A Study on Fetal Wellbeing through the Non-Reactive Non-Stress Test in the Patients Referred to Motazedi Hospital, Kermanshah, Iran
Maryam Zangeneh1,2 and Mohsen Takesh2*
1,2Department of Obstetrics and Gynecology, Kermanshah University of Medical Science, Iran
2Kermanshah University of Medical sciences, Iran
Submission: March 22, 2017; Published: April 06, 2017;
*Corresponding author: Mohsen Takesh, Department of Obstetrics and Gynecology, Kermanshah University of Medical sciences, Kermashah, Iran, Email: mohsen.takesh@gmail.com
How to cite this article: Maryam Z, Mohsen T. A Study on Fetal Wellbeing through the Non-Reactive Non-Stress Test in the Patients Referred to Motazedi Hospital, Kermanshah, Iran. Anatomy Physiol Biochem Int J. 2017; 2(2): 555583.DOI10.19080/APBIJ.2017.02.555583
Abstract
A non-stress test is the first step to determine fetal well being. This study was conducted on 323 pregnant patients, referred to Motazedi hospital, Kermanshah, Iran, to justify the non-stress test's strength. 33.1% were stricken by a fetal distress and 9.9% by meconium passing, around 5% by an Apgar elows even, 5.3%were hospitalized at the NICU, and 86.4% were delivered by the cesarean section. It is believed that studied communities' size might explain the difference between our results and past ones.
Keywords: Non-stress test; Amniotic fluid; Fetal distress; Perinatal mortality
Abbreviations: NST: Non-Stress Test; AFV: Amniotic Fluid Volume; NICU: Neonatal Intensive Care Unit
Introduction
Since 1975, the non-stres stest (NST) has been applying as a first step to assess fetal well being. Over past decades, antepartum fetal heart rate testing has become an integral part in high-risk pregnancy management. During this time,the contraction stress test has given way to the non-stress test for primary fetal surveillance due to its proven reliability and its low false negative rate [1-4]. The main feature of normality to interprete the testis FHR accelerations, i.e., reactive tracing. Accelerations, which resemble aspike-like or transitory increase above baseline as a result of sympathetic nervous system stimulation, have been shown to be reassuring both antepartum and intrapartum [1,2,5-7], and indicate a non-acidotic fetus [1,8].
The suggested optimum number of accelerations varies in the literature from one to five over a period of 20 or 30 minutes [9-11]. In contrast, the absence of accelerations (non-reactive tracing) is considered suspicious, and management of a nonreactive NST first requires extension of the recording time to 40-50 minutes. Clinical evaluations performed on shorter time intervals may be misleading [1,12,13]. However, this investigation was conducted to make an appropriate evaluation for the non-reactive NST applicability in order to predict fetal healthy, necessity of an operation special method during parturition, consideration of essential schemes and so on.
Materials and Methods
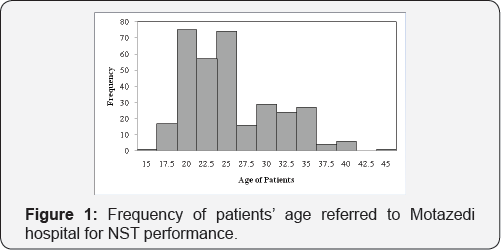
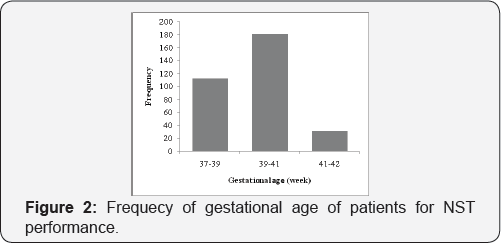
To determine a pregnancy outcome, fetal characteristics and their status through the non-reactive NST, which was performed on 323 pregnant patients with a gestationalageover28weeks, referred to Motazedi hospital, Kermanshah, Iran, abipartite form was prepared that the first part was completed at the beginning of hospitalization to consider a maternal age, a gestational age, the history of a previous or a background disease, a reason for performing the test, and the amniotic fluid volume (AFV), and the second one while patient-releasing for gestational finalization, a manner of labour, a fetal distresss (meconium passing, tachycardia, bradycardia), infant weight, an infant Apgar, perinatal mortality and hospitalization at the neonatal intensive care unit (NICU). The patients were between 15-46 years old (mean=25.33, STD=5.573, (Figure 1) and the gestational age was between 37-42 weeks (mean=38.49, STD=2.007, (Figure2) . Data analysis was statistically performed using the program SPSS (version 16 for Windows; SPSS Inc. Chicago, IL).
Results
Reason of performing NST
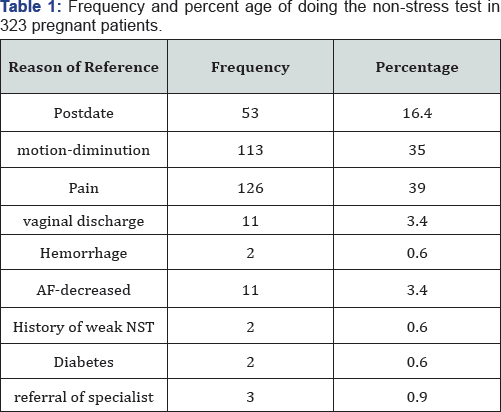
Out of 323 women, 53 individuals (16.4%) as a result of post dating, 113 persons (35%) because of decreased fetal movement, 126 (39%) for pain, eleven (3.4%) due to a vaginal discharge (suspect in membrane rupture), two (0.6%) due to hemorrhage, eleven(3.4%) as a consequence of decreasing the AFV in the sonogram, two (0.6%) because of a preceding weak NST, two (0.6%) as a result of the diabetes, and three (0.9%] due to fetal wellbeing screening referred to Motazedi hospital, Kermanshah, Iran (Table 1).
Volume of amniotic fluid
One (0.3%), 269 (83.3%), 53 (16.4%) patients had increased, normal and decreased AFV in the sonograghy, respectively,
Accompanying diseases
300 cases (92.9%) had no background disease, 13(4%) suffered from a gestational hypertent ion, 7(2.2%) from the diabetes, and three (0.9%) were afflicted by both.
Fetal distress during labor
32 cases (9.9%) striked by the meconiumstain and 107 ones (33.1%) by the tachycardia or bradycardia during the labor.
Perinatal mortality
Six cases (1.9%) had perinatal mortality and 17 ones (5.3%) were hospitalized at the NICU.
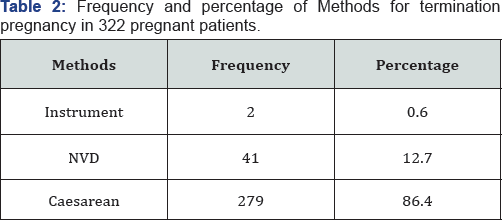
Methods of termination of pregnancy
All cases were finalized the pregnancy. Two out of them (0.6%) had an instrumental delivery, 42(13%) through a normal vaginal delivery (NVD), and 279 (86.4%) by means of cesarean (Figure 3), out of which 56 specimens (20.07%) had a history of cesarean section (repeat CD) (Table 2).
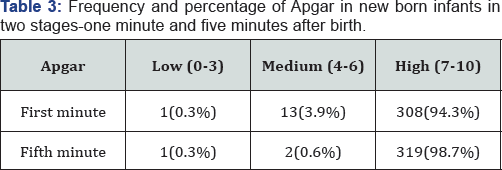
Apgar in newborn infants
First minute Apgar: one case (0.3%) had a low Apgar (03) , 13 ones (3.9%) had a medium Apgar (4-6), and 309 ones (95.6%) had a high Apgar (7-10).
Fifth minute Apgar: one case (0.3%) had a low Apgar (0-3), two (0.6%) had a medium Apgar (4-6), and 320(99%) had a high Apgar (7-10) (Table 3).
Weight of infants and hospitalization at NICU
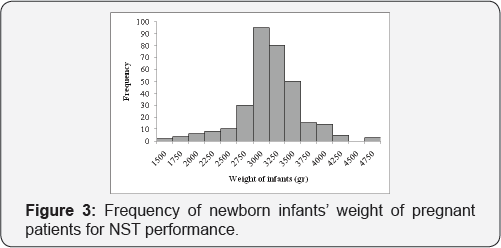
The infants' weight was between 1500-4650 grand 17 newborns (5.3%) were hospitalized at NICU (mean=3144.25, STD=463.9, (Figure 3)
Discussion
The NST is the first step to evaluate fetal healthiness. 1% has been considered as a pseudo-negative measure in which fetal fatality occurs during a following weeks in conducting the reactive NST [14]. In order to demonstrate a fetal distress, a profile biophysical test is usually conducted after the non-reactive NST; in our study, nonetheless, it had not been directed on the instances and they just labored following a non reactive NST due to a complain of pain or decreased fetal movement. Morever, 33.1% led to a fetal distress (tachycardia or bradycardia), and 86.4% delivered by the cesarean section; whereas, Lohana et al. [14] reported that 46.66% did by the cesarean section and in 8.33% a fetal distress was there as one of cesarean. Verma and Shrimali [15] and Eden et al. [16], however, assigned 63.15% and 37.7% to the fetal distress.
The meconium staining of liquor has variously been announced in publications. Schifrin et al. [17] and Patil and Gharegrat [18] recorded 39.1% and 34%; whereas Bano et al. [19] and Lohana et al. [14] reported 42.8% and 33.3%, respectively. 10% in the present study might be related to a more immediate intervention, cesarean and time wasting to perform complementary tests. In as much as this phenomenon could lead to the meconium aspiration syndrome, the number of 10% could be considered significant. First minute/below seven Apgar was registered as 4.2% where as this type of number were done as 6% and 53.3% in Verma and Shrimali [15] and Lohana et al. [14], respectively. Fifth minute/below seven Apgar in the present research is 0.9%; the numbers of Lohana et al. [14] and Bano et al. [19] were, respectively, 60% and 42.8%. Result data showed that hospitalization of the infants at the NICU is 5.3%, where as it is 28.5% in Bano et al. [19]. The sample sizes in Lohana et al. [14] and Bano [19] were 15 and 12, respectively; whereas it is 323 in the present study. This difference might be responsible for the egregious differences of statistical data.
References
- Hoh JK, Park MI, Park YS, Koh SK (2012) The significance of amplitude and duration of fetal heart rate acceleration in non-stress test analysis. Taiwan J Obstet Gynecol 51(3): 397-401.
- Lawrence D, Devoe MD (2008) Antenatal Fetal Assessment: Contraction Stress Test, Non stress Test, Vibro acoustic Stimulation, Amniotic Fluid Volume, Biophysical Profile, and Modified Biophysical Profile-An Overview. Semin Perinatol 32(4): 247-252.
- Nathan EB, Haberman S, Burgess T, Minkoff H (2000) The relationship of maternal position to the results of brief non stress tests: A randomized clinical trial. Am J Obstet Gynecol 182(5): 1070-1072.
- Wu ET, Lin TH, Lin CH, Lee CN (2014) Left ventricular assist device for stress-induced cardiomyopathy after postpartum hemorrhage. Taiwan J Obstet Gynecol 53(3): 429-431.
- Huang YF, Chen WC, Tseng JJ, Ho ESC, Chou MM (2012) FetalIntracranialHemorrhage(FetalStroke): Report of Four Antenatally Diagnosed Cases and Review of the Literature. Taiwan J Obstet Gynecol 2006; 45(2): 135-141.
- Maeda K, Utsu M, Makio A, Serizawa M (1998) Neural network computer analysis of fetal heart rate. J Matern Fetal Investig 8(4): 163171.
- Shaw SW, Chen CP, Cheng PJ (2013) From Down syndrome screening to non invasive prenatal testing: 20 years' experience in Taiwan. Taiwan J Obstet Gynecol 52(4): 470-474.
- Todros T, Preve CU, Plazzotta C, Bioleati M, Lombardo P (1996) Fetal heart rate tracings: observer versus computer assessment. Eur J Obstet Gynecol Reprod Biol 68(1-2): 83-86.
- Bracero LA, Morgan S, Byrne DW (1999) Comparison of visual and computerized interpretation of non stress test results in a randomized controlled trial. Am J Obstet Gynecol 181(5): 1254-1258.
- Spencer JA (1990) Modern antenatal care of the fetus. Blackwell Scientific Publications, pp. 163-188.
- Tongprasert F, Jinpala S, Srisupandit K, Tongsong T (2006) The rapid biophysical profile for early intrapartum fetal well-being assessment. Int J Gynecol Obstet 95(1): 14-17.
- Kashanian M, Javadi F, Haghighi MM (2010) Effect of continuous support during labor on duration of labor and rate o cesarean delivery. Int J Gynecol Obstet 109(1): 198-200.
- Tsai HF, Cheng YC, Ko HC, Kang L, Tsai PY, et al. (2013) Prenatal diagnosis of fetal gastroschis is using three-dimensional ultrasound: Comparison between the 20th and 21st centuries. Taiwan J Obstet Gynecol 52(2): 192-196.
- Lohana RU, Khatri M, Hariharan C (2013) Correlation of non stress test with fetal outcome in term pregnancy (37-42 Weeks). Int J Reprod Contracept Obstet Gynecol 2(4): 639-645.
- 15. Verma A, Shrimali L (2012) Impact of admission non stress test as a screening procedure on perinatal outcome. IJMPS 3(5): 06-10.
- Eden RD, Siefert LS, Koack LD, Trofatter KF, Killam AP, et al. (1988) A modified biophysical profile for antetal fetal surveillance. Obstet Gynecol 71: 365-339.
- Schifrin BS, Foye G, AmatoJ, Kates R, Mac Kenna J (1979) Routine fetal heart rate monitoring in the antepartum period. J Obstet Gynecol 54(1): 21-25.
- Patil SK, Gharegrat RH (1993) Correlation of NST and amniotic fluid volume in antenatal fetal monitoring. J Obstet Gynecol India 43: 178.
- Bano I, Noor N, Motwani L, Arshad Z (2012) Comparative study of Non stress Test and Fetal Acoustic Stimulation of Assessment of Fetal Wellbeing. Int Sci J Jaypee 3(2): 168-171.






























