Ceramic Biomaterials in Dentistry: Review
Angelo Michele Inchingolo, Laura Ferrante, Alessio Danilo Inchingolo, Gianna Dipalma1* and Francesco Inchingolo1*
1Department of Interdisciplinary Medicine, University of Bari “Aldo Moro”, 70124 Bari, Italy
Submission:February 02, 2024; Published:March 04, 2024
*Corresponding author:Francesco Inchingolo, Department of Interdisciplinary Medicine, University of Bari “Aldo Moro”, 70124 Bari, Italy
How to cite this article:Angelo M I, Laura F, Alessio Danilo I, Gianna D, Francesco I. Ceramic Biomaterials in Dentistry: Review. Curr Trends Biomedical Eng & Biosci. 2024; 22(3): 556089. DOI:10.19080/CTBEB.2024.22.556089
Abstract
Recent years have seen significant advancements in the field of materials science, accompanied by progress in analytical techniques and the discovery of new control devices and materials. These advancements have paved the way for the development of innovative approaches for raw material selection, with particular attention to creating advanced materials with specific physical and chemical properties tailored to meet desired criteria. This growing demand is particularly pronounced in environments with complex conditions, such as biological environments like the oral cavity. Consequently, there is a pressing need to identify and design materials that meet rigorous standards capable of withstanding such demanding environments. In the search for materials suitable for these applications, the need for advanced additives or biomaterials arises, which not only possess specific physicochemical attributes but also emulate biological materials, such as teeth, once integrated into biological systems. These biomaterials, spanning a wide range from metals, alloys, and polymers to glasses (bioglass), carbon fiber composites, and biological materials, interface with biological systems such as tissues and human fluids. However, it is essential to emphasize that biomaterials, while in contact with biological entities, differ from pharmaceutical materials. Therefore, they must exhibit biocompatibility, bioabsorbability, or inertness, depending on the intended applications. Unlike traditional inert materials, biomaterials are closely linked to the biological environment. Their surfaces can be customized to mimic organic structures they replace, ensuring optimal adhesion to tissues or skeletal structures. Moreover, they must not only interact harmoniously with organic molecules but also avoid eliciting toxic responses similar to those of xenobiotics. Therefore, interdisciplinary definitions such as biocompatibility, bioabsorbability, and toxicity, along with bioethical considerations, are indispensable for delineating the suitability of various materials in medical contexts.
Keywords:Biomaterials; Ceramics; Dental materials; Biological environment; Xenobiotics; Polycrystalline; Orthophosphates; Microstructure; Biomaterials science; Pharmaceutical
Introduction
In recent years, the field of biomaterials, particularly ceramic-based biomaterials, has witnessed a significant surge in interest and research activity, driven by their remarkable properties and promising applications across various biomedical domains, prominently including dentistry [1-5]. Ceramic materials, characterized by their exceptional attributes such as high temperature resistance, lightweight nature, impressive hardness, and corrosion resistance, stand out as highly desirable materials for a diverse array of applications within the biomedical field [6-11]. Among the spectrum of ceramic materials, dental ceramics hold a pivotal position, primarily due to their ability to offer not only functional advantages but also aesthetic appeal [12-17]. Dental ceramics are engineered to exhibit improved mechanical properties while maintaining a visually pleasing appearance, making them indispensable in restorative and prosthetic dentistry [18-21]. These materials are meticulously designed to seamlessly integrate with natural dental structures, providing patients with both functional and cosmetic benefits [22-25]. The realm of ceramic biomaterials includes various subtypes such as glass-based ceramics, low-glass ceramics, and polycrystalline ceramics [26-29]. Each subtype offers distinct advantages and applications in the field of dentistry and beyond [30-33]. Glass-based ceramics, renowned for their aesthetic appeal and biocompatibility, find widespread use in dental restorations where both functionality and appearance are paramount [34-37]. Low-glass ceramics, on the other hand, are engineered to possess enhanced mechanical properties, catering to applications that demand superior strength and durability [38-43]. Polycrystalline ceramics, characterized by their formidable mechanical strength and resistance to fracture, are favored in dental prosthetics where longevity and reliability are critical [9,44-46]. Furthermore, the emergence of porous bioceramics has opened new avenues in the fields of tissue engineering and regenerative medicine [43,47-49]. Mimicking the microstructure of natural materials like coral, porous bioceramics facilitate tissue growth and integration, offering promising solutions for repairing and regenerating damaged or lost tissues [50-53]. Various manufacturing techniques, including foaming and impurity-induced porosity, enable the customization of porous bioceramics to meet specific application requirements, further enhancing their utility in biomedical settings [50,54-56]. Despite the myriad advantages offered by ceramic biomaterials, they are not without challenges. Intrinsic fragility poses a significant concern, necessitating meticulous consideration of fracture toughness and brittleness in material design and application [57,53,58,59]. Strategies aimed at mitigating fragility, such as the development of high-strength base materials and optimization of manufacturing processes to minimize defects, are essential for enhancing the reliability and performance of ceramic biomaterials[51,60-63]. By exploring the diverse landscape of ceramic biomaterials and addressing challenges associated with their utilization, this paper aims to contribute to the advancement of biomaterials science and pave the way for innovative solutions in healthcare and beyond [64-68].
Discussion
Research on biomaterials, especially those intended for integration into biological systems such as teeth and tissues, requires the adoption of advanced additives or biomaterials that not only possess specific physicochemical attributes but also emulate biological materials once integrated into biological systems [69-72]. These materials, which range from metals, alloys and polymers to glasses (bioglass), carbon fiber composites and biological materials, must interface with biological systems such as human tissues and fluids [73-75]. Crucially, despite their contact with biological entities, biomaterials differ from pharmaceutical materials and must exhibit biocompatibility, bioabsorbability or be inert, depending on their intended applications [76- 79]. Ceramic materials, characterized by properties such as temperature resistance, low weight, hardness, and corrosion, have applications in various fields, including electronics and hightemperature environments [80-83]. Among these, bioceramics, particularly dental ceramics, play a key role, offering aesthetic advantages and improved mechanical properties [19,26,84,85]. Dental ceramics include several categories, such as glass-based ceramics, low-glass ceramics, and polycrystalline ceramics, each with specific characteristics that make them suitable for certain applications [86-89]. Glass-based ceramics, renowned for their aesthetic appeal, are composed mainly of silicon dioxide and are ideal for applications requiring superior aesthetic properties [81,90-94]. Low-glass ceramics, on the other hand, offer improved mechanical properties due to a reinforcing phase based on the SiO2-Li2O system [92,95-98]. Finally, polycrystalline ceramics such as zirconium oxide, characterized by exceptional flexural strengths, find applications in dental restorations due to their distinctive mechanical properties [99-102]. In addition to traditional ceramics, porous bioceramics have attracted attention for their potential in tissue engineering and regenerative medicine (Figure1) [103-105].
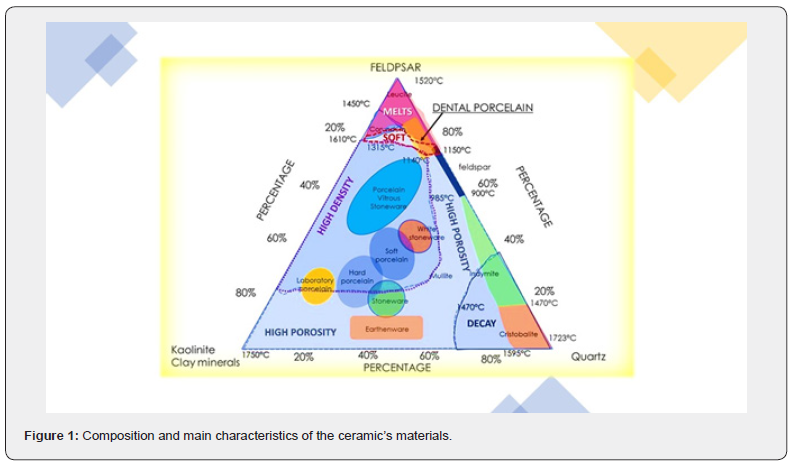
These materials, inspired by the microstructure of natural materials such as coral, facilitate tissue growth and promote biological integration [106-109]. However, the inherent brittleness of ceramics makes them susceptible to brittle fracture under tensile loads, requiring careful consideration of fracture toughness in material design [67,110-112]. Strategies to mitigate brittleness include developing high-strength materials and optimizing manufacturing processes to minimize defects. In the dental context, ceramic materials such as alumina and zirconia are used for dental restorations because of their mechanical properties and biocompatibility [113-117]. The use of bioabsorbable bioceramics such as calcium orthophosphates is aimed at replacing hard tissue with autologous tissue over time, improving biological integration of implants [118-122]. However, research continues to evaluate the risk and prevention of infectious complications in dental materials, with a focus on antimicrobial upgrades to address bacterial and viral resistance [3,68,123-125]. Research on ceramic biomaterials continues to advance, with efforts aimed at improving mechanical properties, biocompatibility, and clinical efficacy [126-130]. Interdisciplinary approaches and innovative fabrication techniques are crucial to unlocking the full potential of ceramics in a wide range of biomedical applications, from dental restoration to tissue engineering [1,131-134].
Conclusion
In conclusion, ceramic biomaterials continue to evolve, driven by ongoing research aimed at improving their mechanical properties, biocompatibility, and clinical efficacy. By leveraging interdisciplinary approaches and innovative manufacturing techniques, researchers seek to unlock the full potential of ceramics in various biomedical applications, ranging from dental restorations to tissue engineering scaffolds. Ceramicbased substitutes for hard tissue repair, bioactive bioceramics, and bioabsorbable ceramics represent promising avenues for future research and development. Moreover, advancements in antimicrobial ceramics offer new possibilities for preventing infectious complications in dental implants and other biomedical devices. Overall, ceramic biomaterials hold immense promise for advancing healthcare and enhancing patient outcomes in the years to come.
References
- Vaiani L, Boccaccio A, Uva AE, Palumbo G, Piccininni A, et al. (2023) Ceramic Materials for Biomedical Applications: An Overview on Properties and Fabrication Processes. J Funct Biomater 14(3): 146.
- Dipalma G, Inchingolo AD, Inchingolo AM, Piras F, Carpentiere V, et al. (2023) Artificial Intelligence and Its Clinical Applications in Orthodontics: A Systematic Review. Diagnostics 13(24): 3677.
- Ramburrun P, Pringle NA, Dube A, Adam RZ, D Souza S, et al. (2021)Recent Advances in the Development of Antimicrobial and Antifouling Biocompatible Materials for Dental Applications. Materials (Basel) 14(12): 3167.
- Zhang K, Wang S, Zhou C, Cheng L, Gao X, et al. (2018) Advanced Smart Biomaterials and Constructs for Hard Tissue Engineering and Regeneration. Bone Res 6: 1-15.
- de León EHP, Valle-Pérez AU, Khan ZN, Hauser CAE (2023) Intelligent and Smart Biomaterials for Sustainable 3D Printing Applications. Current Opinion in Biomedical Engineering 26: 100450.
- Several ceramic materials are commonly used for the ceramic PCB Available online: (accessed on 18 February 2024).
- Silva LHda, Lima E de, Miranda RB de P, Favero SS, Lohbauer U, et al. (2017) Dental Ceramics: A Review of New Materials and Processing Methods. Braz Oral Res 31: e58.
- Klawitter JJ, Weinstein AM, Cooke FW, Peterson LJ, Pennel BM, et al. (1977) An Evaluation of Porous Alumina Ceramic Dental Implants. J Dent Res 56(7): 768-776.
- Materials | Free Full-Text | A Narrative Review on Polycrystalline Ceramics for Dental Applications and Proposed Update of a Classification System.
- Zhao LH, Wang L, Jin YF, Ren JW, Wang Z, et al. (2021) Simultaneously Improved Thermal Conductivity and Mechanical Properties of Boron Nitride Nanosheets/Aramid Nanofiber Films by Constructing Multilayer Gradient Structure. Composites Part B: Engineering 229: 109454.
- Weiss P (2010) Renewal ACS Nano.
- Meskin A, Robson J, Ichino A, Goffin K, Monseré A (2018) Philosophical Aesthetics and Cognitive Science. WIRES Cognitive Science 9(1): e1445.
- Bajraktarova-Valjakova E, Korunoska-Stevkovska V, Kapusevska B, Gigovski N, Bajraktarova-Misevska C, et al. (2018) Contemporary Dental Ceramic Materials, A Review: Chemical Composition, Physical and Mechanical Properties, Indications for Use. Open Access Maced J Med Sci 6(9): 1742-1755.
- Kim BS, Baez CE, Atala A(2000) Biomaterials for Tissue Engineering. World J Urol 18(1): 2-9.
- Fiume E, Barberi J, Verné E, Baino F (2018) Bioactive Glasses: From Parent 45S5 Composition to Scaffold-Assisted Tissue-Healing Therapies. J Funct Biomater 9(1): 24.
- Fu Q, Saiz E, Rahaman N, Tomsia A (2011) Bioactive Glass Scaffolds for Bone Tissue Engineering: State of the Art and Future Perspectives. Materials science & engineering. C, Materials for biological applications 31(7): 1245-1256.
- Moore WR, Graves SE, Bain GI(2001) Synthetic Bone Graft Substitutes. ANZ J Surg 71(6): 354-361.
- Pereira RM, Ribas RG, Montanheiro TL Do A, Schatkoski VM, Rodrigues KF, et al.(2023) An Engineering Perspective of Ceramics Applied in Dental Reconstructions. J Appl Oral Sci 31: e20220421.
- Wang G, Wang S, Dong X, Zhang Y, Shen W(2023) Recent Progress in Additive Manufacturing of Ceramic Dental Restorations. Journal of Materials Research and Technology 26: 1028-1049.
- Temporomandibular Joint Disk Displacement: Etiology, Diagnosis, Imaging, and Therapeutic Approaches - PubMed (accessed on 18 February 2024).
- Datta LP, Manchineella S, Govindaraju T(2020) Biomolecules-Derived Biomaterials. Biomaterials 230: 119633.
- Elevating Cosmetic Dental Transformations: The Magic of Dental Ceramics | Cromwell Dentists | Fedorciw, Massoumi & Kolbig 2023.
- User S. Aesthetic Filling Systems Available online: (accessed on 18 February 2024).
- GYA The Transformative Power of Dental Implants. Creative Dental Haus 2023.
- Schlickewei W, Schlickewei C (2007) The Use of Bone Substitutes in the Treatment of Bone Defects - the Clinical View and History. Macromolecular Symposia 253: 10-23.
- Punj S, Singh J, Singh K (2021) Ceramic Biomaterials: Properties, State of the Art and Future Prospectives. Ceramics International 47.
- Materials | Free Full-Text | Bioactive Glasses and Glass-Ceramics for Healthcare Applications in Bone Regeneration and Tissue Engineering.
- Crescente G, Minervini G, Spagnuolo C, Moccia S (2023) Cannabis Bioactive Compound-Based Formulations: New Perspectives for the Management of Orofacial Pain. Molecules 28(1): 106.
- Inchingolo F, Tatullo M, Abenavoli FM, Marrelli M, Inchingolo AD, et al. (2011) Non-Hodgkin Lymphoma Affecting the Tongue: Unusual Intra-Oral Location. Head & Neck Oncology 3: 1.
- Zhao R, Yang R, Cooper PR, Khurshid Z, Shavandi A, et al. (2021) Bone Grafts and Substitutes in Dentistry: A Review of Current Trends and Developments. Molecules 26(10): 3007.
- Rathi S, Chaturvedi S, Abdullah S, Rajput G, Alqahtani NM, et al. (2023) Clinical Trial to Assess Physiology and Activity of Masticatory Muscles of Complete Denture Wearer Following Vitamin D Intervention. Medicina 59(2): 410.
- Stem Cells in Temporomandibular Joint Engineering: State of Art and Future Persectives – PubMed.
- Anusavice KJ (1992) Degradability of Dental Ceramics. Adv Dent Res 6: 82-89.
- Fu L, Engqvist H, Xia W (2020) Glass-Ceramics in Dentistry: A Review. Materials (Basel) 13(5): 1049.
- Biocompatible Materials in Restorative Dentistry: Innovations and Applications - Unicorn DenMart - Top Dental Equipment Supplier in India.
- Dohan Ehrenfest DM, Del Corso M, Inchingolo F, Sammartino G, Charrier JB (2010) Platelet-Rich Plasma (PRP) and Platelet-Rich Fibrin (PRF) in Human Cell Cultures: Growth Factor Release and Contradictory Results. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 110(4): 418-421.
- Marín Fermín T, Calcei JG, Della Vedova F, Martinez Cano JP, Arias Calderon C, et al. (2009) Classification of Platelet Concentrates: From Pure Platelet-Rich Plasma (P-PRP) to Leucocyte- and Platelet-Rich Fibrin (L-PRF). Journal of ISAKOS .
- Furszyfer Del Rio DD, Sovacool BK, Foley AM, Griffiths S, Bazilian M, et al. (2022) Decarbonizing the Ceramics Industry: A Systematic and Critical Review of Policy Options, Developments and Sociotechnical Systems. Renewable and Sustainable Energy Reviews 157: 112081.
- Khater GA, Safwat E, Kang J, Yue Y, Khater A (2020) Some Types of Glass-Ceramic Materials and Their Applications. International Journal of Research 7: 1-16.
- Akinribide OJ, Mekgwe GN, Akinwamide SO, Gamaoun F, Abeykoon C, et al. (2022) A Review on Optical Properties and Application of Transparent Ceramics. Journal of Materials Research and Technology 21: 712-738.
- Development of Glass & Glass Ceramics for Engineering Applications | Frontiers Research Topic Available online: (accessed on 18 February 2024).
- Farronato M, Farronato D, Giannì AB Inchingolo F, Nucci L, et al. (2022) Effects on Muscular Activity after Surgically Assisted Rapid Palatal Expansion: A Prospective Observational Study. Bioengineering 9(8): 361.
- Marrelli M, Tatullo M, Dipalma G, Inchingolo F (2012) Oral Infection by Staphylococcus Aureus in Patients Affected by White Sponge Nevus: A Description of Two Cases Occurred in the Same Family. Int J Med Sci 9(1): 47-50.
- Zarone F, Di Mauro MI, Ausiello P, Ruggiero G, Sorrentino R (2019) Current Status on Lithium Disilicate and Zirconia: A Narrative Review. BMC Oral Health 19(1): 134.
- Apel E, Deubener J, Bernard A, Höland M, Müller R, et al. (2008) Phenomena and Mechanisms of Crack Propagation in Glass-Ceramics. J Mech Behav Biomed Mater 1(4): 313-325.
- Malcangi G, Inchingolo AD, Inchingolo AM, Piras F, Settanni V, et al. (2022) COVID-19 Infection in Children and Infants: Current Status on Therapies and Vaccines. Children (Basel) 9(2): 249.
- Bioceramic - an Overview | ScienceDirect Topics.
- Rafieerad AR, Bushroa AR, Nasiri-Tabrizi B, Vadivelu J, Yusof F, et al. (2017) Graphene Oxide Modified Anodic Ternary Nanobioceramics on Ti6Al7Nb Alloy for Orthopedic and Dental Applications. Procedia Engineering 184: 409-417.
- Oralbiotica/Oralbiotics: The Impact of Oral Microbiota on Dental Health and Demineralization: A Systematic Review of the Literature – PMC.
- Baino F, Ferraris M (2017) Learning from Nature: Using Bioinspired Approaches and Natural Materials to Make Porous Bioceramics. International Journal of Applied Ceramic Technology 14.
- Mimicking Natural Bio-Mineralization Processes: A New Tool for Osteochondral Scaffold Development – PubMed.
- Anil S, Sweety VK, Joseph B(2023) Marine-Derived Hydroxyapatite for Tissue Engineering Strategies. In: Maia FRA, Oliveira JM, Reis RL (Eds.), Handbook of the Extracellular Matrix: Biologically-Derived Materials. Springer International Publishing: Cham pp.1-26.
- Baino F, Fiume E, Miola M, Vernè E (2018) Bioactive Sol-Gel Glasses: Processing, Properties, and Applications. International Journal of Applied Ceramic Technology 15.
- Miri Z, Haugen HJ, Loca D, Rossi F, Perale G, et al. (2024) Review on the Strategies to Improve the Mechanical Strength of Highly Porous Bone Bioceramic Scaffolds. Journal of the European Ceramic Society 44: 23-42.
- Innovative Concepts and Recent Breakthrough for Engineered Graft and Constructs for Bone Regeneration: A Literature Systematic Review – PMC.
- Di Domenico M, Feola A, Ambrosio P, Pinto F, Galasso G, et al. (2020) Antioxidant Effect of Beer Polyphenols and Their Bioavailability in Dental-Derived Stem Cells (D-dSCs) and Human Intestinal Epithelial Lines (Caco-2) Cells. Stem Cells Int 8835813.
- Chiari MDS, Rodrigues MC, Pinto MFC, Vieira DN, Vichi FM, et al. (2020) Development of Brushite Particles Synthesized in the Presence of Acidic Monomers for Dental Applications. Mater Sci Eng C Mater Biol Appl 116: 111178.
- Zhong J, Greenspan DC (2000) Processing and Properties of Sol-Gel Bioactive Glasses. J Biomed Mater Res 53(6): 694-701.
- Fiume E, Migneco C, Verné E, Baino F (2020) Comparison between Bioactive Sol-Gel and Melt-Derived Glasses/Glass-Ceramics Based on the Multicomponent SiO2–P2O5–CaO–MgO–Na2O–K2O System. Materials 13(3): 540.
- Li Q, Feng C, Cao Q, Wang W, Ma Z, et al. (2023) Strategies of Strengthening Mechanical Properties in the Osteoinductive Calcium Phosphate Bioceramics. Regen Biomater 10: rbad013.
- Örlygsson G, Harbrecht B(1999) Synthesis and Crystal Structure of Zr 2 Te. Distinctions in Bonding to Isotypic Sc 2 Te and the Relationship to the Structures of Congeneric Hf 2 Te and Zr 2 Se. Inorg. Chem 38(14): 3377-3383.
- Czenek A, Blanchard R, Dejaco A, Sigurjónsson ÓE, Örlygsson G, et al. (2014) Quantitative Intravoxel Analysis of Microct-Scanned Resorbing Ceramic Biomaterials–Perspectives for Computer-Aided Biomaterial Design. Journal of Materials Research 29: 2757-2772.
- Riccucci G, Ferraris S, Reggio C, Bosso A, Örlygsson G, et al. (2021) Polyphenols from Grape Pomace: Functionalization of Chitosan-Coated Hydroxyapatite for Modulated Swelling and Release of Polyphenols. Langmuir 37(51): 14793-14804.
- Hazballa D, Inchingolo A, Inchingolo AM, Malcangi G, Santacroce L, et al. (2021) The Effectiveness of Autologous Demineralized Tooth Graft for the Bone Ridge Preservation: A Systematic Review of the Literature. Journal of biological regulators and homeostatic agents 35: 283-294.
- Burtscher S, Krieg P, Killinger A, Al-Ahmad A, Seidenstücker M,et al. (2019) Thin Degradable Coatings for Optimization of Osteointegration Associated with Simultaneous Infection Prophylaxis. Materials (Basel) 12(21): 3495.
- Nutrients | Free Full-Text | Effects of Resveratrol, Curcumin and Quercetin Supplementation on Bone Metabolism— A Systematic Review.
- Bai R, Sun Q, He Y, Peng L, Zhang Y, et al. (2022) Ceramic Toughening Strategies for Biomedical Applications. Frontiers in Bioengineering and Biotechnology 10.
- Cantore S, Mirgaldi R, Ballini A, Coscia MF, Scacco S, et al. (2014)Cytokine Gene Polymorphisms Associate with Microbiogical Agents in Periodontal Disease: Our Experience. Int J Med Sci 11(7): 674-679.
- Advancing Biomaterials of Human Origin for Tissue Engineering – PMC.
- Chen PY, Lopez M, Seki Y, Lin A (2011) Biological Materials: A Materials Science Approach. Journal of the mechanical behavior of biomedical materials 4: 626-657.
- Bio-Inspired Nanomaterials for Micro/Nanodevices: A New Era in Biomedical Applications – PMC.
- Inchingolo AD, Inchingolo AM, Bordea IR, Xhajanka E, Romeo DM,et al. (2021) The Effectiveness of Osseodensification Drilling Protocol for Implant Site Osteotomy: A Systematic Review of the Literature and Meta-Analysis. Materials (Basel) 14(5): 1147.
- Cannio M, Bellucci D, Roether JA, Boccaccini DinoN, Cannillo V (2021) Bioactive Glass Applications: A Literature Review of Human Clinical Trials. Materials (Basel) 14(18): 5440.
- Krishani M, Shin WY, Suhaimi H, Sambudi NS (2023) Development of Scaffolds from Bio-Based Natural Materials for Tissue Regeneration Applications: A Review. Gels 9(2): 100.
- Dipalma G, Inchingolo AD, Piras F, Palmieri G, Pede CD, et al. (2023) Efficacy of Guided Autofluorescence Laser Therapy in MRONJ: A Systematic Review. Eur Rev Med Pharmacol Sci 27(24): 11817-11831.
- Biomaterials in Orthopaedics – PMC.
- Bonferoni MC, Caramella C, Catenacci L, Conti B, Dorati R, et al. (2021) Biomaterials for Soft Tissue Repair and Regeneration: A Focus on Italian Research in the Field. Pharmaceutics 13(9): 1341.
- Schanze KS, Whitten DG, Kell AM, Chi EY, Ista LK, et al. (2020) Highly Effective Inactivation of SARS-CoV-2 by Conjugated Polymers and Oligomers. medRxiv 20204164.
- Inchingolo F, Ballini A, Cagiano R, Inchingolo AD, Serafini M, et al. (2015) Immediately Loaded Dental Implants Bioactivated with Platelet-Rich Plasma (PRP) Placed in Maxillary and Mandibular Region. Clin Ter 166(3): e146-152.
- Piconi C, Maccauro G (1999) Zirconia as a Ceramic Biomaterial. Biomaterials 20(1): 1-25.
- Belmonte M (2006) Advanced Ceramic Materials for High Temperature Applications. Advanced Engineering Materials 8(8): 693-703.
- Subramanian N, Pattanaik P, Mishra A, Dharshini D (2023) Review Study on Mechanical and Thermal Properties of Ceramic Materials for Future Aerospace Applications 01: 107-113.
- Inchingolo AM, Malcangi G, Ferrante L, Del Vecchio G, Viapiano F, et al. (2023)Surface Coatings of Dental Implants: A Review. J Funct Biomater 14(5): 287.
- Hland W, Schweiger M, Rheinberger V, Kappert H (2009) Bioceramics and Their Application for Dental Restoration. Advances in Applied Ceramics 108: 373-380.
- Inchingolo AD, Patano A, Coloccia G, Ceci S, Inchingolo AM, et al. (2021) Genetic Pattern, Orthodontic and Surgical Management of Multiple Supplementary Impacted Teeth in a Rare, Cleidocranial Dysplasia Patient: A Case Report. Medicina (Kaunas) 57(12): 1350.
- Shi HY, Pang R, Yang J, Fan D, Ca H, et al. (2022) Overview of Several Typical Ceramic Materials for Restorative Dentistry. Biomed Res Int 8451445.
- Inchingolo F, Ballini A, Mura SA, Farronato D, Cirulli N, et al. (2015) Use of Platelet Rich Fibrin and Bio-OSS/SINT-Oss for Implant-Prosthetic Rehabilitation in Maxillary Atrophy with Sinus Pathology: A 48-Month Follow-up.
- Ho G, Matinlinna J (2011) Insights on Ceramics as Dental Materials. Part I: Ceramic Material Types in Dentistry. Silicon 3: 109-115
- Giordano R, McLaren EA (2010)Ceramics Overview: Classification by Microstructure and Processing Methods 31(9): 682-684.
- Fraser R, Girtan M (2023) A Selective Review of Ceramic, Glass and Glass-Ceramic Protective Coatings: General Properties and Specific Characteristics for Solar Cell Applications. Materials 16(11): 3906.
- Suri L, Taneja P (2008) Surgically Assisted Rapid Palatal Expansion: A Literature Review. Am J Orthod Dentofacial Orthop 133(2): 290-302.
- Manicone PF, Rossi Iommetti P, Raffaelli L(2007) An Overview of Zirconia Ceramics: Basic Properties and Clinical Applications. Journal of Dentistry 35(11): 819-826.
- Cao W, Hench LL(1996) Bioactive Materials. Ceramics International 22:493-507.
- Sepulveda P, Jones JR, Hench LL(2001) Characterization of Melt-Derived 45S5 and Sol-Gel-Derived 58S Bioactive Glasses. J Biomed Mater Res 58(6): 734-740.
- Maeda K, Akatsuka K, Yasumori A (2021) Practical Strength of Damage-Resistant CaO–Al2O3–SiO2 Glass-Ceramic. Ceramics International 47: 8728-8731.
- Scarano A, Inchingolo F, Lorusso F(2020) Facial Skin Temperature and Discomfort When Wearing Protective Face Masks: Thermal Infrared Imaging Evaluation and Hands Moving the Mask. Int J Environ Res Public Health 17(13): 4624.
- Zhao T, Lian MM, Qin Y, Zhu JF, Kong XG, et al.(2021)Improved Performances of Lithium Disilicate Glass-Ceramics by Seed Induced Crystallization. J Adv Ceram 10: 614-626.
- Vermesan D, Prejbeanu R, Poenaru DV, Petrescu H, Apostol E,et al. (2015) Do Intramedullary Implants Improve Survival in Elderly Patients with Trochanteric Fractures? A Retrospective Study. Clin Ter 166(3): e140-145.
- Review on Synthesis, Properties and Multifarious Therapeutic Applications of Nanostructured Zirconia in Dentistry – PMC.
- Denry I, Kelly J (2008) State of The Art of Zirconia for Dental Applications. Dental materials : official publication of the Academy of Dental Materials 24(3): 299-
- Seghi RR, Daher T, Caputo A (1990) Relative Flexural Strength of Dental Restorative Ceramics. Dent Mater 6(3): 181-184.
- Sepulveda P, Jones JR, Hench LL(2002) In Vitro Dissolution of Melt-Derived 45S5 and Sol-Gel Derived 58S Bioactive Glasses. J Biomed Mater Res 61(2): 301-311.
- Baino F, Novajra G, Vitale BC (2015) Bioceramics and Scaffolds: A Winning Combination for Tissue Engineering. Front Bioeng Biotechnol 3: 202.
- 3D-Printed Bioceramic Scaffolds: From Bone Tissue Engineering to Tumor Therapy - ScienceDirect Available online:(accessed on 18 February 2024).
- Barberi J, Baino F, Fiume E, Orlygsson G, Nommeots-Nomm A, et al. (2019) Robocasting of SiO2-Based Bioactive Glass Scaffolds with Porosity Gradient for Bone Regeneration and Potential Load-Bearing Applications. Materials (Basel) 12(17): 2691.
- Levy N, Berman O, Yuval M, Loya Y, Treibitz T, (2022) Emerging 3D Technologies for Future Reformation of Coral Reefs: Enhancing Biodiversity Using Biomimetic Structures Based on Designs by Nature. Science of The Total Environment 830: 154749.
- Bernardi S, Mummolo S, Ciavarelli LM, Li Vigni M, Continenza MA, et al. (2016) Cone Beam Computed Tomography Investigation of the Antral Artery Anastomosis in a Population of Central Italy. Folia Morphol (Warsz) 75(2): 149-153.
- Ben-Nissan B, Choi A, Green D (2019) Marine Derived Biomaterials for Bone Regeneration and Tissue Engineering: Learning from Nature In pp51-78.
- Zhong J, Huang W, Zhou H (2023) Multifunctionality in Nature: Structure–Function Relationships in Biological Materials. Biomimetics 8(3): 284.
- Brittle Fracture Mechanism - an Overview | ScienceDirect Topics Available online:(accessed on 18 February 2024).
- Inchingolo F, Santacroce L, Cantore S, Ballini A, Del Prete R, et al. (2019)Probiotics and EpiCor® in Human Health. J Biol Regul Homeost Agents 33(6): 1973-1979.
- Andersson M, Razzoog ME, Odén A, Hegenbarth EA, Lang BR (1998) Procera: A New Way to Achieve an All-Ceramic Crown. Quintessence Int 29(5): 285-296.
- Themes, U.F.O. Dental Materials in the Digital Age.
- Additive Manufacturing (3D Printing): A Review of Materials, Methods, Applications and Challenges – ScienceDirect.
- New Implant Design with Midcrestal and Apical Wing Thread for Increased Implant Stability in Single Postextraction Maxillary Implant – PubMed.
- Guazzato M, Albakry M, Ringer SP, Swain MV (2004) Strength, Fracture Toughness and Microstructure of a Selection of All-Ceramic Materials. Part II. Zirconia-Based Dental Ceramics. Dent Mater 20(5): 449-456.
- Kovziridze Z, Nizharadze N, Tabatadze G, Nikoleishvili E, Mshvildadze M (2016) Metal-Ceramic Smart Composite in Ti(C,N)-Ni-Mo-W System. JECTC 06(2): 42-51.
- Calcium Orthophosphate-Based Bioceramics – PMC.
- Improving Biocompatibility for next Generation of Metallic Implants – ScienceDirect.
- Dorozhkin S (2011) Medical Application of Calcium Orthophosphate Bioceramics. BIO 13.
- Comuzzi L, Tumedei M, Romasco T, Petrini M, Afrashtehfar KI, et al. (2023)Insertion Torque, Removal Torque, and Resonance Frequency Analysis Values of Ultrashort, Short, and Standard Dental Implants: An In Vitro Study on Polyurethane Foam Sheets. Journal of Functional Biomaterials 14(1): 10.
- Pröbster L, Diehl J (1992) Slip-Casting Alumina Ceramics for Crown and Bridge Restorations. Quintessence Int 23(1): 25-31.
- Bessa LJ, Botelho J, Machado V, Alves R, Mendes JJ (2022) Managing Oral Health in the Context of Antimicrobial Resistance. Int J Environ Res Public Health 19(24): 16448.
- Salam MdA, Al-Amin MdY, Salam MT, Pawar JS, Akhter N, et al. (2023)Antimicrobial Resistance: A Growing Serious Threat for Global Public Health. Healthcare (Basel) 11(13): 1946.
- Uddin TM, Chakraborty AJ, Khusro A, Zidan BRM, Mitra S, et al. (2021) Antibiotic Resistance in Microbes: History, Mechanisms, Therapeutic Strategies and Future Prospects. Journal of Infection and Public Health 14(12): 1750-1766.
- Brovold M, Almeida JI, Pla-Palacín I, Sainz-Arnal P, Sánchez-Romero N, et al. (2018) Naturally-Derived Biomaterials for Tissue Engineering Applications. Adv Exp Med Biol 1077: 421-449.
- d’Angelo M, Benedetti E, Tupone MG, Catanesi M, Castelli V, et al. (2019)The Role of Stiffness in Cell Reprogramming: A Potential Role for Biomaterials in Inducing Tissue Regeneration. Cells 8(9): 1036.
- Polymers | Free Full-Text | Can 3D-Printed Bioactive Glasses Be the Future of Bone Tissue Engineering?.
- Osazee FO, Ohifuemen AO, Omoruyi JI, Ifijen IH, Otabor G (2024) Bioink Formulations for 3D Printing of Tissue Scaffolds: A Review of Materials and Printability. In Proceedings of the TMS 2024 153rd Annual Meeting & Exhibition Supplemental Proceedings; Springer Nature Switzerland: Cham pp. 484-499.
- (PDF) Sustainable Approach of Functional Biomaterials–Tissue Engineering for Skin Burn Treatment: A Comprehensive Review | Manira Maarof - Academia.Edu.
- Recent Advances of Additive Manufacturing in Implant Fabrication - A Review - ScienceDirect Available online: (accessed on 19 February 2024).
- Sakthiabirami K, Soundharrajan V, Kang JH, Yang YP, Park SW (2021) Three-Dimensional Zirconia-Based Scaffolds for Load-Bearing Bone-Regeneration Applications: Prospects and Challenges. Materials (Basel) 14(12): 3207.
- Esmaeili Y, Bidram E, Bigham A, Atari M, Nasr Azadani R, et al. (2023) Exploring the Evolution of Tissue Engineering Strategies over the Past Decade: From Cell-Based Strategies to Gene-Activated Matrix. Alexandria Engineering Journal 81: 137-169.
- Place E, Evans N, Stevens M (2009) Complexity in Biomaterials for Tissue Engineering. Nature materials 8: 457-470.






























