagnose [1].
Case Report
We report the case of a 46-year-old woman without prior disease who was evaluated in our emergency room with shortness of breath, cough and chest pain, both started two months ago. It progressed with progressive worsening of the condition in the last week. She denied weight loss, denied a fever, and denied drug abuse during that time. In the emergency room, the patient underwent chest radiography and chest tomography. Chest x-ray (Figure 1) showed multiple radiodense lesions, some calcified, spread bilaterally over the lung fields. The initial diagnostic hypotheses were pulmonary tuberculosis, pulmonary neoplasia and pneumoconiosis. The initial support measures were performed, and the patient was admitted to our hospital for diagnostic investigation and treatment. During the hospitalization, a complete anamnesis was performed that discarded a history of exposure to potential pathological particles. Laboratory tests were within normal limits and tuberculosis research was negative. The patient underwent further imaging tests, such as neck, thorax and total abdomen tomography, and performed a battery of laboratory tests, including tuberculosis research.
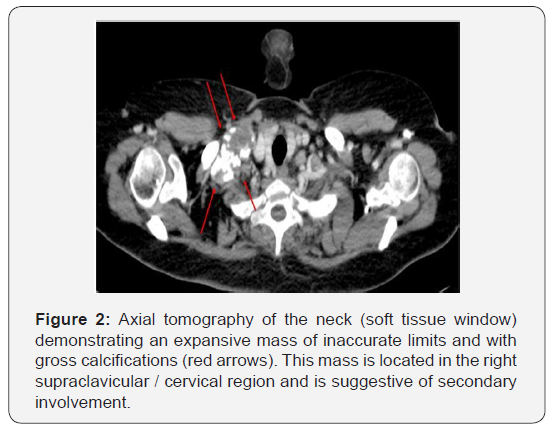
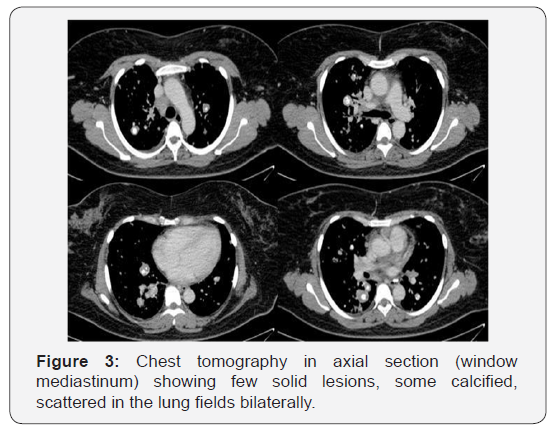
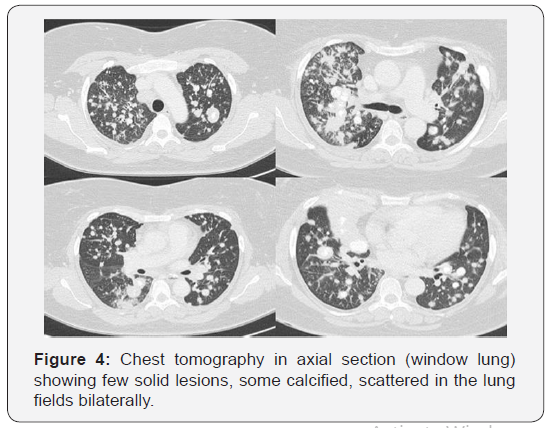
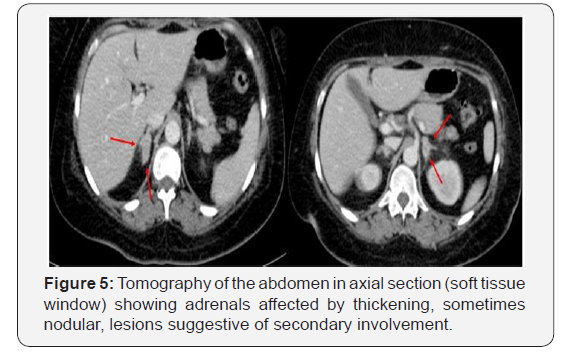
The tomography of the neck (Figure 2) showed an expansive mass of imprecise limits and with gross calcifications in its interior. This mass is located in the right supraclavicular / cervical region and is suspected of secondary involvement. Chest tomography (Figures 3 & 4) shower some nodules and solid lung masses, most with calcifications, both of unknown etiology. Calcified lymph nodes on both sides of the neck and mediastinum were also observed. Tomography of the abdomen (Figure 5) demonstrated a nodular thickening in the adrenal glands, probably due to secondary involvement. Other abdominal organs with no apparent signs of injury. No changes were found in breast, thyroid, and bone. Neoplasia and pneumoconiosis continued as the main hypotheses in the differential diagnoses after this new evaluation.
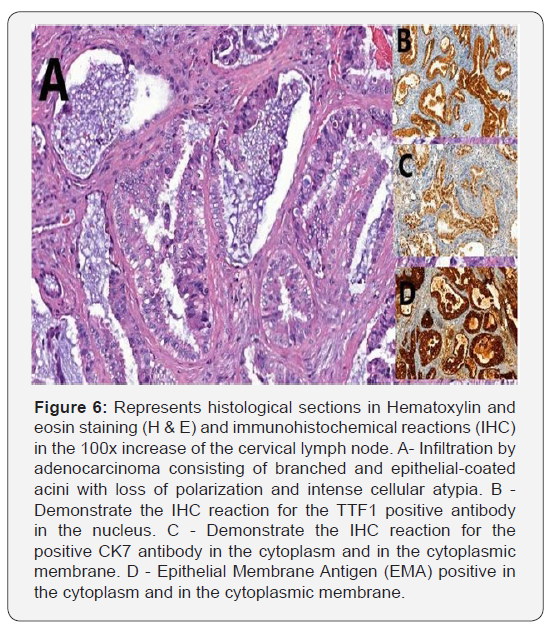
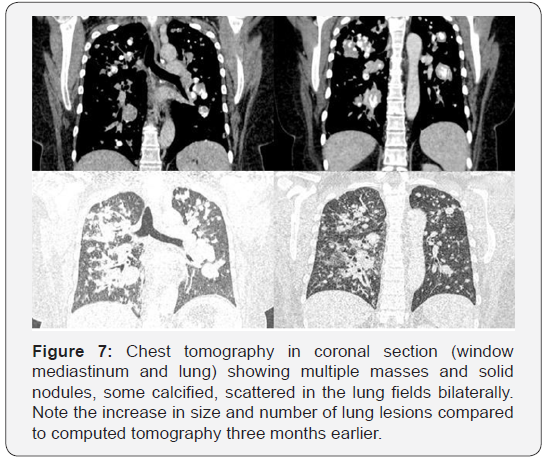
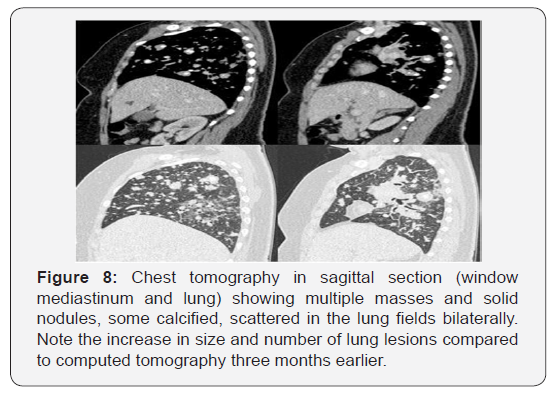
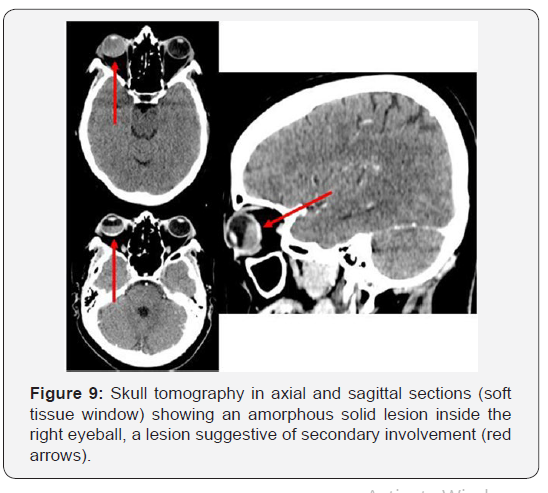
The medical team decided to continue the diagnostic investigation by performing a biopsy of the lesion in the supraclavicular / right cervical region and sent the collected material to the anatomopathological. The anatomopathological result (Figure 6) showed acinar structures in the extracted lesion. An immunohistochemical study (Figure 6) was requested, which resulted in positive cytokeratin 7 (CK-7); Positive Thyroid Transcription Factor 1 (TTF-1); E-cadherin positive; Positive Epithelial Membrane Antigen (EMA); other factors, such as thyroglobulin, chromogranin, CK 5/6, Ca 125, CK 20 estrogen receptor, progesterone receptor and WT-1 were all negative. This immunoexpressed profile is highly suggestive of primary lung cancer [2-4], which was considered the final diagnosis due to the lack of findings in other organs. The chemotherapy regimen for primary lung adenocarcinoma was started and the patient presented progression of the disease with low response to treatment. About three months after diagnosis, a new chest tomography (Figures 7 & 8) revealed an increase in the number and size of lung lesions. In addition, a computed tomography scan of the skull was performed to assess a complaint and a symptom of the patient’s visual turbidity in the right eye. Cranial tomography (Figure 9) showed an amorphous solid lesion within the right eyeball, which evolved from partial involvement to total vitreous humor. No extra-axial or intra-axial cranial changes were found. This eyeball injury was considered as secondary involvement. The clinical team decided to keep the chemotherapy regimen current and the patient had progressive clinical worsening. Currently, the patient is being treated with another chemotherapy regimen for primary lung adenocarcinoma, with a low clinical response, making this case challenging and atypical.
Discussion
Calcified pulmonary nodules are a group with a relatively narrow differential [5]. Usually central, diffuse, laminated or popcorn calcifications are benign patterns [6]. These types can be seen in granulomatous disease and hamartomas. The most common cause of nodule calcification is granuloma formation in response to a healed infection, with residual aspect. All other patterns of calcification should be considered, at least, suspicious. However, there is an exception. If the patient is known to have a primary tumor, a diffuse calcification, for example, may be seen in osteosarcoma pulmonary metastasis [7]. Other examples are central and popcorn patterns, which also may be seen in patients with GI-tumors and patients who already passed throughout chemotherapy. Occupational diseases, also known as pneumoconiosis, are a differential that need to be considered, which explains why is so important to know the patients background history of work [6]. Silicosis is associated with nodal egg-shell calcification and multiple small densely calcified nodules that are upper lobe predominant. Coal worker’s pneumoconiosis may present the same pattern of silicosis, but with smaller nodules, and minimal symptoms [8].
Just as previously said, patients with known history of primary cancer showing multiple calcified pulmonary nodules at CT scan, need to be considered with a high chance of having calcified pulmonary metastasis. Typically, there are a variety of mechanisms that cause calcification in metastasis, such as bone formation in tumors osteoid origin, calcification and ossification of tumor cartilage, dystrophic calcification and ossification of tumor cartilage and dystrophic calcification and mucoid calcification [7]. The spectrum of primary malignancies that can cause calcification of metastatic nodules, includes sarcomas, such as osteosarcoma, chondrosarcoma and synovial sarcoma; mucinous type carcinomas, including colon carcinomas, ovarian cancers and breast cancer; medullary thyroid carcinoma; giant cell tumor of the bone and treated metastatic choriocarcinoma [7]. Primary adenocarcinoma of the lung is the most frequent histological type of lung cancer (around 40% of the cases), being also the most diagnosed one in non-smokers, besides more seen in smokers. Histologically it is classified as a non-small cell carcinoma and is a malignant tumor that can be associated with mucin production, which, in some cases, develops mucoid calcification [5-15].
In 2011 a new classification for adenocarcinoma of the lung was introduced by the International Association for the Study of Lung Cancer (IASLC), American Thoracic Society (ATS), and European Respiratory Society (ERS), dividing its types in: preinvasive adenocarcinoma lesions; minimally invasive adenocarcinoma and invasive adenocarcinoma. One of the variants of this least one type is the invasive mucinous adenocarcinoma (formerly mucinous BAC), which is more likely to be multicentric multilobar, and may show bilateral lung involvement [12], indicating aerogenous spread [13], tending to have a worse prognosis than non-mucinous types.
The anatomopathological report of the biopsied cervical lymph node was infiltration by adenocarcinoma. The sample was submitted to a complementary immunohistochemical examination, which revealed a highly suggestive pattern of primary adenocarcinoma of the lungs: CK 7+, TTF-1 +, and CK 20 -, rejecting the hypothesis of an extrapulmonary primary site with specificity above 98% [2-4]. Other sensitive markers were positive in the sample, such as E-cadherin and epithelial membrane antigen (EMA), which corroborate the diagnosis of carcinoma. Markers such as WT1; Ca 125; Thyroglobulin; Progesterone and Estrogen receptors; CK 5/6 and Chromogranin were negative in the sample, corroborating the findings of previous complementary tests, negative for ovarian, thyroid, breast, gastrointestinal tract and neuroendocrine tumors.
Conclusion
There are not many case reports in the literature showing primary lung adenocarcinomas with calcified aspect associated with metastases. In this case, in addition to the unusual pattern, the secondary involvement of the lung, adrenal and right orbit of the patient (metastasis to the orbits may present as primary site the lungs in up to 23% of the cases) [14]. Such diversity of findings led the medical team to first rule out nonneoplastic hypotheses of calcified pulmonary nodules. After confirming the carcinomatous pattern, all the possible primary sites of extrapulmonary adenocarcinomas were investigated, which did not show relevant alterations. With the result of the anatomopathological and immunohistochemical tests, the diagnosis was closed for this challenging case of pulmonary primary adenocarcinoma of aggressive behavior and calcified pattern.
This case report is important for radiologists and the medical community in general, as it demonstrates through CT scan an infrequent spectrum of lung adenocarcinoma, presenting as lung nodules and calcified metastases.
References
- CERRI, Giovanni Guido, LEITE, Cláudia da Costa, ROCHA et al. (2017) Tratado de Radiologia: Pulmões coração e vasos Gastrointestinal Uroginecologia. In: (Ed.), São Paulo: Manole 3(2).
- Ikeda S, Fujimori M, Shibata S (2006) Combined immunohistochemistry of beta-catenin, cytokeratin 7, and cytokeratin 20 is useful in discriminating primary lung adenocarcinomas from metastatic colorectal cancer. BMC Cancer 6: 31.
- Su YC, Hsu YC, Chai CY (2006) Role of TTF-1, CK20, and CK7 immunohistochemistry for diagnosis of primary and secondary lung adenocarcinoma. Kaohsiung Journal of Medical Sciences 22(1): 14–19.
- Gurda GT, Zhang L, Wang Y, Chen L, Geddes S (2015) Utility of five commonly used immunohistochemical markers TTF-1, Napsin A, CK7, P63 and CK5/6 in primary and metastatic adenocarcinoma and squamous cell carcinoma of the lung. A retrospective study of 246 fine needle aspiration cases. Clin Transl Med 4: 16.
- Mahoney MC (1990) CT demonstration of calcification in carcinoma of the lung. American Journal of Roentgenology 154(2): 255-258.
- Marchiori E, Souza AS, Franquet T (2005) Diffuse high-attenuation pulmonary abnormalities: a pattern-oriented diagnostic approach on high-resolution CT. AJR Am J Roentgenol 184 (1): 273-282.
- Maile Charles W (1982) Calcification in pulmonary metastases. The British Journal of Radiology 55(650): 108-113.
- Remy-Jardin M, Degreef JM, Beuscart R (1990) Coal worker's pneumoconiosis: CT assessment in exposed workers and correlation with radiographic findings. Radiology 177(2): 363-371.
- Gaikwad Anand (2012) Primary adenocarcinoma of lung: A pictorial review of recent updates. European Journal of Radiology 81(12): 4146-4155.
- Khan Alinawaz (2010) The calcified lung nodule: What does it mean?. Annals of Thoracic Medicine 5(2): 67-79.
- Grewal Ritu G, Austin John HM (1994) CT Demonstration of Calcification in Carcinoma of the Lung. Journal of Computer Assisted Tomography 18(6): 867-871.
- Lee KS, Kim Y, Han J (1997) Bronchioloalveolar carcinoma: clinical, histopathologic, and radiologic findings. Radiographics 17(6): 1345-1357.
- Travis WD, Brambilla E, Noguchi M (2011) International association for the study of lung cancer/american thoracic society/european respiratory society international multidisciplinary classification of lung adenocarcinoma. J Thorac Oncol 6(2): 244-285.
- Correa, Zélia Maria da Silva (2005) Prevalência de metástases oculares em pacientes com doença metastática reconhecida: resultados preliminares. Arq. Bras. Oftalmol. 68(2): 189-193.
- Rosado-de-christenson ML, Templeton PA, Moran CA (1994) Bronchogenic carcinoma: radiologic-pathologic correlation. Radiographics 14 (2): 429-446.






























