Factors Associated with Hand Washing Among Healthcare Personnel in Delivery Points at a Tertiary Care Hospital, South India
Haezel Ann Shibu*, B Adhisivam, Latha Chathurvedula and Abdul Basith
1 Intern, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Gorimedu, Puducherry, India
2 Professor, Department of Neonatology, JIPMER, Gorimedu, Puducherry, India
3 Professor, Department of Obstetrics and Gynaecology, JIPMER, Gorimedu, Puducherry, India
4 Junior resident, Department of Preventive and Social Medicine, JIPMER, Gorimedu, Puducherry, India
Submission:January 05, 2024;Published: January 17, 2024
*Corresponding author: Haezel Ann Shibu, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Gorimedu, Puducherry, India
How to cite this article: Haezel Ann Shibu, B Adhisivam, Latha C, Abdul B. Factors Associated with Hand Washing Among Healthcare Personnel in Delivery Points at a Tertiary Care Hospital, South India. Acad J Ped Neonatol 2024; 13(3): 555919. 10.19080/AJPN.2024.13.555919
Abstract
Objectives: Neonatal sepsis is a major cause of neonatal mortality worldwide. Inadequate hand hygiene practices of healthcare workers (HCWs) at delivery points are a major causative factor of early-onset sepsis (EOS). This study aims to assess the prevailing hand washing practices of HCWs at delivery points and analyse the factors affecting these practices.
Methods: A questionnaire-based, descriptive study was conducted in JIPMER, a tertiary care hospital in South India. Resident doctors, nurses, and interns posted at delivery points were recruited as participants. Hand hygiene practices of different groups were reported as frequencies and percentages. Factors affecting hand hygiene were scored on a five-point Likert scale and reported as median with inter-quartile range.
Results: Nurses were found to have highest overall hand hygiene compliance, while interns reported the highest proportions of hand hygiene with respect to handling newborns. Non availability of means to dry hands near washing areas, overuse of gloves, staff shortages, emergency situations, and high patient load were some of the factors found to impede hand hygiene. Installation of CCTVs near washing areas and supervision by seniors were reported as factors that could improve hand washing.
Conclusion: Even though nurses reported the highest overall hand hygiene compliance, they need to observe better hand washing practices before handling newborns. Among the factors found to facilitate and impede hand hygiene, some of them can easily be corrected to optimize hand hygiene practices at delivery points, to reduce EOS.
Keywords: Neonatal Sepsis; Hand Washing; Delivery Points; Healthcare Workers; Early Onset Sepsis
Introduction
Globally, neonatal sepsis is a major health problem and the third leading cause of neonatal mortality [1,2]. An estimated 3 million neonates are affected by sepsis worldwide (22 per 1000 live births) with a mortality of 11 - 19% [3]. Its incidence in developing countries like India is 10 times more than in developed countries [4]. 99% of global neonatal mortality due to sepsis occurs in low and middle-income countries [5]. Early onset sepsis (EOS) is the development of sepsis within the first 72 hours of life. One of the major factors contributing to the development of EOS is poor adherence to hand hygiene practices by healthcare workers (HCWs) at delivery points [1]. Other factors like low birth weight, invasive procedures, delayed or inadequate breastfeeding, and overcrowding in neonatal units can also contribute to neonatal sepsis [6,7]. However, a very easy and cost-effective measure to reduce sepsis in neonates is the implementation of proper hand hygiene practices among HCWs at delivery points [8]. Hence, it is important to analyse the factors that facilitate or impede hand washing among these HCWs, to take appropriate corrective measures. There is a paucity of literature regarding factors leading to reduced hand washing at delivery points in India, which makes this a very relevant study in the Indian context, to make recommendations for better hand hygiene practices.
Methods
After obtaining due approval from the Institute Ethics Committee (JIP/IEC-OS/2022/308), this descriptive study was conducted at Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), a tertiary care hospital, in South India, during Jan - Feb 2023. The participants of the study included three groups of HCWs who worked at the delivery points: resident doctors (senior and junior residents), nurses, and interns. After obtaining informed consent, participants were administered a self-reported questionnaire with responses recorded on a five-point Likert scale. The questionnaire had two parts - the first part assessed the adequacy of hand hygiene practice, whereas the second part assessed the factors affecting hand washing practices. Anonymity of the participants was maintained in the survey. The data collection period was 2 months.
Statistical Analysis
Data was collected using Epicollect-5 and analyzed using STATA v 14 (StataCorp Texas, US). The first seven questions assessed the adequacy of hand hygiene practice among HCWs at delivery points. Responses of ‘always’ and ‘often’ were considered satisfactory, while ‘sometimes’, ‘rarely’, and ‘never’ were considered unsatisfactory hand hygiene practices. If a participant had 4 or more responses satisfactory out of seven, their overall hand hygiene practice was reported to be satisfactory. The frequencies and proportions of satisfactory hand hygiene practices among resident doctors, nurses, and interns were calculated. Different groups were compared using Pearson chi-squared or Fisher’s exact test. The next part of the questionnaire focused on factors affecting hand hygiene, which were classified as patient factors, peer factors, and work environment related factors. The Likert scale score for each factor was represented as the median with interquartile range. Kruskal-Wallis and Wilcoxson rank-sum tests were used to assess the statistical significance. A p-value < 0.05 was considered statistically significant.
Results
Responses were collected from 133 participants, including residents (n=24), nurses (n=21), and interns (n=88) posted at delivery points during the study period.
Current Hand Hygiene Practices of Hcw’s in Delivery Points
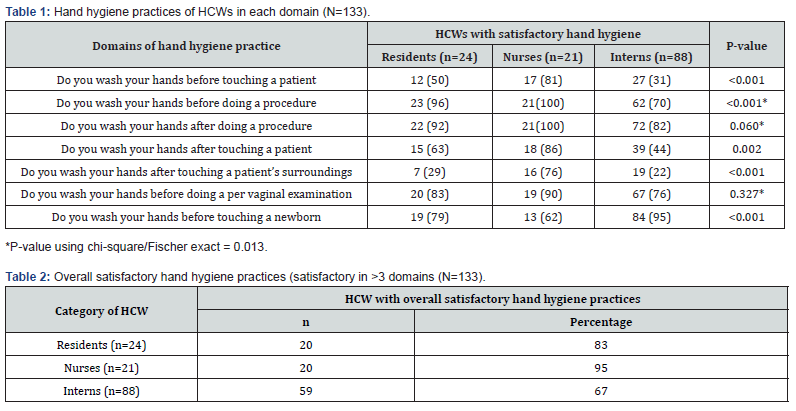
The five moments of hand hygiene, as described by WHO, were followed in the highest proportion by nurses, followed by residents. Interns recorded the lowest proportions in following these practices. All nurses reported that they would wash their hands before and after doing a procedure, compared to 70-80% of interns and more than 90% of residents. The numbers were significantly lower for hand washing before and after touching a patient. Only half of all residents reported hand washing before touching a patient and less than one-third performed hand washing after touching a patient. These numbers were less than 30% for interns, while nurses reported 75-80% compliance. However, the numbers were reversed with respect to hand washing before touching a newborn, with the highest proportions reported by interns (95%), followed by residents (79%), and nurses (62%). With respect to overall hand washing practice, nurses reported the highest satisfactory hand hygiene (95%), while interns reported the lowest satisfactory hand hygiene practices (67%). The responses of HCWs regarding their hand washing practices are described in Table 1 and the overall hand washing practices among HCWs are described in Table 2 respectively.
Factors Affecting Hand Hygiene Practices
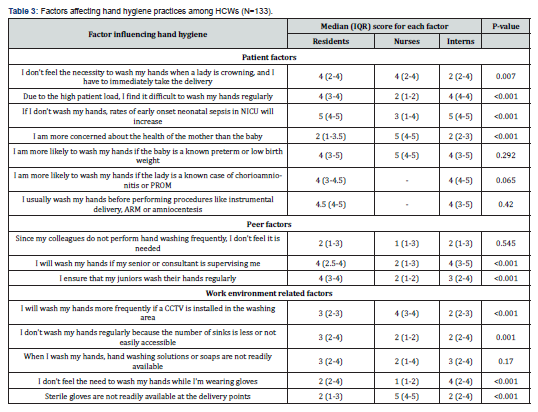
According to resident doctors, the major hindering factor for hand washing was the high patient load in delivery rooms. Another factor that deterred hand washing was emergency situations, for example, if a lady was crowning and they had to immediately conduct the delivery. Most residents reported that supervision by a senior or consultant would increase hand hygiene. They also agreed that they were more likely to wash their hands if the lady was a known case of chorioamnionitis or PROM or if the child was a known preterm or LBW. Residents reported washing their hands before performing invasive procedures (like instrumental delivery, ARM, or amniocentesis). Majority of residents at delivery points were concerned about the health of the baby as well and recognised that if they did not wash their hands, rates of EOS would rise. Nurses posted in delivery points reported to be more concerned about the health of the mother than the baby. However, they would be more likely to wash their hands if the baby was a known preterm or LBW. Nurses also reported that installing CCTVs in washing areas would promote hand washing. In contrast to residents, nurses did not find the high patient load or urgent situations to be a hindering factor for hand washing. Majority of nurses also reported that sterile gloves were not readily available at delivery points. According to interns posted in labour rooms, the main factor that hindered hand washing was the high patient load. They also reported that they did not feel the need to wash their hands if they were wearing gloves. Like residents, they were more likely to wash their hands if the lady was high risk or if the baby was a known preterm or LBW, and they acknowledged that rates of EOS would rise if they did not wash their hands while handling newborns at delivery points. Supervision by their seniors was another factor that they agreed would increase hand washing. Apart from the set questions, a factor mentioned by many participants that would facilitate hand washing was the availability of a means to dry hands in a sterile manner near washing areas, for e.g. tissues or clean towels. Some participants, especially nurses, mentioned that shortage of staff was a factor that hindered hand hygiene in labour rooms. Increased use of hand sanitizers and gloves was also thought to be a factor that led to reduced hand washing. Table 3 describes the factors affecting hand hygiene among HCWs at delivery points.
Discussion
This study analysed the current hand hygiene practices of HCWs at delivery points and the factors which affected these practices. With respect to existing hand hygiene practices, the five moments of hand hygiene as described by WHO were reported to be followed in the highest proportion by nurses, followed by residents. Interns reported the lowest numbers in following these practices. A study from Tamilnadan about hand hygiene among HCWs reported similar results. As per the study, nurses were more compliant to appropriate hand hygiene practices than doctors and other healthcare staff [9]. However, interns reported the highest proportions of hand washing before touching a newborn. This shows that they are more aware of the implications of hand hygiene before handling newborns in delivery rooms and its impact on neonatal sepsis. A major factor that hindered hand washing at delivery points was the high patient load. Staff shortage at delivery points was another factor. This is like the findings of a study conducted at a government hospital in Uttarakhand which reports that under-staffing of HCWs and heavy patient load leads to poor adherence to hand hygiene [10].
Some respondents stated that a means to dry hands in a sterile manner near washing areas was not available, which led to decreased hand washing. Therefore, implementing measures like clean towels or tissues near washbasins to dry hands could improve hand hygiene compliance [11]. It was reported that supervision by seniors or consultants and installing CCTVs near the washing areas would likely improve hand hygiene compliance at delivery points. This was in accordance with the findings of studies done in neonatal ICUs in India where it was found that educational interventions, along with healthcare associated infection surveillance, monitoring of hand hygiene using CCTVs, and regular feedback meetings can improve hand hygiene compliance among HCWs [12,13]. Another study conducted in a neonatal and Pediatric intensive care unit in India demonstrated that the use of an electronic infrared tap with voice reinforcement significantly improved hand hygiene compliance among HCWs [14].
Many nurses also reported that they were more concerned about the health of the mother than the baby and that they were more likely to wash their hands if the baby was a known preterm or LBW as compared to a normal newborn. Therefore, providing multimodal educational interventions about the importance of hand washing in delivery points and its role in reducing EOS would be beneficial in improving hand hygiene as demonstrated by many studies [8,12,15-19]. Interns reported that they did not feel the necessity to wash their hands if they were wearing gloves. Increased use of gloves was also stated as a factor that hindered hand washing. However, WHO states that gloves should be worn only when indicated, and glove use does not modify hand hygiene indications or replace hand hygiene action [20]. A study conducted in a tertiary care hospital in India corroborates this observation, stating that glove use is associated with poor hand hygiene compliance [21]. Therefore, educating HCWs about the importance of hand washing before wearing gloves and the proper indications to wear gloves, as described by WHO, could lead to improved hand hygiene practices. The main limitation of this study is that the results are based on self-reported questionnaires.
Conclusion
This study discusses existing hand hygiene practices of HCWs at delivery points and the factors that affect these practices. Nurses reported better compliance with overall hand washing practices compared to other HCW’s. However, intern doctors observed better hand hygiene before handling newborns at delivery points, while nurses reported the lowest numbers in this area. High patient load and staff shortages were factors reported to impede hand hygiene. Providing tissues or clean towels near washing areas is an easy and cost-effective measure that could improve hand washing practices. Other measures that could improve hand hygiene compliance include CCTVs to monitor hand hygiene compliance, supervision by seniors/consultants, and providing multimodal educational interventions highlighting the importance of hand washing at delivery points. HCWs also need to be sensitized on the proper indications to use gloves and that glove use does not substitute for hand washing if it is indicated, as per WHO guidelines. Some of these corrective measures could easily be implemented in hospitals to optimize hand hygiene at delivery points and reduce rates of sepsis in neonates.
Acknowledgements
We greatly acknowledge Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Puducherry, for allowing us to conduct this study.
Financial Disclosure Statement
No funds, grants or other support was received to conduct this study.
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript.
Informed Consent
Informed consent has been obtained from all participants of the study. Approval has been obtained from the Institute ethics committee (JIP/IEC-OS/2022/308).
References
- Nalule Y, Buxton H, Macintyre A, Ir P, Pors P, et al. (2021) Hand Hygiene during the Early Neonatal Period: A Mixed-Methods Observational Study in Healthcare Facilities and Households in Rural Cambodia. Int J Enviro Res Public Health 18(9): 4416.
- Fanaroff AA, Fanaroff JM (2020) Advances in Neonatal Infections. Am J Perinatol 37(Suppl 2): 5-9.
- Molloy EJ, Wynn JL, Bliss J, Koenig JM, Keij FM, et al. (2020) Neonatal sepsis: Need for consensus definition, collaboration and core outcomes. Pediatr Res 88(1): 2-4.
- Wa K, Mathai S (2002) Newer concepts and management of neonatal sepsis. Medical Journal Armed Forces India. 58(2): 138-142.
- Milton R, Gillespie D, Dyer C, Taiyari K, Carvalho MJ, Thomson K, et al. (2022) Neonatal sepsis and mortality in low-income and middle-income countries from a facility-based birth cohort: an international multisite prospective observational study. The Lancet Global Health 10(5): e661-672.
- Afroza S (2007) Neonatal sepsis - a global problem: an overview. Mymensingh Med J 15(1): 108-114.
- Vain N, Fariña D, Vázquez L (2012) Neonatology in the emerging countries: the strategies and health-economics challenges related to prevention of neonatal and infant infections. Early Human Development 88: S53-S59.
- Chhapola V, Brar R (2014) Impact of an educational intervention on hand hygiene compliance and infection rate in a developing country Neonatal Intensive Care Unit. Int J Nurs Pract 21(5): 486-492.
- Krishnamoorthy Y, Kala M, Kuberan D, Krishnan M, Tondare D (2023) Compliance with hand hygiene practices and its appropriateness among healthcare workers during COVID-19 pandemic in public health facilities of Tamil Nadu, India. Heliyon 9(4): e15410.
- Kumar R, Gupta PK, Sharma P, Kaur Ravneet, Reetu et al. (2017) Hand hygiene, attitude and barriers among health care workers at a tertiary care teaching hospital, Uttarakhand. Int J Health Sci Res 7(9): 159-165.
- De Barra M, Gon G, Woodd S, Graham WJ, De Bruin M, et al. (2021) Understanding infection prevention behaviour in maternity wards: A mixed-methods analysis of hand hygiene in Zanzibar. Soc Sci Med 272: 113543.
- Gopalakrishnan S, Chaurasia S, Sankar MJ, Paul VK, Deorari AK, et al. (2021) Stepwise interventions for improving hand hygiene compliance in a level 3 academic neonatal intensive care unit in North India. J Perinatol 41(12): 28342839.
- Rakshit P, Nagpal N, Sharma S, Mishra K, Kumar A, et al. (2023) Effects of implementation of healthcare associated infection surveillance and interventional measures in the Neonatal Intensive Care Unit: Small Steps matter. Indian J Med Microbiol 44:100369.
- Kathirvel M, Murugesan A, Sastry A, Adhisivam B (2023) Effect of Electronic Infrared Tap with Voice Reinforcement on Hand Hygiene Compliance of Healthcare Personnel. Indian Pediatr 60(9): 744-747.
- Amaan A, Dey SK, Zahan K (2022) Improvement of hand hygiene practices among the healthcare workers in a Neonatal Intensive Care Unit. Can J Infect Dis Med Microbiol 2022: 1-7.
- Deshommes T, Nagel C, Tucker R, Dorcélus L, Gautier J, et al. (2020) A Quality Improvement Initiative to Increase Hand Hygiene Awareness and Compliance in a Neonatal Intensive Care Unit in Haiti. Journal of Tropical Pediatrics 67(3).
- Johnson J, Latif A, Randive B, Kadam A, Rajput U, et al. (2022) Implementation of the Comprehensive Unit-Based Safety Program to Improve Infection Prevention and Control Practices in Four Neonatal Intensive Care Units in Pune, India. Front Pediatr 9: 794637.
- Kaur S, Thomas A, Biswal M, N Rao K, Vig S (2019) Effectiveness of hand hygiene promotional program based on the WHO multimodal hand hygiene improvement strategy, in terms of compliance and decontamination efficacy in an Indian tertiary level neonatal surgical intensive care unit. Indian J Med Microbiol 37(4): 496.
- Laskar AM, Bhat P, Pottakkat B, Narayan S, Sastry AS, et al. (2018) A multimodal intervention to improve hand hygiene compliance in a tertiary care center. American Journal of Infection Control 46(7): 775-780.
- (2009) World Health Organization. Glove Use Information Leaflet. Geneva: World Health Organization.
- Kaur K, Mumtaz Rahim V, Yadav S, Srinivas V, Devrani S, et al. (2020) An observational study to assess hand hygiene compliance rate among health care workers at a tertiary care hospital. Medical Journal of Dr DY Patil Vidyapeeth 13(1): 66-70.






























