Post-Vaccination Acute myocarditis: A Case of Uncommon Link
Sergio Fasullo1*, Giorgio Maringhini1, Vincenzo Bucca1, Giovanni Lipari1, Filippo Ganci1, Giuseppe Vitale1, Debora Cangemi1, Antonio Miserendino1 and Stefania Davi2
1Department of Cardiology, GF Ingrassia Hospital, Italy
2Department of Chemistry and Pharmaceutical Technologies, Italy
Submission: March 01, 2018; Published: March 19, 2018
*Corresponding author: Sergio Fasullo, Chief of Coronary Unit, Department of Cardiology, Paolo Borsellino, Corso Calatafimi 1002, Palermo, Italy, Tel: 3387965572; Email: sergio.fasullo72@gmail.com
How to cite this article: Sergio Fasullo, Giorgio Maringhini, Vincenzo Bucca, Giovanni Lipari, Filippo Ganci, Giuseppe Vitale. Post-Vaccination Acute myocarditis: A Case of Uncommon Link. Anatomy Physiol Biochem Int J: 2018; 4(4): 555643. DOI: 10.19080/APBIJ.2018.04.555643.
Abstract
This case report describes a case of acute myocarditis post-vaccination. Patient who received the Fluad seasonal influenza vaccine. There is evidence in the literature linking vaccines to different auto-immune manifestations. Of late, autoimmune manifestations that appear to be caused by an external adjuvant have been grouped into a complex syndrome referred to as autoimmune/inflammatory syndrome induced by adjuvants (ASIA). She presented to hospital with chest pain and weakness. Laboratory investigations showed elevated creatine kinase and troponin-I, and extensive cardiac investigations yielded a diagnosis of myocarditis. Adjuvants are elements that induce an inflammatory response. In the case of vaccines, adjuvants increase the antigen-specific immune response, to ultimately improve vaccine immunogenicity. The seasonal influenza vaccine is an uncommon trigger for autoimmune disease, and is not commonly associated with myocarditis. The incidence of myocarditis post vaccination is limited to case reports at this time. Given the benefits of the influenza vaccine and the rarity of this complication, we do not discourage its routine usage when clinically indicated. However, ongoing surveillance is required to evaluate the occurrence of rare adverse events.
Keywords: Myocarditis; Flu; Vaccine
Abbrevations: GWS: Gulf War Syndrome; MMF: Macrophagic Myofasciitis Syndrome; ASIA: Autoimmune/Inflammatory Syndrome Induced By Adjuvants; ECG: Electro Cardio Graphy
Case Presentation
A 71 year old with history of hypertension presented to hospital with chest pain, dyspnea and chills of cold. In the morning before admission, she had received the Fluad seasonal influenza vaccine, comprised of one influenza A H1N1 virus, one influenza A H3N2 virus, one influenza B virus, and the MF59 adjuvant.
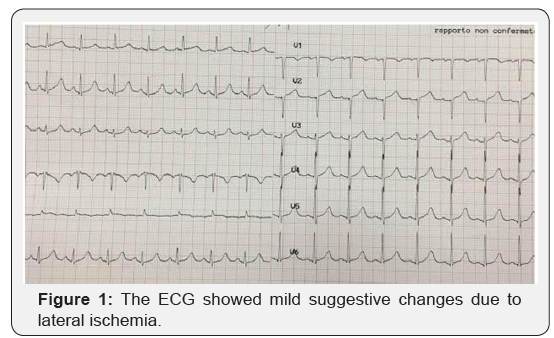
On physical exam her vitals were: BP 145/102, P 130, RR 20, T 37.3°C and her O2 saturation was 93 % on oxygen (2l/min). Her respiratory exam revealed mild crackles in the lower lung zone. The rest of the examination was unremarkable. Her blood counts were WBC 1,484×99/L, hemoglobin 14g/L (MCV 88 fL) and platelets 287×109/L. Electrolytes included sodium 139mmol/L, potassium 4mmol/L. Other investigations showed creatinine 0,74mM/L and troponin 17459g/L (normal <0.2g/L). Her EKG was normal sinus rhythm with ischemic features. She was placed on supplemental oxygen and received a single dose of furosemide 40mg and methylprednisolone 80mg iv, to which he responded well. She also received clopidogrel and aspirin for a possible acute syndrome coronary. The ECG showed mild suggestive changes due to lateral ischemia (Figure 1).
An echocardiogram performed revealed systolic dysfunction with any regional wall motion abnormalities and lateral pericardial effusion (Figure 2). She underwent coronarography on the second day, which showed a coronary tree free of lesions. Her cardiac work-up suggested myocarditis and not myocardial infarction as a cause for her elevated troponins. Her troponin levels began to trend downwards after four days, and almost completely normalized within ten days. Despite the atypical nature of our patient’s presentation, including cardiac involvement, we believe that his intense inflammatory response may be attributed to his recent vaccine in the absence of other causes, especially given the timing of adjuvant exposure. Based on the patient’s clinical and laboratory findings, a presumptive diagnosis of ASIA was made. The patient recovered fully, and was safely discharged home on day fifteen.

Discussion
Patient who received the Fluad seasonal influenza vaccine. There is evidence in the literature linking vaccines to different auto-immune manifestations. The role of various environmental factors in the pathogenesis of immune mediated diseases is well established. Of which, factors entailing an immune adjuvant activity such as infectious agents, silicone, aluminium salts and others were associated with defined and non-defined immune mediated diseases both in animal models and in humans [1,2]. In recent years, four conditions: siliconosis, the Gulf war syndrome (GWS), the macrophagic myofasciitis syndrome (MMF) and postvaccination phenomena were linked with previous exposure to an adjuvant. Furthermore, these four diseases share a similar complex of signs and symptoms which further support a common denominator. Thus, we review herein the current data regarding the role of adjuvants in the pathogenesis of immune mediated diseases as well as the amassed data regarding each of these four conditions.
Relating to the current knowledge we would like to suggest to include these comparable conditions under a common syndrome entitled ASIA, “Autoimmune (Auto-inflammatory) Syndrome Induced by Adjuvants”. Of late, autoimmune manifestations that appear to be caused by an external adjuvant have been grouped into a complex syndrome referred to as autoimmune/ inflammatory syndrome induced by adjuvants (ASIA). Based on the patient’s clinical and laboratory findings, a presumptive diagnosis of a postvaccination inflammatory syndrome was made. The patient recovered promptly in hospital without the usage of immunomodulatory agents. For the diagnosis of ASIA, the presence of at least 2 major (exposure to an external stimuli prior to clinical manifestations; the appearance of ‘typical’ clinical manifestations: myalgia, myositis or muscle weakness) or 1 major and 2 minor criteria (the appearance of auto antibodies or antibodies directed at the suspected adjuvant; other clinical manifestations: irritable bowel syndrome) must be apparent.
Table reprinted from Journal of Autoimmunity C Perricone et al. [3] ASIA – Autoimmune/inflammatory syndrome induced by adjuvants. Significant complications are rare. In addition to handhygiene and respiratory etiquette, immunization is an effective tool to curb the spread of the influenza virus. Annual vaccination has been shown to protect individuals of all ages from the flu, decreasing rates of emergency room visits, hospitalization, and death. These benefits outweigh the mild adverse effects, prompting many countries to continue wide-reaching annual influenza vaccination campaigns. At this time, the incidence of myocarditis post vaccination is limited to case reports. ASIA is an emerging clinical entity, with its share of case reports hypothesizing a causal link with vaccines. Furthermore, most available seasonal flu vaccines do not contain any adjuvants. Ongoing surveillance to establish the existence of this posited entity and to evaluate its risks should be pursued.
Acknowledgment
I would like to express my gratitude to the colleagues and nurses (in particular Mr Rosario Ferrante) as traveling companions and to the patients who have shown me the boundaries of pain and hope.
References
- Cheng, Michael G Kozoriz, Amir A Ahmadi, John Kelsall, Katryn Paquette, et al. (2016) Post‑vaccination myositis and myocarditis in a previously healthy male. Allergy Asthma Clin Immunol 12: 6.
- Matthew, Michael G Kozoriz, Amir A Ahmadi, John Kelsall, Jake M Onrot (2015) Post-Vaccination Myositis and Myocarditis in a Previously Healthy Male. Intern Med 5:5.
- Perricone, Colafrancesco S, Mazor RD, Soriano A, Agmon-Levin N, et al. (2013) Autoimmune/inflammatory syndrome induced by adjuvants (ASIA): Unveiling the pathogenic, clinical and diagnostic aspects. J Autoimmun 47: 1-16.






























