Congenital Diaphragmatic Hernias: A Review Article
Heshmat SW Haroun*
Department of Anatomy and Embryology, Cairo University, Egypt
Submission: January 13, 2018; Published: February 19, 2018
*Corresponding author: Heshmat SW Haroun, Professor of Anatomy and Embryology, Faculty of Medicine, Cairo University, Egypt, Tel: (+20) 01005225350; Email: heshmatsabet@gmail.com;hesmat.haroun@kasralainy.edu.eg.com
How to cite this article: Heshmat SW Haroun. Congenital Diaphragmatic Hernias: A Review Article. Anatomy Physiol Biochem Int J: 2018; 4(2): 555635. DOI: 10.19080/APBIJ.2018.04.555635.
Abstract
Congenital diaphragmatic hernia (CDH) is a rare anomaly that occurs through foramen of Bochdalek (common), foramen of Morgagni (rare), or esophageal hiatus (rare). It is commonly unilateral (right or left) and rarely bilateral. Genetic factors are blamed for the pathogenesis of CDH and other factors as fetal male gender, maternal age above 40, vitamin deficiencies, smoking, alcohol and chemicals during pregnancy are additional contributors to the incidence of this anomaly. CDH commonly presents in neonates and rarely later in life. It may be associated with respiratory, gastrointestinal and urinary complications. Pulmonary agenesis, pulmonary hypoplasia and persistent pulmonary hypertension are the main determinants of mortality and morbidity in neonates with CDH. Reduction of the hernia and repair of the diaphragmatic defect are achieved through either transthoracic or transabdominal approach.
Keywords: Diaphragmatic Hernias, Congenital, Morgagni Hernia, Bochdaleck Hernia, Hiatus Hernia, Clinical Associations
Abbreviations: AGV: Acute Gastric Volvulus, BH: Bochdalek Hernia, CDH: Congenital Diaphragmatic Hernia, CDHs: Congenital Diaphragmatic Hernias, CHA: Congenital Heart Anomaly, CMH: Congenital Morgagni Hernia, CMLH: Congenital Morgagni-Larrey’s Hernia, CPEH: Congenital Paraesophageal Hernia, ECMO: Extracorporeal Membrane Oxygenation, EPS: Extralobar Pulmonary Sequestration, GEJ: Gastroesophageal Junction, L-CDH: Left Congenital Diaphragmatic Hernia, MRI: Magnetic Resonance Imaging, PPFs: Pleuro Peritoneal Folds, R-CDH: Right Congenital Diaphragmatic Hernia, VT: Ventilatory Time
Introduction
Congenital diaphragmatic hernia (CDH) is an uncommon congenital anomaly of the diaphragm resulting in herniation of the abdominal viscera into the thoracic cavity. It develops from incomplete closure and fusion of the fetal pericardioperitoneal canals and pleuroperitoneal folds (PPFs) or abnormality of the esophageal hiatus. Congenital diaphragmatic hernias (CDHs) occur mainly through two diaphragmatic defects: rarely in the foramen of Morgagni and commonly in the foramen of Bochdalek. CDH through the esophageal hiatus is also rarely recognized. All the three types of CDH are repaired surgically. Pulmonary hypoplasia and persistent pulmonary hypertension are the two main determinants of neonatal mortality and morbidity in cases with CDH [1-7]. CDHs are mostly diagnosed early in life; later diagnosis is rare especially if the hernia is asymptomatic. Despite advances in therapeutic modalities, CDH in the newborn represents challenges to the multi-disciplinary teams involved in CDH management [8,9].
Early intubation of antenatally scan-diagnosed CDH in the newborn is crucial in preventing respiratory deterioration and persistent pulmonary hypertension [10,11]. Observed-to-expected lung-to-head ratio, liver position, and total lung volume measured by magnetic resonance imaging (MRI) are the prognostic predictors most often used, and they correlate with neonatal mortality and morbidity [12]. Extralobar pulmonary sequestration (EPS) can be found incidentally in CDH; it usually arises in the chest or the abdomen and rarely in the diaphragm [13]. Hepatopulmonary fusion is a rare malformation associated with R-CDH and is only discovered during surgical repair of the diaphragmatic defect [14].The association of 46,XY sex disorder with CDH is rare; it has been described with or without other congenital anomalies as external ambiguous genitalia, truncus arteriosus, bifid thymus, gut mal rotation, and limb anomalies [15].
Neonates with CDH have a high prevalence of congenital malformations [16]. The prognosis for infants with CDH associated with cardiovascular malformation is poor. The severity of the cardiovascular malformation is more important as a predictive factor for mortality and morbidity than the severity of CDH itself [17]. Minor forms of congenital heart anomaly (CHA) have no negative impact on the survival of infants with CDH. However, mortality appears to be significantly higher in infants with CDH associated with major forms of CHA [18]. The possibility of a diaphragmatic hernia is suspected when a cardiac mass with specific echocardiographic features is observed [19]. Large CDH defect sizes increase mortality while the association between defect sizes and morbidity is not fully elucidated [20]. Growth patterns during the first year of life were described in infants with CDH. Poor growth was a common early finding in CDH patients, which improved during infancy [21].
Furthermore, it was emphasized on the importance of close follow-up and intense nutritional management in CDH infants [22]. A clinical prediction rule, for neonates with CDH, was designed using predictors generated from: very low birth weight, absent or low 5-minute Apgar score, presence of chromosomal or major cardiac anomaly, and pulmonary hypertension. This clinical model discriminated between neonates at high, intermediate or low death risks [23]. Low five minute Apgar score, and high alveolar-arterial gradient are significant predictors of neonatal mortality in CDH. R-CDH is associated with high mortality (50%) and prolonged length of stay than L-CDH [24].
Ventilatory time (VT) is an important marker to identify subjects at risk for short-term neurodevelopmental impairment in CDH survivors [25]. Fetal ultrasonography and MRI are essential antenatal outcome predictors in neonates with CHD [26]. Fetal lung area-to-head circumference ratio and observedto- expected lung-to-head ratio measurements can accurately predict postnatal survival and the need for extracorporeal membrane oxygenation (ECMO) therapy in fetuses with leftsided congenital diaphragmatic hernias [27]. CDH presentation in adults is extremely rare. Patients with late presentation of CDHs complain of a wide variety of symptoms and diagnosis has proved to be difficult [28]. The late-presenting Bochdalek hernias often constitute difficulties in diagnosis that may lead to inappropriate treatment; an example is the herniated stomach that is mistaken for a tension pneumothorax [29].
Etiology, Incidence and Risk Factors Of CDH
The diaphragm is derived from multiple embryonic mesodermal sources, but how these structures give rise to the diaphragm is not definitely known. The exact etiology of CDH is still unknown but some researches point out genetic factors as a possible cause of the defect [30,31]. Although numerous chromosomal aberrations and gene mutations are associated with CDH, the etiology of the diaphragmatic defect is identified in less than 50% of patients [32]. Attention has to be paid to chromosomal abnormality in cases of CDH associated with abdominal wall closure defect in the presence of intact septum transversum [33]. In mouse models, it was demonstrated that the transient embryonic pleuroperitoneal folds (PPFs) were the source of the diaphragm’s muscular tissue and that migration of PPF cells controlled diaphragm morphogenesis.
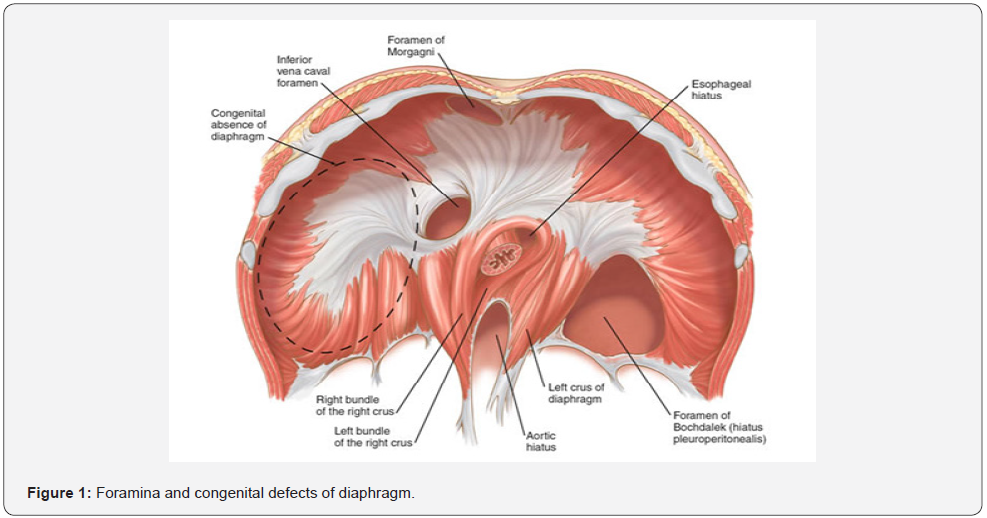
Furthermore, mutations in PPF-derived muscle connective tissue fibroblasts resulted in the development of biomechanically weak and more compliant non-muscular localized parts of the diaphragm, leading to CDH. [34]. The incidence of CDH is reported to be 1 in 2500 births, with left congenital diaphragmatic hernia (L-CDH) being seven times commoner than right-side one (R-CDH). Many cases of CDH are discovered prenatally or during the immediate postnatal period while 5-25% of cases can be late-presenting with respiratory or gastrointestinal problems or complications such as gastric volvulus, obstruction, perforation, peritonitis or necrosis [35]. In USA, the incidence of CDH was estimated to be 1.93/10,000 births. Risk factors for the development of CDH included foetal male gender, maternal age above 40, Caucasian ethnicity, smoking and alcohol use during pregnancy. As compared to foetuses without CDH, foetuses with CDH were at an increased risk of stillbirth, preterm birth, and intrauterine growth restriction. In CDH, neonatal mortality during the first year amounted to 45.89% [36](Figure 1).
Right- Versus Left-Sided CDH
Regarding the sidedness of CDH, Morgagni hernia is typically detected on right side anteriorly while Bochdalek hernia on left side posteriorly, because of the protective roles of the liver and heart on either side respectively. Hiatus hernias range from herniation of a small portion to herniation of the whole stomach into the left thoracic cavity; very rarely into the right thoracic cavity [37]. It was found that the severity of left heart hypoplasia correlated with the severity of CDH. Both right and left CDH had decreased the left ventricular volume and in addition, L-CDH compressed the left heart [38]. Right ventricular dimensions were reported to be significantly reduced in fetuses with isolated R-CDH [39]. R- CDH seems to have a poorer outcome than that reported for fetuses with L-CDH with similar lung size before birth [40].
R-CDH requires prosthetic mesh repair more frequently than L-CDH because of larger defect size or complete agenesis. Recurrent herniation is significantly higher in the R-CDH. Survivors of R-CDH do not have a significantly different neurodevelopmental outcome when compared to L-CDH survivors. Compared to L-CDH, fetuses with R-CDH are less likely to be diagnosed prenatally and have a higher need for extracorporeal membrane oxygenation [41,42]. R-CDH is not associated with increased mortality, but with increased severity of pulmonary hypoplasia necessitating increased requirement for pulmonary vasodilatory therapy and for tracheostomy [43].
Hernia of Morgagni-Larrey
Giovanni Battista Morgagni (1682-1771) was the first to describe anatomical structures like the trigonum sternocostale dextrum (the Morgagni’s foramen), the appendix testis (the Morgagni’s hydatid), the vertical folds of distal rectum (the Morgagni’s columns) and many others. For this, it was said of him: “If all the anatomical findings made by Morgagni should bear his name, probably one third of human body would be called Morgagni’s” [44]. Hernia of Morgagni is a congenital herniation of abdominal contents into the thoracic cavity through a retrosternal (retrocostoxiphoid) diaphragmatic defect (foramen of Morgagni). It is also termed parasternal diaphragmatic hernia of Morgagni-Larrey (retrochondrosternal, retrocostoxiphoid, retrosternal, subcostal, substernal or subcostosternal hernia) [45]. Morgagni-Larrey hernia is the rarest of all CDHs [46].
On CT examination, unusual giant bilateral Mogagni hernia, extending to both thoracic apices, was detected. [47,48]. The incidence of congenital Morgagni’s hernia (CMH) among all CDHs is 3-4% (less than 5%) and about 90% of the hernias occur on the right side, 8% are bilateral and 2% are on the left side [49]. CMH is more recordable from women with advancing age. Embryonic disorder of diaphragmatic differentiation is the major etiological factor but vitamin deficiencies and some chemical substances are also predisposing. CMH, in the pediatric age group, commonly presents with recurrent chest infection and has a high incidence of associated anomalies, commonly congenital heart disease and Down syndrome [50]. A case of CMH has been detected in a 3-month-old child affected by Marfan’s syndrome [51]. In CMH, the hernial sac is usually small and is surgically repaired through either abdominal or lateral thoracotomy approch. Median sternotomy is rarely used as an approach for repair these hernias [52].
Transabdominal approach is preferred to transthoracic one for the surgical repair of Morgagni hernias [53]. There is a high rate of recurrence after laparoscopic repair of Morgagni hernia without the use of a prosthetic polypropylene mesh [54]. Hernia of Morgagni may be associated with mediastinal lipoma in an adult [55]. It may consist of the thoracic protrusion of fat and/ or abdominal viscera through a congenital diaphragmatic defect. It may be asymptomatic, mimicking a large intrathoracic lipoma. Improper diagnosis can cause catastrophe during surgical repair [56,57]. Bilateral Morgagni hernias associated with left Bochdalek diaphragmatic hernia and Down syndrome are very rare congenital anomalies [58]. Congenital Morgagni-Larrey’s hernia (CMLH) is known to be associated with a high incidence of bilaterality and associated anomalies like congenital heart disease, Down’s syndrome, gut malrotation, inguinal hernia, umbilical hernia, and pyloric stenosis [59-62]. Gastric volvulus and intestinal obstruction are described as complications of CMH [63, 64].
Hernia of Bochdalek
Professor Vincenz Alexander Bochdalek was a clever anatomist and athologist who studied and worked at Charles- Ferdinand University in Prague from the 1820s to the early 1870s. His name is permanetly linked to certain anatomico-pathological structures, particuarly the vertebrocostal (lumbocostal) triangle in the posterior part of the diaphragm (foramen of Bochdalek) and the hernia through this foramen (posterolateral hernia of Bochdalek) [65,66]. Bochdalek hernia (BH) is the commonest of all CDHs. It occurs in 1 in 2000 to 3000 newborns [67]. It usually presents in neonates with respiratory failure and very rarely in adults, needs to be early corrected and repaired, and is associated with a high mortality [68-73]. No correlation is found between asymptomatic incidentally discovered BH and age, gender, or body mass index in adults [74].
Symptomatic BH in adults may lead to gastrointestinal dysfunction or severe pulmonary disease. [75] Bilateral occurrence is rare; a case of bilateral BH was associated with severe aortic tortuosity and aberrant right subclavian artery [76].BH may be associated with acute gastric volvulus (AGV) [77,78], intestinal obstruction, perforation, gangrene and empyema [79,80]. Herniated stomach, spleen and colon [81], and ectopic intrathoracic kidney [82-84]. Other rare associations are septic ureteric obstruction [85], and intermittent heart block [86].
Congenital Hiatus Hernia
The pathogenesis of hiatus hernia is attributed to three theories:
1. An increase in the intra abdominal pressure forcing the gastroesophageal junction (GEJ) into the thorax;
2. Shortening of the esophagus due to fibrosis or excessive vagal nerve stimulation; and
3. Widening of the esophageal hiatus in response to congenital or acquired molecular and cellular changes in the diaphragm [87].
Congenital paraesophageal hernia (CPEH) is a rare condition in childhood. It usually presents with non-specific symptoms of recurrent attacks of chest infection and/or vomiting; it may be associated with Marfan’s syndrome [88,89]. Most reported cases of CPEH refer to adult patients. Familial occurrence of sliding hiatus hernias is postulated in some cases [90]. A case of a boy with hiatus hernia that developed eight days following a transabdominal repair of the left BH is mentioned in the literature [91]. An intrathoracic gastric volvulus complicating CPEH is rare; rapid diagnosis and treatment are essential to avoid dreadful complications as gastric dilatation, gangrene and perforation that may lead to cardiopulmonary arrest [92]. In an old cadaver, a congenital hiatus hernia associated with non rotation of the midgut was observed. The hernial sac originated from the peritoneum near the GEJ, and contained the midgut. The duodenum was abnormally placed and the common hepatic duct was variably drained [93]. CPEHs differ from the more common sliding hiatus hernias in anatomy, pathology, symptoms, complications, and management [94].
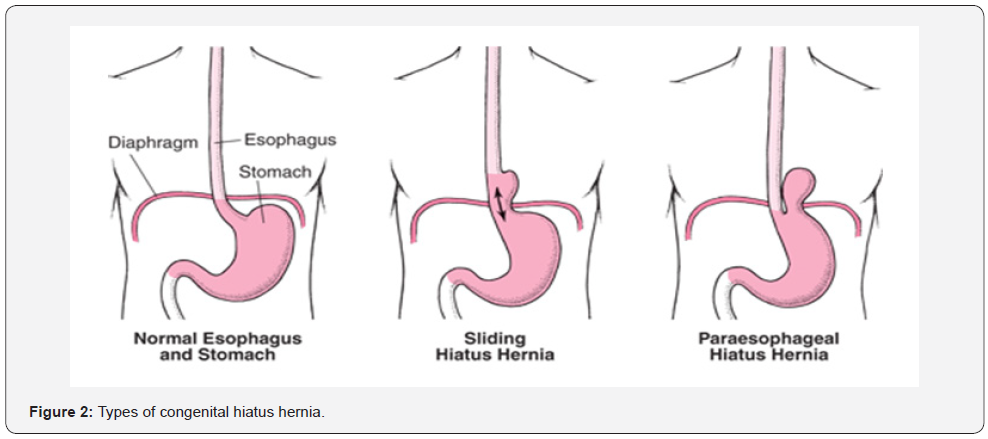
In literature, there are case-reports of intrathoracic stomach secondary to congenitally short esophagus in a preterm infant [95], hiatus hernia associated with unilateral pulmonary agensis and malformations of big vessels [96], CPEH causing severe hyporegenerative anemia [97], massive hiatal hernia containing the colon, intestine, and stomach mimicking chest pathologies [98], and gastric herniation through the aortic hiatus [99]. A case of a child was diagnosed to have congenital bilateral cervical lung herniation associated with retrosternal (Morgagni), posterolateral (Bochdalek), esophageal hiatal, and inguinal hernias, together with multiple urinary bladder diverticula. These multiple herniations were thought to be secondary to defective embryonic celomic mesoderm [100,101](Figure 2)
References
- Cevizci MN, Erdemir G, Cayir A (2015) A Rare Cause of Haemorrhage in the Upper Gastrointestinal System: Bochdalek Hernia. West Indian Med J 64(2): 154-156.
- Kesieme EB, Kesieme CN (2011) Congenital diaphragmatic hernia: review of current concept in surgical management. ISRN Surg 2011: 974041.
- Leeuwen L, Fitzgerald DA (2014) Congenital diaphragmatic hernia. J Paediatr Child Health 50(9): 667-673.
- Sakoda A, Matsufuji H (2015) Current Management of Congenital Diaphragmatic Hernia. Kyobu Geka 68(8): 676-683.
- Sandstrom CK, Stern EJ (2011) Diaphragmatic hernias: a spectrum of radiographic appearances. Curr Probl Diagn Radiol 40(3): 95-115.
- Bolino G, Gitto L, Serinelli S, Maiese A (2015) Autopsy features in a newborn baby affected by a central congenital diaphragmatic hernia. Med Leg J 83(1): 51-53.
- Bedeir K, Hassanein W (2013) Congenital diaphragmatic hernia: unusual presentation in an adult. Thorac Cardiovasc Surg 61(3): 264- 266.
- Chao PH, Huang CB, Liu CA, Chung MY, Chen CC, et al. (2010) Congenital diaphragmatic hernia in the neonatal period: review of 21 years’ experience. Pediatr Neonatol 51(2): 97-102.
- Losty PD (2014) Congenital diaphragmatic hernia: where and what is the evidence? Semin Pediatr Surg 23(5): 278-282.
- McHoney M (2015) Congenital diaphragmatic hernia, management in the newborn. Pediatr Surg Int 31(11): 1005-1013.
- McHoney M (2014) Congenital diaphragmatic hernia. Early Hum Dev 90(12): 941-946.
- Benachi A, Cordier AG, Cannie M, Jani J (2014) Advances in prenatal diagnosis of congenital diaphragmatic hernia. Semin Fetal Neonatal Med 19(6): 331-337.
- Shibuya S, Ogasawara Y, Izumi H, Kantake M, et al. (2014) A case of congenital diaphragmatic hernia with intradiaphragmatic pulmonary sequestration: case report and literature review. Pediatr Surg Int 30(9): 961-963.
- Olenik D, Codrich D, Gobbo F, Travan L, Zennaro F, et al. (2014) Hepatopulmonary fusion in a newborn. An uncommon intraoperatory finding during right congenital diaphragmatic hernia surgery: case description and review of literature. Hernia 18(3): 417-421.
- Esplin ED, Chaib H, Haney M, Martin B, Homeyer M, Urban AE, Bernstein JA (2015) 46,XY disorders of sex development and congenital diaphragmatic hernia: a case with dysmorphic facies, truncus arteriosus, bifid thymus, gut malrotation, rhizomelia, and adactyly. Am J Med Genet A 167(6): 1360-1364.
- Bojanić K, Pritišanac E, Luetić T, Vuković J, Sprung J, Weingarten TN, Schroeder DR, Grizelj R (2015). Malformations associated with congenital diaphragmatic hernia: Impact on survival. J Pediatr Surg 50(11): 1817-1822.
- Takahashi S, Sago H, Kanamori Y, Hayakawa M, Okuyama H, et al. (2013) Prognostic factors of congenital diaphragmatic hernia accompanied by cardiovascular malformation. Pediatr Int 55(4): 492-497.
- Ruano R, Javadian P, Kailin JA, Maskatia SA, Shamshirsaz AA, et al. (2015) Congenital heart anomaly in newborns with congenital diaphragmatic hernia: a single-center experience. Ultrasound Obstet Gynecol 45(6): 683-688.
- Kim SH, Kim MG, Kim SJ, Moon J, Kang WC, et al. (2015) Unusual Diaphragmatic Hernias Mimicking Cardiac Masses. J Cardiovasc Ultrasound 23(2): 107-112.
- Putnam LR, Harting MT, Tsao K, Morini F, Yoder BA, et al. (2016) Congenital Diaphragmatic Hernia Defect Size and Infant Morbidity at Discharge. Pediatrics 138(5). pii: e20162043.
- Leeuwen L, Walker K, Halliday R, Karpelowsky J, Fitzgerald DA (2014) Growth in children with congenital diaphragmatic hernia during the first year of life. J Pediatr Surg 49(9): 1363-1366.
- Leeuwen L, Walker K, Halliday R, Fitzgerald DA (2014) Neurodevelopmental outcome in Congenital Diaphragmatic Hernia survivors during the first three years. Early Hum Dev 90(8): 413-415.
- Brindle ME, Cook EF, Tibboel D, Lally PA, Lally KP (2014) A clinical prediction rule for the severity of congenital diaphragmatic hernias in newborns. Pediatrics 134(2): e413-e419.
- Jani P, Bidarkar SS, Walker K, Halliday R, Badawi N, Cohen RC (2014) Right-sided congenital diaphragmatic hernia: A tertiary centre’s experience over 25 years. J Neonatal Perinatal Med 7(1): 39-45.
- Bevilacqua F, Morini F, Zaccara A, Valfrè L, Capolupo I, et al. (2015) Neurodevelopmental outcome in congenital diaphragmatic hernia survivors: role of ventilatory time. J Pediatr Surg 50(3): 394-398.
- Basiewicz-Slaczka E, Wołoszczuk-Gebicka B, Yaqoub S, Kamiński A (2015) The value of the oxygenation index in the prediction of postnatal outcome in neonates with congenital diaphragmatic hernia. Preliminary report. Dev Period Med 19(3 Pt 1): 283-288.
- Kehl S, Siemer J, Brunnemer S, Weiss C, Eckert S, et al. (2014) Prediction of postnatal outcomes in fetuses with isolated congenital diaphragmatic hernias using different lung-to-head ratio measurements. J Ultrasound Med 33(5): 759-767.
- Stokes KB (1991) Unusual varieties of diaphragmatic herniae. Prog Pediatr Surg 27: 127-147.
- Fatimi SH, Sajjad N, Muzaffar M, Hanif HM (2011) Congenital diaphragmatic hernia presenting in the sixth decade mimicking pneumonia. J Pak Med Assoc 61(6): 600-601.
- Jelin EB, Kim TN, Nathan N, Miniati D (2011) Synchronous ipsilateral Bochdalek and Morgagni diaphragmatic hernias: a case report. J Pediatr Surg 46(12): 2383-2386.
- Hussey M, Własienko P, Adamczyk T, Dangel J (2015) [Familial congenital diaphragmatic hernia with anencephly-exencephaly and spina bifida]. Ginekol Pol 86(2): 155-159.
- Slavotinek AM (2014) The genetics of common disorders - congenital diaphragmatic hernia. Eur J Med Genet 57(8): 418-423.
- Inoue S, Odaka A, Muta Y, Beck Y, Sobajima H, et al. (2016) Coexistence of congenital diaphragmatic hernia and abdominal wall closure defect with chromosomal abnormality: two case reports. J Med Case Rep 10: 19.
- Merrell AJ, Ellis BJ, Fox ZD, Lawson JA, Weiss JA, Kardon G (2015) Muscle connective tissue controls development of the diaphragm and is a source of congenital diaphragmatic hernias. Nat Genet 47(5): 496- 504.
- Topor L, Pătrăncuş T, Caragaţa R, Moga A (2015) Left congenital diaphragmatic hernia -- case report. Chirurgia (Bucur) 110(1): 84-87.
- Balayla J, Abenhaim HA (2014) Incidence, predictors and outcomes of congenital diaphragmatic hernia: a population-based study of 32 million births in the United States. J Matern Fetal Neonatal Med 27(14): 1438-1444.
- Saeed U, Mazhar N, Zameer S (2014) Large hiatal hernia in infancy with right intrathoracic stomach along with left sided morgagni hernia. J Coll Physicians Surg Pak 24 Suppl 3: S178-S179.
- Byrne FA, Keller RL, Meadows J, Miniati D, Brook MM, et al. (2015) Severe left diaphragmatic hernia limits size of fetal left heart more than does right diaphragmatic hernia. Ultrasound Obstet Gynecol 46(6): 688-694.
- DeKoninck P, Richter J, Van Mieghem T, Van Schoubroeck D, Allegaert K, et al. (2014) Cardiac assessment in fetuses with right-sided congenital diaphragmatic hernia: case-control study. Ultrasound Obstet Gynecol 43(4): 432-436.
- DeKoninck P, Gomez O, Sandaite I, Richter J, Nawapun K, et al. (2015) Right-sided congenital diaphragmatic hernia in a decade of fetal surgery. BJOG 122(7): 940-946.
- Collin M, Trinder S, Minutillo C, Rao S, Dickinson J, et al. (2016) A modern era comparison of right versus left sided congenital diaphragmatic hernia outcomes. J Pediatr Surg 51(9): 1409-1413.
- Akinkuotu AC, Cruz SM, Cass DL, Cassady CI, Mehollin-Ray AR, et al. (2015) Revisiting outcomes of right congenital diaphragmatic hernia. J Surg Res 198(2): 413-417.
- Partridge EA, Peranteau WH, Herkert L, Rendon N, Smith H, et al. (2016) Right- versus left-sided congenital diaphragmatic hernia: a comparative outcomes analysis. J Pediatr Surg 51(6): 900-902.
- Zani A, Cozzi DA (2008) Giovanni Battista Morgagni and his contribution to pediatric surgery. J Pediatr Surg 43(4): 729-733.
- Arráez-Aybar LA, González-Gómez CC, Torres-García AJ (2009) Morgagni-Larrey parasternal diaphragmatic hernia in the adult. Rev Esp Enferm Dig 101(5): 357-366.
- Abraham V, Myla Y, Verghese S, Chandran BS (2012) Morgagni-larrey hernia- a review of 20 cases. Indian J Surg 74(5): 391-395.
- Lammy S, Stewart M, Carnochan FM, Walker WS (2013) Bilateral Morgagni hernia: operative discovery of appendix lying on superior pulmonary vein. Scott Med J 58(3): e1-e3.
- Saxena AK, Ruttenstock EM, Singer G (2012) Pediatric bilateral Morgagni-Larrey diaphragmatic hernia: is diagnosis with computed tomography required in the era of laparoscopic approach? Hernia 16(3): 373-374.
- Eroğlu A, Kürkçüoğlu IC, Karaoğlanoğlu N, Yilmaz O (2003) Combination of paraesophageal hernia and Morgagni hernia in an old patient. Dis Esophagus 16(2): 151-153.
- Al-Salem AH, Zamakhshary M, Al Mohaidly M, Al-Qahtani A, Abdulla MR, et al. (2014) Congenital Morgagni’s hernia: a national multicenter study. J Pediatr Surg 49(4): 503-507.
- Winde G, Blum M, Pelster F, Pfisterer M, Krings W (1988) Morgagni hernia. A rare form of diaphragmatic hernia. Zentralbl Chir 113(12): 782-789.
- Laumonerie P, Mouttalib S, Edouard T, Galinier P (2015) Morgagni- Larrey diaphragmatic hernia in a 3-month-old child affected by Marfan syndrome. Arch Pediatr 22(11): 1151-1153.
- Ahmad M, Al-Arifi A, Najm HK (2015) Giant Hernia of Morgagni with Acute Coronary Syndrome: A Rare Case Report and Review of Literature. Heart Lung Circ 24(9): e144-e147.
- Aydin Y, Altuntas B, Ulas AB, Daharli C, Eroglu A (2014) Morgagni hernia: transabdominal or transthoracic approach? Acta Chir Belg 114(2): 131-135.
- Garriboli M, Bishay M, Kiely EM, Drake DP, Curry JI, et al. (2013) Recurrence rate of Morgagni diaphragmatic hernia following laparoscopic repair. Pediatr Surg Int 29(2): 185-189.
- Menditto VG, Cavicchi A, Marchetti G, Marzioni M, Braccioni F, et al. (2011) Hernia of Morgagni and mediastinal lipoma: a case report. Ann Thorac Cardiovasc Surg 17(1): 77-80.
- Pinto CS, Bernardo J, Eugénio L, Antunes MJ (2013) Morgagni hernia mimicking intrathoracic lipomatous tumor. Rev Port Cir Cardiotorac Vasc 20(3): 135-137.
- Komatsu T, Takahashi Y (2013) Is this a mediastinal tumor? A case of Morgagni hernia complicated with intestinal incarceration mistaken for the mediastinal lipoma previously. Int J Surg Case Rep 4(3): 302- 304.
- Niramis R, Poocharoen W, Watanatittan S (2008) Bilateral Morgagni hernias association with left Bochdalek diaphragmatic hernia: a very rare anomaly. J Med Assoc Thai 91 Suppl 3: S157-S160.
- Al-Salem AH (2010) Bilateral congenital Morgagni-Larrey’s hernia. World J Pediatr 6(1): 76-80.
- Radionov M, Ziya DD, Nedevska M (2015) Giant morgagni hernia in a female with malrotation syndrome and thoracic transposition of small bowel, coecum, ascending and transverse colon. Khirurgiia (Sofiia) 81(3):142-148.
- S Breinig, Paranon S, Le Mandat A, Galinier P, Dulac Y, et al. (2010) Morgagni hernia causing cardiac tamponade. Arch Pediatr 17(10): 1465-1468.
- Taşkin GA, Tuncer O, Demir N, Bilici S, Aktar F, et al. (2014) Association of Down syndrome and morgagni hernia. Genet Couns 25(3): 345-347.
- Sonthalia N, Ray S, Khanra D, Saha A, Maitra S, et al. (2013) Gastric volvulus through morgagni hernia: an easily overlooked emergency. J Emerg Med 44(6): 1092-1096.
- Tirumani H, Saddala P, Fasih N (2014) Incarcerated morgagni hernia: an unusual cause of large bowel obstruction. J Emerg Med 47(3): 320- 322.
- Kachlik D, Cech P (2011) Vincenz Alexander Bochdalek (1801-83). J Med Biogr 19(1): 38-43.
- Haller JA (1986) Professor Bochdalek and his hernia: then and now. Prog Pediatr Surg 20: 252-255.
- Wenzel-Smith G (2013) Posterolateral diaphragmatic hernia with small-bowel incarceration in an adult. S Afr J Surg 51(2): 73-74.
- Herling A, Makhdom F, Al-Shehri A, Mulder DS (2014) Bochdalek hernia in a symptomatic adult. Ann Thorac Surg 98(2): 701-704.
- Jubber I, Madani Y, Yousaf S, Jubber A (2014) Bochdalek hernia causing type II respiratory failure in an elderly patient. BMJ Case Rep 2014 pii: bcr2014203915.
- Garófano-Jerez JM, López-González Jde D, Valero-González MA, Valenzuela-Barranco M (2011) Posterolateral Bochdalek diaphragmatic hernia in adults. Rev Esp Enferm Dig 103(9): 484-491.
- Venkatesh SP, Ravi MJ, Thrishuli PB, Sharath Chandra BJ (2011) Asymptomatic Presentation of Bochdalek’s Hernia in an Adult. Indian J Surg 73(5): 382-283.
- Temizöz O, Gençhellaç H, Yekeler E, Umit H, Unlü E, et al. (2010) Prevalence and MDCT characteristics of asymptomatic Bochdalek hernia in adult population. Diagn Interv Radiol 16(1): 52-55.
- Alviar CL, Cordova JP, Korniyenko A, Javed F, Tsukayama M, et al. (2011) Bilateral Bochdalek hernias presenting as respiratory failure in an elderly patient. Respir Care 56(5): 691-694.
- Keijzer R, Puri P (2010) Congenital diaphragmatic hernia. Semin Pediatr Surg 19(3): 180-185.
- Hamid KS, Rai SS, Rodriguez JA (2010) Symptomatic Bochdalek hernia in an adult. JSLS 14(2):279-281.
- Akay S, Battal B, Kara K, Bozlar U (2013) Bilateral Bochdalek hernias associated with severe aortic tortuosity and aberrant right subclavian artery. Singapore Med J 54(8): e169-e171.
- Atef M, Emna T (2015) Bochdalek Hernia With Gastric Volvulus in an Adult: Common Symptoms for an Original Diagnosis. Medicine (Baltimore 94(51): e2197.
- Hadjittofi C, Matter I, Eyal O, Slijper N (2013) Laparoscopic repair of a late-presenting Bochdalek diaphragmatic hernia with acute gastric volvulus. BMJ Case Rep 20: 2013.
- Sakai T, Ogura Y, Yamada Y, Kodama H, Kimura D, et al. (2013) Elderly Bochdalek hernia found out by intestinal obstruction. Kyobu Geka 66(12): 1074-1078
- Salústio R, Nabais C, Paredes B, Sousa FV, Porto E, et al. (2014) Association of intestinal malrotation and Bochdalek hernia in an adult: a case report. BMC Res Notes 7: 296.
- Kurniawan N, Verheyen L, Ceulemans J (2013) Acute chest pain while exercising: a case report of Bochdalek hernia in an adolescent. Acta Chir Belg 113(4): 290-292.
- Onuk Ö, Taş T, Şentürk AB, Sinanoğlu O, Balcı MB, Çelik O, Nuhoğlu B (2014) Right-sided Bochdalek hernia with intrathoracic ectopic kidney in an advanced-age adult: a case report. Urol Int 93(3): 368-370.
- Kawashima S, Urushihara N, Fukumoto K (2014) Laparoscopic repair of Bochdalek hernia with intrathoracic kidney in a 2-year-old child. Asian J Endosc Surg 7(3): 279-281.
- Shah AD, Ajay S, Adalia M, Rathi A (2012) Bochdalek hernia with intrathoracic kidney. Lung India 29(4): 373-375.
- Hatzidakis A, Kozana A, Glaritis D, Mamoulakis C (2014) Right-sided Bochdalek hernia causing septic ureteric obstruction. Percutaneous treatment with placement of a nephroureteral double pigtail. BMJ Case Rep pii: bcr2014207247.
- Etsadashvili K, Rashid HM, Jalabadze K, Melia A (2011) Bochdalek hernia as a cause of intermittent AV block. Indian Pacing Electrophysiol J 11(5): 153-155.
- Weber C, Davis CS, Shankaran V, Fisichella PM (2011) Hiatal hernias: a review of the pathophysiologic theories and implication for research. Surg Endosc 25(10): 3149-3153.
- Jetley NK, Al-Assiri AH, Al Awadi D (2009) Congenital paraesophageal hernia: a 10 year experience from Saudi Arabia. Indian J Pediatr 76(5): 489-493.
- Al-Salem AH (2000) Congenital paraesophageal hernia in infancy and childhood. Saudi Med J 21(2):164-167.
- Baglaj SM, Noblett HR (1999) Paraoesophageal hernia in children: familial occurrence and review of the literature. Pediatr Surg Int 15(2): 85-87.
- Takamatsu H, Akiyama H, Noguchi H, Tahara H, Adachi Y (1991) Association of hiatus hernia with posterolateral diaphragmatic hernia (Bochdalek’s hernia). Eur J Pediatr Surg 1(4): 244-246.
- Kshirsagar AY, Shinde SL, Ahire MD, Langade YB (2008) Congenital paraesophageal hiatus hernia with gastric volvulus. J Indian Assoc Pediatr Surg 13(1): 36-37.
- Chandraraj S, Briggs CA (1991) Congenital diaphragmatic hernia through the oesophageal hiatus with nonrotation of the midgut. A case report. J Anat 178: 265-272.
- Karpelowsky JS, Wieselthaler N, Rode H (2006) Primary paraesophageal hernia in children. J Pediatr Surg 41(9): 1588-1593.
- Leung AW, Lam HS, Chu WC, Lee KH, Tam YH, et al. (2008) Congenital intrathoracic stomach: short esophagus or hiatal hernia? Neonatology 93(3): 178-181.
- Kiszel J, Varga J (1964) Unilateral pulmonary agenesis and hiatus hernia associated with congenital malformation of large vessels. Orv Hetil 105: 749-750.
- Storch de Gracia Calvo P, Novoa Carballal R, Fernández García M, Albi Rodríguez G (2011) Congenital para-esophageal hiatus hernia as a cause of severe hyporegenerative anemia. An Pediatr (Barc) 75(6): 427-428.
- Herek O, Yildiran N (2002) A massive hiatal hernia that mimics a congenital diaphragmatic hernia. An unusual presentation of hiatal hernia in childhood: report of a case. Surg Today 32(12): 1072-1074.
- Spivey JF, Ramachandran V, Graff GR (2004) Aortic hiatus gastric hernia. Pediatr Pulmonol 37(3): 279-282.
- Zaglul HF, Odita JC (1995) Multiple herniae: a defect in the celomic mesoderm? Am J Med Genet 57(4): 537-539.






























