Understanding Computed Tomography (CT) Dose Reduction Techniques and Principles in a Simplified Way
Pradosh Kumar Sarangi*, Jayashree Mohanty, Sasmita Parida and Basanta Manjari Swain
Department of Radiodiagnosis, SCB medical college & Hospital, India
Submission: February 18, 2017; Published: March 16, 2017
*Corresponding author: Pradosh Kumar Sarangi, Junior resident, Department of Radio diagnosis, SCB medical college & Hospital, Dock Road, Manglabag, Cuttack, Odisha 753007, Cuttack, Odisha, India, Tel: 7735860624; Email: lipu90sarangi@gmail.com
How to cite this article: Pradosh K S, Jayashree M, Sasmita P, Basanta M S. Understanding Computed Tomography (CT) Dose Reduction Techniques and Principles in a Simplified Way. Curr Trends Clin Med Imaging. 2017; 1(2): 555557. DOI: 10.19080/CTCMI.2017.01.555557
Abstract
Use of computed tomography (CT) has increased tremendously over the last two decades. Compared to the lowest dose x-ray techniques, CT scans can have 100 to 1,000 time’s higher radiation dose than conventional X-rays. Despite its usefulness, potential risk of radiation induced malignancy does exist which cannot be ignored. One study estimated that as much as 0.4% of all current cancers in the United States are attributable to CT examinations based on CT usage data from 1991–1996. Hence it is imperative to know about CT dose reduction techniques. This review will give readers an insight to strategies for dose reduction and principles behind them.
Keywords: Dose Reduction; Radiation risk; Computed tomography; ALARA principle; Tube current (mA) modulation
Abbreviations: ALARA: As Low As Reasonably Achievable; DLP: Dose length product; CTDIvol : Volume CT Dose Index; ICRP: The International Commission on Radiological Protection; DQE: Detective Quantum Efficiency; AEC: Automatic Exposure Control; HYPR-LR: Highly Constrained Back Projection Local Reconstruction; MBF: Multiband Filtering
Introduction
Since the risk of radiation induced malignancy attributable to CT is not totally zero and in light of dramatic increase in number of CT scans, dose reductions strategies are one of important consideration [1]. Since there is a definite benefit of CT scan in diagnosis and planning therapeutic procedures, a risk-benefit assessment should be done in each individual.
Guiding principles of radiation protection
There are three guiding principles for radiation protection in current clinical practice [2-4].
Justification: CT examination must be appropriately justified in each individual. Unless there is a sufficient benefit to offset the detrimental effect of radiation, CT scan should be avoided
It is the shared responsibility of requesting clinicians and radiologists which helps in directing patients for the most appropriate imaging modality.
Optimization: Simply known as ALARA principle (As Low as Reasonably Achievable). It means for each diagnostic task, all technical aspects of examination must be optimized in relation to magnitude of doses, number of people exposed etc. such that necessary diagnostic information can be obtained while keeping dose as low as possible.
Limitation: To keep dose levels to occupationally expose individuals limited to levels recommended by consensus organisations. For example, Atomic Energy Regulatory Board (AERB) in India.
Before discussing further, it is important to know about quantifying CT radiation output from a CTs canner and various terminologies used in dose measurement.
Scanner radiation output
It is represented by volume CT dose index (CTDIvol) [5]. It measures radiation output from a scanner in a very standardised way using a pair of standardised acrylic phantoms. It is measured from one axial CT scan (one rotation of x ray tube). The head and body phantom measures 16 cm and 32 cm in diameter respectively with a length of 14cm.
Its SI unit is mili-gray (mGy). It is a useful indicator of the radiation output for a specific exam protocol. However, it is important to know that it is not a direct measurement of patient dose.
Dose length product (DLP): It represents the overall energy delivered in a complete scan acquisition [6]. DLP (mGy-cm) = CTDIvol× scan length (cm)
Implication: CTDIvol can be same in abdomen only or abdomen -pelvic CT scan. But DLP is more in the latter type.
Effective dose (E): It is a concept that reflects the stochastic risk (cancer induction) to a given patient. It is not a measurement of dose [7,8].
It is a quantity representing a whole body equivalent dose that would have a similar risk of health determinant as that due to partial body irradiation. It allows an approximate comparison of risk among different types of examination. It is expressed in mSv (millisievert) (Table 1).
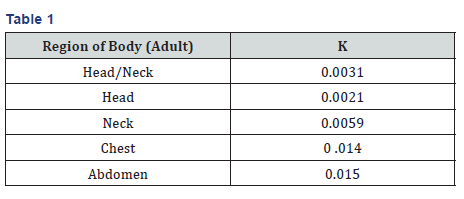
E=DLP (mGy-cm)×k (mSv/mGy-cm), where k is a regionspecific coefficient which depends on the region being scanned also called tissue weighting factor [9]. Value of k for an adult is given below. K values for different ages can be found from ICRP (The International Commission on Radiological Protection) Publication 103 [9].
Relationship between Image Quality, Radiation Dose and Nose
Quality of CT image can be described by several metrics [4] (Table 1).
- Noise- describes the variation of CT numbers or Hounsfield units in a physically uniform region
- SNR (signal to noise ratio)
- CNR (contrast to noise ratio)
- Low kV will produce high contrast but increase radiation dose to the patient.
- Iodine has increase attenuation (CT contrast) at lower tube potential than at higher tube potential. Hence with lower kV superior enhancement occurs with the use of iodinated contrast media.
- Noise increases with lower kV. So, trade-off between noise and contrast enhancement is to be done.
- Iodine attenuation (CT number), image noise and contrast to noise ratio varies according to patient size. For small sized patient (children), noise levels remain almost the same with different kV. But with large sized patient (obese), noise is significantly higher and contrast to noise ratio is low at low kv.
- For noncontract CT, benefit of using lower kV is not established.
- Therefore, always uses an optimum tube potential (not necessarily lower) yielding best image quality considering all above factors. This optimal tube potential is dependent on patient size and specific diagnostic task.
- Avoid unnecessary CT examinations.
- Use alternative modalities like USG or MRI if necessary diagnostic information can be obtained from them
- Avoid multiphase examination (noncontrast, arterial, venous, delayed etc.) if information can be obtained from single-phase scan
- Use automatic exposure control (AEC), technique charts, child size bowtie filter, small field of view.
- optimum tube potential and lower tube current
- High helical pitch and fast rotation time for avoiding motion artefacts.
- Strategies
- Alternative non-radiation based imaging modality if possible and postponing scan until after deliver if not urgently required
- For appendicitis- USG is the best modality, avoid multiphase CT. Scan volume to be restricted to necessary anatomy [28]
- For detection of renal calculi- low mas, high pitch, limited scan range [29]
- For abdominopelvic CT- wider beam collimation, higher pitch, lower mAs, kV and scan range
- Strategie
- ECG based tube current modulation- it involves modulating tube current down to 4-20% of the full tube current for phases that are of minimal interest (i.e. during systole). The percentage of dose reduction is higher with slow and regular heart rates as R-R interval is higher at slow heart rate. Up to 64% dose reduction can be achieved without sacrificing image quality Hence use of β-blocker is indicated. It is not useful for irregular heart rate as it compromises image quality [30].
- Prospective ECG gating (step and shoot acquisitions) [31]: Here X-ray is turned on at the preselected phases during the cardiac cycle unlike retrospectively ECG -gated mode where the x-ray beam is continuously on.Due to lack of overlapping beams at lower spiral pitch, it is very dose efficient. But the disadvantage is it is more susceptible to deterioration of image quality due to motion artefacts and cine sequences (depicting heart motion) cannot be generated unlike from retrospectively ECG-gating data. It needs stable and low heart rate.
- Dual source CT scanners allow for a gapless acquisition with a pitch of up to 3.4 which cannot be achieved with conventional single-source CT scanners. High pitch and ECG based tube current modulation can decrease dose up to 50% as compared to 64 slice scanners [32].
- Use of cardiac bow-tie filter.
Simply put, as Radiation dose↑, noise↓, but image quality↑
The principle is that radiation dose should only be reduced under the condition that the diagnostic image quality is not compromised. The first task is to appropriately define the target image quality for specific Examination not requiring higher spatial resolution or lower noise.
Implication
In high contrast situation like in CT colonography where we want to detect polyps from a background of bowel gas and contrast-tagged stool, noise level can be allowed to remain high with reduction of dose without hampering diagnostic confidence [10,11]. Likewise, in low contrast situation as in CT scan of brain, liver or pancreas, noise must be low for detection and optimal characterisation of lesion [4]. The second task is to improve image quality i.e. to reduce image noise by optimising CT system, scanning techniques, improving image reconstruction and data processing [4].
General Strategies for Dose Reduction
Optimisation of CT system
Detector: Solid state detectors are now widely used instead of ionisation chamber detectors because of higher detective quantum efficiency (DQE) of the former. The DQE describes how effectively an x-ray imaging system can produce an image with a high signal-to-noise ratio (SNR) relative to an ideal detector. If a system DQE is increased, required radiation exposure to a patient can be decreased for the same image SNR and exposure conditions. Detectors with rapid response and low afterglow are desirable to allow faster scanning speed and high image quality with reduced dose [4,12].
Collimators: Pre patient collimator (between x ray source and patient) regulate size and shape of x-ray beam. Closely collimated beam leads to exposure of limited area avoiding unnecessary radiation dose to patient. Secondly, well collimated beam produce less scatter radiation, thus improving image quality [4,13].
Post patient collimators (between the patient and the detector) reject scatter radiation which improves image quality but sacrifices dose efficiency. Hence a trade-off is needed in designing scatter-rejection collimators [14].
X ray beam shaping filter: Filters are devices for absorbing low energy radiation which does not contribute to image formation, but gets absorbed by the patient. In other way, filters harden X ray beam (increase mean energy). Special shaped filters e.g. bow tie filters reduce the x-ray intensity in the peripheral region of body, thus reducing skin dose. Different types of filters for different applications are available now for example adult head, adult abdomen, and paediatric and cardiac filters [15,16]. It is important that patient be properly centred to avoid underexposure of central region and overexposure of peripheral region [17].
Scan range: Keep scan range as small as possible but as large as necessary.
Technique charts (Fixed tube current): It allows operators to select appropriate mAs (milliampere-second) as a function of patient size [18,19]. Since radiation dose increases with increase in mAs, it has to be kept low, but not as low to produce noise and degrade image quality. Since, tube potential (kV) is usually kept low for better contrast and exposure time (sec) is kept low for reducing motion artefacts, tube current (mA) is adapted to patient size. Children and small adult need lower mA as compared to larger patients. For obese patients tube current (mA), and the tube potential (kV) has to be increased for sufficient exposure.
Tube current (mA) modulation
Principle: since patient’s body is not uniform, there is large variation in absorption of x ray both with projection angle and anatomic region. Data acquired through body part having less attenuation can be acquired with substantially less radiation exposure and without negatively affecting image noise [3,4,20,21].
Angular (X,Y) mA modulation: it addresses the differences in attenuation around patient by modulating tube current as the x-ray tube rotates about the patient between AP and lateral projection.
Longitudinal (z) mA modulation: it addresses the variation in x ray attenuation along Z axis of patient (shoulder to abdomen for example) by varying mA.
Combined (both angular and longitudinal mA modulation): dose is adjusted according to patient attenuation in all three dimensions. (most comprehensive approach)
Automatic exposure control (AEC): It is an advanced technique currently available on scanners. Which adjusts tube current in real time in response to x ray intensity at the detector [22,23]. It can reduce dose up to 40%. It is vendor specific. e.g. General electric (GE) uses Auto Ma AND Siemens CARE Dose4D for AEC.
Optimal kV (tube potential)
Principle [3,4,24-26]:
Examination and Patient Specific Dose Reduction Strategies
Paediatric patients [25,27]: Risk of cancer is 2-3 times higher than adults
Pregnant patients: Usually CT scan is indicated for suspected appendicitis, pulmonary embolism and urinary tract calculi.
Cardiac CT: Cardiac CT has inherent high radiation dose because of use of relatively high mas and low pitch values for improving temporal and spatial resolution. Dose is proportional to mAs/pitch.
Cardiac CT: Cardiac CT has inherent high radiation dose because of use of relatively high mas and low pitch values for improving temporal and spatial resolution. Dose is proportional to mAs/pitch.
Dual Energy Ct [33,34]:
- There is no increase in radiation exposure when dualsource dual energy CT technology is used instead of singleenergy techniques.
- It allows creation of virtual non-contrast images from a post contrast DECT dataset, thus obviating the need for prior non-contrast scanning with substantial beneficial impact on the overall radiation dose associated with the exam. But image quality of virtual noncontract CT has high noise level.
- It is especially useful for patients who require frequent follow-up CT examinations. E.g. follow up of aortic stent grafting [35].
CT Perfusion
Radiation dose is usually higher than routine CT scan because of long scanning time. Special filtering techniques which reduce noise are HYPR-LR (highly constrained back projection local reconstruction) and MBF (multiband filtering) [36]. Animal model has shown tenfold dose reduction in renal perfusion CT (80 kV, 160mAs to 80 KV 16 mAs).
Interventional CT [37,38]:
- Optimising scanning technique in CT fluoroscopy (lowering kV, mA and exposure time, increasing slice thickness and limiting the scan range to only necessary anatomy).
- Intermittent or quick check mode than continuous mode.
- Proper shielding garments (lead apron, thyroid shield and leaded eyeglasses), needle holders to reduce direct exposure to hand.
- Shielding adjacent to the scanning plane (171) to reduce scatter radiation.
- With increased operator experience, exposure time gets reduced.
Future prospective
Iterative reconstruction: It improves image quality and reduces radiation dose in CT than conventional filtered back projection (FBP) techniques. It can reduce image artefacts such as beam hardening, windmill and metal artefacts. Iterative reconstruction is also superior to filtered back projection in handling insufficient data. It is expected that iterative reconstruction will be implemented into clinical practice in the near future [39].
Photon-counting detector: Current clinical CT scanners use “current mode” type of detector. Photon counting detectors/ pulse mode detectors are research interests [40]. These detectors count each photon and record its energy individually so that information can be detected and discriminated on a photon-by-photon basis. A dedicated photon-counting digital mammography system is already commercially available. It is expected to have photon counting-based clinical CT available soon.
Dynamic Bowtie Filter for Cone-Beam/Multi-Slice CT: It is largely a research interest. The attenuation profile it produces can be adaptively changed with the gantry rotation further reducing dose [41].
Selective In-plane Shielding [3,42,43]: Selective shielding of radiation sensitive tissues and organs such as eye lens, thyroid, or breasts can be done during brain, cervical spine, or chest CT scan respectively. Shields made of thin sheets of flexible latex impregnated with bismuth are used. For each organ, dose reduction is accompanied by increased noise and artefacts. The artefact on the reconstructed images can be minimized by keeping the distance between the shielding and the organs >1 cm. however, it has not come to wider practice.
Conclusion and Recommendation
Whatever CT dose reduction strategies are to be followed, ALARA (As Low as Reasonably Achievable) principle is a must. Considering tremendous benefit of CT scan and potential risk associated with it, a risk-benefit assessment should be done in each patient. Certain group of patients (e.g. pregnant, children) need special dose reduction strategies.
References
- Brenner DJ, Hall EJ (2007) Computed tomography-an increasing source of radiation exposure. N Engl J Med 357(22): 2277-2284.
- American College of Radiology, USA 2016.
- McCollough CH, Primak AN, Braun N, Kofler J, Yu L, et al. (2009) Strategies for reducing radiation dose in CT. Radiol. Clin. North Am. 47(1): 27-40.
- Lifeng Yu, Xin Liu, Shuai Leng, James M Kofler, Juan C Ramirez Giraldo (2009) Radiation dose reduction in computed tomography: techniques and future perspective. Imaging in medicine 1(1): 65-84.
- International Electrotechnical Commission (2002) Medical electrical equipment (Part 2-44): Particular requirements for the safety of x-ray equipment for computed tomography. IEC 60601-2-44: 2009.
- Jessen KA, Panzer W, Shrimpton, PC Tosi G (2000) EUR 16262: European Guidelines on Quality Criteria for Computed Tomography. Paper presented at: Office for Official Publications of the European Communities; Luxembourg.
- International Commission on Radiological Protection (1991) 1990 Recommendations of the International Commission on Radiological Protection (Report 60). Annals of the ICRP 21(1-3).
- Mc Collough CH, Schueler BA (2000) Calculation of effective dose. Med Phys 7(5): 828-837.
- International Commission on Radiological Protection (2007) Recommendations of the International Commission on Radiological Protection (ICRP Publication 103). Ann ICRP 37: 1-332.
- Fletcher JG, Johnson CD, Welch TJ, MacCarty RL, Ahlquist DA, et al. (2000) Optimization of CT colonography technique: prospective trial in 180 patients. Radiology 216: 704-711.
- Zueco Zueco C, Sobrido Sampedro C, Corroto JD, Rodriguez Fernandez P, Fontanillo Fontanillo M (2012) CT colonography without cathartic preparation: positive predictive value and patient experience in clinical practice. Eur Radiol 22(6): 1195-1204.
- Hsieh J (2006) Computed Tomography: Principles, Design, Artifacts, and Recent Advances. Bellingham, WA, SPIE Press, USA.
- Curry TS, Dowdey JE, Murry RC (1990) Christensen’s physics of diagnostic radiology. Lippincott Williams & Wilkins, USA.
- Siewerdsen JH, Jaffray DA (2000) Optimization of x-ray imaging geometry (with specific application to flat-panel cone-beam computed tomography). Med Phys 27(8)1903-1914.
- Thomas L Toth, Cesmelia E, Ikhlefa A, Horiuchib T (2005) Image quality and dose optimization using novel x-ray source filters tailored to patient si ze. Proc. Soc Photo Opt Instrum Eng 5745: 283-291.
- Zhang G, Marshall N, Jacobs R, Liu Q, Bosmans H (2013) Bowtie filtration for dedicated cone beam CT of the head and neck: a simulation study. The British Journal of Radiology 86(1028): 20130002.
- CT Physics: Dose Measurement in CT. Xray Physics 2017.
- Linton OW, Mettler FA (2003) Jr National conference on dose reduction in CT, with an emphasis on pediatric patients. Am J Roentgenol 181(2): 321-329.
- Food and Drug Administration (2002) FDA public health notification: reducing radiation risk from computed tomography for pediatric and small adult patients. Pediatr Radiol 32(4): 314-316.
- Greess H, Wolf H, Baum U, Lell M, Pirkl M, et al. (2000) Dose reduction in computed tomography by attenuation-based, on-line modulation of tube current: Evaluation of six anatomical regions. Eur Radiol 10(2): 391-394.
- McCollough CH, Bruesewitz MR, Kofler JM (2006) Jr CT dose reduction and dose management tools: overview of available options. Radiographics 26(2): 503-512.
- Gies M, Kalender WA, Wolf H, Suess C, Madsen M (1999) Dose reduction in CT by anatomically adapted tube current modulation: Simulation studies. Medical Physics 26(11): 2235-2247.
- Kalender WA, Wolf H, Suess C (1999) Dose reduction in CT by anatomically adapted tube current modulation: Phantom measurements. Med Phys 26(11): 2248-2253.
- Huda W, Scalzetti EM, Levin G (2000) Technique factors and image quality as functions of patient weight at abdominal CT. Radiology 217(2): 430-435.
- Boone JM, Geraghty EM, Seibert JA, Wootton-Gorges SL (2003) Dose reduction in pediatric CT: a rational approach. Radiology 228: 352-360.
- Siegel MJ, Schmidt B, Bradley D, Suess C, Hildebolt C (2004) Radiation dose and image quality in pediatric CT: effect of technical factors and phantom size and shape. Radiology 233(2): 515-522.
- Paterson A, Frush DP (2007) Dose reduction in paediatric MDCT: general principles. Clin Radiol 62(6): 507-517.
- Wagner LK, Huda W (2004) When a pregnant woman with suspected appendicitis is referred for a CT scan, what should a radiologist do to minimize potential radiation risks? Pediatric Radiology. 34(7): 589- 590.
- Forsted DHv (2000) CT of pregnant women for urinary tract calculi, pulmonary thromboembolism, and acute appendicitis. Am J Roentgenol 178(5): 1285.
- Jakobs TF, Becker CR, Ohnesorge B, Flohr T, Suess C et al. (2002) Multislice helical CT of the heart with retrospective ECG gating: reduction of radiation exposure by ECG-controlled tube current modulation. Eur Radiol 12(5): 1081-1086.
- Hsieh J, Londt J, Vass M, Li J, Tang X, et al. (2006) Step-and-shoot data acquisition and reconstruction for cardiac x-ray computed tomography. Med Phys 33(11): 4236-4248.
- McCollough CH, B Schmidt, L Yu, A Primak, S Ulzheimer, et al. (2008) Dose performance of a 64-channel dual-source CT scanner. Radiology 35(2): 764-768.
- Johnson TR, Krauss B, Sedlmair M, Grasruck M, Bruder H, et al. (2007) Material differentiation by dual energy CT: initial experience. Eur Radiol 17(6): 1510-1517.
- Fletcher JG, Takahashi N, Hartman R, Guimaraes L, Huprich JE, et al. (2009) Dual-energy and dual-source CT: is there a role in the abdomen and pelvis? Radiol. Clin North Am 47(1): 41-57.
- Laks S, Macari M, Chandarana H (2010) Dual-energy computed tomography imaging of the aorta after endovascular repair of abdominal aortic aneurysm. Semin Ultrasound CT MR 31(4): 292-300.
- Mistretta CA, Wieben O, Velikina J, Block W, Perry J, et al. (2006) Highly constrained backprojection for time-resolved MRI. Magn Reson Med 55(1): 30-40.
- Daly B, Krebs TL, Wong-You-Cheong JJ, Wang SS (1999) Percutaneous abdominal and pelvic interventional procedures using CT fluoroscopy guidance. AJR Am J Roentgenol 173(3): 637-644.
- Paulson EK, Sheafor DH, Enterline DS, McAdams HP, Yoshizumi TT (2001) CT fluoroscopy - guided interventional procedures: techniques and radiation dose to radiologists. Radiology 220(1): 161-167.
- Nuyts J, De Man B, Dupont P, Defrise M, Suetens P,et al (1998) Iterative reconstruction for helical CT: a simulation study. Phys Med Biol 43(4): 729-737.
- Lundqvist M, Cederstrom B, Chmill V, Danielsson M, Hasegawa B (2001) Evaluation of a photon-counting x-ray imaging system. IEE Trans. Nucl Sci 48(4): 1530-1536.
- Liu F, Yang Q, Cong W, Wang Gn (2014) Dynamic Bowtie Filter for Cone-Beam/Multi-Slice CT. Tian J, ed PLoS ONE 9(7): e103054.
- McLaughlin DJ, Mooney RB (2009) Dose reduction to radiosensitive tissues in CT. Do commercially available shields meet the users’ needs? Clin Radiol 59(5): 446-450.
- Chang K-H, Lee W, Choo DM, Lee CS, Kim Y (2010) Dose reduction in CT using bismuth shielding: measurements and Monte Carlo simulations. Radiation Protection Dosimetry 138(4): 382-388.






























