Radiological and Anatomical Findings in Parathyroid Carcinoma: A Case Report
Masoume Soleymaninejad1, Zabihollah Gholizadeh2, Vida Garousi3 and Ahmad Farrokhi4*
1Ayatollah Mousavi hospital, Aniography center, Zanjan University of Medical Sciences, Iran
2BSc of operating room, Shafa hospital, Iran
3Medical student, Zanjan University of medical sciences, Iran
4Department of Anatomical Sciences, Zanjan University of Medical Sciences, Iran
Submission: March 05, 2018; Published: March 19, 2018
*Corresponding author: Ahmad Farrokhi, Department of Anatomical Sciences, Zanjan University of Medical Sciences, Iran, Tel: 00989178172415; Email: farrokhi_a68@yahoo.com
How to cite this article: Ibrahim A Ai, Hisham M Abdel Rahim, Babiker Almobasher, Rihab M Badi, Abdarahiem Alborai, Abdelmohisen Hussein. Kamal M Awad,Reference Range of Hemoglobin A1c in Khartoum State. Anatomy Physiol Biochem Int J: 2018; 4(4): 555645. DOI: 10.19080/APBIJ.2018.04.555645.
Abstract
Parathyroid Carcinoma is a rare cause of primary hyperparathyroidism often resulting in severe hypocalcaemia. Diagnosis of parathyroid carcinoma requires radiological Investigations. We presented the case of a 52 year old lady, with a past history of abdominal pain, frequent vomiting, curettage and a large swelling on the neck there. The novelty of this study was abnormally large of parathyroid tumour that led doctors to suspect thyroid cancer. In benign hyperparathyroidism, experienced surgeons will successfully detect the tumours during their exploration; but imaging plays an important role when the carcinoma is suspected as a differential diagnosis of parathyroid adenoma and hyperplasia due to clinical manifestations.
Keywords: Parathyroid glands; Parathyroid Carcinoma; Spect imaging
Introduction
Parathyroid glands are four tiny glands behind the thyroid gland. The size of each of these glands is 5-7×3-4×0.5-2mm and weight of each these glands is 30-50mg [1]. These glands are involved in calcium homeostasis and metabolism of phosphate. Overactive of these glands, can cause hyperparathyroidism as a result of the increase in PTH hormone. Also, hyperparathyroidism can cause adenoma, hyperplasia and carcinoma [2]. Parathyroid carcinoma is created in 1-3% of cases of hyperparathyroidism [3]. Parathyroid carcinoma is a rare disorder with a difficult clinical diagnosis and high mortality [3-6]. The etiology of the disorder is largely unknown [5]. Reports indicate that the average age of onset of the disease is 48 years and the incidence is equal in men and women [3]. Although some sources have reported incidence in women is twice that of men [7]. Diagnosis of this rare endocrine disorderis carried out through biochemical, histological, molecular biology and radiological tests. Radiological evaluation by CT scan, MRI, ultrasonography, scintigraphy and TC99-msestamibi carried out. Since parathyroid tumors require surgery to reduce the risk and treatment with parathyroidectomy action is done, the diagnosis of cancer is very important [4,8]. Therefore, this study aimed to diagnosis faster and more accurate parathyroid carcinoma to reduce side-effects for the patient.
Case Report
We presented the case of a 52 year old lady, with a past history of abdominal pain, frequent vomiting, curettage and a large swelling on the neck there. Early diagnosis was hyperparathyroidism. A hard palpable right neck mass approximately 6.5 to 5.5cm diameter was discovered on first examinations.
Radionuclide evaluation of parathyroid
The anterior view of the neck and chest was performed, almost at 20, 30, 60, 70, 90 and 100 minutes after IV administration of 15mCi TC99-msestamibi (Figure 1). There was a homogeneous radiotracer accumulation in the below right lobe, which extends to the substernal areas corresponding to palpable nodule, which was holding the radiotracer out the study. Early diagnosis of the nuclear physician was parathyroid adenoma, parathyroid hyperplasia, thyroid adenoma, thyroid carcinoma and parathyroid carcinoma.

Parathyroidectomy
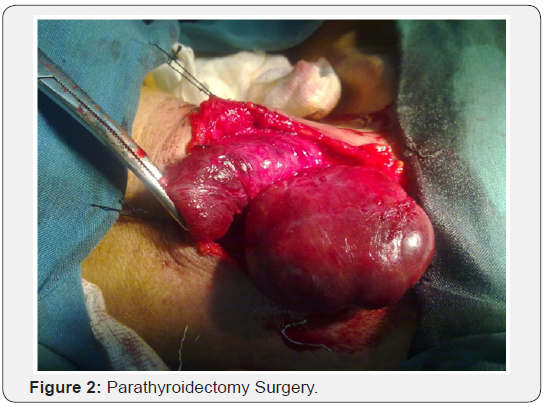
To reduce the risk of mortality and morbidity, parathyroidectomy (Figure 2) surgery was performed and right lobe of the thyroid and parathyroid glands were removed (Figure 3). Observations and measurements after parathyroidectomy have shown a nodule 5.5×4.5×2.5cm dimension. After bringing the sample to pathology unit, the pathologist was diagnosed parathyroid carcinoma.

Discussion
Parathyroid carcinoma is a rare malignancy that occurs in 1-2% [9] or 1-3% [3] of patients with hyperparathyroidism. Among the most important risk factors for this disease is a palpable mass in the neck with a size of more than 3cm [4] which causes anatomical changes in the parathyroid glands. Radiological techniques such as Technetium TC 99-msestamibi can have an important role in the clinical diagnosis of the disease and Show anatomical changes in the glands. Some surgeons believe that imaging techniques are not useful for surgery [8]. In terms of treatment, early treatment for parathyroid carcinoma is complete removal of the gland through surgery for all tumours [10]. However, in the last century, parathyroidectomy was the most common method for direct visualization of the parathyroid glands in patients with hyperparathyroidism but recently, preoperative localization methods which have fewer side effects are being replaced [8]. Of course, to remove the tumour detected in the patient reported in this study parathyroidectomy is used.
In this patient, according to the image of TC 99-msestamibi, change in normal anatomical sizes which is one of the main risk factors for parathyroid carcinoma was observed. The novelty of this study was abnormally large of parathyroid tumour that led doctors to suspect thyroid cancer. According to a painful mass in the neck, the early radiological detection and pathological secondary diagnosis, the patient reported was suffering from parathyroid carcinoma. Therefore, it is recommended to surgeons that if they see carcinoma risk factors and also tumour metastases to the liver area, lymph nodes and lungs, complete radiological and pathological tests before surgery. Because onethird of parathyroid carcinoma metastasis seen that reliability indices to prove the rare disease [1] and Imaging is also useful for detecting metastases or recurrent diseases.
Conflict of Interest
The authors have no conflict of interest.
References
- Doherty GM (2006) Parathyroid Glands. In: Mulholland MWL, et al. (Eds.), Greenfield’s Surgery: Scientific Principles and Practice. p. 1-71.
- Nanka O, Sedy J, Vitkova I, Libansky P, Adamek S (2006) Surgical anatomy of parathyroid glands with emphasis on parathyroidectomy. Prague medical report 107(2): 261-272.
- Temmim L, Sinowatz F, Hussein WI, Al-Sanea O, El-Khodary H (2008) Intrathyroidal parathyroid carcinoma: a case report with clinical and histological findings. Diagnostic pathology 3: 46.
- Duan K, Mete O (2015) Parathyroid Carcinoma: Diagnosis and Clinical Implications. Turk patoloji dergisi 31(Suppl 1): 80-97.
- Marcocci C, Cetani F, Rubin MR, Silverberg SJ, Pinchera A, et al. (2008) Parathyroid carcinoma. J Bone Miner Res 23(12): 1869-1880.
- Rodriguez C, Naderi S, Hans C, Badoual C (2012) Parathyroid carcinoma: a difficult histological diagnosis. Eur Ann Otorhinolaryngol Head Neck Dis 129(3): 157-159.
- Salesi M, Salimi F, Mahzouni P (2011) Thyroid or Parathyroid Adenoma.
- Godazandeh G, Sharif F, Akha O, Khalilian A (2010) Simultaneous Use of Ultrasonography and TC99mSS Scan in the Diagnosis of Hyperparathyroidism Preoperatively CAB Direct 20: 20-25.
- Yousem DM (2014) Parathyroid and Thyroid Imaging. Head and Neck Imaging pp. 435-459.
- Wynne AG, van Heerden J, Carney JA, Fitzpatrick LA (1992) Parathyroid carcinoma: clinical and pathologic features in 43 patients. Medicine 71(4): 197-205.






























