Cerebral Venous Thrombosis Secondary to Hyperthyroidism: A Case Report
Malika Bajracharya, Avinash Chandra, Ramita Bati, Reema Rajbhadari, Sameer Acharya, Pranaya Shrestha, Resha Shrestha, Pravesh Rajbhandari, Robin Bhattarai and Basant Pant*
1Annapurna Neurological Institute and Allied Sciences, Maitighar, Nepal
Submission: March 12, 2017; Published: March 26, 2018
*Corresponding author: Basant Pant, Annapurna Neurological Institute and Allied Sciences, Maitighar, Nepal, Email: neuronepal@wlink.com.npHow to cite this article: Malika B, Avinash C, Ramita B, Reema R, Basant P,et.al. Cerebral Venous Thrombosis Secondary to Hyperthyroidism: A Case Report. Curr Trends Biomedical Eng & Biosci. 2018; 14(2): 555885.DOI:10.19080/CTBEB.2018.14.555885
Abstract
Cerebral Venous Thrombosis (CVT) is a rare form of Stroke characterized by thrombus formation in the cerebral veins. CVT is a result of various reasons among which the hyperthyroidism is not so frequently encountered. This is probably the first case report published from Nepal. The aim of this case report is to give the message that persistent severe headache in patient with hyperthyroidism can be the red flag and needs to be investigated further. We present a case of a 35 years old female who presented with complaints of severe headache and persistent in nature associated with vomiting since 5 days. She was a diagnosed subacute thryroiditis and under medicine from 1 month before presenting to us. Her Magnetic Resonance Venography (MRV) brain showed venous thrombosis within superior saggital sinus, left transverse sinus and sigmoid sinus.Her thyroid function test showed pretreatment T3 of 2.98ng/ml T4 of 1.02mg/ml and TSH of 0.12μIU/L. She was kept on anticoagulants and other supportive measures. The patient showed improving status with the conservative management.
Keywords: Cerebral venous thrombosis; Hyperthyroidism; Seizure; Headache.
Introduction
Headache is the most common presenting features seen in almost 90% of the cases in Cerebral Venous Throbosis. Headache is usually diffused and often progresses in severity over days to weeks [1]. Cerebral Venous Thrombosis is an uncommon form of Stroke, usually affecting young female individuals. It represents 0.5% to 1% of all strokes. Risk factors for CVT includes, antithrombin III, protein C, protein S deficiency, antiphospholipid and anticardiolipin antibodies, factor V leiden gene mutation, hyperhomocysteinemia, pregnancy and puerperium, oral contraceptives, cancer [2]. Clinical findings of CVT falls into 2 major categories; i) Those that are related to increased intracranial pressure attributable to impaired venous drainage and ii) Those that are related to venous ischemia/infarction or hemorrhage.3 CVT is an important diagnostic consideration in patients with persistent headache and papilledema or diplopia ( caused by sixth nerve palsy). When focal brain injuries occur due to venous ischemia or hemorrhage then neurological sign and symptoms referable to the affected region as often present. Most commonly involved is the superior saggital sinus which presents with headache and papilledema. A motor deficit sometime with seizure can also occur. Dilated scalp veins and scalp oedema may be seen on examination.
Case Report
35 years old female, presented to the emergency with the chief complaints of headache since 1 month which had increased in severity progressively since 5 days. Headache was more over the frontal region and was throbbing in nature. It was associated with multiple episodes of vomiting. She also developed sudden onset weakness over the left half of the body since 1 day. Her history revealed that she was a diagnosed case of subacute thyroiditis 1 month back for which she was kept on carbimazole but not well controlled. The history also revealed that she had been suffering from hyperthyroidism from last several years but not taking medication. She had no history of taking contraceptive pills or other medications. She was non smoker and no other medical issue. She was married and had one child. There was no family history suggestive of any medical illnesses. On examination her motor power was 5/5 in the right upper and lower limb and 1/5 in the left upper limb and 2/5 in the left lower limb. Deep tendon reflexes were normal and her sensory system was intact. Her respiratory, cardiovascular and per abdomen findings showed no abnormal findings. On investigations her total counts was 11300/cumm with neutrophil of 88%, ESR 25mm/ 1st hour. Her kidney function test, liver function tests were within normal limit. Thyroid function test showed FT3 2.98 ng/ml, FT4 1.02mg/ml, TSH 0.12 μIU/L. Her bleeding profile showed bleeding time of 3 minutes, clotting time of 7 minutes and INR of 1.0. Echocardiography was done which did not show any thrombi. Carotid artery Doppler was done that did not show any abnormality. MRV was done which revealed thrombosed veins (superior saggital sinus, left transverse sinus and Sigmoid sinus), and irregular straight sinus attenuated in the center and partially thrombosed (Figure 1).
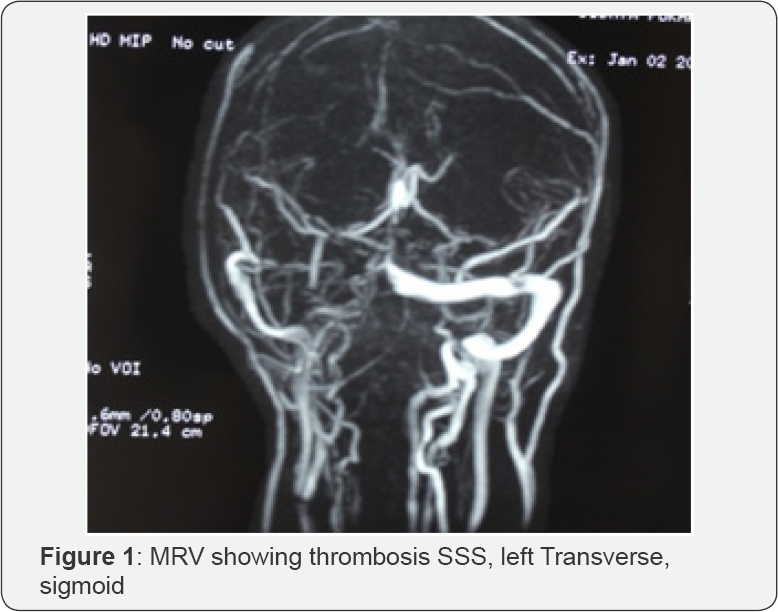
We kept her on anticoagulant, warfarin was started and dose adjustment was made monitoring her INR. Carbimazole was continued in the dose of 5mg per day. On the day of admission she developed multiple episodes of Generalized Tonic Clonic seizure. We kept her on anti epileptic drug Levetiracetam. She did not develop seizure after that. She was started on low molecular heparin 60mg q 12 hourly for few days and bridged with warfarin 5mg once a day dosage. She improved significantly, and was later on discharged with oral warfarin, carbimazole and levetiracetam. She was cheduled for foullow up for regular PT/ INR monitoring. Her MRV was scheduled for 10 days later to see the evidence of recanalization.
Discussion
Hyperthyroidism is found to be associated with CVT as it is found to be associated with hypercoagulable states although the exact mechanism is not known. Increased thyroid hormones may enhance coagulation factor synthesis or secretion or may decrease fibrinolysis [3]. Several studies of hyperthyroidism show increased incidence of thromboembolic events.3 Increased level of fT4 is associated with increased synthesis and secretion of factor VIII. In overt hyperthyroidism, cardioembolic stroke is clearly associated to thyrotoxic atrial fibrillation [4], and in subclinical hyperthyroidism with serum thyroid-stimulating hormone levels 0.1μU/L, the incidence of atrial fibrillation is increased [5]. The risk of atherosclerosis is also seen, although not clearly established [6]. Abnormalities in the coagulation such as increased fibrinogen, von wilibrand factor, plasminogen inhibitor activator 1, coagulation factor VIII, IX and X and decreased activated plasma thromboplastin time (APTT) have been found in hyperthyroid patients[7].
Conclusion
Several cases on Cerebral Venous Thrombosis due to different mechanisms have been reported. Some studies and case reports reveal that high thyroxin level is associated with hypercoagulable states and atrial fibrillation thereby increasing the chances of hemodynamic derangement going on inside the patient. Any patient presenting to us with headache and the history of hyperthyroidism, should be suspected for cerebral venous thrombosis and subsequently blood screening for coagulation profile should be done.
References
- Einhaupl K, Stam J, Bousser MG, De Bruijn SF, Ferro JM, et al. (2010) EFNS guideline on the treatment of cerebral venous and sinus thrombosis in adult patients. Eur J Neurol 17(10): 1229-1235.
- Franchini M, Lippi G, Manzato F, Vescovi PP, Targher G (2010) Hemostatic abnormalities in endocrine and metabolic disorders. Eur J Endocrinol162(3): 439-451.
- Ferro JM, Canhao P, Stam J, Bousser MG (2004) ISCVT Investigators Prognosis of cerebral vein and dural sinus thrombosis: results of the international study on cerebral vein and dural sinus thrombosis (ISCVT). Stroke 35: 664-670.
- Kootte RS, Stuijver DJ, Dekkers OM, van Zaane B, Fliers E, et al. (2012) The incidence of venous thromboembolism in patients with overt hyperthyroidism: a retrospective multicentre cohort study. Thromb Haemost 107(3): 417-422.
- Kraut E, Sarkar R, Houlden RL (2017) Cerebral venous thrombosis associated with graves hyperthyroidism. AACE Clinical Case Reports 3(1): e70-e3.
- Saposnik G, Barinagarrementeria F, Brown RD, Bushnell CD, Cucchiara B, Cushman M, et al. (2011) Diagnosis and management of cerebral venous thrombosis: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 42(4): 1158-1192.
- Squizzato A, Gerdes VEA, Brandjes DPM (2005) Thyroid diseases and Cerebrovascular disease. Stroke 36: 2302-2310.






























