A Review on: Stein-Leventhal Syndrome (SLS)
Nirav R Soni*
Department of Quality Assurance (QA), Gujarat Technological University (GTU), India
Submission: December 13, 2017; Published: January 24, 2018
*Corresponding author: Nirav R Soni, Department of Quality Assurance (QA), Gujarat Technological University (GTU), India, Email: nirav_sonic@yahoo.com
How to cite this article: Nirav R S. A Review on: Stein-Leventhal Syndrome (SLS). Curr Trends Biomedical Eng & Biosci. 2018; 11(3): 555812. DOI: 10.19080/ CTBEB.2018.10.555812.
Abstract
Stein-Leventhal Syndrome (SLS)” is the most common health problem that causes important distress to women and so many costs for healthcare accounting. In fact, SLS is mainly causes of female infertility. The symptoms of SLS are apparently unrelated to one another; changing definitions and a range of symptoms have made the path to diagnosis for many women difficult in the community remain undiagnosed. The National Institutes of Health (NIH) estimates that half percentage of women with SLS will become diabetic or pre-diabetic by age of fourty. There was various available studies shown that the women with SLS to be at higher risk for suicide as well as endometrial, ovarian and breast cancer. SLS affects the quality of life and can worsen anxiety and depression either due to the features of SLS or due to the diagnosis of a chronic sickness. The cause of SLS is not fully understood, but genetics may be a factor. SLS seems to run in families, so your chance of having it is higher if other women in your family have it or have irregular periods or diabetes. SLS can be passed down from either your mother’s or father’s side.
Keywords: Sign and symptoms; Management and lifestyle
Introduction
SLS is the most common hormonal disorder among women between the ages of 18 and 44. It is one of the leading causes of poor fertility. It is often associated with psychological impairments including depression and other mood disorders and metabolic derangements [1,2]. There are a number of definitions of SLS, the Rotterdam consensus is the most widely accepted across Europe, Asia and Australia was the definition used for the guideline. Polycystic means “many cysts,” and SLS regularly causes clusters of small, pearl-sized cysts in the ovaries [3]. The cysts are fluid-filled and immature eggs. SLS is also known as “Polycystic Ovary Syndrome (PCOS)”.1 Women with SLS produce a minute amount of male hormones known as androgens, which contribute to some of the symptoms of the condition [2-4]. To prevent this depressive symptoms, nobody can know how to progress symptoms during the infertility. We can utilize several techniques for own stress therapy, emphasizing baths, essential oils, and guided imagery, but all can be amazingly effective! Each woman must try out several and discover what works particularly well for her. If you feel specially down or stressed, be sure to ill assistance and to get your personal path to emotional, spiritual, and mental wellbeing etc [1-5].
Signs and symptoms of SLS
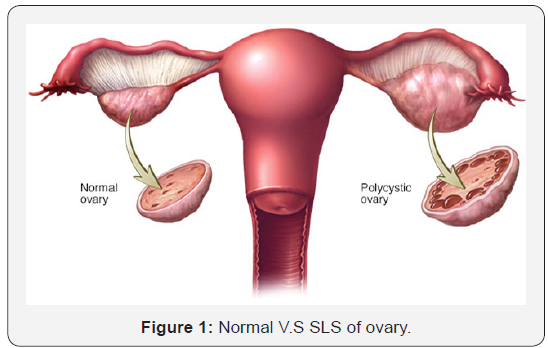
It includes irregular or absent of menstrual periods, it may be heavy periods ,facial hair and gain weight , acne or skin rashes, pelvic pain, difficulty getting pregnant, and patches of thick, darker, velvety skin. Associated with potential complications includes type-II diabetes, obesity, obstructive sleep apnea 1,4,5, heart disease 3, mood or behavior disorders and acanthosis nigricans, Hashimoto diseases, endometrial cancer and breast cancer [6]. Also, a large number of people diagnosed with rheumatoid arthritis (RA), multiple sclerosis and lupus combined [5]. Cysts may be detectable by ultrasound. Other conditions that produce similar symptoms involved adrenal hyperplasia, hyperprolactinemia and hypothyroidism [3-7]. 5-10% of women of childbearing age are affected and with <50% of women diagnosed. SLS is only responsible for 70% of infertility issues in women who have difficulty ovulating. Post-menopausal women can also suffer from SLS. Some studies have shown that approximately 40% of patients with diabetes between the ages of 20-50 have SLS. In addition, some studies have found that if a mother has SLS, there is a 50% chance that her daughter will have this syndrome. According to the “U.S. Department of Health and Human Services”, between 1/10 and 1/20 women of childbearing age suffers from SLS. The condition currently affects up to 5 million women in the same country [5-8] (Figure 1).
Current management option for SLS [9-15]
The management of SLS can include:
I. Lifestyle modifications: Increasing physical activity levels or yoga or gym and eating a healthy diet [6,12,14]
II. Weight reduction: Research has shown that even five to 10 % weight loss can provide significant health benefits [7,11,16-19]
III. Medical treatment 10-15: The oral contraceptive pill
IV. Hormonal medication: To block hormones like testosterone (for example, spironolactone) [18-23]
V. Infertility medications: Clomiphene citrate (sold as Clomid) or metformin may be taken orally to bring about ovulation. For infertility, “clomiphene” is first-line treatment. For metabolic disturbances and for improving menstrual regularities problem, Metformin is of limited or no benefit for managing abnormally facial hair growth is known as hirsutism, acne, or infertility. Overall, thiazolidinediones have not favourable riskbenefit ratio.
VI. Psychological counselling [11-17]
VII. Novel Therapy [12-14]: Pineol & inositol are currently in trials for the management option. The various reason for taking inositol based powder and other medications. Reduced Insulin Resistance , Reduced Testosterone, Less Unwanted Hair Growth , clearer skin, Increased Chances of Ovulation, Higher egg quality, Lower Chance of Gestational Diabetes, Healthier Liver, Reduced Appetite and Food Cravings, More Stable Mood, Help for Symptoms of Menopause 16, Less Inflammation and panic, Improved nerve function, lipolysis and cost effective [17- 24].
Conclusion
SLS continues to be a global health problem that presents major challenges to our health care systems. It indicates a much need for more public education and awareness on SLS in the country. In comparison with other complications remains one of the least understood and the most confusing medical conditions by health care public and also for the other population as well as the least funded hormonal disorder. Even World Health Organization (WHO), ACOG (American Congress of Obstetricians and Gynecologists) and National Institutes of Health (NIH) also mentioned in its report that in most of the countries where; SLS is a major public health concern. According to the scale of the public health problem, there must be a comprehensive approach to prevention and management of SLS is urgently required for the major fertility problem in women’s. Programs like surveillance and education must be delivered at the community and rural level through the primary health care system so as to increase public awareness about the problem and lengthen the survival of affected individuals and also prevent the general from becoming affected. The most important challenge is thus to improve the projection for implementation of research for the patients with SLS in developing countries. This study may benefit government to find a new vision and mission in control of SLS. So, our aim to explore the understanding and to Study the changes of the hormonal profile in SLS adolescents. Also, to manage lifestyle program on clinical symptoms of the adolescent SLS.
References
- Lujan ME, Jarrett BY, Brooks ED, Reines JK, Peppin AK, et al. (2013) Updated ultrasound criteria for polycystic ovary syndrome: reliable thresholds for elevated follicle population and ovarian volume. Hum Reprod 28(5): 1361-1368.
- Stepto NK, Cassar S, Joham AE, Hutchison SK, Harrison CL, et al. (2013) Women with polycystic ovary syndrome have intrinsic insulin resistance on euglycaemic-hyperinsulaemic clamp. Hum. Reprod. 28: 777-784.
- Yildiz BO, Bozdag G, Yapici Z, Esinler I, Yarali H (2012) Prevalence, phenotype and cardiometabolic risk of polycystic ovary syndrome under different diagnostic criteria. Hum Reprod 27(10): 3067-3073.
- Goodarzi MO, Dumesic DA, Chazenbalk G, Azziz R (2011) Polycystic ovary syndrome: etiology, pathogenesis and diagnosis. Nat Rev Endocrinol 7(4): 219-231.
- March WA, Moore VM, Willson KJ, Phillips DI, Norman RJ, et al. (2010) The prevalence of polycystic ovary syndrome in a community sample assessed under contrasting diagnostic criteria. Hum Reprod 25: 544– 551.
- Nicandri KF, Hoeger K (2012) Diagnosis and treatment of polycystic ovarian syndrome in adolescents. Curr Opin Endocrinol Diabetes Obes 19(6): 497-504.
- Wang ET, Cirillo PM, Vittinghoff E, Bibbins-Domingo K, Cohn BA, et al. (2011) Menstrual irregularity and cardiovascular mortality. J Clin Endocrinol Metab 96: E114-E118.
- Dokras A, Clifton S, Futterweit W, Wild R (2011) Increased risk for abnormal depression scores in women with polycystic ovary syndrome: a systematic review and meta-analysis. Obstet Gynecol 117(1): 145-152.
- Teede H, Deeks A, Moran L (2010) Polycystic ovary syndrome: a complex condition with psychological, reproductive and metabolic manifestations that impacts on health across the lifespan. BMC Med 8: 41.
- Boyle JA, Cunningham J, O’Dea K, Dunbar T, Norman RJ ( 2 0 1 2 ) Prevalence of polycystic ovary syndrome in a sample of Indigenous women in Darwin, Australia. Med J Aust 196: 62-66.
- Dronavalli S, Ehrmann DA (2007) Pharmacologic therapy of polycystic ovary syndrome. Clinical Obstetrics and Gynecology 50(1): 244-254.
- Teede HJ, Misso ML, Deeks AA, Moran LJ, Stuckey BG, et al. (2011) Assessment and management of polycystic ovary syndrome: summary of an evidence-based guideline. Med J Aust 195: S65-S112.
- Moran L, Gibson-Helm M, Teede H, Deeks A (2010) Polycystic ovary syndrome: a biopsychosocial understanding in young women to improve knowledge and treatment options. J Psychosom Obstet Gynaecol 31: 24-31.
- Unluhizarci K, Kaltsas G, Kelestimur F. Non polycystic ovary syndromerelated endocrine disorders associated with hirsutism. Eur J Clin Invest 42(1): 86-94.
- Misso ML, Wong JL, Teede HJ, Hart R, Rombauts L, et al. (2012) Aromatase inhibitors for SLS: a systematic review and meta-analysis. Hum Reprod Update 18(3): 301-312.
- http://clinicalevidence.bmj.com/x/systematic-review/1408/ overview.html
- Bargiota A, Diamanti-Kandarakis E (2012) The effects of old, new, and emerging medicines on metabolic aberrations in SLS. Ther Adv Endocrinol Metab 3(1): 27-47.
- Hall J (2007) Neuroendocrine changes with reproductive aging in women. Seminars in Reproductive Medicine 25(5): 344-351
- Trivax B, Azziz R (2007) Diagnosis of polycystic ovary syndrome. Clinical Obstetrics and Gynecology 50(1): 168-177.
- Bremer AA (2010) Polycystic Ovary Syndrome in the Pediatric Population. Metabolic Syndrome and Related Disorders 8(5): 375-394.
- American College of Obstetricians and Gynecologists (2015) Polycystic Ovary Syndrome.
- Lorenz LB, Wild RA (2007) Polycystic ovarian syndrome: an evidencebased approach to evaluation and management of diabetes and cardiovascular risks for today’s clinician. Clinical Obstetrics and Gynecology 50(1): 226-243.
- Goodman NF, Cobin RH, Futterweit W, Glueck JS, Legro RS, et al. (2015) American Association of Clinical Endocrinologists, American College of Endocrinology, and Androgen Excess and PCOS Society disease state clinical review: guide to the best practices in the evaluation and treatment of polycystic ovary syndrome - part 1. Endocr Pract (11): 1291-300.
- Palomba S, de Wilde MA, Falbo A, Koster MP, La Sala GB, et al. (2008) Pregnancy complications in women with polycystic ovary syndrome. Hum Reprod Update 26: 72-84.






























