Detection of a Rare Haemoglobin Variant- Hbj during Glycosylated Haemoglobin Analysis- A Rare Single Case Report
Neelima Verma1* and Jyoti Chakraverty2
1Department of Clinical Biochemistry, Fortis Hospital, India
2Department of Histopathology, Fortis Hospital, India
Submission: March 12, 2018; Published: April 13, 2018
*Corresponding author: Neelima Verma, Department of Clinical Biochemistry, Senior Consultant in Clinical Biochemistry, Fortis Hospital, Shalimar Bagh, India, Email: drnilimaverma@gmail.com
How to cite this article: Neelima V, Jyoti C. Detection of a Rare Haemoglobin Variant- Hbj during Glycosylated Haemoglobin Analysis- A Rare Single Case Report. Anatomy Physiol Biochem Int J: 2018; 4(4): 555650. DOI: 10.19080/APBIJ.2018.04.555650.
Abstract
We report the case of a very rare haemoglobin variant, “Haemoglobin J”, discovered while performing haemoglobin electrophoresis following low HbA1C value reported in pregnant female with Gestational diabetes mellitus. Haemoglobin J is an alpha chain variant and heterozygous group of fast moving Haemoglobin (FMH).
Abbrevations: FMH: Fast Moving Haemoglobin; Hb: Haemoglobin; HCT: Haemocrit; RBC: Red Blood Cell; RWD: Red Cell Distribution Width; MCH: Mean Corpuscular Haemoglobin; MCHC: Mean Corpuscular Hemoglobin Concentration; IBCT: Iron Binding Capacity Total; GTT: Glucose Tolerance Test
Introduction
Glycosylated Haemoglobin is routinely used to maintain long term glycemic control in diabetic patients [1]. But sometimes HbA1C levels are formed contradicting with plasma glucose levels. This may be because of presence of abnormal and rare haemoglobin HbJ which was first reported in an American Negro family by Thorup et al. [2]. HbJ is fast moving hemoglobin (FMH). This alpha globulin gene variant resulting from substitution of a negatively charged amino acid residue is alpha, beta or gamma globulin chain [3]. HbJ can be differentiated and identified solely from its retention time. Prevalence of Fast Moving Haemoglobin Variant HbJ is very rare. Different authors during epidemiologic investigation in different population did not find any single case of HbJ showing it to be rare variant [4-6]. In a large study of 13,913 individuals of North Americans 524 had abnormal Hb variant but none of the patient had HbJ variant [7].
Similarly in a study of 9792 cases of Tunisian population only 228 cases (2.33%) were found to be having abnormal Hb Variant but none was having HbJ variant [8]. Although during a large retrospective study (65,779 cases) for screening, detection, and identification of Hb variants within a clinical laboratory setting of India only 46 cases (0.07%) were found to be having HbJ variant [9] and 10 yr study of hemoglobin variant on 1,19,336 cases from eastern Indian population only three cases were found to be having Hb J variant [10] which shows this variant to be very rare. Here we report our experience of detection of abnormal Hb variant (HbJ) during further investigation of pregnant female as low HbA1C value was contradicting with high glucose level. It was not a case of Sickle cell disease (SCD) nor had received any blood transfusion.
Case Report
A 29 years old four and a half months pregnant female with gestational diabetes mellitus presented to Gynae OPD of Fortis Hospital, Shalimar Bagh for routine ante natal check up. As a part of routine investigation Complete Blood Count, GTT, HbA1C and Iron Profile was advised. EDTA anticoagulated whole blood specimen collected in Becton Dickinson Vacutainer was analyzed for CBC, HbA1C and 2 ml blood sample was collected in fluoride vial for Blood glucose levels. After 2 hours of taking 75gms glucose her blood glucose levels were on the higher side (blood glucose- 203mg/dl). Hb (9.8%) was on the lower side with low haemocrit (32.1), low MCV and MCHC (Table 1). Complete Blood Count was done on Sysmex XN 550 (L Series). Blood glucose was performed on Dimension RxL Max series.
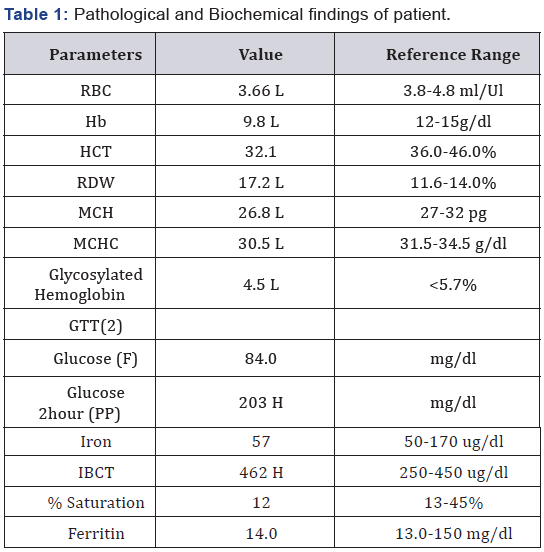
Abbreviations: Hb: Haemoglobin; HCT: Haemocrit; RBC: Red Blood Cell; RWD: Red Cell Distribution Width; MCH: Mean Corpuscular Haemoglobin; MCHC: Mean Corpuscular Hemoglobin Concentration; IBCT: Iron Binding Capacity Total; GTT: Glucose Tolerance Test
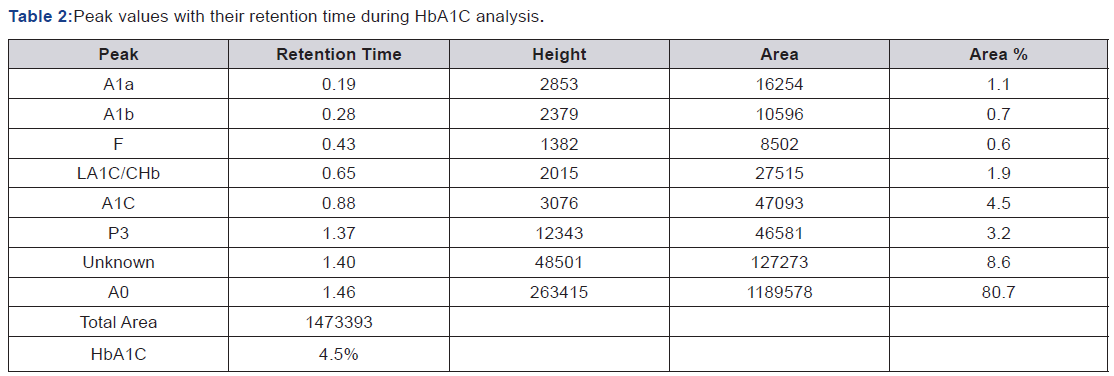
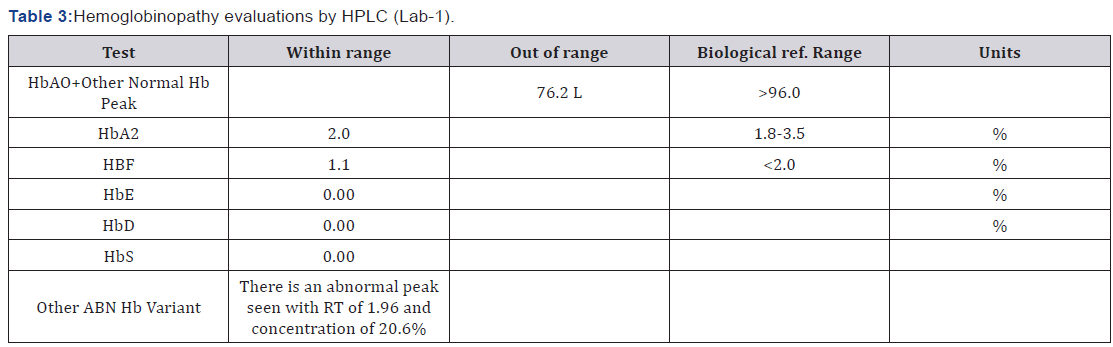
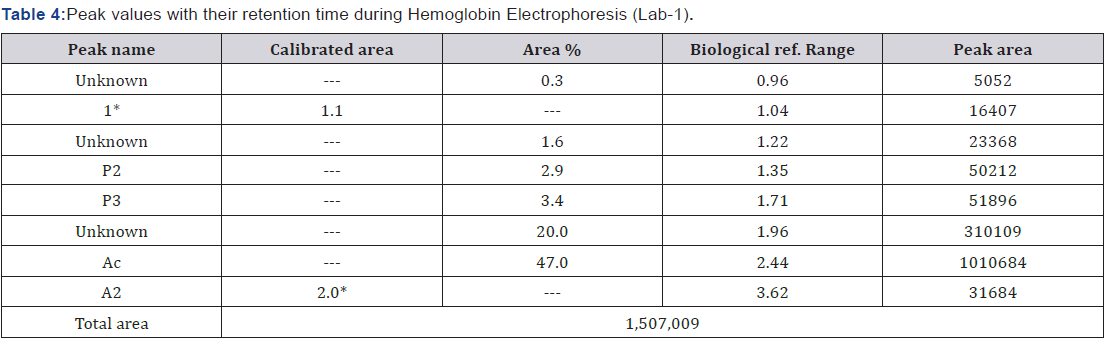
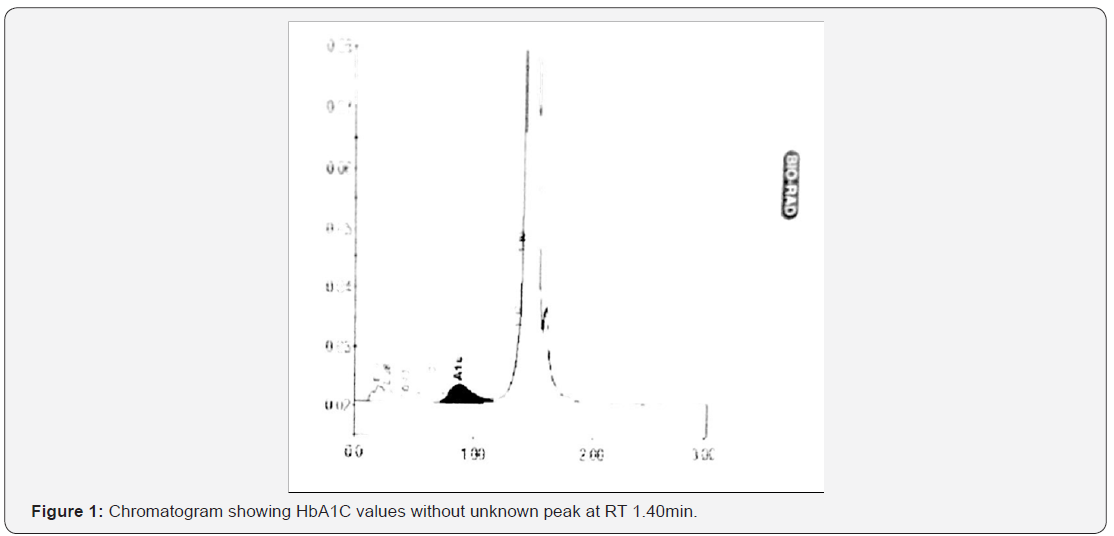
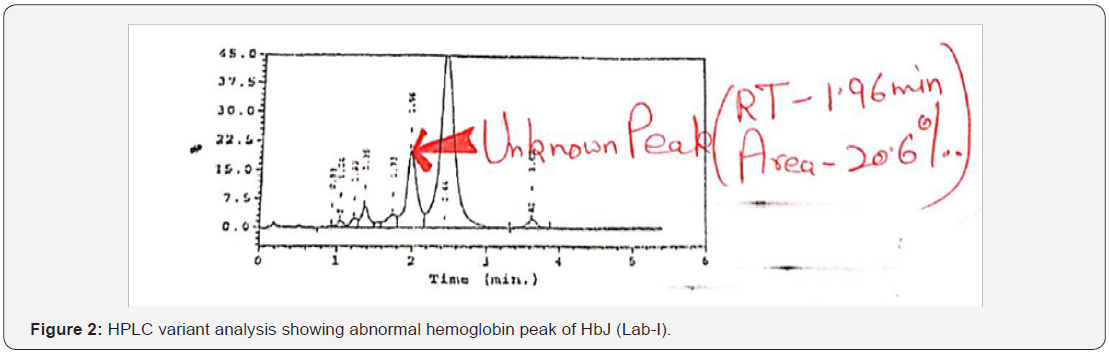
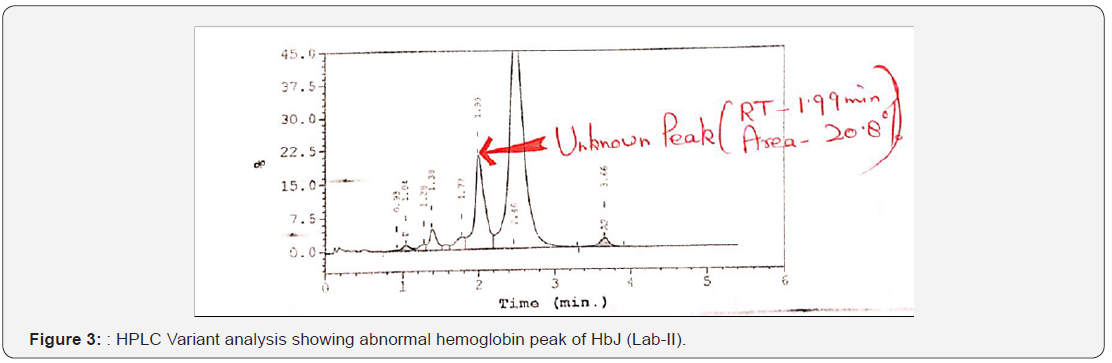
Treatment And Follow Ups
Family studies, DNA studies and genetic counselling were advised for the patient from both the laboratories. But as HbJ is rather clinically silent and our patient had no adverse symptoms related to abnormal variant. Further characterization of this haemoglobin variant was not indicated clinically, so molecular studies were not pursued (Table 5).

Discussion
HbA1C is used for long term management of patients with DM type-1 and 2 [11] but wherever the value of HbA1C is discrepant there is always possibility of abnormal fast moving haemoglobin [12]. In our patient HbA1C came out to be low in spite of High glucose levels during antenatal screening indicating the possibility of abnormal variant. Abnormal haemoglobin like Hb J which produces no haematological symptoms is rarely detected. Similarly a case of HbJ-Meerut was detected when pregnant female came for routine antenatal check up showing falsely low HbA1C levels not corresponding to their Blood glucose levels. HPLC analysis for patient’s mother and two younger siblings showed the presence of same abnormal haemoglobins seen in patient herself. The mean percentage of this abnormal Hb variant in these four family members was 19.025 eluted at a retention time of 1.87-1.90min [3]. During study of abnormal haemoglobin variant in large Indian Population other authors [13-15] found out only one case of HbJ Meerut among 232 cases, 543 cases, 290 cases of abnormal hemoglobin variant respectively showing it to be very rare (Table 6).
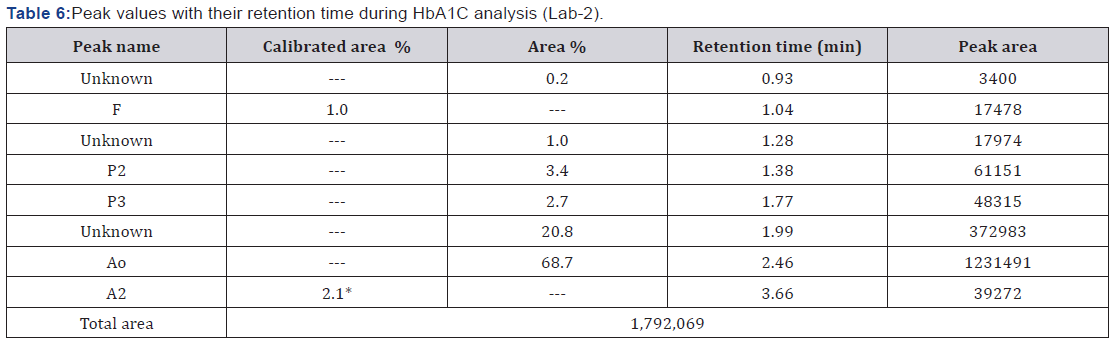
HbJ variant which is an alpha chain variant found in heterozygous state may also be detected via using different techniques - mass spectrometry. In a study Bhatt, et al. [16] identified Variant HbJ - Rajappen using mass spectrometry technique. Patient being diabetic had blood sugar levels 232 mg/dl but HbA1C level 4.4% indicating presence of abnormal variant. Upon electrophoresis a p3 Peak with a retention time of 1.3 min and a percentage of 23.4% was found out. This finding is very much similar to our findings [16].
Even though hemoglobin variants are prevalent in general population, reports of transfusion acquired Hb Variants are rare. Soumya P et al [17] performed a retrospective analysis on SCD patients who underwent blood transfusion. 66 patients were found to be having abnormal Hb Variant and only on patient had HbJ variant. There are more than 40 HbJ variants described in the literature. They all have an electrophoretic mobility faster than the Hb variants. All are classified under variants of the alpha or beta chains [18-20]. In sickle cell disease patients due to number of blood transfusion, it is very common to found abnormal variant. N Sweden et al. [21] discovered HbJ variant while performing Hemoglobin electrophoresis following exchange transfusion of SCD patient after red cell exchange. The clinical impact of rare hemoglobin variant such as HbJ when combined with hemoglobin SCD (or trait) is not clear in the medical literature. Clinical follow up of the patient showed no complications and the clinical cause was consistent with the patient’s underlying medical condition. Five units of RBC’s
were donated by two sisters. When hemoglobin electrophoresis was performed on samples of two sisters they were found to be having HbJ variant [21].
Take Home Message
1. Wherever there is falsely low HbA1C with Unknown peak in case of known chronic diabetic one should raise alarm to look for Unusual Variant affecting HbA1C.
2. HbJ is a rare Hemoglobin Variant which is heterozygous alpha globulin gene variant.
3. Unknown peak on HbA1C chromatogram and retention time are very useful information for detection and identification of rare hemoglobin variant.
References
- American diabetes association (2003) Standards of Medical care for patients with diabetes Mellitus. Diabetes Care 26 Suppl 1: s33-s50.
- Thorup OA, Itano HA, Wheby M, Leavell BS (1956) Hemaoglobin. J Science 123: 889.
- A Sharma, S Marwah, G Buxi, RB Yadav (2012) Falsely lowHbA1c value due to a rare hemoglobin variant (HemoglobinJ-Meerut) - A family study. Indian J Pathol Microbiol 55(2): 270-271.
- K Ghosh, RB Colah, MB Mukherjee (2015) Haemoglobinopathies in tribal populations of India. Indian J Med Res 141(5): 505-508.
- NM Wasim, M Thevarajah, CY Yean (2010) Hemoglobin variants detected by hemoglobin A1C (HbA1C) analysis and the effects on HbA1C measurements, Int J Diabetes Dev Ctries 30(2): 86-90.
- P Jain, Vinod K, R Sen, S Bhargava (2016) Prevalence of haemoglobinopathies in anemic females. Int J Res Med 4(10): 4329- 4334.
- Wilburn CR, Bernard DW, Zieske AW, Andrieni J, Miller T, et al. (2017) The Prevalence and Role of Hemoglobin Variants in Biometric Screening of a Multiethnic Population: One Large Health System’s Experience. Am J Clin Pathol 147(6): 589-595.
- K Bouzid, HB Ahmed, E Kalai, S Blibeche, N Couque, et al (2014) Prevalence of hemoglobin variants in a diabetic population at high risk of hemoglobinopathies and optimization of HbA1c monitoring by incorporating HPLC in the laboratory workup. Libyan Journal of Medicine 9: 25768.
- S Warghade, J Britto, R Haryan, T Dalvi, R Bendre, et al. (2018) Prevalence of hemoglobin variants and hemoglobinopathies using cation-exchange high-performance liquid chromatography in central reference laboratory of India: A report of 65779 cases. J Lab Physicians 10(1): 73-79.
- SK Mondal, Saikat Mandal (2016) Prevalence of thalassemia and hemoglobinopathy in eastern India: A 10-year high-performance liquid chromatography study of 119,336 cases. Asian J Transfus Sci 10(1): 105-110.
- Nuttall FQ (1998) Comparison of percent total GHb with percent HbA1c in people with and without known diabetes. Diabetes Care 21(9): 1475-1480.
- Srinivas U, Mahapatra M, Patil HP (2007) HemoglobinJ Meerut, A fast moving hemoglobin - A study of seven cases from India and review of literature. Am J Hematol 82: 666-667.
- L Pant, S Singh, M Kudesia, S Mendiratta, M Mittal, A Mathur (2014) Detection of Abnormal Hemoglobin Variants by HPLC Method: Common Problems with Suggested Solutions. International Scholarly Research Notices 2014: 1-10.
- V Chandrashekar, M Soni (2012) Hemoglobin Disorders in South India. Indian J Clin Biochem. 27(4): 414-416.
- R Sachdev, AR Dam, G Tyagi (2010) Detection of Hb Variants and hemoglobinopathies in Indian Population using HPLC: Report of 2600 cases. Indian J Pathol Microbiol 53(1): 57-62.
- VS Bhatt, AK Mandal (2012) Identification of a Rare Hemoglobin Variant HbJ - Rajappen [alpha90(FG2) Lys - Thr] Using Mass Spectrometry Ind J Clin Biochem 27(4): 414-416.
- S Pandey, M Cottler Fox, G Drobena (2015) Hemoglobin Variants Acquired Post Exchange transfusion in Pediatric Cell disease (SCD) patients. Annals of Clinical & Laboratory Science 45(6): 627-630.
- Botha MC, Beale D, Isaacs WA (1996) Hemoglobin J Cape Town-alpha-2 92 arginine replaced by glutamine beta-2. Nature 212(5064): 792- 7955.
- Lambridis AJ, Ramsay M, Jenkins T (1986) The haematological puzzle of Hb J (Cape Town) is partly solved. Br J Haematol 63(2): 363-367.
- Huisman TH, Carver MF, Efremov GD (1998) A Syllabus of Human Hemoglobin Variants. The Sickle Cell Anemia Foundation California, USA.
- N Sweden, K Nicol, P Moder, S Kahwash (2008) An “Acquired” hemoglobin J Variant in a sickle cell disease patient. Ther Clin Risk Manag 4(3): 649-652.






























