Iatrogenic Esophageal Perforation in Preterm Neonate Managed Conservatively
Mohamed Gaber Elsayed*
Department of surgery, Faculty of medicine, Jazan university, Jazan, Saudi Arabia
Submission:November 09, 2023;Published: December 01, 2023
*Corresponding author: Mohamed Gaber Elsayed, Department of surgery, Faculty of medicine, Jazan university, Jazan, Saudi Arabia
How to cite this article: Mohamed Gaber Elsayed. Iatrogenic Esophageal Perforation in Preterm Neonate Managed Conservatively. Acad J Ped Neonatol 2023; 13(2): 555911. 10.19080/AJPN.2023.13.555911
Abstract
We present a premature male neonate in whom insertion of a nasogastric tube for feeding resulted in perforation injury of the esophagus, which is a conceivable fatal condition. Esophageal perforation in Infants is usually iatrogenic. A chest radiograph in suspected cases, along with careful inspection of the nasogastric tube in relation to surrounding structures, can lead to the diagnosis of this condition; flexible endoscopy is also helpful to confirm the perforation site. Surgery is avoided in most cases, and management is usually conservative. The outcome is not always favorable, especially as premature infants are at risk of associated pathology.
Keywords: Nasogastric Tube; Esophageal Perforation; Preterm Infant; Iatrogenic Injury; Broad-Spectrum Antimicrobial Therapy
Abbreviations: NGT: Nasogastric tube; TPN: Total Parenteral Nutrition
Introduction
Nasogastric tube (NGT) insertion is one of the procedures that is commonly done for feeding in extremely low- birth-weight infants. The incidence of mislaying NGTs in children is difficult to determine because of the differing definitions across studies; however, it has been reported to be as high as 21 - 43.5%. [1,2] The complications of tube malposition range from aspiration pneumonia and pneumothorax to perforation of the esophagus or the stomach. Iatrogenic esophageal injury in the neonates usually occurs at the pharyngoesophageal junction where the lumen is narrowed by the cricopharyngeus muscle. [3,4] Over the past decade, a shift from an urgent surgical intervention to more wise, nonsurgical management of esophageal perforation in selected adult patients has been reported. [5,6] In children although the most important prognostic factor is the time span between the injury and the initiation of treatment, The experience in managing esophageal perforation, especially in extremely low-birth-weight infants, is relatively lacking [3,7]. We described one case of probable iatrogenic esophageal perforation was adequately managed by watchful waiting for 2 weeks of broad-spectrum antimicrobial therapy.
Case presentation
A male baby was admitted to our ward complaining of cyanosis on feeding and respiratory distress since birth otherwise heart rate, temperature and blood pressure was within normal parameters according to age. Birth history was normal spontaneous vaginal delivery after 30 weeks’ gestation with a birth weight of 1.3 g. The pregnancy was not complicated. Umbilical venous and arterial catheters were fixed. A radiopaque polyvinyl chloride nasogastric tube (Argyle 5F, 36 inches/91.44 cm long) was inserted by a resident physician at a nearby hospital. He was admitted to a referring hospital because of respiratory distress and Chest radiography showed hyaline membrane disease. The baby improved initially after two doses of surfactant and was started on total parenteral nutrition (TPN). Oral feeding was also started on the 5th day with expressed breast milk, the amount of which increased slowly. Three days after, while the baby was stable on low ventilator settings, he suddenly deteriorated with apnea, hypotension and desaturation.
On clinical examination, there was diminished air entry, especially on the right side of the chest, and heart sounds were muffled. Immediate chest radiography confirmed a right-side pneumothorax and collapsed lung. A chest tube was inserted at right 5th intercostal space (Figure 1) and the drainage was milky in nature, so we made a provisional diagnosis of esophageal perforation. This was confirmed by careful and slow injection of 1 ml contrast solution into the nasogastric tube under fluoroscopic guidance while monitoring oxygen saturation and blood pressure. There was free flow of contrast material into pleural cavity and extra pleural indicating right pneumomediastinum at level of the thoracic esophagus and collapse of right lung. Oesophgoscopy was done revealing minor tear in middle esophagus confirming our provisional diagnosis, so we decided to continue our conservative management plan. A repeated chest radiograph showed settled pneumothoraces with no evidence of pneumomediastinum. The baby became very sick. Septic workup was done, and broad-spectrum antibiotics were administered.
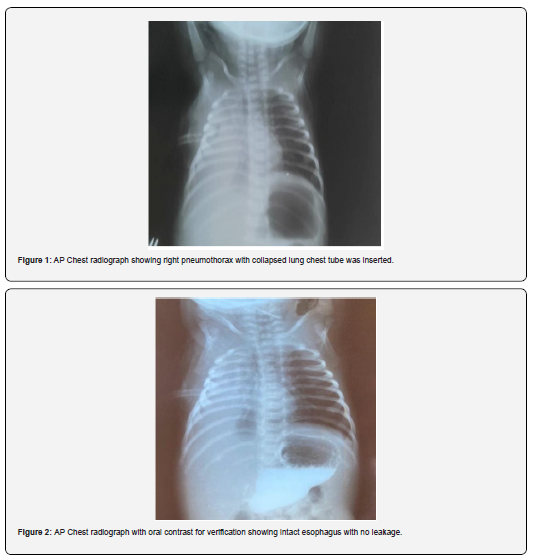
He was kept NPO with total parenteral nutrition supplement and broad-spectrum antimicrobial therapy (both antibiotic and antifungal agents), infants survived without significant complications. Enteral feeding through NGTs was restarted in these patients nine days later and chest tube was removed, no complications were noted. Preventive plan of action, including gentle manipulation, softening of NGTs, use of lubricants, verification prior to feeding by contrast study (Figure 2), and prolonged intervals for replacement (interval for planned change of feeding catheters: from 3-5 days), were initiated in this neonatal intensive care unit. These guidelines are considered effective because complications were not noted thereafter. Five days later the baby’s general condition improved, oral feeding resumed with no clinical evidence of respiratory distress and chest radiograph revealed expansion of right lung zone. On the next day he was discharged from neonatal intensive care unit.
Discussion
Tube feeding is widely used in intensive care units to meet the nutritional needs of low-birth-weight infants. It is an appropriate and efficient method of alimentation with a relatively low risk of significant complication. [4,6] Esophageal injury is not a common complication of nasogastric intubation; however, it could be fatal; premature infants and those of very low birth weight are most at risk [2,5]. Mortality rate could reach up to 20–30% in affected cases [1,8]. Although some measures could help such as mechanical ventilation, hemodynamic monitoring, TPN and effective antibiotic therapy, this figure remains high [9]. Esophageal perforation injury divided to three patterns pseudodiverticulum, mucosal perforation where limited extravasation extends posteriorly in a blind-ending submucous tract, and full-thickness esophageal injury with free intrapleural leak of air/esophageal contents [2,10]. Proximal esophageal perforation normally gives signs and radiological abnormalities on the left side of chest radiograph while distal perforation gives signs and radiological abnormalities on the right [3,7]. Most common causes of injury to the esophagus are iatrogenic injuries and account for up to 73% of the cases in reported series [6,11,12]. The commonest anatomical site of perforation is the thoracic esophagus, followed by the cervical esophagus [11,12]. Iatrogenic cervical perforations occur mostly on the posterior wall of the esophagus through the cricopharyngeal muscle due to absence of a longitudinal muscle group and lack of protective serosa layer decrease the thickness of the wall of the esophagus.
Moreover, there is considerable narrowing of the esophagus in this region [6,9]. Chest radiography is the most reliable modality for confirmation of nasogastric tube position seeing the tip of the tube is positioned below the level of the gastroesophageal junction [3,7]. The abnormal position of the nasogastric tube on the chest radiograph easily suggested perforation of the esophagus. The diagnosis was confirmed using a water-soluble contrast study. Only a small amount of contrast material was used, and the study was done under fluoroscopic guidance. The likelihood of this complication could be avoided by adequate tube lubrication, use of gentle pressure at insertion and guidance of the tube into the esophagus manually with an index finger. After nasogastric intubation, the clinical confirmation of correct position of nasogastric tube requires insufflating air while auscultating at the epigastrium and by aspirating gastrointestinal contents via the tube [4,5,10]. Moreover, using silastic nasogastric tubes reported less episodes of esophageal perforation than polyvinyl tubes in very-low-birth-weight infants [11]. Unfortunately, associated pathology often complicates the outcome. These complications can be localized to esophagus itself (esophageal dysmotility or an esophageal stenosis) or affecting other systems (severe respiratory distress, bronchopneumonia, abscess, mediastinitis, fatal septicemia, bronchodysplasia or necrotizing enterocolitis).
Surgical repair is still the cornerstone of management, but recently there has been a tendency toward more conservative management. Many studies reported the effectiveness of nonsurgical management in selected cases of esophageal perforation [9,10]. Early recognition and aggressive strategies are increasingly important. Treatment should be started as early as possible and includes intravenous fluid, stopping of oral feeding, broad-spectrum antibiotics, narcotic analgesics, total parenteral nutrition, chest tube insertion, and prompt decisions regarding surgical repair versus nonsurgical management [10,11]. Gastric perforation seldom occurs but is considered a life-threatening complication of NGT placement. Literature reported infants who survived gastric perforation were managed with laparoscopic repair [12]. In adults, although patients with small, well-defined esophageal tears and minimal pneumothorax are better managed by conservative management, However, no clear criteria can be applied in children with esophageal perforation [5,9,10].
Conclusion
Iatrogenic esophageal injury caused by NGT should be suspected if respiratory distress developed soon after tube insertion. Chest radiograph together with contrast study and oesophogoscopy help to confirm this perforation injury. Nil per mouth, total parenteral nutrition, chest tube drains, and broad-spectrum antimicrobial therapy is adequate management for iatrogenic esophageal perforation in extremely low- birth-weight infants. This further strengthens the conservative strategy as an effective treatment option for esophageal injury associated with NGT placement in extremely low-birth-weight infants. Surgical intervention may be needed if conservative management failed, or further complications developed.
References
- Mileder LP, Müller M, Reiterer F, Pilhatsch A, Gürtl-Lackner B, et al. (2016) Esophageal Perforation with Unilateral Fluidothorax Caused by Nasogastric Tube. Case Rep Pediatr 2016: 4103734.
- Thanhaeuser M, Lindtner-Kreindler C, Berger A, Haiden N (2019) Conservative Treatment of Iatrogenic Perforations Caused by Gastric Tubes in Extremely Low Birth Weight Infants. Early Hum Dev 137:
- Elgendy MM, Othman H, Aly H (2021) Esophageal Perforation in Very Low Birth Weight Eu J Pediatr 180(2): 513-518.
- Sorensen E, Yu C, Chuang SL, Midrio P, Martinez L, et al. (2023) Iatrogenic Neonatal Esophageal Perforation: A European Multicentre Review on Management and Children 10(2): 217.
- Mikołajczak A, Kufel K, Żytyńska-Daniluk J, Rutkowska M, Bokiniec R (2023) Iatrogenic Esophageal Perforation in Premature Infants: A Multicenter Retrospective Study from Poland. Children (Basel) 10(8):
- Rentea RM, Peter SDS (2017) Neonatal and Pediatric Esophageal Semin Pediatr Surg 26(2): 87-94.
- Rizzo R, Paradiso FV, Silvaroli S, Nanni L (2023) Iatrogenic Esophageal Perforation in Infant: How to avoid Thoracotomy? A Case J Neonatal Surgery 12: 18-18.
- Yong SB, Ma JS, Chen FS, Chung MY, Yang KD (2016) Nasogastric tube placement and esophageal perforation in extremely low birth weight Pediatrics & Neonatology 57(5): 427-430.
- Kato Y, Hirata K, Oshima Y, Wada K (2020) Weight-Based Estimation of Insertion Length of the Nasogastric Tube in Extremely Low Birth-Weight Advances in Neonatal Care 20(2): E31-E34.
- Brankov O, Shivachev H, Antonova D, Pahnev Y (2017) Iatrogenic Pharyngeoesophageal Perforation in the Neonatal Period–Clues for Conservative Treatment. Int J Surg Med 3(2): 107-107.
- Filippi L, Pezzati M, Poggi C (2005) Use of Polyvinyl Feeding Tubes and Iatrogenic Pharyngo‐ Oesophageal Perforation in Very‐Low‐Birthweight Acta Paediatrica 94(12): 1825-1828.
- Sakaria RP, Zaveri PG (2021) Neonatal Gastric Perforation: 14-year Experience from A Tertiary Neonatal Intensive Care Am J Perinatol 40(10): 1112-1118.






























