Abstract Background
Ovarian torsion in childhood and adolescence is an uncommon gynecological emergency that requires urgent surgical intervention. Clinical presentation is often non-specific, making timely diagnosis challenging yet crucial for early detection and ovarian preservation. In this case report, we present a case of a 12-year-old girl with acute abdominal pain and vomiting. On examination, she had left flank tenderness with pain radiating to suprapubic area. Ultrasound and MRI demonstrated ovarian enlargement and edema. Ovarian torsion was diagnosed and urgent laparoscopic surgery was performed.
Keywords:Gynecological; Pediatric; Gastrointestinal; Urinary Tract; Magnetic Resonance Imaging
Introduction
Ovarian torsion is rare entity in pediatric and adolescent patients. The occurrence of ovarian torsion in females aged 1 to 20 years is approximately 4.9 per 100.000 [1]. Despite its low incidence rate, ovarian torsion should be considered in the differential diagnosis of every young girl who presents with any degree of abdominal pain [2]. Predisposing factors of ovarian torsion in pediatric patients include longer and laxer uteroovarian ligaments, small size of uterus providing less stabilization, ovarian hypermobility and prepubertal hormonal changes. Ovarian torsion often occurs in the presence of ovarian cyst, benign neoplasm or less commonly malignancy.
The mechanism of ovarian torsion is like that in adults: twisting of supporting ovarian ligaments causing venous obstruction initially, edema and further arterial ischemia causing infarction and necrosis. However, due to hypermobility of pediatric ovaries, torsion can occur earlier and with fewer risk factors. Polycystic ovarian morphology with increased ovarian volume as in our case also may play a role as a predisposing factor for torsion. The clinical presentation of ovarian torsion is typically nonspecific abdominal pain and may mimic some gastrointestinal or urinary tract pathologies which may result in delayed diagnosis increasing the risk of irreversible ischemia and ovarian loss. Imaging plays a crucial role in early diagnosis, particularly when clinical findings are nonspecific.
Case Presentation
The patient is a 12-year-old girl who presented to emergency department with severe left-sided abdominal pain associated with persistent vomiting for the past two days. On physical examination left flank tenderness was noted with radiation to suprapubic area, there was no diarrhea or fever. Pelvic ultrasound with Doppler demonstrated bilaterally enlarged ovaries with small follicles with a markedly enlarged left ovary showing reduced vascularity and no evidence of identifiable ovarian cyst (Figures 1-4). Magnetic resonance imaging (MRI) demonstrated bilateral ovarian enlargement with multiple small follicles, assuming polycystic ovarian morphology. The left ovary was significantly enlarged, positioned posterior to the uterus and showed stromal edema with decreased post-contrast enhancement compared to contralateral side, findings consistent with ovarian torsion (Figures 5-10).
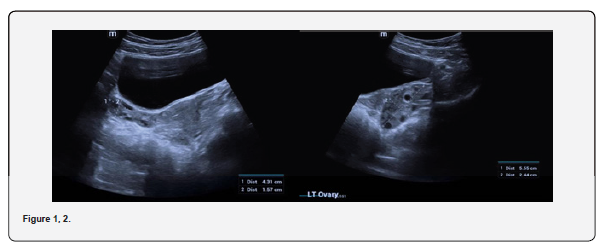
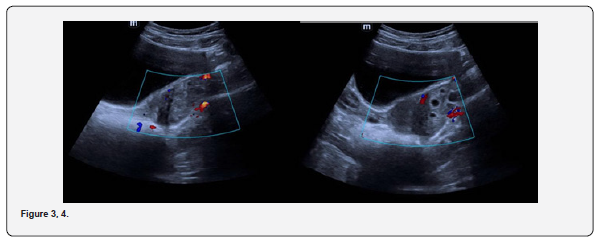
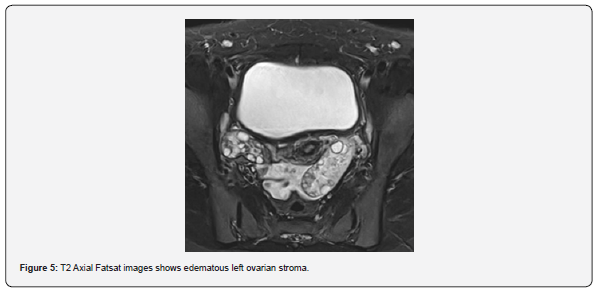
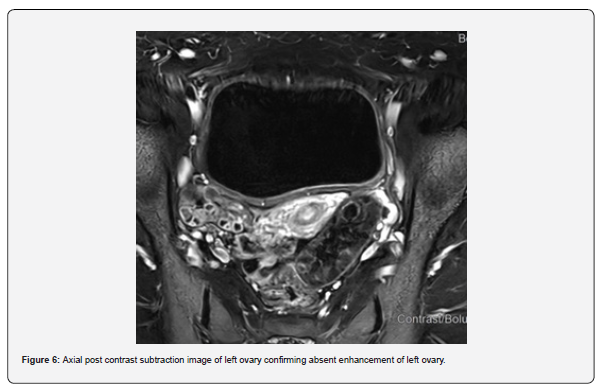
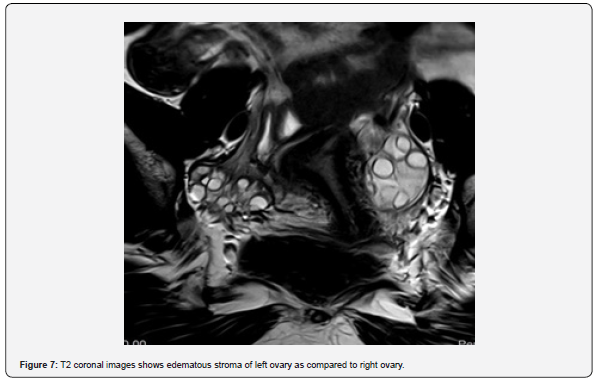
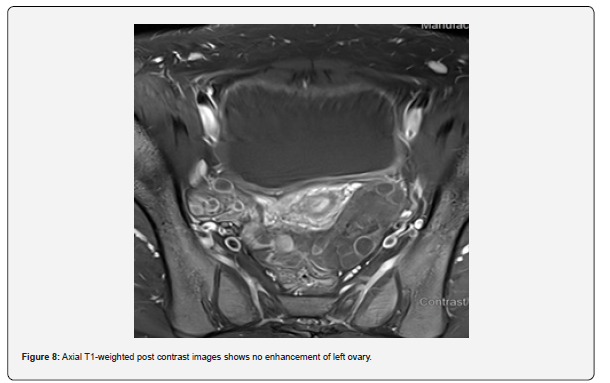
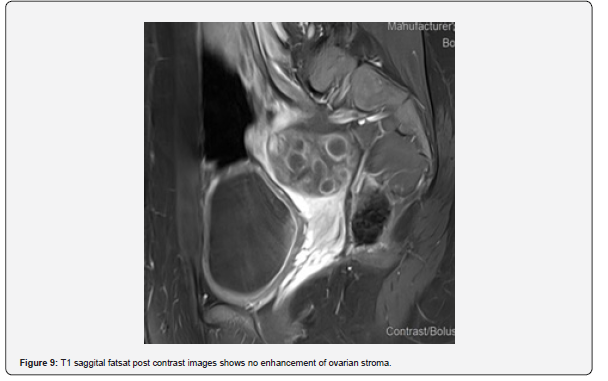
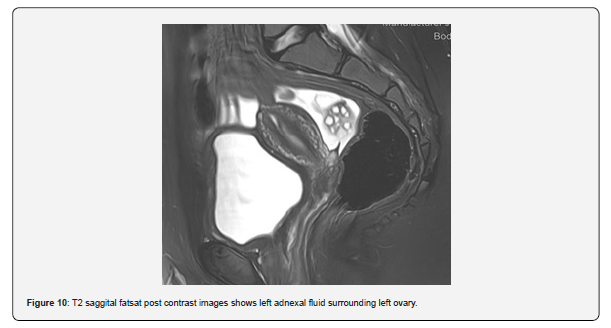
No definite ovarian cyst was identified on MRI. Mild free fluid was noted in the left adnexa. Patient underwent emergency laparoscopy and ovarian torsion was confirmed intraoperatively. Left ovary was found enlarged and torsed with two twists. A small ovarian cyst measuring approximately 2x2 cm was detected. Ovarian sparing laparoscopic detorsion of the left ovary was performed with cyst marsupialization. Patients were discharged on postoperative day 3 in stable condition. Follow-up visit in clinic after one week showed uneventful recovery. This case report highlights the importance of prompt diagnosis of ovarian torsion for timely surgical intervention even in absence of detectable cyst on imaging. aiming to preserve ovarian torsion and future fertility.
Discussion
Ovarian torsion is an uncommon but significant cause of acute abdominal pain in pediatric and adolescent patients. It is a surgical emergency.as delayed diagnosis and treatment may lead to ovarian ischemia, necrosis and loss of ovarian function. In children, diagnosis is often difficult because symptoms are nonspecific and can mimic other common causes of acute abdomen, such as appendicitis, renal colic or gastrointestinal pathologies. Previously reported literature review of 14 studies found that Sudden onset abdominal pain with nausea/vomiting is the most common symptom occurring in 88.4% of cases [3]. Ultrasound with Doppler assessment is the first line imaging modality for suspected ovarian torsion due to its wide availability, easy and fast use in emergency settings and low cost.
Common ultrasound findings include ovarian enlargement, peripheral displacement of follicles, heterogenous ovarian echotexture due to edema and reduced or absent blood flow, However, normal or preserved blood flow does not exclude ovarian torsion, particularly in cases of intermittent torsion. Previous studies have reported that the presence of Doppler flow on ultrasound cannot be used to exclude ovarian torsion whereas the absence of Doppler flow represents a significant diagnostic marker [4]. Emergency medicine literature similarly reports that Doppler flow may be present in cases of ovarian torsion and should not be used alone to exclude the diagnosis [5]. In the present case, ultrasound showed ovarian enlargement with decreased blood flow, which raised suspicion for torsion despite the absence of a clearly identifiable ovarian cyst or mass.
This finding demostrates the limitations of imaging in detecting small or subtle ovarian lesions and highlights the importance of clinical judgement together with supportive imaging findings when evaluating suspected ovarian torsion. Polycystic ovarian morphology in pediatric patients should also be considered a potential risk factor for ovarian torsion, even when a dominant cyst is not present. Additionally, MRI demonstrated bilateral polycystic ovarian morphology, with greater enlargement of the affected ovary. Increased ovarian volume associated with polycystic morphology has been reported as a possible predisposing factor for ovarian torsion. In this case, asymmetric ovarian enlargement in the setting of polycystic morphology may have increased the susceptibility of the affected ovary to torsion.
From an anatomical perspective, ovarian torsion occurs when the ovary rotates around its supporting ligaments, most commonly the utero-ovarian ligament and infundibulopelvic ligament, leading to compromised venous drainage, followed by arterial obstruction if torsion persists. In pediatric patients, several anatomical and developmental factors increase ovarian mobility and predispose it to torsion. These factors include relatively longer uteroovarian and infundibulopelvic ligament, lax pelvic supporting structures, reduced pelvic fat, and a smaller uterus, all of which provides less stabilisation of the ovary and allow greater range of movement.
These anatomical and developmental factors, including increased ligamentous laxity and adnexal mobility have been documented as important risk factors for ovarian torsion in pediatric patients, even in the absence of large adnexal mass [6]. In the present case, intraoperative findings revealed a small ovarian cyst that was not detected on ultrasound or MRI. This discrepancy may be explained by torsion related ovarian edema, hemorrhage and distortion of normal ovarian anatomy, which can obscure small cysts on imaging studies. This case underscores that the absence of visible ovarian cyst on imaging does not exclude ovarian torsion and highlights the importance of correlating imaging findings with clinical presentation and clinical judgement.
Early surgical intervention remains essential when ovarian torsion is suspected, even when imaging findings are inconclusive. Prompt diagnosis and timely management are critical to maximizing ovarian preservation, which is particularly important in pediatric patients. This case further demonstrates the limitations of imaging modalities in detecting small ovarian cysts or masses associated with torsion related changes. However, these limitations should not outweigh clinical judgement or supportive imaging signs suggestive of ovarian torsion as in pediatric patients’ torsion can occur without a large adnexal mass or cyst.
Conclusion
Ovarian torsion in pediatric patients remains a diagnostic challenge due to non-specific symptoms and variable imaging findings. Although ultrasound with Doppler and MRI are important diagnostic tools, the absence of visible ovarian cyst or definitive imaging features does not exclude torsion. Anatomical factors related to pediatric patients, as well as conditions such as polycystic ovarian morphology, may increase ovarian mobility and susceptibility to torsion.
Early recognition and urgent surgical intervention are essential to preserve ovarian function and future fertility. This case emphasizes the importance of maintaining a high level of clinical suspicion and prioritizing clinical judgement when imaging findings are inconclusive. Clinical judgement and supportive imaging signs remain critical to timely diagnosis and ovarian preservation in pediatric patients.
Ethical Approval
This case report was approved by the ethics committee, Al Ahli hospital, Doha, Qatar. A copy of the approval letter is available for review by the Editor-in-Chief of this journal on request.
Consent
Verbal and written informed consent were obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
References
- Guthrie BD, Alder MD, Powell EC (2006) Incidence and trends of paediatric ovarian torsion hospitalizations in the United States, 2000-2006, Pediatrics 125(3): 532-538.
- Chang YJ, Yan DC, Kong MS, et al. (2008) Adnexal torsion in children. Pediatric Emergency Care 24(8): 534-537.
- Celine Rey-Bellet Gasser, Mario Gehri, Jean-Marc Joseph, Jean-Yves Pauchard (2016) Is it ovarian torsion? A systematic literature review and evaluation of prediction signs. Pediatr Emerg Care 32: 256-261.
- Sims MJ, Price AB, Hirsig HR Hill JG, Titus MO (2022) Pediatric ovarian torsion: should you go with the flow? Pediatr Emerg Care 38(6): e1332- e1335.
- Pediatric Ovarian torsion (2015) EMRA.
- Scheier E (2022) Diagnosis and management of pediatric ovarian torsion in the Emergency department: Current insights. Open access Emergency Medicine 14: 283-291.






























