Titanium Based Biomaterials
Fehim Findik*
Biomedical, Magnetic and Semiconductor Materials Application & Research Center, Sakarya University, Turkey
Submission: August 07, 2017; Published: August 23, 2017
*Corresponding author: Fehim Findik, Biomedical, Magnetic and Semiconductor Materials Application & Research Center, Sakarya University, Sakarya, 54187, Turkey; Email: flndik@sakarya.edu.tr
How to cite this article: Fehim F. Titanium Based Biomaterials. Curr Trends Biomedical Eng & Biosci. 2017; 7(3): 555714. DOI: 10.19080/CTBEB.2017.07.555714.
Keywords
Keywords: Titanium alloys; biomedical; manufacture; mechanical properties
Introduction
A biomaterial can be defined as any material used to make devices to replace a part or a function of the body in a safe, reliable, economic, and physiologically acceptable manner. A variety of devices and materials is used in the treatment of disease or injury. Commonplace examples include sutures, tooth fillings, needles, catheters, bone plates, etc.
Improvement resolutions are along these lines:
i. To eliminate poisonous elements;
ii. To reduce the Young's modulus to evade stress protection influence in bone obsession;
iii. To develop blood and tissue suitability;
iv. To make small medical apparatus.
Titanium based alloys are used perfectly as implant materials. Stainless steels (SS) and Co-Cr alloys have some hazardous rudiments, such as Ni, Co and Cr. Therefore, Ti was advised as a substitute for the 316L SS and Co-Cr alloys due to well biocompatibility and corrosion resistance. However, once high strength is essential, the Young's modulus of Ti cannot sometimes fulfill the necessities of biomaterials. To eliminate such limitations, Ti was replaced by α+β-type Ti-based alloys, especially Ti-6Al-X (X=V, Nb, Fe, Zr, Ta) alloys [1].
Requirements
The choice of biomaterials and also design rely on the proposed medical usage. Improvement of novel biomaterials involves a collective struggle between biomedical engineers, material scientists and clinicians. An implant should have the subsequent characteristics to function for lengthier retro without elimination.
Mechanical properties
The modulus of bone differs around 4 to 30 GPa depending upon the bone variety and the measurement direction. If implant materials have greater stiffness than bone, the required stress being transferred to adjacent bone is prevented, bone resorption is resulted nearby the implant and subsequently implant releasing occurs. This biomechanical incompatibility causes death of bone cells and this is called as “stress shielding effect" [2]. Therefore a material having high strength and low modulus nearer to bone must be utilized for implantation to shun releasing of implants during service life.
Biocompatibility
The materials utilized as implants are anticipated to be nontoxic in the human body. The achievement of the biomaterials is mostly dependent upon the response of the human body to the implant, and this determines the biocompatibility of a material [3]. The host reaction tempted by the material and the materials degradation in the body control the biocompatibility of a material.
Corrosion and wear resistance
The discharge of non-compatible metal ions are resulted by the implants into the body because of the low corrosion and wear resistance of the implants in the body fluid. The discharged ions initiate allergic and toxic responses [4]. Therefore progress of implants with high corrosion resistance is of crucial significance for the permanency of the material in the human structure.
Osseointegration implant
Relaxation occurs because of the incapability of an implant surface to incorporate with the neighboring bone and other tissues as a result of micromotions [5]. For the improvement of decent osseointegration, chemistry, roughness and topography of the surface perform a key role.
Applications
Biomaterials can be used in hip and knee implants (Figure 1). Currently, Ti-based alloys consisted biocompatible alloying rudiments are being established mostly for biomedical implants to be utilized as implant apparatus substituting botched hard tissues and dental yields. Finally, Ti-based alloys are also projected to be utilized to repair soft tissue for example blood vessels.
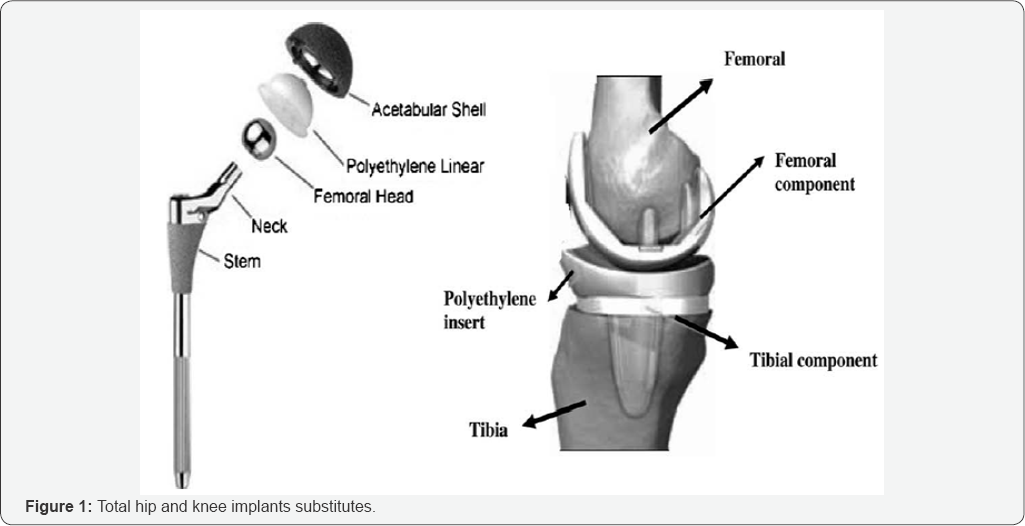
Production
Biomaterials can be produced via casting, powder metallurgy, additive manufacturing and so on. Casting is a manufacturing process in which a liquid material is usually poured into a mold, which contains a hollow cavity of the desired shape, and then allowed to solidify. Production of biomedical components conventionally entails arc or induction melting. To minimize possibility of contamination during melting, an inert gas working atmosphere is used. Pure raw materials are essential to achieve good mixing of the constituent elements for making alloys with homogeneity and uniformity in the properties.
Powder metallurgy (PM)
Is a term covering a wide range of ways in which materials or components are made from metal powders. PM processes can avoid, or greatly reduce, the need to use metal removal processes, thereby drastically reducing yield losses in manufacture and often resulting in lower costs. Powder metallurgy techniques can be employed to produce near-net shape components from metal powders with properties that can be tailored to specific requirements. In the present review, three surgical implant alloys were considered in terms of the commercial powders available and processing techniques used to consolidate these powders. Generally, all consolidation techniques are designed to produce a fully dense component with mechanical properties similar to the wrought/cast material.
Additive manufacturing
The industrial version of 3-D printing is already used to make some niche items, such as medical implants, and to produce plastic prototypes for engineers and designers. But the decision to mass-produce a critical metal-alloy part to be used in thousands of jet engines is a significant milestone for the technology. And while 3-D printing for consumers and small entrepreneurs has received a great deal of publicity, it is in manufacturing where the technology could have its most significant commercial impact.
Future
The range of application of titanium and its alloys in medical area is truly astonishing. The applications cover dental implants and parts for orthodontic surgery, joint replacement parts for hip, knee, shoulder, spine, elbow and wrist, bone fixation materials like nails, screws, nuts and plates, housing device for the pacemakers and artificial heart valves, surgical instruments and components in high-speed blood centrifuges [6]. Titanium alloys are privileged in a sense that a wide spectrum of microstructures is possible depending upon alloy chemistry and thermomechanical processing. This makes titanium alloys very responsive to modify its properties according to particular necessities. However the building belongings associations have been fine established and reported for structural titanium alloys, the character of microstructure is lightly addressed in the case of alloys.
Conclusion
Despite previously used Ti-Al-V alloys, due to some problems (toxicity and high elastic modulusetc), recently many alternative Ti-based alloys (such as Ti-Nb-Fe, Ti-Nb-Zr, Ti-Nb-Ta etc) have been extensively used. For production methods, in one side conventional casting methods are used, in the other side PM techniques (both conventional and modern PIM ones) as well as additive manufacturing have been widely employed.
References
- Zwicker U, Buhler K, Muller R (1980) J Mechanical Properties and Tissue Reactions of a Titanium Alloy for Implant Material. In Kimura I (Ed.), Titanium'80, Science and Technology. Metallurgical Society of AIME, New York, USA, 1: 505-514.
- Black J, Hastings GW (1998) Handbook of biomaterials properties. Chapman and Hall. London. UK.
- Sumner DR, Turner TM, Igloria R, Urban RM, Galante JO (1998) J Biomech 31: 909-917.
- Hallab NJ, Anderson S, Stafford T, Glant T, Jacobs JJ (2005) J Orthop Res 23(2): 384-391.
- Williams DF (2008) Biomaterials. 29: 2941-2953.
- Teoh SH (2000) Int J Fatigue 22(10): 825-837.






























