Exploring the Role of Human Gut Microbiota in Atopic Asthma - The Gut Lung Node
Vijayasri Hari and Deepa Parvathi V*
Department of Biomedical Sciences, Sri Ramachandra Institute of Higher Education and Research, India
Submission:May 02, 2022;Published:May 19, 2022
*Corresponding author:Deepa Parvathi Venkatachalam, Assistant Professor, Department of Biomedical Sciences, Sri Ramachandra Institute of Higher Education and Research, Porur, Chennai, India
How to cite this article: Vijayasri H, Deepa P V. Exploring the Role of Human Gut Microbiota in Atopic Asthma - The Gut Lung Node. Curr Trends Biomedical Eng & Biosci. 2022; 20(5): 556048. DOI:10.19080/CTBEB.2022.20.556048
Abstract
Atopic asthma is a hypersensitive reaction that occurs on exposure to allergens mediated by immunoglobulin E. Environmental, genetic and immunological factors concurrently influence the onset, development and severity of the disease characterized by wheezing, bronchospasm, cough and airway remodeling. Human gut microbiota is a complex, dynamic and diverse environment that regulates physiological mechanisms and prevents occurrence of disorders. The role of gut microbiota in atopic asthma has been established due to its effects at the immunological and histological levels. Composition of microbiota in the case of atopic asthma has been found to vary with age, health status, maternal effect, usage of antibiotics and method of delivery. Therapeutics that can modify the microbiota including probiotics, prebiotics and synbiotics are implicated in treatment of atopic asthma. Furthermore, traditional medicine-based interventions are also being explored among which curcumin has proven to be highly efficacious. This review provides a comprehensive view on factors, diagnosis, treatment, association of gut microbiome and remedies for asthma.
Keywords: Atopic asthma; Gut microbiota; Curcumin
Abbreviations: IgE: Immunoglobulin E; IL: Interleukin; Fc receptor: Fragment crystallizable receptor; Th17: T helper Cell 17; Th2: T helper Cell 2; SCIT: Subcutaneous Immunotherapy; SLIT: Sublingual Immunotherapy; TNF-β: Tumor Necrosis Factor Beta; IgA: Immunoglobulin A; IgG4: Immunoglobulin G4; Treg: Regulatory T cell; DC: Dendritic Cell; iNKT: invariant Natural Killer T cell; C-section: Caesarean section; MMP9: Matrix Metalloproteinase 9; eNO: Exhaled Nitric Oxide; Th1: T helper Cell 1; HLA-DR: Human Leukocyte Antigen-DR isotype; HMOs: Human Milk Oligosaccharides; TNF-α – Tumor Necrosis Factor α; NF-κB: Nuclear Factor kappa B; LPS: Lipopolysaccharide; RSV: Respiratory Syncytial Virus; eIF2α: Eukaryotic Translation Initiation Factor 2 Subunit 1; PKR: Protein Kinase R; AQP: Aquaporin; LGG: Lactobacillus rhamnosus GG; CCL17: Chemokine Ligand 17;
Introduction
Asthma is a pulmonary disorder associated with inflammation, bronchoconstriction and hyperactivity [1,2]. Approximately, 300 million people are affected by asthma worldwide with 8% in India alone [3]. There is a complex interplay between genetic, environmental and immunological factors throughout the progression of the disease. In recent times, the role of gut microbiome in asthma has been investigated providing insights into mechanism as well as treatment.
Types of Asthma
Asthma can be broadly classified as atopic and non-atopic asthma [4]. Atopic asthma is a type I hypersensitivity reaction occurring from infancy, triggered on exposure to allergens. On the other hand, non-atopic asthma is related to viral infections and certain allergens. Drugs and air pollutants have also been reported to induce asthmatic attacks [2,4].
Atopic Asthma
Atopic asthma, also known as allergic or extrinsic asthma, is initiated from childhood characterized by an exaggerated hyperresponsiveness to common aeroallergens. Individuals with a familial predisposition are susceptible and display this phenomenon mediated by IgE antibodies. It is accompanied by rhinitis, wheezing and eczema [4-6]. Diet, ozone, dust mites, pets, endotoxin, pollen [7-10], animal dander are few of the risk factors [4]. Pertaining to childhood asthma, tobacco, oxidative stress and method of delivery have been noted [11,12]. An increased consumption of fast food and polyunsaturated fatty acids (PUFAs) can precipitate while antioxidant sources including fruits, vegetables and omega-3 fatty acids containing fish constitute a protective action [13,14]. These effects arise from the influence on biogenesis of inflammatory mediators [15]. Interestingly, not all asthmatics with atopy develop atopic asthma [16].
Pathogenesis of Atopic Asthma
Cellular and humoral mediated immune responses together contribute to pathogenesis of asthma. This occurs in two phases: early and late. Early phase is largely resolvable whereas late phase progressively leads to irreversible damage [1]. When an allergen enters the airway, it is endocytosed and processed by antigenpresenting cells (APCs), predominantly dendritic cells. It is then presented to T-cells stimulating their maturation. T-helper-2 and T-helper-17 cells (Th2, Th17) are the two major subtypes involved in pathogenesis of asthma. Upon binding to the antigen via cell surface receptors, they produce interleukins IL-4, IL-13, IL-5 and IL-17 respectively. IL-4 and IL-13 induce B-lymphocytes, which then secrete IgE antibodies. IgE antibodies interact with mast cells and basophils via Fc receptors. It remains in circulation as well as bound to the surfaces. On subsequent contact with the same allergen, an antigen-antibody (immune) complex is formed on their surfaces and causes degranulation. Degranulation results in release of cytokines such as histamine, prostaglandins, leukotrienes that promote vasodilation, inflammation and smooth muscle contraction. In addition, they increase the permeability of vessels and synthesis of mucus. Because of chemotaxis, eosinophils, T-lymphocytes and neutrophils are recruited to the site, which establish a sustained inflammatory reaction. IL-5 from Th2 cells enhances eosinophils, which also emit inflammatory mediators. Th-17 support Th-2 mediated response through IL-17 [17]. Consequences of this cascade are epithelial injury, obstruction, bronchospasm, oedema and airway remodeling [18,19] . These pathophysiological changes manifest as wheezing, dyspnea and cough [1]. At the histological level; hyperplasia, hypertrophy, fibrosis, accumulation of mucus, denudation of epithelium, infiltration of cells, thickening of basement membrane and presence of goblet cells have been observed [1,20].
Factors
Factors responsible for asthma can be attributed to the individual (host) and environment (causal or precipitating). Host factors refer to variations within the individual such as genetic mutations, inherited vulnerability and atopy [4]. ORMDL3, GSDMB [21], ZPBP2 [22] on 17q21 locus; IL33 [21,22], CYBRD1 [23], RAD50, IL2RB, IL1RL1, DENND1BI [22], TNFSF15 [23], ADAM33 [24], ABI3BP, MICA, NAF1 [21], IL-4 , IL-10, SCYA11, PHF11, iNOS, CD14 FcεRIβ [24] and HLA-DQB1 [22] are demonstrated to be associated with asthma. In addition to allergens, diet, tobacco, rhinoviral and respiratory syncytial viral infections above mentioned [25-27]; obesity [28], exercise [2], usage of nonsteroidal anti-inflammatory (NSAIDs) [2], indoor and outdoor air pollutants [11], climate changes, fetal health [29-30] and chemical irritants are categorized as causal factors [11].
Diagnosis
Diagnosis of asthma begins with description and occurrence of symptoms, exposure to potential allergens, familial atopy and consolidation of case history. Expiration tests and evaluation of nasal cavity is performed routinely. Since atopic asthma is an allergic response, allergy testing either in-vitro or in-vivo is recommended. Skin prick test, an in-vivo technique, utilizes a panel of allergens and controls to identify hypersensitivity responses of the individual. It is crucial that the test is based on regulated reagents to produce valid, reliable and safe results. Panel of allergens to be included will be determined by the case history. Skin prick test is conducted at regular intervals to identify new allergic reactions. Measurement of IgE in serum is done in-vitro depending on the nature and severity of the response [31].
Treatment
Treatment is based on pharmacotherapy and immunotherapy.
Pharmacotherapy
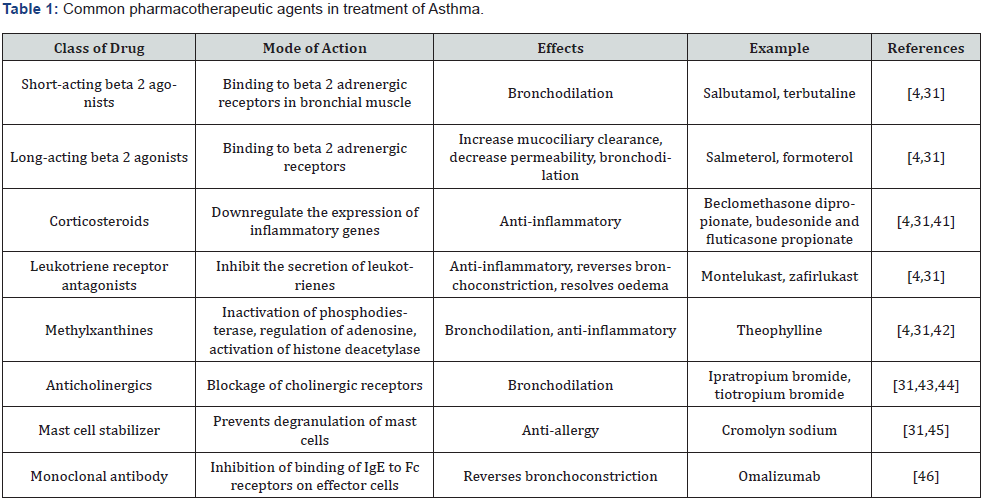
Objective of pharmacotherapy is to alleviate the symptoms, reduce the exaggerated responses with minimal side effects. The design depends upon severity of attacks, effectiveness of drugs and phenotype [31]. Some of commonly used drugs for treatment of asthma are given in Table 1.
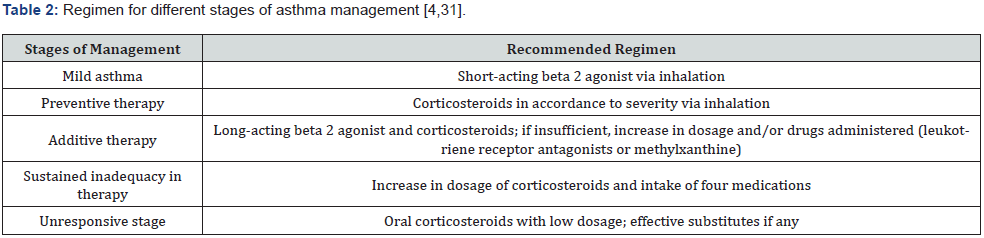
Based on stage of management of asthma, different regimes varying in number, type, route of administration and dosage of drugs should be followed as given in Table 2.
Drugs can be administered in different ways depending upon the type, physical properties, dosage, intended bioavailability, duration and site of action which can be oral or inhalation routes [31]. For inhalation route, inhaler devices are commonly used. Types of inhalers include metered-dose inhaler and dry powder inhaler. Nebulisers are rarely used [4].
Immunotherapy
Immunotherapy is a therapeutic intervention that administers allergens based on sensitisation profile in periodic and progressive concentrations in order to develop immunological tolerance in the individual. The modes of immunotherapy can be subcutaneous (SCIT) or sublingual (SLIT) [47]. SCIT has better efficacy. However, it relies upon injections containing aqueous extracts that can be only delivered in healthcare facilities with increased risk for immune reactions [48]. SLIT is suitable for self-management formulated as tablets or drops [48,49] . Immunotherapy modifies action of both the innate and adaptive components, producing antiinflammatory actions. Upon immunotherapy, regulatory T and B cells are activated which prevent Th2 mediated actions, inhibitory cytokines (IL-10, TNF-beta, IL-35) secreted, IgE-related effects suppressed along with presence of IgA and IgG4 in serum [48].
Extracts derived from Phleum pratense and Dermatophagoides pteronyssinus are used for preparations. Immunotherapy is indicated for atopic and controlled asthmatics elder than 5 years [49]. Since immunotherapy directly targets the immunological mechanisms involved in asthma, it can alter the advancement of the disease and thus is significant [48]. Other remedial measures include Th2 targeted strategies such as usage of Th2 cytokine inhibitor Suplatast tosilate in atopic asthma and inhibition of memory cells [50-52], incorporation of statins (Atorvastatin) for enhancing anti-inflammatory action, administration of cytokines in low concentrations, promising monoclonal antibodies against mediators like TNF (Infliximab) [53-55], Temperature controlled laminar airflow (TLA) decreasing allergen exposure beneficial in extrinsic asthma and adjunction of medications with acupuncture capable of regulating immune responses [56,57].
Overview of Gut Microbiome
Gut microbiome comprises of a plethora of diverse microorganisms ranging from bacteria, viruses, protozoa and fungi that interact with the gastrointestinal system establishing a dynamic environment [58,59]. As embryogenesis occurs, the microbiota is also gradually organised within the foetus. During neonatal development, there is a period defined as critical window which is when the infants respond more sensitively to microbiotadriven immunoregulatory mechanisms [60]. If the microbiota is altered in this period, it can underly atopic disorders [61]. Factors such as mode of delivery, formula-based feeding [61-64], vitamin D, breast feeding [58], nutrition [62], usage of antibiotics [58,61,62], ambient air pollution, environmental exposure, absence of pets and having siblings are implicated in maturation of gut microbiota. Canine associated households have a unique particulate microbial community with L. johnsonii being the focal bacterium [62,64]. It has been accounted to minimise respiratory syncytial viral (RSV) infection and overall atopy. Increase in Treg cells, production of fatty acid metabolites and a decrease in interleukins 4,5, 17 and DCs were responsible for the effects [64].
The environment within the gut is characterized by an interdependent, symbiotic relationship between the human and microorganisms. Essentiality of this association is implied in maintenance of physiological activities involving immunological,neural, metabolic and epithelial systems along with homeostasis. Microbes within the gut are sensitive to cues from the internal as well as the external milieu, producing different responses [59]. These responses may result in establishment of inflammatory bowel disease (IBD), obesity, autoimmune disorders, cancer, diabetes mellitus, autistic spectrum disorder, cardiovascular disorders and atopic asthma [64]. Distribution and abundance of microbes in the gut is influenced by host and co-existing microbial competition. Due to these variations, individuals are classified based on enterotypes. Enterotypes are defined as communities of microbes inhabiting within the individual. A metagenomic study conducted with samples from four different countries revealed variations arising from three dominant enterotypes belonging to Bacteroides, Prevotella and Ruminococcus genera, with microbial genes as potential biomarkers [65].
Association Between Gut Microbiome and Atopic Asthma
Experimental data have ascertained that gut microbiome can regulate and modify behaviour of innate and adaptive immune system components by influencing the secretion of cytokines. Enhancing the synthesis of IL-10 and suppressing release of Chemokine ligand (CCL5), TNF, IL-12 and nuclear factor kappa B (NF-κB) constitutes an anti-inflammatory state. By expressing ligands for CXC chemokine receptor 2 (CXCR2) presents on surface of mast cells, epithelial cells home mast cells to the intestine, managing the functioning of the immune system. The maturation and differentiation of CD4+ cells and Treg cells are impacted by gut microbiome. Recruitment of pili-like protein stimulates Treg cells which in turn switch off Th2 cells. It is also responsible for maintaining the epithelial integrity through short chain fatty acid (SCFA) synthesis along with promotion of IgA class switching [58].
It is evident that role of gut microbiome is critical in protecting and preventing the host from disorders. Dysbiosis arises due to a disproportion in constitution and abundance of microbiota. Increase in infectious and decrease in beneficial microbial population can contribute to dysbiosis. An important consequence of dysbiosis is the loss of epithelial integrity. Without the presence of a functional barrier, intestinal permeability is distorted, allowing entry of foreign antigens which trigger an immune response. This lack of epithelial integrity is involved in many disorders including asthma. Activation of self-reactive immune cells, enzymatic production of epitopes, resistance of bacteria to their own inflammatory processes and alteration in production of antibodies are results of dysbiosis. Modifications in gut microbiome enhance the levels of IgE, activation of invariant Natural Killer T (iNKT) cells synthesising IL-4 and IL-13 which independently cause isotype switching of IgE to IgA, accompanied by profusion of circulating basophils and mast cells. Exposure to gut microbiota reducing the levels of iNKT in mice have been observed. Likelihood of an adult developing asthma later in life increases with dysbiosis during infancy [58]. Affluence of various microbial families in asthma has been described in table 3. Among these, a low distribution of Bifidobacterium, Lactobacilli, Akkermansia and Faecalibacterium can amplify the probability of child developing asthma [66].
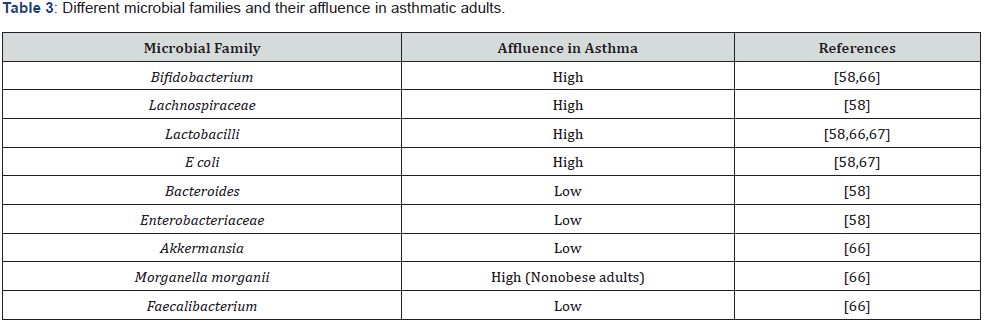
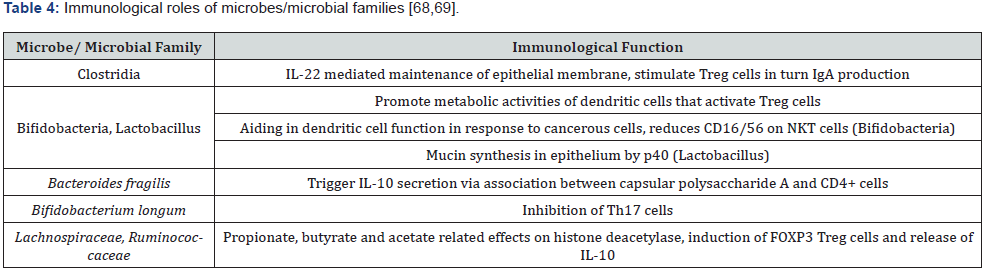
Table 4 elucidates the immunological impact of microbes and microbial families. In asthmatics, Escherichia coli, Lactobacillus vaginalis, and Morganella morganii were shown to release histamine which may play a role in sustaining the allergic responses [68]. Composition of microflora varies with different stages of childhood. Its association with asthma in turn differs as given in table 5. Interestingly, occurrence of Clostridium difficile in children correlated with hospitals deliveries and C-sections with increased chances of acquiring asthma as well eczema when born to atopic individuals [58]. Culture samples were distinct between C-sections and normal delivery with former having lower counts of Bifidobacterium, Bacteroides and relatively higher in Staphylococcus, Streptococccus [62]. It is noted that diversity of microbial colonisation can have different effects at different periods of infancy. When microbial profile was compared between healthy adults and five-year-old asthmatic children, there was a paradigm shift in nature and abundance of composition. This has been depicted in table 6.


Asthmatic mothers can impact the composition of gut microbiota of the offspring in a gender-specific manner. The research conducted by Koleva PT et al. identified a higher occurrence of Bacteriodaceae and lower occurrence of Lactobacillus in female and male infants respectively, at 4 months of age. The alterations could be a susceptibility factor for acquiring asthma. Microbial remnants from elder siblings, on the other hand, could be beneficial in conferring an immunoprotective state against asthma [71]. Early-life exposure to antibiotics such as Vancomycin and Streptomycin can transform the microbiota constituents with a reduction in Clostridium and Bacteriodaceae in addition to depletion of regulatory cells [72].
Microbiota-based Remedies
Objective of microbiota-based remedies is to lessen overgrowth of certain microbes thus reinstituting the flora. Probiotics, prebiotics, and synbiotics represent the means for microbiota modulation [62,73].
Probiotics
Probiotics are live, active microorganism cultures that can be prescribed to improve and maintain the intestinal biota [73]. The quantity and schedule of prescription in addition to existing microbial population determine the usefulness of probiotics 62]. A well-documented bacterium in designing probiotic is Lactobacillus rhamnosus GG (LGG) that has proven to inhibit MMP9 [74,75], prevent intrusion of immune cells, reduce levels of eNO in children and Ovalbumin sensitised responses in mice [76]. Similarly, Lactobacillus rhamnosus reduced hyperresponsiveness, cytokines and strengthened gut microbiota [77]. Bifidobacterium lactis has been shown to decrease IgE levels, eosinophils and trigger of Treg cells in a mice model [74]. Bifidobacterium breve M-16V has been demonstrated to inhibit Th2 responses and regulate Th1/Th2 balance [73].
Dispense of atopic asthmatic children with Trilac (1.6 × 109 lactic acid bacteria cells: Lactobacillus acidophilus - 37.5%, Bifidobacterium bifidum - 37.5% and Lactobacillus delbrueckii subsp. bulgaricus - 25%) resulted in fewer attacks, better pulmonary ability, higher monocytic HLA-DR and lower CD8/ CD45RA+ cells [78]. A randomized trial employed the use of Bifidobacterium lactis (Probio-M8 powder) as an additive to Budesonide/formoterol (Symbicort Turbuhaler) to evaluate the effects on asthmatics. Reduction in nitric oxide and increase in relative abundance of Bifidobacterium, Prevotella species and their associated metabolites indicate a promising therapeutic intervention [79]. Bacterial derivatives such as flagellin and endotoxin repress asthma in experimental models by recruiting Treg cells or ubiquitin-modifying enzyme A20 [62].
Prebiotics
Prebiotics are specific substances that are metabolised by microbes [73]. Galacto-oligosaccharide (GOS) and fructooligosaccharide (FOS) containing prebiotics offered protection against asthma in infants. However, data related to benefits of prebiotics in asthma is limited [62]. Human breast milk is enriched with nutrients, human milk oligosaccharides (HMOs), microbes and hormones. Once ingested, HMOs can act as prebiotics that can affect the immune system. HMOs get distributed to different organs and create a cross-talk between different immunological barriers. When this cross-talk occurs between the pulmonary barrier, HMOs could potentially guide the mucosa to confer immunity [80].
Synbiotics
Synbiotics is a mixture of prebiotic substrates and probiotic cultures. A combination of Bifidobacterium breve and galacto/ fructooligosaccharide alleviated asthmatic symptoms in children with atopic dermatitis [81]. Hydrolysed casein together with L. rhamnosus GG enhanced the endurance of the infant gut microbiome in response to bovine milk allergy [62]. The period of administration (prenatal or postnatal) might be an important factor for efficiency of biotics [62].
Curcumin in Treatment of Asthma
Curcumin or diferuloylmethane is a phytocompound rich in polyphenols, oils, saccharides and proteins obtained from the rhizome of Curcuma longa. It is a renowned medication in regions of Asia indicated in cancer, asthma, arthritis, cardiovascular and gastrointestinal diseases. Curcumin exhibits antioxidant, anti-tumoral, antimicrobial and anti-inflammatory effects [82- 84]. As a pharmacologic agent, it has spasmolytic properties via hypothesised blockage of calcium ion channels in addition to a differentiable range of vasoconstriction and vasodilation properties [85]. The bioavailability of curcumin is considerably low which disrupts its distribution and consequently therapeutic actions. Construction of nanoparticle-based curcumin could be a novel approach in improving pharmacodynamics and thus its efficacy [86]. At the molecular level, it suppresses the release of cytokines TNF-α, IL-6, IL-12, IL-1 and NF-κB. It also inhibits the synthesis of monocyte chemotactic proteins 1,3 and eotaxin from bronchial muscles [83]. It interferes with angiotensin converting enzyme (ACE), granulocyte-macrophage colony-stimulating factor (GM-CSF) and interferon gamma (IFN-γ). Contrastingly, it enhances production of IL-10 whose dysfunction is implicated in neurodegenerative, allergic and autoimmune disorders [87].
Curcumin, at the microbiota, induces proliferation of beneficial microbes Bifidobacteria, Lactobacilli while inhibiting that of Prevotellaceae, Coriobacterales, Enterobacteria, and Rikenellaceae thus varying the microbial ratio of beneficial to harmful microbes promoting a healthy microflora. Furthermore, it regulates epithelial integrity counteracting IL-1β [84]. Microbiota can release lipopolysaccharide (LPS) into circulation upon disorganisation of intestinal barrier which has been associated with several disorders. Curcumin decreases the amount of LPS thus ameliorating the inflammatory condition [88]. Curcumin has a remarkable antiviral activity against RSV via proteosome, NF-κB inhibition and phosphorylation of eIF2α and PKR, which might be beneficial in prevention of virus-induced asthma [82,89].
In an ovalbumin sensitized murine model, curcumin demonstrated to reduce IL-4,5, eotaxin, TNF and heat shock protein 70 and enhance aquaporins AQP 1,5 resolving inflammation and oedema [90]. Another investigation with the same model analysed the efficacy of tetrahydrocurcumin, a metabolite of curcumin, in reversal of airway inflammation through exerting influence on intestinal microbiota by faecal microbiota transplantation technique. Results denoted a decrease in Proteobacteria, Ruminococcaceae, Intestinimonas and Lachnospiraceae and Th2 induced actions [91]. Additionally, tetrahydrocurcumin in combination with dexamethasone synergistically relived asthmatic symptoms along with reduction in Th2, Th17 counts as well as IL-4,5 [92]. The usage of LGG and turmeric extract as a synbiotic in house dust mite (HDM) allergised mice model revealed a decrease in Th2, Th17, eosinophils, IL-5, IL-13, CCL17 and an increase in Treg [93].
Conclusion
Atopic asthma is a multifactorial disorder which occurs as an exaggerated response of the immune system to aeroallergens. Components of cellular and humoral immune systems trigger a cascade of events resulting in bronchospasm, oedema, epithelial damage and airway remodelling. This hypersensitive reaction is initiated by intrinsic (genetic mutations, familial predisposition, obesity) and extrinsic (pollutants, allergens, irritants) causes. Diagnosis is based on allergy and physiological testing, radiological examination, haematological analysis, spirometry, expiratory methods and biomarkers. Currently available therapeutic intervention includes pharmacotherapy and immunotherapy. Pharmacotherapy aims for symptomatic relief employing different classes of drugs such as short-acting beta 2 agonists, long-acting beta 2 agonists, corticosteroids, leukotriene receptor antagonists, methylxanthines, anticholinergics, mast cell stabilizer and monoclonal antibodies. A regimen depending upon the stage of the disease has been prescribed to incorporate one or more therapeutics at a specific concentration and route of administration. Immunotherapy, on the other hand, delivers allergens subcutaneously or sublingually according to sensitivity profile of the individual. It thus alters the immune responses in vivo and subsequently the severity of the asthmatic attack. Human gut microbiota is defined as the microbial flora existing in the gastrointestinal tract. As embryogenesis occurs, the microbiota also undergoes development. Any variations during this period can bring about atopic disorders. Mode of delivery, formulabased feeding, having siblings; exposure to antibiotics, vitamin D, absence of pets and pollutants influence the differentiation of the microbiota. Host and microbial population thrive together in a mutually dependent relationship. This is substantiated by the role of microbiome in maintenance of physiological mechanisms and instigation of several diseases like inflammatory bowel disease, atopic asthma, diabetes, autism spectrum disorder, obesity and autoimmune diseases. Due to host and co-existing microbeimposed changes, the abundance and diversity of gut flora varies accounting for enterotypes. Role of gut microbiome in causation of atopic asthma stems from evidential data indicating that the microbiota modifies nature of immune responses and affects integrity of respiratory epithelium. Additionally, dysbiosis can impact epithelial permeability, aid self-reactive cells and modify antibody synthesis. Microbial profiling has revealed differences in microbial population between healthy individuals and asthmatics, abundance in various stages of asthma, affluence in asthma and influence on immunological system. Furthermore, composition of microbiota was found to differ with mode of delivery, asthmatic status of mothers, presence of elder siblings and exposure to antibiotics. In order to establish an equilibrium between beneficial and harmful microbes hence abetting occurrence and severity of atopic asthma, microbiota-based remedies like probiotics, prebiotics and synbiotics are recommended. Examples include Lactobacillus rhamnosus GG, oligosaccharides and Trilac. Apart from the conventional treatment modalities, traditional medicine is being extensively explored as a safe and effective alternative. Curcumin, a phytochemical obtained from the rhizome of Curcuma longa, shows anti-inflammatory, antimicrobial and antioxidant properties. It interferes with the actions of cytokines and increases abundance of beneficial microbes in the gut. Curcumin can also be incorporated with pharmacological agents or probiotics to synergistically improve efficacy. From this study, it is evident that natural products capable of interacting with and modifying the gut microbiota might be promising agents for treatment of atopic asthma. Future directions must focus on discovery and validation of traditional medicine compounds that resolve the condition from the level of microbiota.
Conflict of Interest
Authors declare that they have no conflict of interest.
References
- Yeh SY, Schwartzstein R (2009) Asthma: pathophysiology and diagnosis. In: Harver A, Kotses H, (Eds.), A Public Heal Perspect. Asthma Heal Soc 19-42.
- Lemanske Jr RF, Busse WW (2010) Asthma: clinical expression and molecular mechanisms. J Allergy Clin Immunol 125(2 Suppl 2): S95-S102.
- Rashmi R, Kumar P, Srivastava S, Muhammad T (2021) Understanding socio-economic inequalities in the prevalence of asthma in India: an evidence from national sample survey 2017-18. BMC Pulm Med 21(1): 372.
- Kaufman G (2011) Asthma: pathophysiology, diagnosis and management. Nurs Stand 26(5): 48-56; quiz 58.
- Ying S, Zhang G, Gu S, Zhao J (2006) How much do we know about atopic asthma: where are we now? Cell Mol Immunol 3(5): 321-332.
- Ronchetti R, Jesenak M, Rennerova Z, Barreto M, Ronchetti F, et al. (2009) Relationship between atopic asthma and the population prevalence rates for asthma or atopy in children: atopic and nonatopic asthma in epidemiology. In: Allergy and asthma proceedings. OceanSide Publications, UK, 30(1): 55-63.
- McKeever TM, Britton J (2004) Diet and asthma. Am J Respir Crit Care Med 170(7): 725-729.
- Koren HS (1997) Environmental risk factors in atopic Asthma. Int Arch Allergy Immunol 113(1-3):65-68.
- Dorward AJ, Colloff MJ, Mac Kay NS, Mc Sharry C, Thomson NC (1988) Effect of house dust mite avoidance measures on adult atopic asthma. Thorax 43(2): 98-102.
- Schwartz DA (2001) Does inhalation of endotoxin cause asthma? Am J Respir Crit Care Med 163(2): 305-306.
- Beasley R, Semprini A, Mitchell EA (2015) Risk factors for asthma: is prevention possible? Lancet 386(9998): 1075-1085.
- Noutsios GT, Floros J (2014) Childhood asthma: causes, risks, and protective factors; a role of innate immunity. Swiss Med Wkly 144: w14036.
- Ellwood P, Asher MI, Garcia-Marcos L, Williams H, Keil U, et al (2013) Do fast foods cause asthma, rhinoconjunctivitis and eczema? Global findings from the International Study of Asthma and Allergies in Childhood (ISAAC) Phase Three. Thorax. 68(4): 351-360.
- Willers SM, Devereux G, Craig LC, McNeill G, Wijga AH, et al. (2007) Maternal food consumption during pregnancy and asthma, respiratory and atopic symptoms in 5-year-old children. Thorax 62(9): 773-779.
- Ellwood P, Asher MI, Bjorksten B, Burr M, Pearce N, et al. (2001) Diet and asthma, allergic rhinoconjunctivitis and atopic eczema symptom prevalence: an ecological analysis of the International Study of Asthma and Allergies in Childhood (ISAAC) data. Eur Respir J 17(3): 436-443.
- Arbes SJ (2012) Do all asthmatics with atopy have atopic asthma? J Allergy Clin Immunol 130(5): 1202-1204.
- Kudo M, Ishigatsubo Y, Aoki I (2013) Pathology of asthma. Front Microbiol 4: 263.
- Ishmael FT (2011) The inflammatory response in the pathogenesis of asthma. J Osteopath Med 111(s117): 11-17.
- Holgate ST (2008) Pathogenesis of Asthma. Clin Exp Allergy 38(6): 872-897.
- Trejo Bittar HE, Doberer D, Mehrad M, Strollo DC, Leader JK, et al. (2017) Histologic findings of severe/therapy-resistant asthma from video-assisted thoracoscopic surgery biopsies. Am J Surg Pathol 41(2): 182-188.
- Nieuwenhuis MA, Siedlinski M, van den Berge M, Granell R, Li X, et al. (2016) Combining genomewide association study and lung eQTL analysis provides evidence for novel genes associated with asthma. Allergy 71(12): 1712-1720.
- Akhabir L, Sandford AJ (2011) Genome-wide association studies for discovery of genes involved in asthma. Respirology. 16(3): 396-406.
- Kim KW, Kim DY, Yoon D, Kim KK, Jang H, et al. (2022) Genome-wide association study identifies TNFSF15 associated with childhood asthma. Allergy 77(1): 218-229.
- Bijanzadeh M, Mahesh PA, Ramachandra NB (2011) An understanding of the genetic basis of asthma. Indian J Med Res 134(2): 149-161.
- Edwards MR, Bartlett NW, Hussell T, Openshaw P, Johnston SL (2012) The microbiology of asthma. Nat Rev Microbiol 10(7): 459-471.
- Friedlander SL, Busse WW (2005) The role of rhinovirus in asthma exacerbations. J Allergy Clin Immunol 116(2): 267-273.
- Sly PD, Kusel M, Holt PG (2010) Do early-life viral infections cause asthma? J Allergy Clin Immunol 125(6): 1202-1205.
- Ali Z, Ulrik CS (2013) Obesity and asthma: A coincidence or a causal relationship? A systematic review. Respir Med 107(9): 1287-1300.
- Weiland SK, Husing A, Strachan DP, Rzehak P, Pearce N (2004) Climate and the prevalence of symptoms of asthma, allergic rhinitis, and atopic eczema in children. Occup Environ Med 61(7): 609-615.
- Henderson AJ, Warner JO (2012) Fetal origins of asthma. Semin Fetal Neonatal Med 17(2): 82-91.
- Bacharier LB, Boner A, Carlsen KH, Eigenmann PA, Frischer T, et al. (2008) Diagnosis and treatment of asthma in childhood: a PRACTALL consensus report. Allergy 63(1): 5-34.
- Berkman N, Avital A, Breuer R, Bardach E, Springer C, et al. (2005) Exhaled nitric oxide in the diagnosis of asthma: comparison with bronchial provocation tests. Thorax 60(5): 383-388.
- Barbinova L, Baur X (2006) Increase in exhaled nitric oxide (eNO) after work-related isocyanate exposure. Int Arch Occup Environ Health 79(5): 387.
- Brannan JD, Koskela H, Anderson SD (2007) Monitoring asthma therapy using indirect bronchial provocation tests*. Clin Respir J 1(1): 3-15.
- Leuppi JD (2014) Bronchoprovocation tests in asthma: direct versus indirect challenges. Curr Opin Pulm Med 20(1): 31-36.
- Chhabra SK (2015) Clinical application of spirometry in asthma: Why, when and how often? Lung India 32(6): 635-637.
- Szefler SJ, Wenzel S, Brown R, Erzurum SC, Fahy JV, et al. (2012) Asthma outcomes: Biomarkers. J Allergy Clin Immunol 129(3 Supplement): S9-S23.
- Tiotiu A (2018) Biomarkers in asthma: state of the art. Asthma Res Pract 4(1):10.
- Licari A, Castagnoli R, Brambilla I, Marseglia A, Tosca MA, et al. (2018) Asthma endotyping and biomarkers in childhood asthma. Pediatr Allergy Immunol Pulmonol 31(2): 44-55.
- Zissler UM, Esser-von Bieren J, Jakwerth CA, Chaker AM, Schmidt-Weber CB (2016) Current and future biomarkers in allergic asthma. Allergy 71(4): 475-494.
- Barnes PJ (2006) How corticosteroids control inflammation: Quintiles Prize Lecture 2005. Br J Pharmacol 148(3):245-254.
- Tilley SL (2011) Methylxanthines in asthma. Handb Exp Pharmacol (200): 439-456.
- Aaron S, Aaron SD (2001) The use of ipratropium bromide for the management of acute asthma exacerbation in adults and children: a systematic review. J Asthma 38(7): 521-530.
- Rodrigo GJ, Rodrigo C (2000) First-line therapy for adult patients with acute asthma receiving a multiple-dose protocol of ipratropium bromide plus albuterol in the emergency department. Am J Respir Crit Care Med 161(6): 1862-1868.
- Sinniah A, Yazid S, Flower RJ (2017) The anti-allergic cromones: past, present, and future. Front Pharmacol.
- Damato G, Liccardi G, Noschese P, Salzillo A, Damato M, et al. (2004) Anti-IgE monoclonal antibody (omalizumab) in the treatment of atopic asthma and allergic respiratory diseases. Curr Drug Targets-Inflammation Allergy 3(3): 227-279.
- Yukselen A, Kendirli SG (2014) Role of immunotherapy in the treatment of allergic asthma. World J Clin Cases 2(12): 859-865.
- Tosca MA, Licari A, Olcese R, Marseglia G, Sacco O, et al. (2018) Immunotherapy and Asthma in Children. Front Pediatr 6.
- Tabar AI (2017) Specific allergen immunotherapy for the treatment of allergic asthma: a review of current evidence. J Investig Allergol Clin Immunol 27(1): 1-35.
- Bosnjak B, Stelzmueller B, Erb KJ, Epstein MM (2011) Treatment of allergic asthma: Modulation of Th2 cells and their responses. Respir Res 12(1): 114.
- Yoshihara S, Ono M, Yamada Y, Fukuda H, Abe T, et al. (2009) Early intervention with suplatast tosilate for prophylaxis of pediatric atopic asthma: A pilot study. Pediatr Allergy Immunol 20(5): 486-492.
- Epstein MM (2006) Targeting memory Th2 cells for the treatment of allergic asthma. Pharmacol Ther 109(1): 107-136.
- Hothersall EJ, Chaudhuri R, McSharry C, Donnelly I, Lafferty J, et al. (2008) Effects of atorvastatin added to inhaled corticosteroids on lung function and sputum cell counts in atopic asthma. Thorax 63(12): 1070-1075.
- Gariboldi S, Palazzo M, Zanobbio L, Dusio GF, Mauro V, et al. (2009) Low dose oral administration of cytokines for treatment of allergic asthma. Pulm Pharmacol Ther 22(6): 497-510.
- Erin EM, Leaker BR, Nicholson GC, Tan AJ, Green LM, et al. (2006) The Effects of a Monoclonal Antibody Directed against Tumor Necrosis Factor-Alpha in Asthma. Am J Respir Crit Care Med 174(7): 753-762.
- Boyle RJ, Pedroletti C, Wickman M, Bjermer L, Valovirta E, et al. (2012) Nocturnal temperature controlled laminar airflow for treating atopic asthma: a randomised controlled trial. Thorax 67(3): 215-221.
- Joos S, Schott C, Zou H, Daniel V, Martin E (2000) Immunomodulatory effects of acupuncture in the treatment of allergic asthma: a randomized controlled study. J Altern Complement Med 6(6): 519-525.
- Salameh M, Burney Z, Mhaimeed N, Laswi I, Yousri NA, et al. (2020) The role of gut microbiota in atopic asthma and allergy, implications in the understanding of disease pathogenesis. Scand J Immunol 91(3): e12855.
- Barko PC, McMichael MA, Swanson KS, Williams DA (2018) The gastrointestinal microbiome: a review. J Vet Intern Med 32(1): 9-25.
- Stiemsma LT, Turvey SE (2017) Asthma and the microbiome: defining the critical window in early life. Allergy, Asthma Clin Immunol 13(1): 3.
- Sbihi H, Boutin RC, Cutler C, Suen M, Finlay BB, et al. (2019) Thinking bigger: How early-life environmental exposures shape the gut microbiome and influence the development of asthma and allergic disease. Allergy 74(11): 2103-2115.
- Pascal M, Perez-Gordo M, Caballero T, Escribese MM, Lopez Longo MN, et al. (2018) Microbiome and allergic diseases. Fron Immunol 9: 1584.
- van Nimwegen FA, Penders J, Stobberingh EE, Postma DS, Koppelman GH, et al. (2011) Mode and place of delivery, gastrointestinal microbiota, and their influence on asthma and atopy. J Allergy Clin Immunol 128(5): 948-955.e1-e3.
- Durack J, Lynch SV (2019) The gut microbiome: Relationships with disease and opportunities for therapy. J Exp Med. 216(1): 20-40.
- Arumugam M, Raes J, Pelletier E, Le Paslier D, Yamada T, et al. (2011) Enterotypes of the human gut microbiome. Nature. 473(7346): 174-180.
- Huang YJ, Marsland BJ, Bunyavanich S, O’Mahony L, Leung DY, et al. (2017) The microbiome in allergic disease: Current understanding and future opportunities-2017 PRACTALL document of the American Academy of Allergy, Asthma & Immunology and the European Academy of Allergy and Clinical Immunology. J Allergy Clin Immunol 139(4): 1099-1110.
- Okba AM, Saber SM, Abdel-Rehim AS, Amin MM, Mohamed DA (2018) Fecal microbiota profile in atopic asthmatic adult patients. Eur Ann Allergy Clin Immunol 50(3): 117-124.
- Smolinska S, Groeger D, O’Mahony L (2017) Biology of the microbiome 1: interactions with the host immune response. Gastroenterol Clin 46(1): 19-35.
- Sokolowska M, Frei R, Lunjani N, Akdis CA, O’Mahony L (2018) Microbiome and asthma. Asthma Res Pract 4(1): 1.
- Melli L, do Carmo-Rodrigues MS, Araújo-Filho HB, Sole D, De Morais MB (2016) Intestinal microbiota and allergic diseases: A systematic review. Allergol Immunopathol (Madr) 44(2): 177-188.
- Stokholm J, Blaser MJ, Thorsen J, Rasmussen MA, Waage J, et al (2018) Maturation of the gut microbiome and risk of asthma in childhood. Nat Commun 9(1): 141.
- Russell SL, Gold MJ, Hartmann M, Willing BP, Thorson L, et al. (2012) Early life antibiotic‐driven changes in microbiota enhance susceptibility to allergic asthma. EMBO Rep 13(5): 440-447.
- Meirlaen L, Levy EI, Vandenplas Y (2021) Prevention and Management with pro-, pre and synbiotics in children with asthma and allergic rhinitis: a narrative review. Nutrients 13(3): 934.
- Feleszko W, Jaworska J, Rha RD, Steinhausen S, Avagyan A, et al. (2007) Probiotic-induced suppression of allergic sensitization and airway inflammation is associated with an increase of T regulatory-dependent mechanisms in a murine model of asthma. Clin Exp Allergy 37(4): 498-505.
- Spacova I, Van Beeck W, Seys S, Devos F, Vanoirbeek J, et al. (2020) Lactobacillus rhamnosus probiotic prevents airway function deterioration and promotes gut microbiome resilience in a murine asthma model. Gut Microbes 11(6): 1729-1744.
- Mennini M, Dahdah L, Artesani MC, Fiocchi A, Martelli A (2017) Probiotics in Asthma and Allergy Prevention. Front Pediatr 5:165.
- Yu J, Jang SO, Kim BJ, Song YH, Kwon JW, et al. (2010) The effects of Lactobacillus rhamnosus on the prevention of asthma in a murine model. Allergy Asthma Immunol Res 2(3): 199-205.
- Gutkowski P, Madaliński K, Grek M, Dmenska H, Syczewska M, et al. (2010) Clinical immunology Effect of orally administered probiotic strains Lactobacillus and Bifidobacterium in children with atopic asthma. Cent Eur J Immunol 35(4): 233-238.
- Liu A, Ma T, Xu N, Jin H, Zhao F, et al. (2021) Adjunctive probiotics alleviates asthmatic symptoms via modulating the gut microbiome and serum metabolome. Microbiol Spectr 9(2): e00859-e00921.
- Moossavi S, Miliku K, Sepehri S, Khafipour E, Azad MB (2018) The prebiotic and probiotic properties of human milk: implications for infant immune development and pediatric asthma. Front Pediatr 6:197.
- van der Aa LB, van Aalderen WM, Heymans HS, Sillevis Smitt JH, Nauta AJ, et al. Synbiotics prevent asthma-like symptoms in infants with atopic dermatitis. Allergy 66(2): 170-177.
- Moghadamtousi SZ, Kadir HA, Hassandarvish P, Tajik H, Abubakar S, et al. (2014) A review on antibacterial, antiviral, and antifungal activity of curcumin. In: Carvalho JCT, (Ed.), Biologic Activity and Biotechnological Development of Natural Products 2014. Biomed Res Int 2014: 186864.
- Kim DH, Phillips JF, Lockey RF (2011) Oral curcumin supplementation in patients with atopic asthma. Allergy Rhinol (Providence) 2(2): e51-e53.
- Scazzocchio B, Minghetti L, D’Archivio M (2020) Interaction between gut microbiota and curcumin: a new key of understanding for the health effects of curcumin. Nutrients 12(9):2499.
- Gilani AH, Shah AJ, Ghayur MN, Majeed K (2005) Pharmacological basis for the use of turmeric in gastrointestinal and respiratory disorders. Life Sci 76(26): 3089-3105.
- Flora G, Gupta D, Tiwari A (2013) Nanocurcumin: a promising therapeutic advancement over native curcumin. Crit Rev Ther Drug Carrier Syst 30(4): 331-368.
- Mollazadeh H, Cicero AF, Blesso CN, Pirro M, Majeed M, et al. (2019) Immune modulation by curcumin: The role of interleukin-10. Crit Rev Food Sci Nutr 59(1): 89-101.
- Ghosh SS, He H, Wang J, Gehr TW, Ghosh S (2018) Curcumin-mediated regulation of intestinal barrier function: the mechanism underlying its beneficial effects. Tissue Barriers 6(1): e1425085.
- Obata K, Kojima T, Masaki T, Okabayashi T, Yokota S, et al. (2013) Curcumin prevents replication of respiratory syncytial virus and the epithelial responses to it in human nasal epithelial cells. PLoS One 8(9): e70225.
- Shahid H, Shahzad M, Shabbir A, Saghir G (2019) Immunomodulatory and anti-inflammatory potential of curcumin for the treatment of allergic asthma: effects on expression levels of pro-inflammatory cytokines and aquaporins. Inflammation 42(6): 2037-2047.
- Wu Y, Chen Y, Li Q, Ye X, Guo X, et al. (2021) Tetrahydrocurcumin alleviates allergic airway inflammation in asthmatic mice by modulating the gut microbiota. Food Funct 12(15): 6830-6840.
- Wu YF, Chen YQ, Li Q, Ye XY, Zuo X, et al. (2020) Supplementation with tetrahydrocurcumin enhances the therapeutic effects of dexamethasone in a murine model of allergic asthma. Int Arch Allergy Immunol 181(11): 822-830.
- Ghiamati Yazdi F, Zakeri A, Ark I van, Leusink-Muis T, Braber S, et al. (2020) Crude turmeric extract improves the suppressive effects of lactobacillus rhamnosus GG on allergic inflammation in a murine model of house dust mite-induced asthma. Front in Immunol 11: 1092.






























