Systemic Therapeutic Alliance in the Context of Pediatric Interventions for Neurodevelopmental Disorders
John Robert C Rilveria*
Department of Psychology, University of the Philippines Diliman, National Capital Region, Philippines
Submission: August 11, 2022; Published: September 26, 2022
*Corresponding author: John Robert C Rilveria, Block 3 Lot 12 Kalikasan Hills Townhomes Barangay 171, Caloocan City, Philippines
How to cite this article:John Robert C R. Systemic Therapeutic Alliance in the Context of Pediatric Interventions for Neurodevelopmental Disorders. Acad J Ped Neonatol 2022; 12(1): 555883. 10.19080/AJPN.2022.12.555883
Abstract
Children with neurodevelopmental disorders live in a multi-system setting, with multiple providers forming the system of care. In order to reinforce the quality of childcare, strong alliances with the child as well as alliances among care providers must be established and maintained. A systemic therapeutic alliance composed of child-parent, child-caregiver, child-professional, parent-professional, caregiver-professional, and inter-professional alliances must be considered when providing interventions for children with neurodevelopmental disorders. Future research capturing the development of each of the components of the systemic therapeutic alliance can provide useful information in bolstering pediatric interventions.
Keywords: Neuro Developmental Disorders; Systemic Therapeutic Alliance; Childcare; Interventions
Abbreviations: NDD: Neuro Developmental Disorders
Introduction
Pediatric interventions for neurodevelopmental disorders (NDD) like autism spectrum disorder, attention-deficit hyperactivity disorder, intellectual disability, down syndrome, etc. are multi-faceted and multi-modal [1,2]. Children with NDD mostly require skills-based interventions [3] such as occupational therapy to address sensori-motor problems, speech-language therapy to manage speech and communication difficulties, physical therapy to rehabilitate musculoskeletal and mobility concerns, applied behavior analysis therapy to address maladaptive behaviors, and special education services to respond to academic needs. Moreover, they are seen routinely by developmental pediatricians, neurologists, and other pediatric medical specialists for medical, cognitive, nutritional, and other developmental evaluations [4].
Despite the variety of interventions available to manage NDDs, it has been proven that treatment success takes place not in the type of intervention but in the context of relationships---highlighting importance of therapeutic alliance [5,6]. Therapeutic alliance refers to the functional, collaborative relationship between a service provider and a client [7,8] composed of three elements: agreement on goals, engagement on tasks, and formation of bond [9]. However, this conceptualization of the therapeutic alliance only applies to the dyadic relationship between the therapist and the client.
In the context of pediatric interventions, the therapeutic alliance is not just confined within the child-therapist relationship but also with the child’s immediate family, particularly with the parents [10,11]. It is the decision of parents to bring their child to therapy or seek other medical services. It is also up to the parents whether to continue or terminate the interventions. In this regard, parents become significant allies in pediatric intervention [12]. In addition, the presence of a hired caregiver broadens the network of the therapeutic alliance. A competent caregiver plays an important role in the implementation of treatment recommendations at home [13]. It is usually the caregiver who spends more time with the child for assisting in daily needs and comes with the child during therapy sessions as the parents are usually at work.
Lastly, due to the multidisciplinary approach is evident in handling cases of neurodevelopmental disorders [14,15], an alliance among professional care providers (e.g., medical doctors, therapists, teachers) must be considered as well. Alliance among different professionals is fostered when they “share a common language”. Considering all agents involved in a pediatric intervention, a systemic therapeutic alliance is formed as shown in Figure 1.
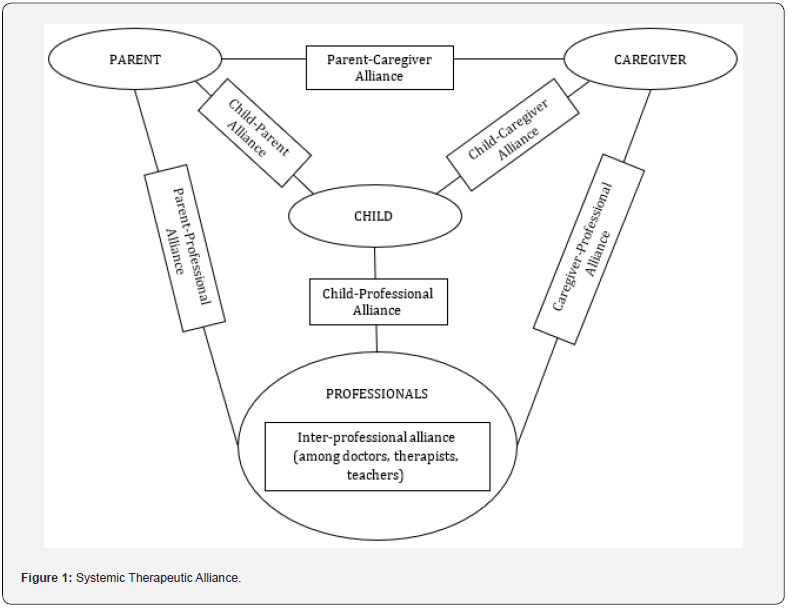
Systemic therapeutic alliance
The concept of therapeutic alliance in the context of child and family psychotherapy is substantially different from the concept of therapeutic alliance in adult and individual psychotherapy [16,17]. There are two subsystems of therapeutic alliance existing in child psychotherapy: primary and secondary systems of therapeutic alliance. The primary system of therapeutic alliance comprises of relationships involving direct contact with the child -- relationship between professional (doctor, therapist, teacher) and child, between parent and child, between caregiver and child, etc. On the other hand, the secondary therapeutic alliance, comprises of relationships that do not have a direct contact with the child but has an indirect impact on the overall treatment progress – relationship between professional and parent, between parent and another caregiver, between one professional and another, etc. [17,18]. As an integrative framework, these subsystems of therapeutic alliance form the child’s “system of care” [17].
Primary system of therapeutic alliance
Alliance between the professional and the child
In a content analysis of studies investigating the concept of therapeutic alliance involving both child and adult client relationship with a therapist, results revealed that the quality of the client–therapist alliance is a significant predictor of positive clinical outcome independent of the psychotherapeutic orientation [7,19]. Likewise, in the context of pediatric interventions for neurodevelopmental disorders, alliance between the professional and child is acknowledged as an important variable. Great childprofessional alliance is associated with decreased likelihood of escape-motivated behaviors and increased child compliance [20].
In child psychotherapy, “a familiar pattern of relating with the professional” contributes to the establishment of an alliance, giving more importance to the quality of the relationship than quantitative changes in behavior. This pattern of relating is established through a series of ongoing therapy sessions. Conversely, the professional’s own pattern of relating with the client as a result of continuing therapy sessions also improves this relationship [21]. The professional’s positive expectations in therapy also serves as a driving force maintaining the established alliance. Nevertheless, factors associated with the fact that children’s clients are usually not self-referred and frequently engage in therapy in a resistant, pre-contemplative stage are considered the major obstacles in developing a stable alliance with the professional [22,23].
Although child compliance and volume of therapy sessions are considered to be associated with child-professional alliance, there are also potential mediators that influence the said relationship. There are evidence that more experienced professionals would have more skills in developing a solid alliance with their clients than less experienced ones [24]. This is due to acquired skills and techniques in effectively establishing rapport. Furthermore, the severity of the child’s condition could also play a vital role in the association between compliance and establishment of an alliance [25].
Alliance between the parent and the child
The quality of parent-child relationship becomes therapeutic if it contributes to the improvement of the child. Parental acceptance or rejection is a critical factor in developing a therapeutic alliance between the parent and child [26,27]. When parents come to terms with and accept their child’s condition, a positive relationship with the child is formed. Several research studies have revealed that a positive relationship between parents and their children with autism significantly predicts the child’s development [28,29].
Although parents generally report positive relationship with their children, elevated stress levels were also observed in some parents. Higher stress levels are associated with difficulty forming a positive relationship with the child. Narratives of parents revealed that a major stressor is the severity of their child’s condition [30] characterized by challenges in communicating, problem behaviors, social isolation, difficulties in self-care, and lack of community understanding [31].
Alliance between the caregiver and the child
Shirk & Saiz [32] has theorized that an alliance between the caregiver and the child is reflected on degrees of compliance and levels of positive performance (when the child starts to follow simple commands, be able to listen to his/her caregiver, and is less likely to exhibit problem behaviors). However, for the caregivers, there are actually innate concerns and worries that are translated into high levels of stress regarding the possibility of the child to live a normal social life such as opportunities in education, marriage, employment, etc. [13,33]. Caregivers of children with NDD have difficulty coping primarily due to the severity of the child’s condition [34]. Children with NDD that have severe impairments in cognitive, behavioral and language domains are the most difficult to handle compared to those with minimal impairments.
This adds to the high level of caregiving stress and affect the way caregivers relate with children with ASD [34].
Secondary System of Therapeutic Alliance
Alliance between the professional and the child’s parents
In child psychotherapy, the child is not just the client, but also the child’s parents [11,35]. Children with NDD are brought to therapy mostly based on the decision of the parents. It has been found out that a positive relationship between parents of children and the children’s therapist(s) contributes to increased parental compliance, and decreased stress levels of the parents based on qualitative studies done by Hoagwood [36] and Thompson et al. [37] and quantitative studies done by Myers [38] and Krakovich et al. [39]. There are also studies suggesting that the parentprofessional alliance begins to develop after a few sessions when they regularly discuss a program that can be implemented at home through feedback sessions [28].
Parental compliance and frequency of feedback sessions are mostly the associated factors in parent-professional alliance. However, there are also potential mediators. When parents perceive the professional as a competent service provider for their child, and begin noticing improvements on their child, then they would start complying with the therapist’s recommendations – leading to stronger alliance [26,40,41]. However, parents who felt “disrespected” by their children’s mental health providers (e.g., feedbacks that imply inappropriate parenting, thus being offended) are more likely to lose trust and no longer comply with future treatment, thus hampering the development of an alliance [42].
Alliance between the professional and the child’s caregiver
Most of the time, parents of children with special needs hire or seek for services of a caregiver to take care of their children when they are away from work. In this kind of set-up, the professional is expected to form an alliance with the caregiver as well. According to a qualitative study done by Hawks (2015), the caregiver is given an active role in the therapeutic process. Constant communication and collaboration between the professional and the child’s caregiver can help in improving the child’s condition. The caregiver is responsible for getting the child to therapy, modify the family environment according to therapy recommendations. When caregivers follow instructions given by the therapist in terms of how to implement activities at home, then their relationship becomes stronger [43]. The caregiver-professional alliance is also enhanced when there are regular feedback sessions carried out by the professional and regular update about the child’s behavior at home reported by the caregiver.
However, when caregivers do not comply with the professional’s recommendations, the whole therapeutic milieu becomes inconsistent. Because of this, opportunities for future collaboration and the progress of treatment for the child may be compromised [43]. Compliance and non-compliance with professional’s recommendations may be attributed to perceived improvements on the child. When caregivers see progress in therapy, then they are more likely to trust the child’s therapist, doctor, or teacher and comply with the intervention program [40].
Alliance among professionals
Using a multidisciplinary approach is evident in handling cases of neurodevelopmental disorders [14,44]. This is due to the fact that NDDs often present with a range of needs that span multiple providers and service systems. In this kind of set-up, an interprofessional collaborative alliance is necessary [45]. Interprofessional collaboration involves an alliance among professionals who work together toward a unitary goal of providing high quality client care. Specific to managing children with special needs, these professionals include behavior therapists, occupational therapists, recreational therapists, speech therapists, psychiatrists, pediatricians, psychologists, schoolteachers, and social workers [45,46].
At the very least, all professionals catering to a single child with NDD must be open to differing opinions in the etiology and management of autism and must be able to practice shared decision-making in setting treatment goals. However, openness to contradicting approaches are difficult to establish. Incompatible views make it difficult to share a common language and alliance is compromised. To resolve this issue, it has been suggested that all professionals involved in childcare must adopt a sharable criterion that is based on up-to-date and evidence-based research on autism [47,48]. One good example is the constant exchange of information among professionals (e.g., consensus meetings or team conferences). Moreover, the use of structured instruments like a session notebook where professionals can take note of observed behaviors, level of progress achieved, etc. during their own corresponding sessions facilitate good communication among therapists involved.
Professionals who agree in interprofessional collaborative care in autism management are more willing to work with other professionals and attend consensus meetings while those who remain bounded to their own approaches to NDD have difficulty collaborating with other professionals [47]. Alliance between the Parent and the Caregiver. When parents of a child with NDD are away from work or cannot provide ample time in taking care of their child, caregivers at home have the primary responsibility for the child - in terms of basic needs, welfare, and security. The caregiver may be an immediate or extended family member, a non-relative or romantic partner, or a family friend [49]. Usually, for cases of children with NDD, parents hire caregiver or set of caregivers who can take care of the child full-time. Hiring a caregiver is a struggle for most parents especially that they must place their full trust on the caregiver’s capability to handle their child.
The alliance between a parent and the child’s caregiver is characterized by mutual child investment, negotiation of respective roles, responsibilities, and contributions, valuing of each other’s involvement and judgment regarding children, and positive communication patterns regarding children [50]. Parents can form an alliance with their child’s caregiver if they have already observed a bond between their child and the caregiver characterized by increased compliance of the child [50]. However, the amount of psychosocial burden, physical and mental stress of the caregiver weaken the relationship between the two [51]. So, in order to overcome this challenge, the family, especially the parents are expected to help caregivers adjust their expectations of their children [52]. Nonetheless, despite the amount of stress on the part of the child’s caregiver, he/she is more likely to form an alliance with the parent when the parenting style is perceived to be appropriate [51].
Conclusion
It is very important to acknowledge the systemic therapeutic alliance because children with NDDs are surrounded by multiple therapeutic agents (parents, caregivers, and professionals) that do not only interact with them but also interact with one another [16,53]. Furthermore, research studies have shown that positive therapeutic outcomes are not just mediated by the quality of relationship between the child and the care provider, but also by the quality of relationship among the care providers themselves [15,28]. With regular therapy sessions with the child, consistent meetings with professional care providers, and coordination between the child’s parents and caregivers, a healthy alliance among the members of treatment team is nurtured. When a healthy alliance is established, it can be argued that the implementation of the treatment plan will be efficient, and the treatment progress will be ensured.
References
- Hadders-Algra M (2021) Early Diagnostics and Early Intervention in Neurodevelopmental Disorders-Age-Dependent Challenges and Opportunities. J Clin Med 10(4): 861.
- Palermo TM (2014) Evidence-based interventions in pediatric psychology: progress over the decades. J Pediatr Psychol 39(8): 753-762.
- Hyman SL Levy SE, Myers SM (2020) Identification, Evaluation, and Management of Children With Autism Spectrum Disorder. Pediatrics 145(1): e20193447.
- Wetmore DZ, Garner CC (2010) Emerging pharmacotherapies for neurodevelopmental disorders. J Dev Behav Pediatr 31(7): 564-581.
- Tschuschke V, Koemeda-Lutz M, von Wyl A, Crameri A (2020) The impact of patients' and therapists' views of the therapeutic alliance on treatment outcome in psychotherapy. J Nerv Ment Dis 208(1): 56-64.
- Welmers-van de Poll MJ, Roest JJ, van der Stouwe T, van den Akker AL, Stams G, et al. (2018) Alliance and Treatment Outcome in Family-Involved Treatment for Youth Problems: A Three-Level Meta-analysis. Clin Child Fam Psychol Rev 21(2): 146-170.
- Ardito RB, Rabellino D (2011) Therapeutic Alliance and Outcome of Psychotherapy: Historical Excursus. Measurements and Prospects for Research. Front Psychol 2: 270.
- Gelso CJ, Kline KV (2019) The sister concepts of the working alliance and the real relationship: on their development, rupture, and repair. Res Psychother 22(2) 373.
- Bordin E (1979) The generalizability of the psychoanalytic concept of the working alliance. Psychotherapy: Theory, Research and Practice 16(3): 252-260.
- Nuñez L, Fernández S, Alamo N, Midgley N, Capella C, et al (2022) The therapeutic relationship and change processes in child psychotherapy: a qualitative, longitudinal study of the views of children, parents and therapists. Res Psychother 25(1): 556.
- Rodriguez N (2011) The Parent-Therapist Alliance in the Psychological Treatment of Children. (Doctoral dissertation). University College London.
- Weersing RV, Weisz JR (2002) Mechanisms of action in youth psychotherapy. J Child Psychol Psychiatry 43(1): 3-29.
- Kheir NM, Sandridg AL, Hayder SA, Al-Ismail MS, Al-Rawi F (2012) Concerns and considerations among caregivers of a child with autism in Qatar. BMC Res Notes 5:290.
- Alderson J (2009) Moving toward a multi-treatment approach to autism: The whole is greater than the sum of the parts. The Autism File 30.
- Beaudry-Bellefeuille I, Pomoni M, Welch A, Moriyón-Iglesias T, Suárez-González M, et al. (2021) Multidisciplinary approach to assessment and intervention of feeding problems in children with autism spectrum disorders: a clinical perspective. Irish Journal of Occupational Therapy 49(2): 77-83.
- Escudero V (2016) Guest editorial: the therapeutic alliance from a systemic perspective. Journal of Family Therapy 38(1): 1-4.
- Karam EA, Ko M, Pinsof B, Mroczek D, Sprenkle D (2015) The Multisystemic and Multilevel Investigation of the Expanded Therapeutic Alliance-Psychological Functioning Relationship in Individual Therapy. J Marital Fam Ther 41(4): 401-414.
- Feinstein NR, Fielding K, Udvari-Solner A, Joshi SV (2009) The Supporting Alliance in Child and Adolescent Treatment:Enhancing Collaboration among Therapists, Parents, and Teachers. Am J Psychother 63(4): 319.
- Klebanoff SM, Rosenau KA, Wood JJ (2019) The therapeutic alliance in cognitive-behavioral therapy for school-aged children with autism and clinical anxiety. Autism 23(8): 2031-2042.
- McLaughlin DM, Carr EG (2005) Quality of rapport as a setting event for problem behavior. Journal of Positive Behavior Interventions 7(2): 68-91.
- Arnd-Caddigan M (2012) The Therapeutic Alliance: Implications for Therapeutic Process and Therapeutic Goals. Journal of Contemporary Psychotherapy 42(2): 77-85.
- Diguiseppe R, Linsicott J, Jilton R (1996) Developing the therapeutic alliance in child adolescent psychotherapy. Applied and Preventive Psychology 5(2): 85-100.
- Gopalan G, Goldstein L, Klingenstein K, Sicher C, Blake C, et al. (2010) Engaging families into child mental health treatment: updates and special considerations. J Can Acad Child Adolesc Psychiatry 19(3): 182-196.
- Mallinckrodt B, Nelson M L (1991) Counselor training level and the formation of the psychotherapeutic working alliance. Journal of Counseling Psychology 38(2): 133-138.
- Vivanti G, Prior M, Williams K, Dissanayake C (2014) Predictors of outcomes in autism early intervention: why don’t we know more? Front Pediatr 2: 58.
- DeVet KA, Kim YJ, Charlot-Swilley D, Ireys HT (2003) The Therapeutic Relationship in Child Therapy: Perspectives of Children and Mothers. J Clin Child Adolesc Psychol 32(2): 277-283.
- McCauley JB, Solomon M (2022) Characterizing Parent–Child Interactions in Families of Autistic Children in Late Childhood. Soc. Sci. 2022 11(3): 100.
- Kazdin AE, Whitley M, Marciano PL (2006) Child–therapist and parent–therapist alliance and therapeutic change in the treatment of children referred for oppositional, aggressive, and antisocial behavior. J Child Psychol Psychiatry 47(5): 436-445.
- Ma PS (2012) Children with autism in taiwan and the United States: Parental stress, parent child relationships, and the reliability of a child development inventory (Doctoral dissertation). Retrieved from ProQuest Dissertations and Theses database (Order No. 3533591).
- Sullivan JM (2011) Parents of children with high-functioning autism: Experiences in child parent relationship therapy (CPRT) (Doctoral dissertation). Retrieved from Proquest Dissertations and Theses database. (Order No. 3529258).
- Shieve LA, Blumberg SJ, Rice C, Visser SN, Boyle C (2007) The Relationship Between Autism and Parenting Stress. Pediatrics 119 (Suppl 1): S114-S121.
- Shirk SR ,Saiz CC, (1992) Clinical, empirical, and developmental perspectives on the therapeutic relationship in child psychotherapy. Development and Psychopathology 4(4):713-728.
- Tathgur MK, Kang HK (2021) Challenges of the Caregivers in Managing a Child with Autism Spectrum Disorder- A Qualitative Analysis. Indian J Psychol Med 43(5): 416-421.
- Lai WW, Oei TPS (2014) Coping in Parents and Caregivers of Children with Autism Spectrum Disorders (ASD): a Review. Review Journal of Autism and Developmental Disorders 1(3): 207-224.
- Perkins SN, Glass VQ, D’Aniello C (2019) It’s all about the balance: therapists’ experience of systemic alliance development. Contemporary Family Therapy 41: 420-434.
- Hoagwood KE (2005) Family-based services in children’s mental health: A research review and synthesis. J Child Psychol Psychiatry 46(7): 670-713.
- Thompson SJ, Bender K, Lantry J, Flynn PM (2007) Treatment Engagement: Building Therapeutic Alliance in Home-Based Treatment with Adolescents and their Families. Contemp Fam Ther 29(1-2): 39–55.
- Myers SJ (2008) Relationship between the consultant-parent working alliance and ratings of the consultation process with parents of children having autism spectrum disorder. Dissertation Abstracts International: Section A. Humanities and Social Sciences 69(6): 2222.
- Krakovich T, McGrew J, Yu Y, Ruble L (2016) Stress in Parents of Children with Autism Spectrum Disorder: An Exploration of Demands and Resources. J Autism Dev Disord 46(6): 2042-2053.
- Accurso E, Garland A (2015) Child, caregiver, and therapist perspectives on therapeutic alliance in usual care child psychotherapy. Psychol Assess 27(1): 347-352.
- Kalyva E (2013) Collaboration Between Parents of Children with Autism Spectrum Disorders and Mental Health Professionals. Recent Advances in Autism Spectrum Disorders 1.
- Kerkorian D, McKay M, Bannon WM (2006) Seeking help a second time: Parents'/caregivers' characterizations of previous experiences with mental health services for their children and perceptions of barriers to future use. Am J Orthopsychiatry 76(2): 161-166.
- Shirk SR, Karver M (2003) Prediction of treatment outcome from relationship variables in child and adolescent therapy: A meta-analytic review. J Consult Clin Psychol 71(3): 452-464.
- Dillenburger K, Röttgers HR, Dounavi K, Sparkman CR, Keenan M, et al. (2014) Multidisciplinary Teamwork in Autism: Can One Size Fit All? The Australian Educational and Developmental Psychologist, 31:2, 97-112, DOI: 10.1017/edp.2014.13.
- Summers J, Bartha C, Desarkar P, Duggan L, Fineczko J, et al. (2016) Inter-Professional Collaborative Care: A Way to Enhance Services for Adults with Intellectual Disability and/or autism spectrum disorder and Mental Health Problems. Journal of Intellectual Disability 4: 17-24.
- D’Amour D, Ferrada-Videla M, San Martin Rodriguez L, Beaulieu M (2005) The conceptual basis for interprofessional collaboration: Core concepts and theoretical frameworks. J Interprof Care 19(Suppl 1): 116-131.
- Raffin C (2001) A multidisciplinary approach to working with autistic children. Educational and Child Psychology 18(2).
- Tsilimingras D, Gibson ScipioW, ClancyK, Hudson L, Liu X, et al (2018) Interprofessional education during an autism session. J Commun Disord 76: 71-78.
- Loper AB, Philipps B, Nichols EB, Dallaire DH (2013) Characteristics and Effects of the Co-parenting Alliance between Incarcerated Parents and Child Caregivers. Journal of Child & Family Studies 23: 225-241.
- Drugli MB, Undheim AM (2012) Partnership between Parents and Caregivers of Young Children in Full-time Daycare. Child Care in Practice 18(1) doi.org/10.1080/13575279.2011.621887.
- Rabideau A (2017) Caregiver descriptions of services received for children with autism and the impact on family life: A case study. (Doctoral dissertation). Retrieved from ProQuest Dissertations and Theses database (Order No. 10259457).
- Al-Dujaili A, Al-Mossawy D (2017) Psychosocial burden among caregivers of children with autism spectrum disorder in Najaf province. Current Pediatrics Research 21(2): 272-282.
- Pinsof WM (1994) An integrative systems perspective on the therapeutic alliance: Theoretical, clinical and research implications. In: A Horvath and L Greenberg (Eds.), The working alliance: Theory, research and practice, John Wiley & Sons, Pp. 173-195.






























