Rare Bulging Fissure Sign in Chest X-Ray (CXR) of a Three Years Old in Tertiary Centre In KSA: A Case Report
Hayat AlJutaily*, Khaled Bagis and Ayed Alenazi
Department of Pediatrics, Unaizah College of Medicine and Medical Sciences, Qassim University, Unaizah, Kingdom of Saudi Arabia
Submission: March 17, 2023; Published: April 21, 2023
*Corresponding author: Hayat AlJutaily, Department of Pediatrics, Unaizah College of Medicine and Medical Sciences, Qassim University, Unaizah, Kingdom of Saudi Arabia, Tel: +966553640600; Email: hayat.i.aljutaily@hotmail.com
How to cite this article:Hayat A, Khaled B, Ayed A. Rare Bulging Fissure Sign in Chest X-Ray (CXR) of a Three Years Old in Tertiary Centre In KSA: A Case Report. Acad J Ped Neonatol 2023; 12(4): 555898. 10.19080/AJPN.2023.12.555898
Abstract
Imaging plays a critical role in the diagnosis of respiratory infections. Early diagnosis of respiratory infections can aid in treatment of patients [1]. The bulging fissure sign is characteristic of Klebsiella pneumonia infection, although it could be present in pneumonia due to Streptococcus pneumoniae , P. aeruginosa , S. aureus [2]. In this report, we describe the case of a patient with necrotizing pneumonia with the bulging fissure sign; however, we were not able to culture Klebsiella pneumonia or other bacteria from sputum samples. The patient was also reported to be negative for SARS-CoV-2 infection.
Keywords: necrotizing pneumonia, bulging fissure sign, cavitation.
Abbreviations: NP: Necrotizing pneumonia; CXR: Chest X-Ray; CAP: Community-Acquired Pneumonia; CT scan: Computed Tomography scan
Introduction
Necrotizing pneumonia (NP) is a rare but severe complication of bacterial pneumonia. The disease is associated with high morbidity and mortality. NP is characterized by the loss of lung parenchyma and peripheral necrosis, resulting in multiple thin-walled small cavities. The compromised bronchial and pulmonary vascular supply impedes antibiotic delivery, resulting in uncontrolled bacterial infection [3]. The disease can develop into bronchopleural fistula, empyema, respiratory failure, and septic shock if left untreated. The most common causative agents of NP in children are Klebsiella pneumonia, Staphylococcus aureus and Streptococcus pneumoniae. Prolonged antibiotic therapy is the mainstay of treatment. However, in severe cases, surgical drainage may be a lifesaving option [4].
Case Presentation
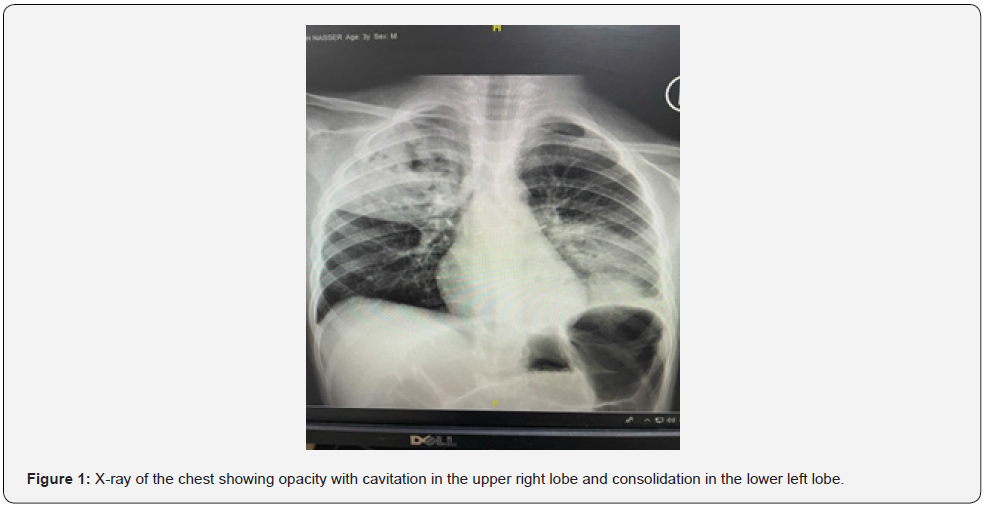
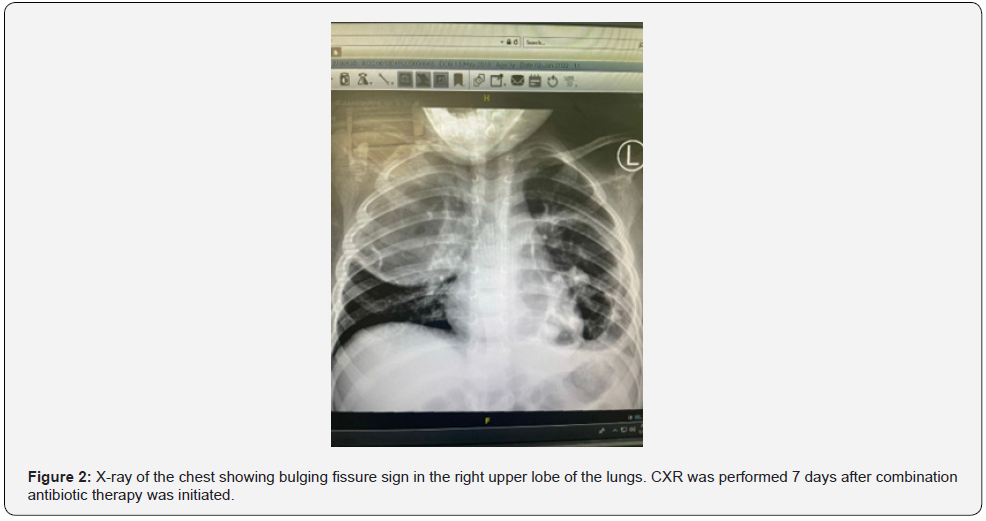
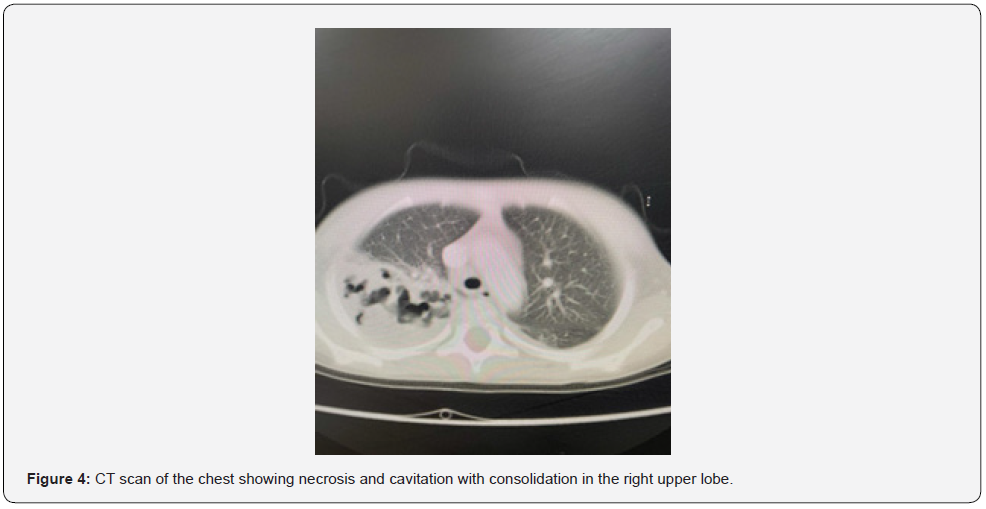
A three -year-old boy presented to the Pediatric ER department with complaints of shortness of breath and cough. The patient was diagnosed with community-acquired pneumonia, as seen in the initial CXR shown in Figure 1. The patient was treated with ceftriaxone and azithromycin. However, after five days of post treatment, the condition worsened. A computer tomography (CT) scan revealed cavitation and necrotizing pneumonia, and the patient was admitted to the intensive care unit (ICU). The antibiotic regimen was changed to intravenous piperacillin/tazobactam 100 mg/kg, and high flow nasal cannula (HFNC) therapy was initiated. After 6 days, the patient was transferred to the ward under the care of a pulmonologist. Later, while the patient was on piperacillin/tazobactam and room air developed a high-grade fever, and partial septic follow-up revealed increased leukocytosis as well as increased CRP, ferritin, and D-dimer levels. Antibiotics were changed to an intravenous combination of meropenem 20 mg/kg every 8 hours and vancomycin 22 mg/kg every 6 hours, The patient’s condition started to improve. Figure 2 shows the CXR 7 days after combination antibiotic therapy was initiated.
The basic immunological profile was within the normal range.
A Tuberculosis mycobacterium workup was performed, and the results were negative.
Interestingly sputum culture, which was performed repeatedly throughout the course of illness, was consistently negative.
The patient finished a 4-week IV course of the antibiotics meropenem and vancomycin, and no repeated chest CT was performed.
The patient was discharged home in good condition.
The results of all repeated laboratory tests were normal (Figure 1-4).
Discussion
NP is characterized by the destruction of the underlying lung parenchyma, which results in multiple small, thin-walled cavities and is often accompanied by empyema and bronchopleural fistulae [3].
Pathological investigations of lung specimens from autopsies or resections have demonstrated inflammation in the lungs and compromised alveolar capacity due to fluid accumulation. Moreover, necrosis and the presence of multiple small cavities due to intrapulmonary artery thrombosis have also been observed. The decreased blood flow thrombosed arteries lowers the antibiotic concentration inside the affected lung tissues, resulting in chronic infection [3].
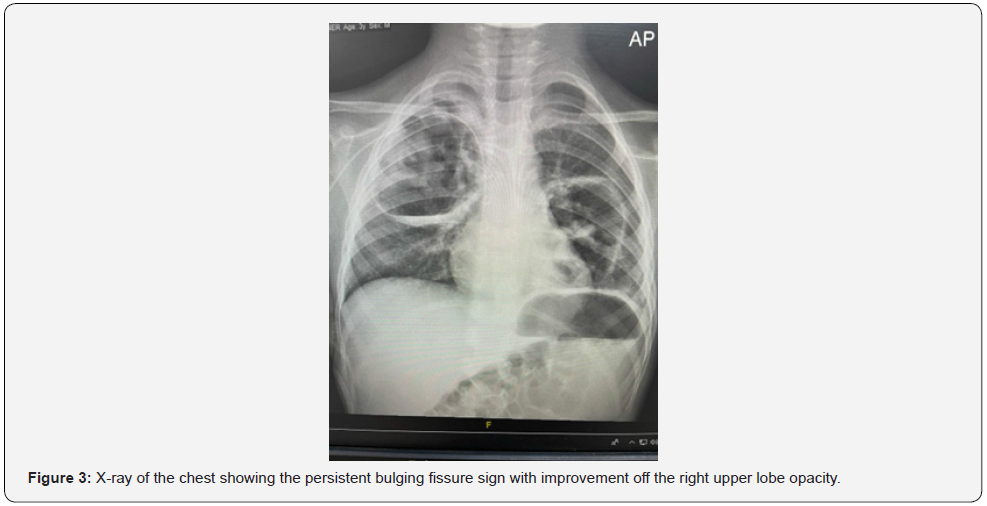
Expansile pneumonia is defined by an increased volume of the affected lobe or segment during a bout of pneumonia, which results in a densely consolidated lobe or segment with bulging fissures on radiography. Traditionally, a bulging fissure indicates Klebsiella pneumoniae infection [5][7]. In affected patients, tracheal aspirates and blood culture samples reveal the presence of gram-negative bacilli, which are positive on a string test, confirming the presence of Klebsiella pneumoniae [6][8].
Expansile pneumonia caused by Klebsiella pneumoniae frequently affects the right upper lobe. Although Klebsiella pneumoniae is still the leading causative agent of the disease cases of expansile pneumonia with Staphylococcus aureus have also been reported. Expansile pneumonia caused by Klebsiella pneumoniae frequently affects the right upper lobe [7].
In this case report, a bulging fissure sign was observed on Day 7 after combination antibiotic therapy was initiated the patient responded to meropenem and vancomycin.
Excessive lobar consolidation causes fissure swelling or displacement by inflammatory exudate inside the affected parenchyma. The bulging fissure sign can be observed in all kinds of pneumonia. However, this condition is more frequently reported in pneumococcal pneumonia. Currently, due to advancements in diagnostics and antibiotic therapies, the condition is rarely reported in clinical settings. Pulmonary hemorrhage, lung abscess and malignancy are other predisposing factors for the bulging fissure sign [1,8]. Other causes, such as echinococcus infection, can appear in CXR as a homogeneous density occupying the right upper lobe and displacing the horizontal fissure [9]. Adenocarcinoma and lymphoma should be considered in the differential diagnosis.
Conclusion
The bulging fissure sign is an uncommon radiological finding resulting from a complication of CAP and is frequently observed in the right upper lobe. Here, we report the case of a 3-year-old boy suffering from CAP with a large cystic lesion with a bulging fissure sign. Blood and sputum cultures are important to find causative organisms.
Conflict of Interest
The authors have no perceptible conflicts of interest.
Ethics Approval
Informed consent was obtained from the patient’s parents. The confidentiality of the patient’s data was obtained on all occasions.
Funding Source
No founding resource specify for this case report.
References
- Walker CM, Abbott GF, Greene RE, Shepard JA, Vummidi D, et al. (2014) Imaging pulmonary infection: classic signs and patterns. AJR Am J Roentgenol 202(3): 479-492.
- Grosso A, Famiglietti A, Luna C (2015) Community-acquired pneumonia due to gram-negative bacteria. Community Acquired Infection 2(4): 117.
- Masters IB, Isles AF, Grimwood K (2017) Necrotizing pneumonia: an emerging problem in children? Pneumonia (Nathan) 9: 11.
- Ramgopal S, Ivan Y, Medsinge A, Saladino RA (2017) Pediatric Necrotizing Pneumonia: A Case Report and Review of the Literature. Pediatr Emerg Care 33(2): 112-115.
- Yamakawa H, Yoshida M, Katagi H, Kuwano K (2014) Pulmonary Hodgkin's lymphoma presenting with a bulging fissure sign. Intern Med 53(17): 2021-2022.
- Mazloum M, Le Meur M, Barnaud G, Messika J (2016) Hypermucoviscous Klebsiella pneumoniae pneumonia: follow the string! Intensive Care Med 42(12): 2092-2093.
- Goussard P, Gie RP, Kling S, Beyers N (2004) Expansile pneumonia in children caused by Mycobacterium tuberculosis: clinical, radiological, and bronchoscopic appearances. Pediatr Pulmonol 38(6): 451-455.
- Rafat C, Fihman V, Ricard JD (2013) A 51-year-old man presenting with shock and lower-lobe consolidation with interlobar bulging fissure. Chest 143(4): 1167-1169.
- Thümler J, Muñoz A (1978) Pulmonary and hepatic echinococcosis in children. Pediatr Radiol 7: 164-171.






























