Oral-Gut Microbiome and Bone Health: Exploring Interplay
Laura Ferrante, Angelo Michele Inchingolo, Alessio Danilo Inchingolo, Gianna Dipalma* and Francesco Inchingolo
Department of Interdisciplinary Medicine, University of Bari “Aldo Moro”, 70124 Bari, Italy
Submission:February 20, 2024; Published:February 27, 2024
*Corresponding author:Gianna Dipalma and Francesco Inchingolo, Department of Interdisciplinary Medicine, University of Bari “Aldo Moro”, 70124 Bari, Italy
How to cite this article:Laura F, A Michele I, Alessio Danilo I, Gianna D, Francesco I. Oral-Gut Microbiome and Bone Health: Exploring Interplay. Curr Trends Biomedical Eng & Biosci. 2024; 22(3): 556088. DOI:10.19080/CTBEB.2024.22.556088
Abstract
This review provides a comprehensive analysis of the intricate interplay among the gut microbiome (GM), bone health, interleukins, chronic periodontitis, and COVID-19 within a concise 300-word limit. It begins by exploring the symbiotic relationship between the GM and bone health, delineating their composition, functions, and influencing factors. The discussion seamlessly transitions to the interaction between the GM and bone metabolism, emphasizing nutrient absorption, microbial metabolites, specific bacteria, and immune modulation. Experimental evidence highlights the significant impact of the GM on bone health, elucidating the roles of microbial metabolites and bacterial strains. The analysis further investigates the complex nexus between interleukins, chronic periodontitis, and COVID-19, underscoring genetic variations and immune responses shaping susceptibility and severity in viral infections. Chronic periodontitis emerges as a crucial focal point for understanding systemic dysbiosis, with genetic factors, dysbiosis, and therapeutic approaches offering insights into risk assessment and potential interventions. The proposed shift in therapeutic strategies centers on addressing dysbiosis, immune dynamics, and endocrine balance to manage degenerative and infectious diseases effectively. In conclusion, this review navigates the intricate landscape of human physiology, weaving together diverse elements to provide a holistic understanding. It underscores the importance of ongoing research to unravel the complex interplay of genetics, immune responses, and systemic health, emphasizing the need for continued exploration in this field.
Keywords:Bone health, Gut microbiome, Oral microbiome, Chronic periodontitis, Dysbiosis, gastrointestinal tract, Archaea, Predominant phyla, Actinobacteria, Proteobacteria, Bacteroidetes, biomarkers
Introduction
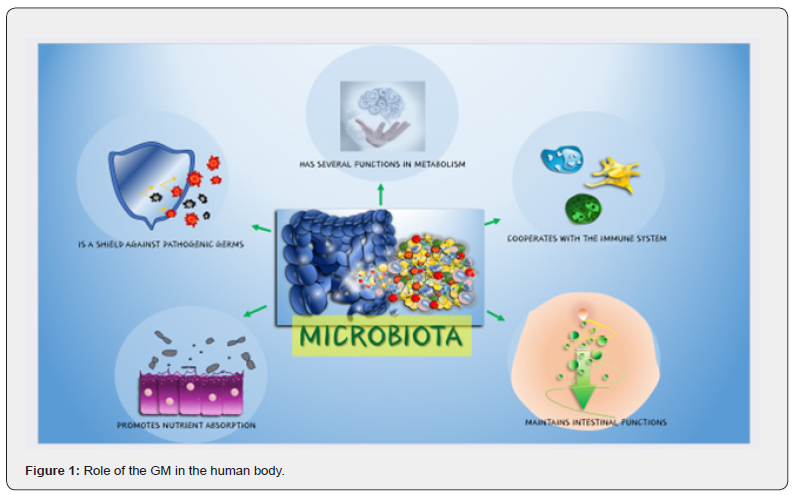
The human body functions as a complex web of various systems and organs, with recent research shedding light on the intricate relationship between GM and bone health [1-4]. The GM, a vast community of microorganisms residing in the gastrointestinal tract, has been recognized for its crucial role in influencing several physiological processes crucial to maintaining overall health (Figure1) [5-8]. This review explores the multifaceted connections between GM and bone health, examining the composition and importance of GM, the fundamentals of bone health, and emerging evidence indicating a mutualistic relationship between the two [9-13].
Discussion
GM is a complex and dynamic ecosystem residing in the gastrointestinal tract, comprising trillions of microorganisms, including bacteria, viruses, fungi, and archaea [14-18]. This microbial community plays a crucial role in maintaining overall health and homeostasis within the human body [19-23]. The composition of the GM is diverse and varies among individuals, shaped by numerous factors including genetics, diet, age, lifestyle, and environmental exposures [24-28]. Predominant phyla in the GM include Firmicutes, Bacteroidetes, Actinobacteria, and Proteobacteria. Each individual’s microbiome is unique, resembling a fingerprint that reflects their own genetic heritage and distinct life experiences [29-33]. The functions of the GM are multifaceted [34-40].
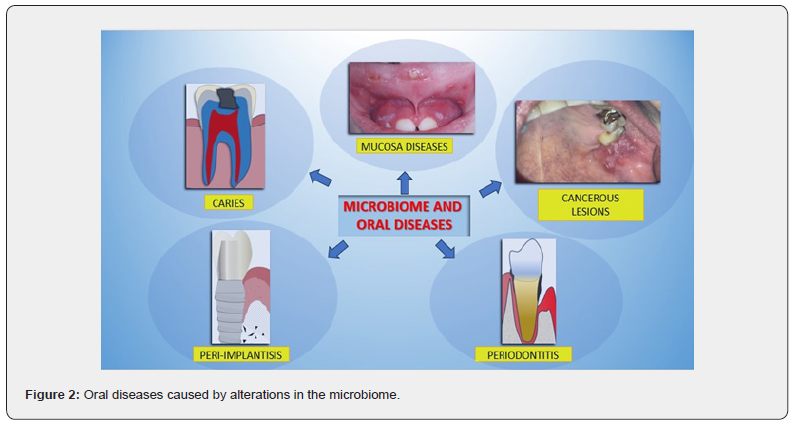
Recently, microbiome research is focusing on issues related to genetics, oral dysbiosis, bacteraemia, and chronic periodontitis (Figure 2) [41-47].GM actively participates in the digestion and absorption of nutrients, breaking down complex carbohydrates and producing enzymes that the human body cannot generate on its own [48-50]. Additionally, the GM contributes to the synthesis of certain vitamins, such as B vitamins and vitamin K, which are essential for various physiological processes [51-57]. When discussing the relationship between our gut and bones, we delve into a complex and fascinating world [58-64]. This interaction, often referred to as the gut-bone axis, is influenced by a wide range of factors concerning our dietary choices, lifestyle, medications we take, and even our environmental exposures [65- 70]. Understanding these factors is crucial for comprehending how the gut microbiota influences bone health and for identifying possible avenues for positive intervention [71-77].
Let’s start with diet and nutrient intake, two fundamental pillars for bone health [78-83]. Calcium and vitamin D are essential, and our gut microbiota plays a crucial role in absorbing these nutrients [84-90]. A balanced diet promotes microbial diversity and optimal nutrient utilization. Moving on to antibiotic use, we see how these medications, although essential for treating bacterial infections, can have a significant impact on our microbiota [91-98]. Broadspectrum antibiotics can alter the microbial balance, potentially influencing bone metabolism [99-105]. Lifestyle factors are equally important. Regular physical activity and weight-bearing exercises benefit bone health [106-112]. Physical activity may contribute to greater microbial diversity, influencing the gut-bone axis through the release of exercise-influenced factors [113-115]. We cannot overlook age and hormonal changes, which have a significant impact on bone health [116-118]. Postmenopausal women, for example, experience a decrease in estrogen levels, leading to increased bone resorption [119-123]. These hormonal changes may also affect the gut microbiota, creating an intricate interplay between aging, hormones, and bone health. Medications represent another important piece of the puzzle [74,124-126].
Drugs that alter gastric acidity, such as proton pump inhibitors and antacids, can affect calcium absorption in the intestine, with potential consequences for bone health in the long term [118]. Stress and mental health also play a role in the broader picture. Chronic stress may contribute to influence inflammatory responses that could affect bone health through their interaction with the gut-brain axis [127-132]. Disease states, such as inflammatory bowel disease and celiac disease, can have a negative impact on gut microbiota health and nutrient absorption, with implications for bone density [133-137]. Finally, we cannot underestimate the importance of genetic factors and early environmental exposures in shaping our gut microbiota and, consequently, our bone health throughout life [18,138-140].
This growing understanding of the interaction between the microbiota and bone health has significant clinical implications, paving the way for potential therapeutic interventions aimed at optimizing skeletal well-being [141-144]. The use of probiotics and prebiotics, for example, represents a promising option for modulating the microbiota and positively influencing bone metabolism. Personalized approaches are becoming increasingly relevant, considering the variability in microbiota composition among individuals. Microbiota analysis can guide tailored therapeutic interventions, taking into account each individual’s unique microbial landscape. Dietary recommendations are crucial to support bone health and microbial diversity [33,145-146]. Nutrient-rich diets containing calcium, vitamin D, and prebiotic fibers are crucial, as well as the inclusion of fermented foods that introduce beneficial probiotic microorganisms[147]. Physical exercise and lifestyle modifications can be a powerful tool in promoting bone health and microbial diversity. Responsible antibiotic use and awareness of their potential effects on the microbiota must be integral to clinical practices [148-150]. Regular clinical monitoring and the development of specific biomarkers for the gut-bone axis can help identify early issues and adopt targeted interventions [141,4]. Educating patients about the importance of gut health for skeletal well-being can promote active participation in managing their health [151-153]. Finally, therapeutic innovation, multidisciplinary involvement, and ongoing research are crucial for translating this knowledge into effective and personalized clinical interventions that improve patient outcomes and prevent skeletal-related disorders [101,154,155]. This holistic view, considering both the microbiota and bone health, offers extraordinary opportunities to improve people’s health and quality of life, and continuing to study and test these insights is essential for the success of these innovative strategies [101,156].
Conclusion
The gut and microbiomes are interconnected and mutually influence overall health. Integrated therapeutic approaches considering both microbiomes are emerging as promising strategies to improve overall health. Future research should delve deeper into this complex relationship to develop increasingly effective and personalized therapies for preventing and treating a wide range of pathological conditions, both intestinal and oral.
References
- IJMS | Free Full-Text | Interactions between Dental MSCs and Biomimetic Composite Scaffold during Bone Remodeling Followed by In Vivo Real-Time Bioimaging.
- Aggarwal N, Kitano S, Puah GRY, Kittelmann S, Hwang IY, et al. (2022) Microbiome and Human Health: Current Understanding, Engineering, and Enabling Technologies. Chem Rev 123(1): 31-72.
- Santacroce L, Charitos IA, Ballini A, Inchingolo F, Luperto P, et al.(2020)The Human Respiratory System and Its Microbiome at a Glimpse. Biology 9(10): 318-318.
- Ballini A, Dipalma G, Isacco CG, Boccellino M, Di Domenico M, et al.(2020) Oral Microbiota and Immune System Crosstalk: A Translational Research. Biology (Basel) 9(6): 131.
- Thursby E, Juge N (2017) Introduction to the Human Gut Microbiota. Biochem J 474(11): 1823-1836,
- Liu J, Tan Y, Cheng H, Zhang D, Feng W, et al.(2022) Functions of Gut Microbiota Metabolites, Current Status and Future Perspectives. Aging Dis 13(4): 1106-1126.
- The Hidden Threat: Environmental Toxins and Their Effects on Gut Microbiota – ScienceDirect.
- Gut Microbiota Changes in the Extreme Decades of Human Life: A Focus on Centenarians | Cellular and Molecular Life Sciences.
- Zhou RX, Zhang YW, Cao MM, Liu CH, Rui YF, et al. (2023) Linking the Relation between Gut Microbiota and Glucocorticoid-Induced Osteoporosis. J Bone Miner Metab 41(2): 145-162.
- Balzanelli MG, Distratis P, Lazzaro R, Cefalo A, Catucci O, et al. (2021) The Vitamin D, IL-6 and the eGFR Markers a Possible Way to Elucidate the Lung–Heart–Kidney Cross-Talk in COVID-19 Disease: A Foregone Conclusion. Microorganisms 9(9):1903.
- Ballini A, Santacroce L, Cantore S, Bottalico L, Dipalma G, et al. (2019) Probiotics Efficacy on Oxidative Stress Values in Inflammatory Bowel Disease: A Randomized Double-Blinded Placebo-Controlled Pilot Study. Endocr Metab Immune Disord Drug Targets 19(3): 373-381.
- Bhardwaj A, Sapra L, Tiwari A, Mishra PK, Sharma S, et al. (2022)“Osteomicrobiology”: The Nexus Between Bone and Bugs. Front Microbiol 12: 812466.
- You K, Yang L, Shen J, Liu B, Guo Y(2022) Relationship between Gut Microbiota and Bone Health. Mini-Reviews in Medicinal Chemistry 22(18): 2406-2418.
- Louis P, Scott KP, Duncan SH, Flint HJ (2007) Understanding the Effects of Diet on Bacterial Metabolism in the Large Intestine. J Appl Microbiol 102(5): 1197-1208.
- Metzler-Zebeli BU, Canibe N, Montagne L, Freire J, Bosi P, et al.(2019) Resistant Starch Reduces Large Intestinal pH and Promotes Fecal Lactobacilli and Bifidobacteria in Pigs. Animal 13: 64-73.
- Foster BL, Ao M, Salmon CR, Chavez MB, Kolli TN, et al. (2018) Osteopontin Regulates Dentin and Alveolar Bone Development and Mineralization. Bone 107: 196-207.
- Maspero C, Gaffuri F, Castro IO, Lanteri V, Ugolini A, et al.(2019) Correlation between Dental Vestibular-Palatal Inclination and Alveolar Bone Remodeling after Orthodontic Treatment: A CBCT Analysis. Materials (Basel) 12(24): 4225.
- Formation of Propionate and Butyrate by the Human Colonic Microbiota - Louis - 2017 - Environmental Microbiology - Wiley Online Library.
- Elhennawy K, Manton DJ, Crombie F, Zaslansky P, Radlanski RJ, et al. Structural, Mechanical and Chemical Evaluation of Molar-Incisor Hypomineralization-Affected Enamel: A Systematic Review. Arch Oral Biol 83: 272-281.
- Inchingolo AM, Malcangi G, Ferrante L, Del Vecchio G, Viapiano F, et al. (2023) Damage from Carbonated Soft Drinks on Enamel: A Systematic Review. Nutrients 15(7): 1785.
- Agarwal A, Chaudhary B (2020) Clinical and Microbiological Effects of 1% Matricaria Chamomilla Mouth Rinse on Chronic Periodontitis: A Double-Blind Randomized Placebo Controlled Trial. J Indian Soc Periodontol 24(4): 354-361.
- Crescente G, Minervini G, Spagnuolo C, Moccia S(2023) Cannabis Bioactive Compound-Based Formulations: New Perspectives for the Management of Orofacial Pain. Molecules 28: 106.
- Butera A, Gallo S, Pascadopoli M, Scardina GA, Pezzullo S, et al. (2022)Home Oral Care Domiciliary Protocol for the Management of Dental Erosion in Rugby Players: A Randomized Clinical Trial. Journal of Clinical Medicine 11(16): 4893.
- Rinninella E, Raoul P, Cintoni M, Franceschi F, Miggiano GAD, et al. (2019) What Is the Healthy Gut Microbiota Composition? A Changing Ecosystem across Age, Environment, Diet, and Diseases. Microorganisms 7(1): 14.
- Worsley SF, Davies CS, Mannarelli ME, Hutchings MI, Komdeur J, et al. (2021) Gut Microbiome Composition, Not Alpha Diversity, Is Associated with Survival in a Natural Vertebrate Population. Animal Microbiome 3: 84.
- The Person-to-Person Transmission Landscape of the Gut and Oral Microbiomes | Nature.
- Host Genetic Control of Gut Microbiome Composition | Mammalian Genome.
- Inchingolo F, Tatullo M, Abenavoli FM, Marrelli M, Inchingolo AD, et al. (2011) Oral Piercing and Oral Diseases: A Short Time Retrospective Study. Int J Med Sci 8(8): 649-652.
- Belizário JE, Napolitano M (2015) Human Microbiomes and Their Roles in Dysbiosis, Common Diseases, and Novel Therapeutic Approaches. Front Microbiol 6: 1050.
- Magne F, Gotteland M, Gauthier L, Zazueta A, Pesoa S, et al. (2020) The Firmicutes/Bacteroidetes Ratio: A Relevant Marker of Gut Dysbiosis in Obese Patients? Nutrients 12(5): 1474.
- Bioengineering | Free Full-Text | Sixty-Month Follow Up of Clinical MRONJ Cases Treated with CGF and Piezosurgery.
- Bradley PH, Pollard KS (2017) Proteobacteria Explain Significant Functional Variability in the Human Gut Microbiome. Microbiome 5: 36.
- Isacco CG, Ballini A, De Vito D, Nguyen KCD, Cantore S, et al. (2021) Rebalancing the Oral Microbiota as an Efficient Tool in Endocrine, Metabolic and Immune Disorders. Endocr Metab Immune Disord Drug Targets 21(5): 777-784.
- Maier T (2023) Oral Microbiome in Health and Disease: Maintaining a Healthy, Balanced Ecosystem and Reversing Dysbiosis. Microorganisms 11(6): 1453.
- Boccellino M, Di Stasio D, Dipalma G, Cantore S, Ambrosio P, et al.(2019) Steroids and Growth Factors in Oral Squamous Cell Carcinoma: Useful Source of Dental-Derived Stem Cells to Develop a Steroidogenic Model in New Clinical Strategies. Eur Rev Med Pharmacol 23(20): 8730-8740.
- Inchingolo F, Inchingolo AM, Malcangi G, De Leonardis N, Sardano R,et al.(2023) The Benefits of Probiotics on Oral Health: Systematic Review of the Literature. Pharmaceuticals 16: 1313.
- Cantore S, Mirgaldi R, Ballini A, Coscia MF, Scacco S, et al. (2014) Cytokine Gene Polymorphisms Associate with Microbiogical Agents in Periodontal Disease: Our Experience. Int J Med Sci 11(7): 674-679.
- Inchingolo AM, Patano A, Piras F, Mancin A, Inchingolo AD, et al. (2023) Interconnection between Microbiota-Gut-Brain Axis and Autism Spectrum Disorder Comparing Therapeutic Options: A Scoping Review. Microorganisms 11: 1477.
- Fischer RG, Lira Junior R, Retamal-Valdes B, Figueiredo Lcde, Malheiros Z, et al. (2020) Periodontal Disease and Its Impact on General Health in Latin America. Section V: Treatment of Periodontitis. Braz Oral Res 34: e026.
- Li Z, Zhu L, Sha Y (2011) [Effects of periodontal health and related factors on the oral health-related quality of life in type 2 diabetic patients with chronic periodontitis]. Hua Xi Kou Qiang Yi Xue Za Zhi 29(4): 379-383.
- Li Y, Zhu M, Liu Y, Luo B, Cui J, (2022) The Oral Microbiota and Cardiometabolic Health: A Comprehensive Review and Emerging Insights. Front Immunol 13: 1010368.
- Microbiota in Health and Diseases – PMC.
- Inchingolo F, Inchingolo AD, Palumbo I, Trilli I, Guglielmo M, et al. (2024) The Impact of Cesarean Section Delivery on Intestinal Microbiota: Mechanisms, Consequences, and Perspectives-A Systematic Review. International Journal of Molecular Sciences 25(2): 1055.
- Floyd PD, Ide M, Palmer RM(2014) Clinical Guide to Periodontology: Reconstructive Periodontal Treatment. Br Dent J 216(9): 511-518.
- Clinical Guide to Periodontology: Reconstructive Periodontal Treatment | Request PDF.
- Murphy, J. The Effect of Mechanical Vibration on Alveolar Bone Following Experimental Periodontitis: A Time Course Study.
- Commentary: The Evolution of Periodontology: Science Always Wins - Genco - 2014 - Journal of Periodontology - Wiley Online Library.
- Rowland I, Gibson G, Heinken A, Scott K, Swann J, et al. (2018) Gut Microbiota Functions: Metabolism of Nutrients and Other Food Components. Eur J Nutr 57(1): 1-24.
- Montagnani M, Bottalico L, Potenza MA, Charitos IA, Topi S, et al. (2023)Crosstalk between Gut Microbiota and Nervous System: A Bidirectional Interaction between Microorganisms and Metabolome. International Journal of Molecular Sciences 24: 10322.
- Carbohydrate Digesting Enzymes: Topics by Science.Gov.
- Kennedy DO (2016) B Vitamins and the Brain: Mechanisms, Dose and Efficacy-A Review. Nutrients 8(2): 68.
- Vitamin K - Sources, Physiological Role, Kinetics, Deficiency, Detection, Therapeutic Use, and Toxicity | Nutrition Reviews | Oxford Academic.
- Pharmacokinetics of Vitamin Dosage Forms: A Complete Overview - Sugandhi - 2024 - Food Science & Nutrition - Wiley Online Library.
- Gholami L, Asefi S, Hooshyarfard A, Sculean A, Romanos GE, et al. (2019) Photobiomodulation in Periodontology and Implant Dentistry: Part 1. Photobiomodul Photomed Laser Surg 37(12): 739-765.
- Cremon C, Barbaro MR, Ventur M, Barbara G (2018) Pre- and Probiotic Overview. Curr Opin Pharmacol 43: 87-92.
- Shin SY, Park S, Moon JM, Kim K, Kim JW, et al. (2022) Compositional Changes in the Gut Microbiota of Responders and Non-Responders to Probiotic Treatment Among Patients With Diarrhea-Predominant Irritable Bowel Syndrome: A Post Hoc Analysis of a Randomized Clinical Trial. J Neurogastroenterol Motil 28(4): 642-654.
- Inchingolo F, Pacifici A, Gargari M, Acitores Garcia JI, Amantea M, et al.(2014) CHARGE Syndrome: An Overview on Dental and Maxillofacial Features. Eur Rev Med Pharmacol Sci 18(15): 2089-2093.
- The Gut-Brain Connection and 10 Important Tips to Improve Gut Health Available online:(accessed on 19 February 2024).
- The Gut Connection: How to Improve Your Digestion and Gut Health in 6 - Nuzest.Com.
- Association Between Gut Microbiota and Bone Health: Potential Mechanisms and Prospective | The Journal of Clinical Endocrinology & Metabolism | Oxford Academic.
- The Role of Microbiota-Gut-Brain Axis in Neuropsychiatric and Neurological Disorders – ScienceDirect.
- Ghosh TS, Shanahan F, O Toole PW (2022) The Gut Microbiome as a Modulator of Healthy Ageing. Nat Rev Gastroenterol Hepatol 19: 565-584.
- Inchingolo F, Tatullo M, Marrelli M, Inchingolo AD, Corelli R, et al. (2012) Clinical Case-Study Describing the Use of Skin-Perichondrium-Cartilage Graft from the Auricular Concha to Cover Large Defects of the Nose. Head Face Med 8: 10.
- Coloccia G, Inchingolo AD, Inchingolo AM, Malcangi G, Montenegro V, et al. (2021) Effectiveness of Dental and Maxillary Transverse Changes in Tooth-Borne, Bone-Borne, and Hybrid Palatal Expansion through Cone-Beam Tomography: A Systematic Review of the Literature. Medicina (Kaunas) 57(3): 288.
- The Impact of Diet and Lifestyle on Gut Microbiota and Human Health – PMC.
- Zhang YW, Song PR, Wang SC, Liu H, Shi ZM, et al.(2024)Diets Intervene Osteoporosis via Gut-Bone Axis. Gut Microbes 16: 2295432.
- Tu Y, Yang R, Xu X, Zhou X (2021) The Microbiota-Gut-Bone Axis and Bone Health. Journal of leukocyte biology 110.
- Drug-Microbiota Interactions: An Emerging Priority for Precision Medicine | Signal Transduction and Targeted Therapy.
- Zaiss M, Jones R, Schett G, Pacifici R (2019) The Gut-Bone Axis: How Bacterial Metabolites Bridge the Distance. Journal of Clinical Investigation 129(8): 3018-3028.
- Sasso JM, Ammar RM, Tenchov R, Lemmel S, Kelber O, et al. (2023) Gut Microbiome–Brain Alliance: A Landscape View into Mental and Gastrointestinal Health and Disorders. ACS Chem. Neurosci 14(10): 1717-1763.
- Wang Y, Zhang X, Tang G, Deng P, Qin Y, et al. (2023) The Causal Relationship between Gut Microbiota and Bone Mineral Density: A Mendelian Randomization Study. Frontiers in Microbiology 14.
- Singh S, Sarma DK, Verma V, Nagpal R, Kumar M (2023) From Cells to Environment: Exploring the Interplay between Factors Shaping Bone Health and Disease. Medicina (Kaunas) 59(9): 1546.
- Zhang J, Lu Y, Wang Y, Ren X, Han J (2018) The Impact of the Intestinal Microbiome on Bone Health. Intractable Rare Dis Res 7(3): 148-155.
- Inchingolo F, Santacroce L, Cantore S, Ballini A, Del Prete R, et al. (2019) Probiotics and EpiCor® in Human Health. J Biol Regul Homeost Agents 33(6): 1973-1979.
- Inchingolo AD, Inchingolo AM, Bordea IR, Malcangi G, Xhajanka E, et al.(2021) SARS-CoV-2 Disease Adjuvant Therapies and Supplements Breakthrough for the Infection Prevention. Microorganisms 9(3): 525.
- Chen Y, Wang X, Zhang C, Liu Z, Li C, et al. (2022) Gut Microbiota and Bone Diseases: A Growing Partnership. Frontiers in Microbiology 13.
- Kunika, Frey N, Rangrez AY (2023) Exploring the Involvement of Gut Microbiota in Cancer Therapy-Induced Cardiotoxicity. International Journal of Molecular Sciences 24(8): 7261.
- Rizzoli R, Biver E, Brennan-Speranza TC(2021) Nutritional Intake and Bone Health. Lancet Diabetes Endocrinol 9: 606-621.
- Simple Tips for Maintaining Bone Strength and Health with a Focus on Food for Strong Bones and Muscles 2023.
- Kostecka M (2014) The Role of Healthy Diet in the Prevention of Osteoporosis in Perimenopausal Period. Pak J Med Sci 30(4): 763-768.
- Godman, H. Essential Nutrients Your Body Needs for Building Bone.
- New SA, Robins SP, Campbell MK, Martin JC, Garton MJ, et al. (2000)Dietary Influences on Bone Mass and Bone Metabolism: Further Evidence of a Positive Link between Fruit and Vegetable Consumption and Bone Health?123. The American Journal of Clinical Nutrition 71(1): 142-151.
- Inchingolo AD, Inchingolo AM, Bordea IR, Xhajanka E, Romeo DM, et al. (2021) The Effectiveness of Osseodensification Drilling Protocol for Implant Site Osteotomy: A Systematic Review of the Literature and Meta-Analysis. Materials (Basel) 14(5): 1147.
- Akimbekov NS, Digel I, Sherelkhan DK, Lutfor AB, Razzaque MS (2020) Vitamin D and the Host-Gut Microbiome: A Brief Overview. Acta Histochem Cytochem 53(3): 33-42.
- Hadadi N, Berweiler V, Wang H, Trajkovski M (2021) Intestinal Microbiota as a Route for Micronutrient Bioavailability. Current Opinion in Endocrine and Metabolic Research 20: 100285.
- Vitamins, the Gut Microbiome and Gastrointestinal Health in Humans – ScienceDirect.
- How Vitamin D Aids Digestive Health and Improves Gut Microbiome.
- Exploring the Role of Vitamin D and the Vitamin D Receptor in the Composition of the Gut Microbiota.
- Favero C, Giordano L, Mihaila SM, Masereeuw R, Ortiz A, (2022) Postbiotics and Kidney Disease. Toxins 14(9): 623.
- Fei Y, Chen Z, Han S, Zhang S, Zhang T, et al. (2023) Role of Prebiotics in Enhancing the Function of Next-Generation Probiotics in Gut Microbiota. Crit Rev Food Sci Nutr 63(8): 1037-1054.
- Leeming ER, Johnson AJ, Spector TD, Le Roy CI (2019) Effect of Diet on the Gut Microbiota: Rethinking Intervention Duration. Nutrients 11(12): 2862.
- Influence of Foods and Nutrition on the Gut Microbiome and Implications for Intestinal Health – PMC.
- Interplay of Dietary Antioxidants and Gut Microbiome in Human Health: What Has Been Learnt Thus Far? – ScienceDirect.
- Ramirez J, Guarner F, Bustos FL, Maruy A, Sdepanian VL (2020) Antibiotics as Major Disruptors of Gut Microbiota. Frontiers in Cellular and Infection Microbiology 10.
- Fernandez MA, Marette A (2017) Potential Health Benefits of Combining Yogurt and Fruits Based on Their Probiotic and Prebiotic Properties. Adv Nutr 8(1): 155S-164S.
- Belli WA, Marquis RE (1991) Adaptation of Streptococcus Mutans and Enterococcus Hirae to Acid Stress in Continuous Culture. Appl Environ Microbiol 57(4): 1134-1138.
- Ferrarese R, Ceresola ER, Pret A, Canducci F (2018) Probiotics, Prebiotics and Synbiotics for Weight Loss and Metabolic Syndrome in the Microbiome Era. Eur Rev Med Pharmacol Sci 22(21): 7588-7605.
- Inchingolo AD, Di Cosola M, Inchingolo AM, Greco Lucchina A, Malcangi G, et al. (2021)Correlation between Occlusal Trauma and Oral Microbiota: A Microbiological Investigation. J Biol Regul Homeost Agents 35: 295-302.
- Lyu Z, Hu Y, Guo Y, Liu D (2023) Modulation of Bone Remodeling by the Gut Microbiota: A New Therapy for Osteoporosis. Bone Res 11(1): 1-15
- Zhao X, Zhang Z, Wang Y, Qian K, Qin H, et al.(2021) Association of Antibiotic Alterations in Gut Microbiota With Decreased Osseointegration of an Intramedullary Nail in Mice With and Without Osteomyelitis. Front Endocrinol (Lausanne) 12: 774257.
- Yan Q, Cai L, Guo W (2022) New Advances in Improving Bone Health Based on Specific Gut Microbiota. Front Cell Infect Microbiol 12: 821429.
- Rios-Arce ND, Schepper JD, Dagenais A, Schaefer L, Daly-Seiler CS, et al. (2020) Post-Antibiotic Gut Dysbiosis-Induced Trabecular Bone Loss Is Dependent on Lymphocytes. Bone 134: 115269.
- Yan J, Herzog JW, Tsang K, Brennan CA, Bower MA, et al. (2016) Gut Microbiota Induce IGF-1 and Promote Bone Formation and Growth. Proceedings of the National Academy of Sciences 113: E7554-E7563.
- Sc, HA The Effect of Antibiotics on the Gut Microbiome.
- D’Amelio P, Sassi F (2018) Gut Microbiota, Immune System, and Bone. Calcif Tissue Int 102(4): 415-425.
- Carter MI, Hinton PS (2014) Physical Activity and Bone Health. Mo Med 111(1): 59-64.
- Sheng B, Li X, Nussler AK, Zhu S (2021) The Relationship between Healthy Lifestyles and Bone Health. Medicine (Baltimore) 100(8): e24684.
- Exercise and Bone Health - OrthoInfo – AAOS.
- Osteoporosis and Exercise - Better Health Channel.
- Gader AGMA (2018)The Effect of Exercise and Nutrition on Bone Health. JMSR 2: 142.
- Slowing Bone Loss with Weight-Bearing Exercise.
- Troy KL, Mancuso ME, Butler TA, Johnson JE(2018) Exercise Early and Often: Effects of Physical Activity and Exercise on Women’s Bone Health. International Journal of Environmental Research and Public Health 15(5): 878.
- Monda V, Villano I, Messina A, Valenzano A, Esposito T, et al.(2017) Exercise Modifies the Gut Microbiota with Positive Health Effects. Oxidative Medicine and Cellular Longevity 2017.
- Wegierska AE, Charitos IA, Topi S, Potenza MA, Montagnani M, et al.(2022) The Connection Between Physical Exercise and Gut Microbiota: Implications for Competitive Sports Athletes. Sports Med 52(10): 2355-2369.
- Aya V, Jimenez P, Muñoz E, Ramírez JD (2023)Effects of Exercise and Physical Activity on Gut Microbiota Composition and Function in Older Adults: A Systematic Review. BMC Geriatrics 23: 364.
- Cheng CH, Chen LR, Chen KH (2022) Osteoporosis Due to Hormone Imbalance: An Overview of the Effects of Estrogen Deficiency and Glucocorticoid Overuse on Bone Turnover. Int J Mol Sci 23(3): 1376.
- Rizzoli R, Bonjour JP (1997) Hormones and Bones. The Lancet 349: S20-S23.
- OpenStaxCollege Exercise, Nutrition, Hormones, and Bone Tissue. 2013.
- Ji MX, Yu Q (2015) Primary Osteoporosis in Postmenopausal Women. Chronic Dis Transl Med 1(1): 9-13.
- Thapa S, Nandy A, Rendina-Ruedy E(2022) Endocrinal Metabolic Regulation on the Skeletal System in Post-Menopausal Women. Front Physiol 13: 1052429.
- Baron R (2006) FSH versus Estrogen: Who’s Guilty of Breaking Bones? Cell Metabolism 3(5): 302-305.
- Møller AMJ, Delaissé JM, Olesen JB, Madsen JS, Canto LM,et al. (2020) Aging and Menopause Reprogram Osteoclast Precursors for Aggressive Bone Resorption. Bone Res 8: 1-11.
- Borsani E, Bonazza V, Buffoli B, Nocini PF, Albanese M, et al. (2018) Beneficial Effects of Concentrated Growth Factors and Resveratrol on Human Osteoblasts In Vitro Treated with Bisphosphonates. BioMed Research International Pp1-13.
- Jackova Z, Stepan JJ, Coufal S, Kostovcik M, Galanova N,et al.(2023)Interindividual Differences Contribute to Variation in Microbiota Composition More than Hormonal Status: A Prospective Study. Front Endocrinol (Lausanne) 14: 1139056.
- Ogunrinola GA, Oyewale JO, Oshamika OO, Olasehinde GI (2020) The Human Microbiome and Its Impacts on Health. Int J Microbiol 8045646.
- Seely KD, Kotelko CA, Douglas H, Bealer B, Brooks AE (2021) The Human Gut Microbiota: A Key Mediator of Osteoporosis and Osteogenesis. International Journal of Molecular Sciences 22(17): 9452.
- Madison A, Kiecolt-Glaser JK (2019) Stress, Depression, Diet, and the Gut Microbiota: Human–Bacteria Interactions at the Core of Psychoneuroimmunology and Nutrition. Curr Opin Behav Sci 28: 105-110.
- Clapp M, Aurora N, Herrera L, Bhatia M, Wilen E, et al. (2017) Wakefield, S. Gut Microbiota’s Effect on Mental Health: The Gut-Brain Axis. Clin Pract 7(4): 987.
- Ritz NL, Draper LA, Bastiaanssen TFS, Turkington CJR, Peterson VL, et al.(2024) The Gut Virome Is Associated with Stress-Induced Changes in Behaviour and Immune Responses in Mice. Nat Microbiol 9: 359-376.
- Frontiers | The Microbiota-Gut-Brain Axis in Stress and Depression.
- Frontiers | Signalling Cognition: The Gut Microbiota and Hypothalamic-Pituitary-Adrenal Axis.
- Ma Q, Xing C, Long W, Wang HY, Liu Q, et al.(2019) Impact of Microbiota on Central Nervous System and Neurological Diseases: The Gut-Brain Axis. Journal of Neuroinflammation 16: 53.
- The Brain-Gut Axis: Psychological Functioning and Inflammatory Bowel Diseases – PMC.
- Ge L, Liu S, Li S, Yang J, Hu G, et al. (2022)Psychological Stress in Inflammatory Bowel Disease: Psychoneuroimmunological Insights into Bidirectional Gut–Brain Communications. Frontiers in Immunology 13.
- Oligschlaeger Y, Yadati T, Houben T, Condello Oliván CM, Shiri-Sverdlov R (2019) Inflammatory Bowel Disease: A Stressed “Gut/Feeling.” Cells 8(7): 659.
- Microbiota-Gut-Brain Axis and Its Affect Inflammatory Bowel Disease: Pathophysiological Concepts and Insights for Clinicians.
- Inchingolo F, Martelli FS, Gargiulo Isacco C, Borsani E, Cantore S, et al.(2020) Chronic Periodontitis and Immunity, Towards the Implementation of a Personalized Medicine: A Translational Research on Gene Single Nucleotide Polymorphisms (SNPs) Linked to Chronic Oral Dysbiosis in 96 Caucasian Patients. Biomedicines 8(5): 115.
- The Gut Microbiome: Relationships with Disease and Opportunities for Therapy - PMC Available online:(accessed on 19 February 2024).
- Toubon G, Butel MJ, Rozé JC, Nicolis I, Delannoy J,et al. (2023) Early Life Factors Influencing Children Gut Microbiota at 3.5 Years from Two French Birth Cohorts. Microorganisms 11(6): 1390.
- Hansen KE, Jones AN, Lindstrom MJ, Davis LA, Ziegler TE, et al. (2010)Do Proton Pump Inhibitors Decrease Calcium Absorption? J Bone Miner Res 25(12): 2786-2795.
- Contaldo M, Fusco A, Stiuso P, Lama S, Gravina AG, et al. (2021) Oral Microbiota and Salivary Levels of Oral Pathogens in Gastro-Intestinal Diseases: Current Knowledge and Exploratory Study. Microorganisms 9(5): 1064.
- Zheng D, Liwinski T, Elinav E (2020) Interaction between Microbiota and Immunity in Health and Disease. Cell Res 30(6): 492-506.
- (10) Microbiome-Based Personalized Nutrition as a Result of the 4.0 Technological Revolution: A Mini Literature Review | Request PDF Available online: (accessed on 19 February 2024).
- Signorini L, Ballini A, Arrigoni R, De Leonardis F, Saini R, et al.(2021) Evaluation of a Nutraceutical Product with Probiotics, Vitamin D, Plus Banaba Leaf Extracts (Lagerstroemia Speciosa) in Glycemic Control. Endocr Metab Immune Disord Drug Targets 21(7): 1356-1365.
- Lozupone CA, Stombaugh JI, Gordon JI, Jansson JK, Knight R(2012) Diversity, Stability and Resilience of the Human Gut Microbiota. Nature 489: 220-230.
- Montemurro N, Perrini P, Marani W, Chaurasia B, Corsalini M, et al. (2021) Multiple Brain Abscesses of Odontogenic Origin. May Oral Microbiota Affect Their Development? A Review of the Current Literature. Applied Sciences 11(8): 3316.
- Cantore S, Ballini A, De Vito D, Abbinante A, Altini V, et al. (2018) Clinical Results of Improvement in Periodontal Condition by Administration of Oral Probiotics. J Biol Regul Homeost Agents 32(5): 1329-1334.
- Impact of Antibiotics on the Human Microbiome and Consequences for Host Health - PMC Available online:(accessed on 19 February 2024).
- Sartelli M, Barie PS, Coccolin F, Abbas M, Abbo LM, et al. (2023) Ten Golden Rules for Optimal Antibiotic Use in Hospital Settings: The WARNING Call to Action. World Journal of Emergency Surgery 18(1): 50.
- Aljeldah MM(2022) Antimicrobial Resistance and Its Spread Is a Global Threat. Antibiotics (Basel)11(8): 1082.
- Inchingolo AD, Cazzolla AP, Di Cosola M, Greco Lucchina A, Santacroce L, et al.(2021) The Integumentary System and Its Microbiota between Health and Disease. J Biol Regul Homeost Agents 35: 303-321.
- Rapid Inactivation of SARS-CoV-2 Variants by Continuous and Intermittent Irradiation with a Deep-Ultraviolet Light-Emitting Diode (DUV-LED) Device. - Cerca Con Google Available online: (accessed on 19 February 2024).
- Nishisaka-Nonaka R, Mawatari K, Yamamoto T, Kojima M, Shimohata T, et al.(2018)Irradiation by Ultraviolet Light-Emitting Diodes Inactivates Influenza a Viruses by Inhibiting Replication and Transcription of Viral RNA in Host Cells. J Photochem Photobiol B 189: 193-200.
- Cullen CM, Aneja KK, Beyhan S, Cho CE, Woloszynek S, et al.(2020) Emerging Priorities for Microbiome Research. Frontiers in Microbiology 11: 36.
- Nutrients | Free Full-Text | Unraveling the Gut Microbiome–Diet Connection: Exploring the Impact of Digital Precision and Personalized Nutrition on Microbiota Composition and Host Physiology Available online:(accessed on 19 February 2024).
- Gut Microbiota for Health on LinkedIn: New findings show novel links between gut microbiome and bone density Available online:(accessed on 19 February 2024).






























