Prevalence of Child-Adolescent Chronic Pathologies in Cantabria (Spain)
Carlos Fernández-Viadero1,2*, Iñaki Lapuente-Heppe3, Abraham Delgado-Diego3, Verónica García-Cernuda3, Silvia Somonte-Segares3,4, Rosario Verduga-Vélezs5 and Dámaso Crespo-Santiago6
1Psychiatry Service. University Hospital Marqués de Valdecilla. Ave. Valdecilla, 25, 39008. Santander, Cantabria. Spain
2IDIVAL (Research Institute Valdecilla). Ave. Cardenal Herrera Oria, s/n. 39011 Santander, Cantabria. Spain.
3Department of Care and Chronic Diseases. Cantabria Health Service. Ave. Herrera Oria, s/n. 39011 Santander, Cantabria. Spain
4Psychiatry Service. Regional Hospital Sierrallana. Ganzo, s/n, 39300 Torrelavega, Cantabria. Spain.
5ICASS (Social Service Institute of Cantabria). Government of Cantabria. General Dávila Street, 87, 39006 Santander, Cantabria. Spain
6Department of Anatomy and Cell Biology. Faculty of Medicine. University of Cantabria. Ave. Cardenal Herrera Oria, 2. 39011 Santander, Cantabria. Spain
Submission: May 12, 2022; Published: July 25, 2022
*Corresponding author:Carlos Fernández-Viadero, Psychiatric Long-Term Care Unit. Psychiatry Service. University Hospital Marqués de Valdecilla, Liencres. Piélagos, 39120. Cantabria. Spain, Tel: +34 619571252 +34 942202520, office number: 76139
How to cite this article:ACarlos F-V, Iñaki L-H, Abraham D-D, Verónica G-C, Silvia S-S, et al. Prevalence of Child-Adolescent Chronic Pathologies in Cantabria (Spain) Acad J Ped Neonatol 2022; 12(1): 555881. 10.19080/AJPN.2022.12.555881
Abstract
Objective: The study of child-adolescent chronic pathologies (CACPs) is a relevant aspect for public health and this knowledge is necessary for prevention and control. Our objective was to analyze the prevalence and distribution of the main CACPs in the region of Cantabria (Spain).
Methodology: The stratified data were obtained from the whole child and adolescent population treated by the Cantabria Health Service in the year 2019. The prevalence of the most frequent CACPs and their differences based on sex, urban non-urban location and levels of complexity and risk were assessed. The statistical analysis was performed with the SPSS program.
Results: 90,163 people aged from birth to 17-year-olds were analyzed (48.7% girls and 51.3% boys). At least one CACP was present in 29.1% of the population studied (26,234). CACPs were less prevalent in girls (25.5%) than in boys (32.6%), (χ2, p <0.001; OR: 0.708; IC 95%: 0.688-0.729). The two most common CACPs were: asthma (16.7%) and attention deficit hyperactivity disorder (6.3%). Multimorbidity occurred in 1,978 girls (4.5%) and in 2,916 boys (6.3%). Those chronic pathologies were less prevalent in urban areas (26.5%) than in non-urban areas (28.0%), (χ2, p <0.001; OR: 1.037; 95% CI: 1.023-1.052). CACPs level of complexity was slightly higher in girls and in non-urban locations. The level of risk was similar when sex and location where compared.
Conclusion: CACPs were very common in the age group studied. Our data indicate that not only is there a need for a greater number of descriptive studies, but also a greater accuracy on the clinical records of CACPs. These actions would allow the implementation of effective programs for prevention and early detection of CACPs and better treatment and control, once they are diagnosed.
Keywords: Childhood, chronic diseases, prevalence, urban, non-urban, adjusted morbidity groups
Abbreviations: ADHD: Attention deficit hyperactive disorder; AMG: Adjusted Morbidity Groups; CAAG: child-adolescent age group; CACPs: Child-Adolescent Chronic Pathologies; SCS: Cantabria Health Service
Introduction
Chronic diseases and multi-morbidity are, generally, associated with adults and elderly people [1]. However, chronic pathologies that occur in paediatric and adolescent ages are a relevant public health aspect since the report titled “Chronic childhood illness:assessment of outcome” was published almost fifty years ago [2]. Furthermore, there was described, throughout the last decades an increase in the prevalence of paediatric chronic diseases, both occurring as a single entity or associated to other illnesses [3- 5]. The exact number and degree of incidence of chronic diseases in childhood is being discussed, due to several intervening factors such as: the different types of approaches used to define chronicity and multimorbidity, diseases’ timespan, home-care interventions, hospital incomes and even social aspects [6,7]. Moreover, the increase on the number of chronic diseases throughout infancy and childhood could be influenced by the diagnostic improvement and the introduction of specific medical records for these chronic diseases, such as asthma, obesity, high blood pressure, hyperlipidaemia, to name few [5,8]. Other factors that could be responsible for the increase of the number of chronic diseases are the improvement of the quality and quantity of medical treatments that result in survival increase [9] together with an increase in early diagnosis of several neurodevelopmental and behavioural alterations [10,11]. Between 5-10% of the childhood affected population present multimorbidity because they suffer concomitantly several of these conditions [12]. As it has been suggested, all these considerations explain some of the difficulties that epidemiologic studies must confront when dealing with childhood diseases making it quite difficult to compare the results obtained in different studies [13,14]. The method employed for chronic disease assessment and recording has been reported as a reason of the great variability on the prevalence of these illnesses. Consequently, a wide range of incidences, that varies between 5-25 %, had been published [5,8,10,15-17]. An important issue that must be present when talking about CACPs is the fact that 0.67% of them are present in new-born babies [18].
When dealing with CACPs it is important to bear in mind, apart from the health problems, the fact that they may cause associated drawback effects on the academic outcomes of the patients and the quality of life for both children and the other family members [19-21]. These factors determine that up to 7.5% of the childteenager population reported non-solved health necessities [5]. Moreover, they are prone to attend health facilities both: primary health care services and specialised hospital units [22,23]. Thus, this demand represents an increase in health care costs [24] and due to CACPs persistence along the coming years of the affected people they may increase the need of further health assistance in adulthood and the rest of the patient´s life cycle [25].
In Europe there are several health programs aimed at the prevention and control of chronic diseases along the vital cycle [26-28], and some of them are especially oriented to the childadolescent age stages, such as the TIChroN project [29], whose main goal is to improve several educational aspects to prevent and control CACPs. A better knowledge of the epidemiological situation state may improve specific health programs for the child-adolescent group of age [24,30]. Taking into consideration those reasons, it is necessary to approach these studies through stratification tools such as the Kaiser Permanent pyramid model [31,32] or the King´s Fund [33]. These models have had a great influence when planning governmental welfare strategies to deal with chronicity [34]. Moreover, upon morbidity stage they allow attention planification and the identification of patients in a greater risk, thus, it will make it easier exert more specific and proactive interventions on these patients [14].
In Spain several morbidity classification systems have been employed, among them Clinical Risk Group [35] and Adjusted Clinical Groups [36]. In recent years health authorities are encouraging the use of Adjusted Morbidity Groups (AMGs) as the system for the population stratification suffering from chronic diseases [37]. Several studies have been published about AMG´s usefulness in relation to the stratification of chronic patients according to complexity and risk levels [38-40]. The number of publications relating AMGs, and child-adolescent people is not abounding because people suffering from CACPs are quite different from that of the adult population both in morbidity´s aetiology and health resources use [41,42].
The main goal of our study was to analyse gender, frequency, prevalence, and geographical distribution of some of the most frequent CACP´s in the entire under eighteen years of age population of Cantabria (Spain). To get this goal the data from the SCS´s were analysed and special attention was focused to comorbidity and risk level according to AMGs [37,42].
Methods
A cross-sectional descriptive observational study of the entire population under 18 years of age in Cantabria, attended by the SCS, has been carried out. As of December 31st, 2019, Cantabria had a population of 576,710 people attended by the public health system, with an average age of 45.6 years, (297,171 women -51.52%- and 279,539 men -48.48%). Of these, 90,163 people (15.63%), is the child-adolescent age group (CAAG).
Disease data, anonymized, were obtained from coded morbidity registers of clinical records stored in the minimum data sets of hospitals databases, and from the Primary Care clinical databases. These data were grouped according to the International Classification of Diseases (ICD-9-CM and ICD-10), and the International Classification of Primary Care (CIAP-1 and CIAP-2), following the National Strategy for Chronic Diseases into the AMGs. This grouping was obtained through the electronic medical records of the SCS as a source of information. Any childadolescent person, who presents at least one of the diseases described in Annex 1 was considered a chronic patient.
This morbidity grouper, AMG, is a population classification complexity case-mix tool that allows patients to be grouped into mutually exclusive categories, according to their multimorbidity, complexity, and risk level.
Complexity is the variable resulting from assessing aspects such as hospital admissions, mortality, visits to primary care and pharmacy spending for each diagnostic code. Assigning a value to complexity, complexity index, allows the population to be stratified in five grades, (which are obtained by identifying the 40, 70, 85 and 95 percentiles of the qualitative-quantitative models obtained from a previous study in the Spanish population [37] and following the Kaiser Permanent pyramid model. According to this individual value of complexity, each patient is assigned to one of four risk levels (high, medium, low and population without risk or relevant chronic disease). Additionally, this procedure offers for each patient a summary label of the occurring diseases.
The variables analysed were age, gender, and place of residence: urban areas of big cities (Santander and Torrelavega with a total of 44,875 CAAG), and the rest, 45,288 CAAG, that live in non-urban areas. Furthermore, we analysed risk levels and complexity according to AMG procedures, number, and type of chronic diseases and, finally multimorbidity (equal or more than two chronic diseases).
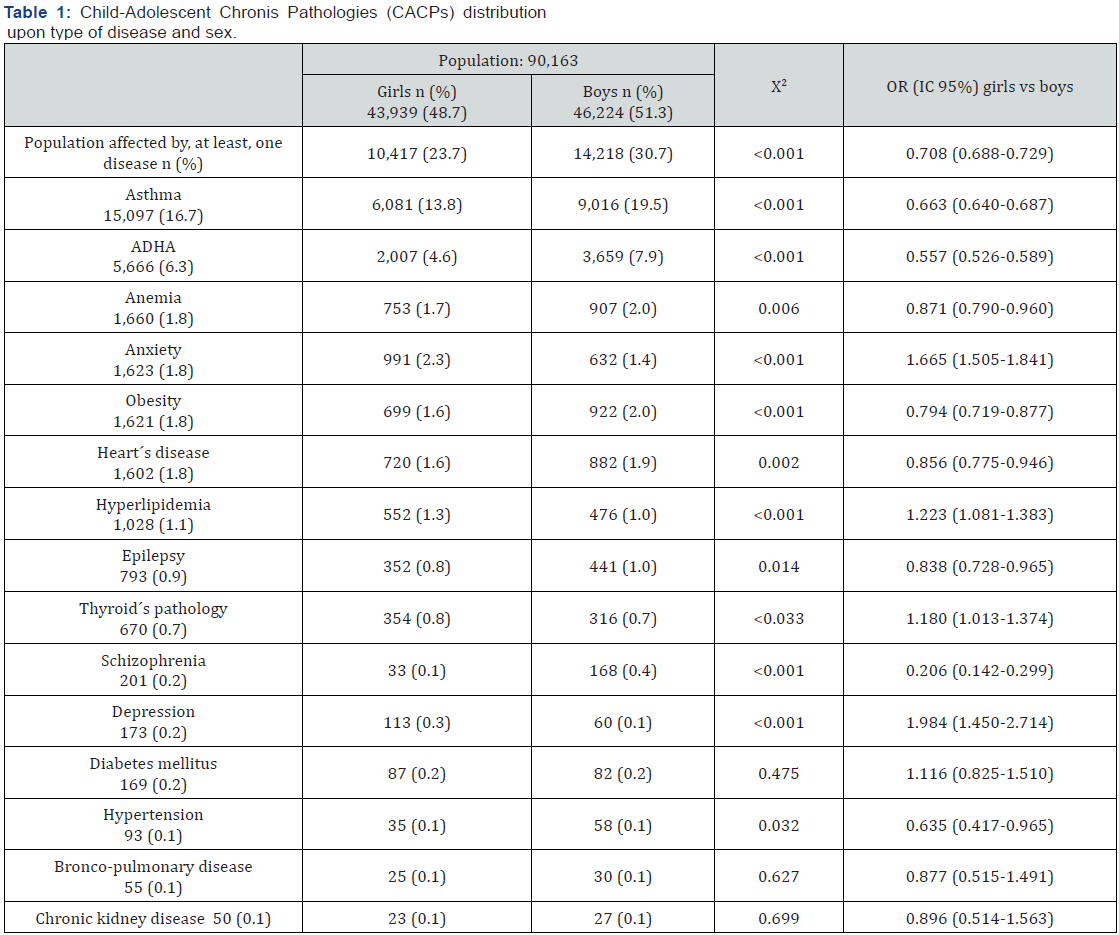
In the table 1 the CACPs analysed in our study are represented. They were arranged into two groups; one group included those that had a prevalence equal or superior to 1%, and a second group that consisted of those chronic pathologies that had a frequency lower than 1%. For this study neoplastic processes or acute illness were not included.
To facilitate the bivariant analysis the five groups of complexity were grouped into two: the high complexity group which included the very complex and complex groups and a second group of low complexity that included those of medium, low and without any complexity groups. Similarly, the risk groups were unified into two: high risk group, which comprises very high- and high-risk groups and, a low-risk group that included the rest.
Statistical analysis
The process of data´s analysis was carried out using the IBM SPSS Statistics version 25 (University of Cantabria´s licence). The level of significance was a p<0.05. Age was defined as a continuous variable and therefore represented as the mean value ± the standard deviation. The nonparametric Kolmogorov-Smirnov test was employed to assess the null hypothesis (H0) of a normal distribution of age in our population (mean 9.0 ± 4.98 years, p<0.01). Furthermore, a Mann-Whitney U test was employed to compare age in the different groups. Categorical variables were described through the frequencies’ distribution. Descriptive and comparative analysis were completed after their stratification upon sex and habitat through the Chi-squared distribution for independent samples or Fisher´s exact test when it was appropriate. The girls-boys and urban vs non-urban Odds Ratio (OR) were estimated upon the different CACPs analysed and their complexity and risk.
Ethical aspects
The use of the data from the Chronicity Strategy Stratification of Cantabria, for this and other studies, was reviewed and approved by the Clinical Trials and Medical Research Committee (CEIm) of Cantabria. Those data were anonymized prior to the study, ensuring confidentiality in accordance with current legislation and laws. Since these studies are restricted to the analysis of secondary data from population-based and anonymized files, the CEIm did not consider the need to have the consent requirement signed by each person included in these studies. (Evaluation code 2020.334. Resolution 24/2020).
Results
Data from 90,163 children and adolescents between 0 and 17 years of age (43,939 girls, 48.7% and 46,224 boys, 51.3%) were analyzed. 26,234 people in this child and adolescent population had at least one chronic pathology, which represents a prevalence of 29.1%. There were no differences in age by gender: girls 9.08 ± 4.98 years and boys 9.07 ± 4.97 years (p = 0.822). The most prevalent chronic pathology at this age was asthma (16.7%), followed by attention deficit hyperactive disorder (ADHD) (6.3%). The prevalence of anemia, anxiety, obesity, heart disease, and hyperlipidemia ranges from 1.1 to 1.8%. With prevalence figures below 1% are: epilepsy, thyroid disease, schizophrenia, depression, diabetes mellitus, high blood pressure, bronchopulmonary diseases, and chronic kidney diseases (Table 1). In our population, chronicity was less prevalent in girls (n= 11,188, 25.5%) than in boys (n= 15,046, 32.6%) (χ2, p < 0.001 and OR for girls in relation to boys of 0.708; 95% CI: 0.688-0.729).
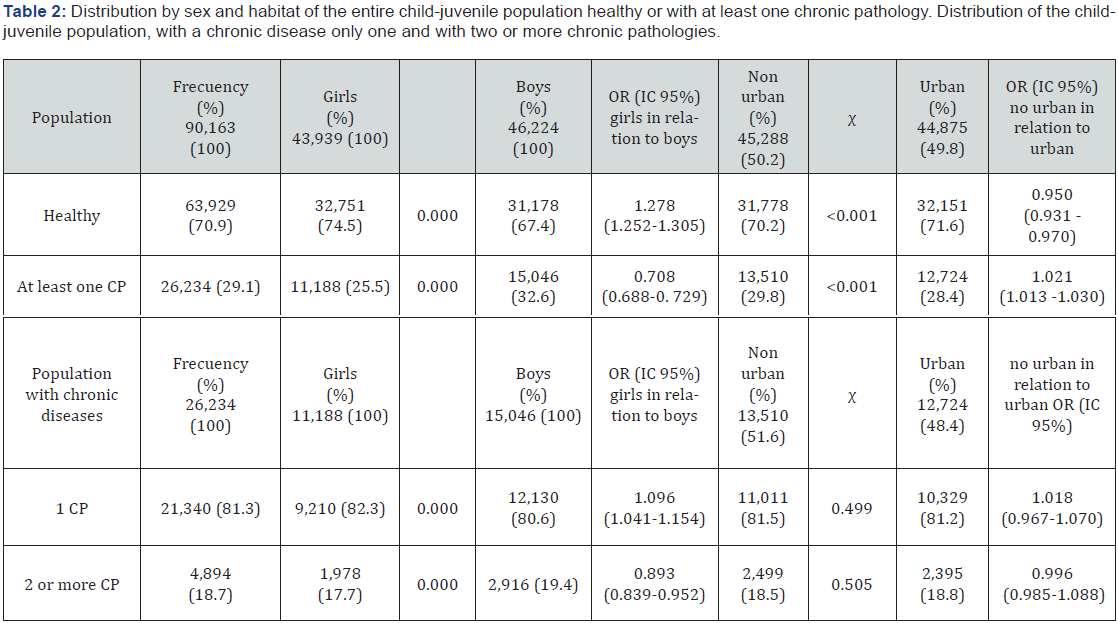
Multimorbidity, two or more chronic pathologies, affected 1,978 girls (4.5%), and 2,916 boys (6.3%), (χ2, p < 0.001 and OR for girls in relation to boys of 0.893; CI 95%: 0.859 -0.952) (Table 2). Regarding the presence or not of chronic pathologies, if these were unique or this population presents multimorbidity, with two or more chronic pathologies, girls and the urban population were healthier and had a lower burden of chronicity than boys and the non-urban population (Table 2)
In the group of most prevalent chronic pathologies, girls had a higher frequency of anxiety and hyperlipidemia, and boys had more asthma, ADHD, anaemia, obesity, and heart disease. In the group of less prevalent chronic diseases, thyroid disease and depression were more frequent among girls and epilepsy, schizophrenia, and hypertension among boys. The risk of girls compared to boys presents the highest values in depression (OR: 1.984; 95% CI: 1.450-2.714) and the lowest in schizophrenia (OR: 0.206; 95% CI: 0.142-0.299), (Table 1).
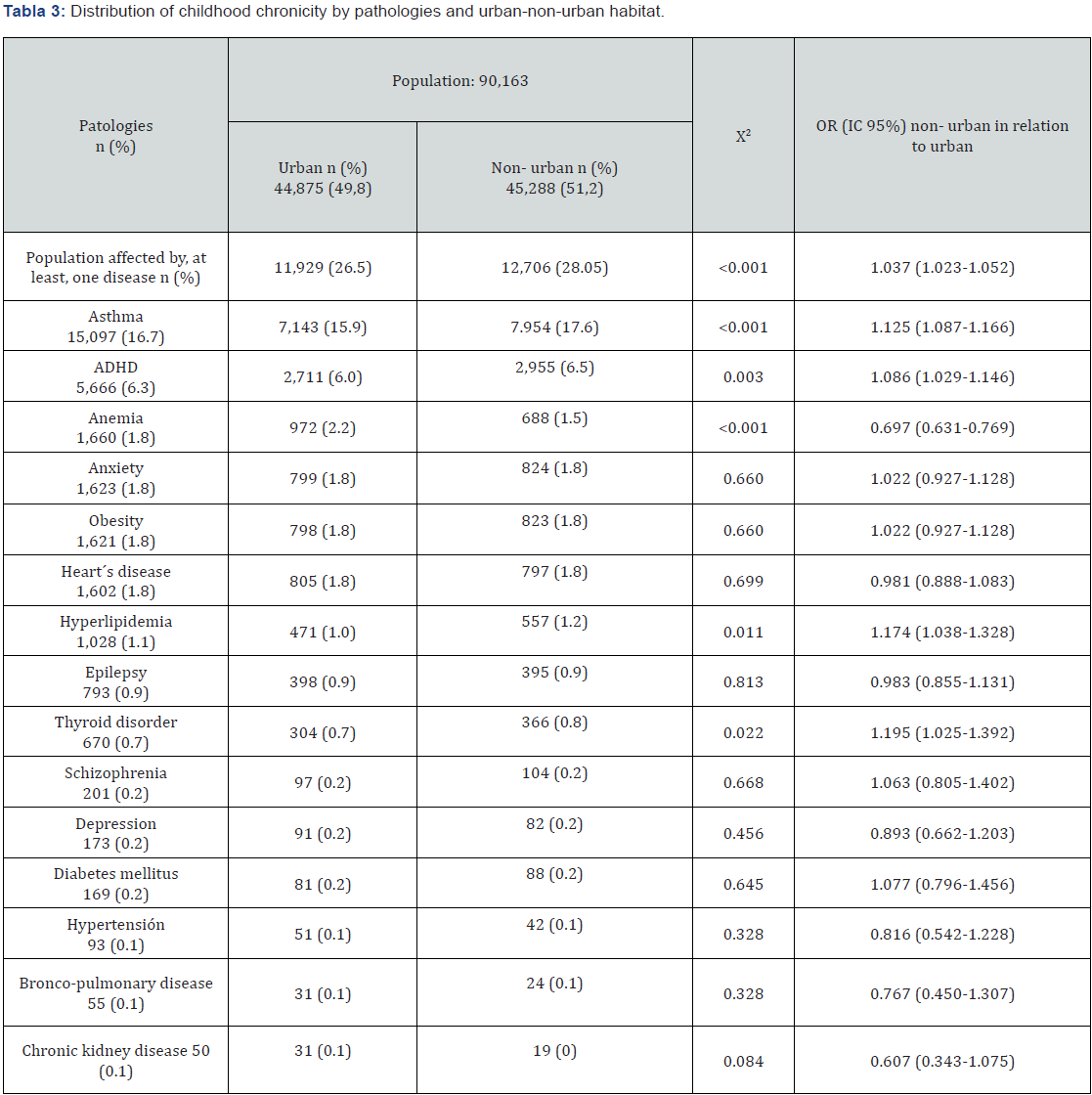
Regarding the area of residence, childhood and adolescent chronic pathologies were slightly more prevalent in non-urban areas (n= 13,510, 29.8%) compared to urban areas (n= 12,724, 28.4%) (χ2, p < 0.001 and OR for non-urban vs. urban 1.021; 95% CI: 1.013-1.030) (Table 2).
Anaemia was more common in urban areas, while asthma, ADHD, hyperlipidaemia, and thyroid disease were more common in non-urban areas. The rest of the chronic pathologies studied had a similar prevalence between urban and non-urban areas (Table 3).
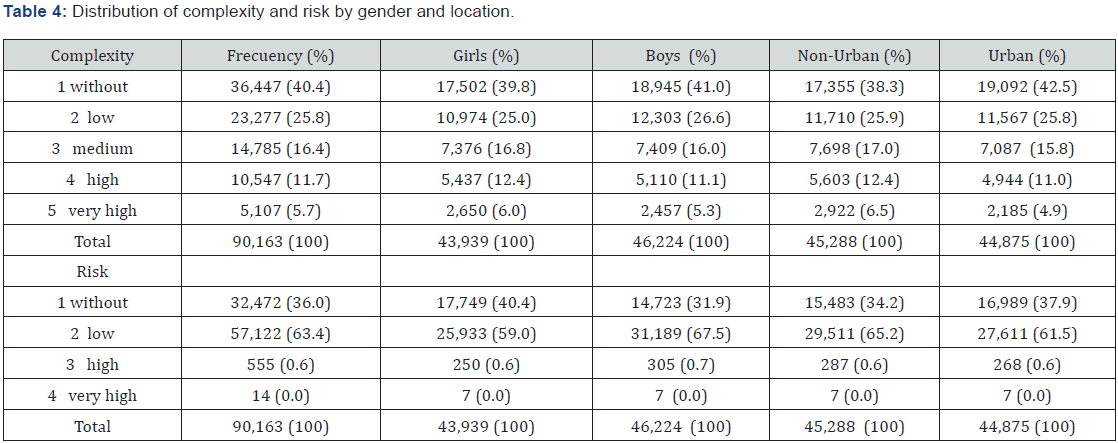
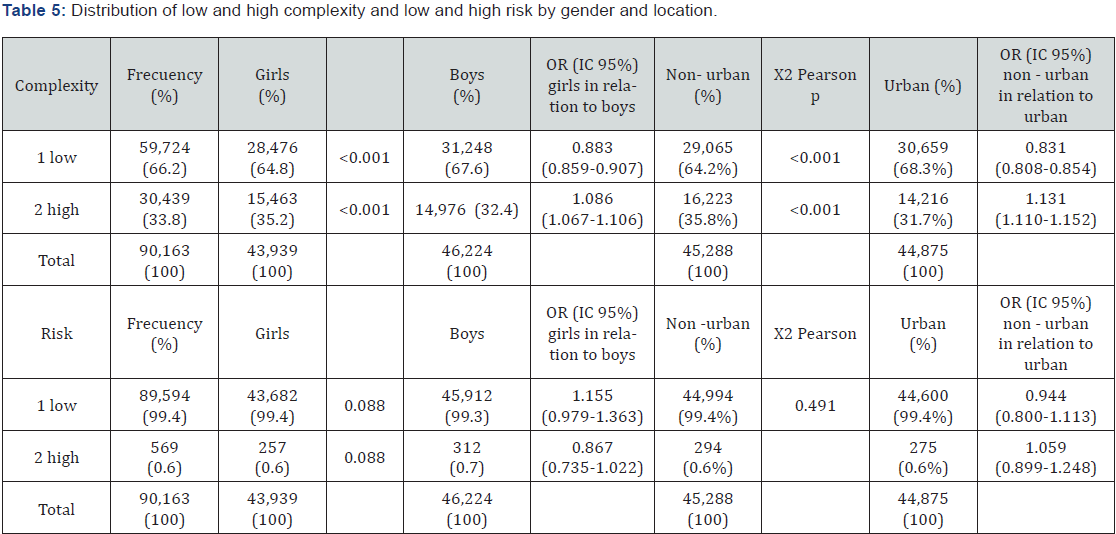
The data of the complexity and risk groups appear in Tables 4 and 5. Complexity was slightly higher in girls 15,463 (35.2%) than in boys 14,976 (32.4%) (χ2, p < 0.01 and OR for girls in relation to boys 1.086; 95% CI 1.067-1.106) and in the non-urban setting 16,223 (35.8%) versus urban 14,216 (31.7%) (χ2, p < 0.01 and OR for non-urban versus urban 1.131 95% CI 1.110-1.152). On the other hand, in the risk variable there were no differences by sex or by location, urban-non-urban, of the child-juvenile population, although the data may be biased because of the high-risk group only includes 0.6% of the total population.
Discussion
Currently the data that we have about the prevalence and distribution of CACPs is quite scant [43]. To the best of our knowledge this is the first approach to study CACPs based on the medical records of the whole under-18 population cared by a public health service in a European region to determine, not estimate, the prevalence of the most important pathologies that occur in this age group. To do this we used the AMG classification system. Our data showed a 29.1% prevalence of chronic diseases. This value was comprised on the wide range (from 5% up to over 30%) of prevalence reported in previous articles. We can observe that our prevalence value was quite close to the maximum level described [44,45]. Moreover, our result was higher than the one recently reported, employing a similar methodological approach where they obtained a prevalence value of 15.7% for the same age population [41]. Therefore, said study was performed on a very limited number of children (2,961) and a local population (the one attended in a primary health care centre in Madrid). On the other hand, we had similar data to the ones described in the mentioned paper when we compare the data for the groups of low-risk children with the ones obtained in the present study (99.9% for the former study and 99.4% in ours). When analysing the most common CACPs our results were like those reported in previous studies where both asthma and ADHD were the most frequent [46-49]. But the values, for the same diseases, in our results are statistically higher than those reported in the paper [41].
Differences among our results and those from other previous studies might exits due to fact that different criteria could have been used to define CACPs or to the use of a different data collection methodology. Our data were collected from the records of the total population of one European region (Cantabria) while other studies collected their data from interviews with parents, teachers and affected children and, on some occasions, data were collected from self-completed inventories. As an example, we might point out asthma, the most prevalent pathology on this age group, that is habitually assessed according to the questionnaires of the International Study of Asthma and Allergies in Childhood (ISAAC) [50,51], both overseas and in Spain [52,53]. Another cause of discrepancy between those data from other studies and ours could be related to the inclusion in the case of the previously mentioned CACPs that we do not consider since they are, in our opinion, acute pathologies such as certain infections (otitis, cystitis, tonsillitis, etc.).
When we paid attention to differences in gender, girls in general did present fewer numbers of pathologies than boys, in the total number of people affected, in multimorbidity, and in the clinical aspects, except for complexity, that was slightly higher in girls than in boys. These results were like those obtained employing our same methodology [41].
Our results showed a slight difference upon CACPs prevalence when comparing urban and rural areas (28.4% vs 29.8%). Similar differences were found when analysing multimorbidity and complexity level, but the risk was similar. We do not have an explanation for this fact. Our analysis of the data obtained showed lower values (which means a healthier environment) for the urban population, but our results have showed that several pathologies do not follow that trend. In this sense urban population and its range related to health has not been an issue of noteworthy attention in previous studies. However, several recent studies pay attention to the relationship between the urban population (urban and non-urban) and chronic pathologies, like the methodology that we have employed. An urban area is the one comprised by a town of a geographical area [54,55]. Some chronic pathologies are more frequent in urban areas, as published, such as obesity, hyperlipidaemia, and diabetes [56,57]. Those pathologies might be closely related to dietetic factors and a decrease in physical activity which are two factors that are related to urban life and sedentarism. Furthermore, a relation between those pathologies and the exposition to allergens, pollutants or some other toxins has previously been reported [58,59]. Most of the studies that analyse health differences between urban/ non-urban settings were centred on the occurrence of a specific pathology and in the total population or specifically to adults. Asthma, hyperlipidaemia, and ADHD were more frequent in nonurban settings, but anaemia was more frequent in urban areas. In our study there were no significant differences based on habitat for the rest of CACPs with a prevalence >1%. Our findings are not in agreement with some previously published results [59]. The analysis of chronicity´s complexity and the risk it originates was not an issue of much study using the AMG methodology in general and even less attention was paid in relation to the child-adolescent population. Furthermore, those studies were performed in a very geographically restricted population and the number of people studied was highly reduced in number [41], in comparison to the large population analysed in the present study.
It must be said that our study has some drawbacks. It´s transversality limits its capacity to investigate possible associations of some other factors with chronicity. Nevertheless, transversal studies are of paramount importance to evaluate diseases´ prevalence, which was the focus of the present study. In addition, our study is neither an estimation nor a sample approximation, as we employed an AMG approach obtained through the thorough analysis of the computerised clinical records of the whole CAAG population cared for by the public health service of our region (Cantabria). The described prevalence was the one that has been recorded, thus it increases the statistical power of our results. But admittedly the stratification program used to record the data could be biased. To give an example, we must mention the possibility to diagnose as epilepsy something that is in reality a case of febrile seizure, and on the other hand we have to admit that some pathologies could be underrepresented due to the fact that they were not well evaluated. In this last group of pathologies, we must include obesity, mainly because there is some controversy upon the criteria to assess it. Throughout the last decades the criteria to assess overweight among child and adolescent populations showed varying results [60,61]. Those data present a higher prevalence of obesity in Europe and in Spain than the one reported in this study [62,63], but these data are higher than the one reported in a previous study performed with the same methodological approach and in our country [41].
Another drawback is the absence of a “gold standard” for the optimal diagnosis of some of the CACPs. Our study it not unbiased due to the lack of an accurate recording system for some clinical diagnostics, this cannot be ruled out. In our opinion this bias is lower than those obtained through estimations and surveys, although these two methods were the proposed methodology to carry out epidemiological studies [64]. From our point of view that traditional methodological approach must be reviewed. As presently we can employ big data approaches. Another aspect to be mentioned is the fact that some members of the population under study have no disease symptoms and for this fact they do not look for medical care. In our opinion this circumstance is almost irrelevant because they are infant-adolescent and it’s their parents who will ask for their children’s health care [65]. Finally, the high frequency of some CACPs such as asthma and ADHD might introduce a bias of prevalence and for this reason lead to worse clinical data among boys and those inhabiting in a non-urban area.
There is no doubt that when studying chronicity´s attention, an important line of action will be the analysis of CACPs. This analysis will have to introduce an improved codification diagnostic and a better knowledge of the epidemiological distribution of those pathologies. All these actions will introduce new factors for a better prevention and health and social dealing with CACPs. This approach to the CACPs will help to place a reasonable budget and its accurate management, decreasing health expenditures and introducing a correct treatment that will improve the health of these individuals when reaching adulthood [66]. Additionally, this approach must be complemented with the introduction of specific health programs to educate and raise awareness to both health care professionals, teachers, family members and the childadolescent population.
Financing
The present work was financed with the funds of the Interreg SUDOE TiChroN project and INCVAL 17/03 project (in which C F-V, I L-H and A D-D participate), as well as the publication costs will also be assumed through the aforementioned projects.
ANNEX 1. Chronic pathologies analyzed
Attention deficit hyperactive disorder (ADHD)
Anemia
Anxiety
Asthma
Bronco-pulmonary disease
Chronic kidney disease
Depression
Diabetes
Epilepsy
Heart´s disease (including dysrhythmia, ischemic heart
disease, heart failure, valvular heart disease)
Hyperlipidemia
Hypertensión
Obesity
Schizophrenia
Thyroid disorder.
References
- Barnett K, Mercer SW, Norbury M, Watt G, Wyke S, et al. (2012) Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross-sectional study. Lancet 380(9836): 37-43.
- Grave GD, Pless IB (1974) Chronic childhood illness: assessment of outcome. A conference sponsored by the John E. Fogarty International Centre for Advanced Study in the Health Sciences and the National Institute of Child Health and Human Development, National Institutes of Health, Bethesda, Md., pp. 1-2.
- Davis AM, Brown RF, Taylor JL, Epstein RA, McPheeters ML (2014) Transition care for children with special health care needs. Pediatrics 134(5): 900-908.
- Compas BE, Jaser SS, Dunn MJ, Rodriguez EM (2012) Coping with chronic illness in childhood and adolescence. Annu Rev Clin Psychol 8: 455-480.
- Perrin JM, Bloom SR, Gortmaker SL (2007) the increase of childhood chronic conditions in the United States. JAMA 297: 2755.
- Van der Lee JH, Mokkink LB, Grootenhuis MA, Heymans HS, Offringa M (2007) Definitions and measurement of chronic health conditions in childhood. JAMA 297: 2741.
- Mokkink LB, van der Lee JH, Grootenhuis MA, Offringa M, Heymans HAS (2008) Defining chronic diseases and health conditions in childhood (0-18 years of age): National consensus in the Netherlands. Eur J Pediatr 167: 1441-1447.
- Van Cleave J (2010) Dynamics of obesity and chronic health conditions among children and youth. JAMA 303(7): 623-630.
- Nasir A, Nasir L, Tarrell A, Finken D, Lacroix A, et al. (2018) Complexity in pediatric primary care. Prim Health Care Res Dev.20: e59.
- Denny S, de Silva M, Fleming T, Clark T, Merry S, et al. (2014) The prevalence of chronic health conditions impacting on daily functioning and the association with emotional well-being among a national sample of high school students. J Adolesc Health. 54(4): 410-415.
- Pinquart M, Shen Y (2011) Depressive symptoms in children and adolescents with chronic physical illness: An updated meta-analysis. J Pediatr Psychol 36(4): 375-384.
- Gerteis J, Izrael D, Deitz D, LeRoy L, Ricciardi R, et al. (2014) Multiple chronic conditions chart book. Agency for Healthcare Research and Quality; Rockville, MD: 2014.
- Goodman R, Posner SF, Huang ES, Parekh AK, Koh HK (2013) Defining and measuring chronic conditions: Imperatives for research, policy program, and practice. Prev Chronic Dis 10: E66.
- Violan C, Foguet-Boreu Q, Flores-Mateo G, Salisbury C, Blom J, et al. (2014) Prevalence determinants and patterns of multi-morbidity in primary care: A systematic review of observational studies. PLOS ONE 9(7): e102149.
- Judson L (2004) Global childhood chronic illness. Nurs Adm Q 28(1): 60-66.
- Compas BE, Jaser SS, Dunn MJ, Rodriguez EM (2012) Coping with chronic illness in childhood and adolescence. Annu Rev Clin Psychol 8: 455-480.
- Catalá-López F, Gènova-Maleras R, Álvarez-Martín E (2013) Carga de enfermedad en adolescentes y jóvenes en España. Rev Psiquiatr Salud Ment 6(3): 80-85.
- Flegel K (2014) chronically ill children and fragile families. CMAJ 186(16): 1195.
- Bell MF, Bayliss DM, Glauert R, Harrison A, Ohan JL (2016) Chronic Illness and Developmental Vulnerability at School Entry. Pediatrics 137(5): e20152475.
- Forrest CB, Bevans KB, Riley AW, Crespo R, Louis TA (2011) School outcomes of children with special health care needs. Pediatrics 128(2): 303–312.
- Deavin A, Greasley P, Dixon C (2018) Children's Perspectives on Living with a Sibling with a Chronic Illness. Pediatrics 142(2): e20174151.
- van Til JA, Groothuis-Oudshoorn C, Vlasblom E, Kocken PL, Boere-Boonekamp MM (2019) Primary care in five European countries: A citizens' perspective on the quality of care for children. PloS one 14(11): e0224550.
- Silber JH, Rosenbaum PR, Pimentel SD, Calhoun S, Wang W, et al. (2019) Comparing Resource Use in Medical Admissions of Children With Complex Chronic Conditions. Med Care 57(8): 615-624.
- Wise PH (2017) the future pediatrician: the challenge of chronic illness. J Pediatr 151(5 Suppl): S6-S10.
- Maslow GR, Haydon AA, Ford CA, Halpern CT (2011) Young adult outcomes of children growing up with chronic illness: an analysis of the National Longitudinal Study of Adolescent Health. Arch Pediatr Adolesc Med 165(3): 256–261.
- Busse R, Blümel M, Scheller-Kreinsen D, Zentner A (2014) Tackling chronic disease in Europe. Strategies, interventions and challenges. Observatory Studies Series No 20. European Observatory on Health Systems and Policies. World Health Organization 2010.
- OECD/European Union (2018) Health at a Glance: Europe 2018: State of Health in the EU Cycle. OECD Publishing.
- Joint Action Chrodis Plus (2017-2019) Implementing good practices for chronic diseases.
- Utilización de las TICs como herramienta de mejora en la atención integral de niños con enfermedades crónicas (2018-2021)
- McDougall J, King G, De Wit DJ, Miller LT, Hong S, et al. (2004) Chronic physical health conditions and disability among Canadian school-aged children: A national profile. Disabil Rehabil 26(1): 35–45.
- Hendricks R (1993) A Model for National Health Care: The History of Kaiser Permanente. Rutgers University Press, New Brunswick, NJ, USA, Pp. 13-17.
- Nuño Solinís R (2007) Buenas prácticas en gestión sanitaria: el caso Kaiser Permanente. Rev Adm Sanit Siglo XXI 5: 283-292.
- Humphries R (2011) Social care funding and the NHS An impending crisis? The King’s Fund.
- Ministerio de Sanidad Servicios Sociales e Igualdad (2012) Estrategia para el abordaje de la cronicidad en el Sistema Nacional de Salud. Madrid. Ministerio de Sanidad.
- Hughes JS, Averill RF, Eisenhandler J, Goldfield NI, Muldoon J, et al. (2004) Clinical Risk Groups (CRGs) Med Care 42(1): 81-90.
- Orueta JF, Urraca J, Berraondo I, Darpón J, Aurrekoetxea J (2006) Adjusted Clinical Groups (ACGs) explain the utilization of primary care in Spain based on information registered in the medical records: A cross-sectional study. Health Policy 76(1): 38-48.
- Monterde D, Vela E, Clèries M (2016) Los grupos de morbilidad ajustados: nuevo agrupador de morbilidad poblacional de utilidad en el ámbito de la atención primaria. Atención Primaria 48: 674-682.
- Monterde D, Vela E, Clèries M, García Eroles L, Pérez Sust P (2019) Validez de los grupos de morbilidad ajustados respecto a los clinical risk groups en el ámbito de la atención primaria. Aten Primaria 51(1): 153-161.
- Barrio-Cortes J, del Cura-González I, Martínez-Martín M, López-Rodríguez C, Jaime-Sisó MÁ, et al. (2020) Grupos de morbilidad ajustados: características y comorbilidades de los pacientes crónicos según el nivel de riesgo en Atención Primaria. Atención Primaria 52(2): 86-95.
- Grupo de trabajo Ministerio de Sanidad Servicios Sociales e Igualdad (2018) Informe del proyecto de estratificación de la población por grupos de morbilidad ajustados (GMA) en el Sistema Nacional de Salud (2014-2016) Fundació de Tecnologia, innovació i salut (TicSalut) Madrid, MSCBS.
- Barrio Cortes J, Suárez Fernández C, Bandeira de Oliveira M, Muñoz Lagos C, Beca Martínez MT, et al. (2020) Enfermedades crónicas en población pediátrica: comorbilidades y uso de servicios en Atención Primaria. An Pediatr 93(3): 183-193.
- Estupiñán-Ramírez M, Tristancho-Ajamil R, Company-Sancho MC, Sánchez-Janáriz H (2019) Comparación de modelos predictivos para la selección de pacientes de alta complejidad. Gac Sanit 33: 60-65.
- Odgers HL, Tong A, Lopez-Vargas P, Davidson A, Jaffe A, et al. (2018) Research priority setting in childhood chronic disease: a systematic review. Arch Dis Child. 103(10): 942-951
- Lopez-Vargas P, Tong A, Crowe S, Alexander SI, Caldwell PHY, et al. (2019) Kaleidoscope Project workshop investigators. Research priorities for childhood chronic conditions: a workshop report. Arch Dis Child. 104(3): 237-245.
- Secinti E, Thompson EJ, Richards M, Gaysina D. (2017) Research Review: Childhood chronic physical illness and adult emotional health - a systematic review and meta-analysis. J Child Psychol Psychiatry 58 (7): 753-769.
- The Global Asthma Report (2018) Auckland, NewZealand: Global Asthma Network.
- Carvajal-Urueña I, García-Marcos L, Busquets-Monge R, Morales Suárez-Varela M, García de Andoin N, et al. (2005) Variaciones geográficas en la prevalencia de asma en los niños y adolescentes españoles. International Study of Asthma and Allergies in Childhood (ISAAC) fase III España. Arch Bronconeumol 41: 659-666.
- Reale L, Bonati M (2018) ADHD prevalence estimates in Italian children and adolescents: a methodological issue. Ital J Pediatr 44(1): 108.
- Morkem R, Handelman K, Queenan JA, Birtwhistle R, Barber D (2020) Validation of an EMR algorithm to measure the prevalence of ADHD in the Canadian Primary Care Sentinel Surveillance Network (CPCSSN). BMC Med Inform Decis Mak 20(1): 166.
- Asher MI, Weiland SK (1998) The International Study of Asthma and Allergies in Childhood (ISAAC) ISAAC Steering Committee. Clin Exp Allergy 28(Suppl 5): 52-66; discussion 90-91.
- (1998) Worldwide variation in prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and atopic eczema: ISAAC. The International Study of Asthma and Allergies in Childhood (ISAAC) Steering Committee. Lancet 351(9111): 1225-1232.
- Álvarez Dobaño, JM (2016) Asma infantil en el área sanitaria de Santiago: prevalencia, gravedad y factores de riesgo asociados. Tesis Doctoral. Universidad de Santiago de Compostela.
- Elizalde-Beiras I, Guillén-Grima F, Aguinaga-Ontoso I (2018) Prevalencia y factores asociados al asma infantil en la zona media de Navarra: Tesis Doctoral. Universidad Pública de Navarra. Aten primaria 50(6): 332-339. [Article in Spanish].
- Vlahov D, Galea S (2002) Urbanization, urbanicity, and health. J Urban Health 79(4 Suppl 1): S1–S12.
- Allender S, Foster C, Hutchinson L, Arambepola C (2008) Quantification of urbanization in relation to chronic diseases in developing countries: a systematic review. J Urban Health 85(6): 938-951.
- Mohan V, Mathur P, Deepa R, Deepa M, Shukla DK, et al. (2008) Urban rural differences in prevalence of self-reported diabetes in India: The WHO-ICMR Indian NCD risk factor surveillance. Diabetes Res Clin Pract 80(1): 159-168.
- Wolch J, Jerrett M, Reynolds K, McConnell R, Chang R, et al. (2011) Childhood obesity and proximity to urban parks and recreational resources: a longitudinal cohort study. Health Place 17(1): 207–214.
- Godfrey R, Julien M (2005) Urbanisation and health. Clin Med (Lond) 5(2): 137-141.
- Timperio A, Giles-Corti B, Crawford D, Andrianopoulos N, Ball K, et al (2008) Features of public open spaces and physical activity among children: findings from the CLAN study. Prev Med 47(5): 514–518.
- Brug J, van Stralen MM, Te Velde SJ, Chinapaw MJ, De Bourdeaudhuij I, et al. (2012) Differences in weight status and energy-balance related behaviors among School children across Europe: the ENERGY-project. PLoS One 7(4): e34742.
- Ng M, Fleming T, Robinson M, Thomson B, Graetz N, et al (2014) Global, regional, and national prevalence of overweight and obesity in children and adults during 1980-2013: a systematic analysis for the global burden of disease study 2013. Lancet 384(9945): 766–781.
- Schröder H, Ribas L, Koebnick C, Funtikova A, Gomez SF, et al. (2014) Prevalence of Abdominal Obesity in Spanish Children and Adolescents. Do We Need Waist Circumference Measurements in Pediatric Practice? PLoS ONE 9(1): e87549.
- Garrido-Miguel M, Cavero-Redondo I, Álvarez-Bueno C, Rodríguez-Artalejo F, Moreno LA, et al (2019) Prevalence and Trends of Overweight and Obesity in European Children From (1999 to 2016): A Systematic Review and Meta-analysis. JAMA Pediatr 173(10): e192430.
- Remes ST, Pekkanen J, Remes K, Salonen RO, Korppi M. (2002) In search of childhood asthma: questionnaire, tests of bronchial hyperresponsiveness, and clinical evaluation. Thorax 57(2): 120-6.
- Serbin LA, Hubert M, Hastings PD, Stack DM, Schwartzman AE (2014) the influence of parenting on early childhood health and health care utilization. J Pediatr Psychol 39(10): 1161-1174.
- Modi AC, Pai AL, Hommel KA, Hood KK, Cortina S, Hilliard ME, et al. (2012) Pediatric self-management: a framework for research, practice, and policy. Pediatrics 129(2): e473-85.






























