Prolonged Survival in a Liveborn Male Prenatally Diagnosed Non-Mosaic (Complete) Trisomy 22: A Case Report
D. Pineda*, K Schmidbauer and J Holcomb
Children’s Hospital of Georgia, Augusta University, USA
Submission: October 13, 2020; Published: February 21, 2022
*Corresponding author:D. Pineda, Children’s Hospital of Georgia, Augusta University, 1446 Harper St, Augusta, GA 30912, USA, Tel: (706) 721-5437
How to cite this article:D. Pineda, K Schmidbauer, J Holcomb. Prolonged Survival in a Liveborn Male Prenatally Diagnosed Non-Mosaic (Complete) Trisomy 22: A Case Report. Acad J Ped Neonatol 2022; 11(3): 555866. 10.19080/AJPN.2022.11.555866
Abstract
Trisomy 22 is a chromosomal disorder rarely associated with the survival of live-born infants secondary to severe, congenital anomalies. Most affected children die before one year of age. Typical malformations include microcephaly, congenital heart disease, and renal malformations, along with other atypical features. This case presents a complete, non-mosaic trisomy 22 male with prolonged survival to-day of life 112 (four months of age). Trisomy 22 was confirmed via peripheral blood cytogenic studies showing complete, non-mosaic additional chromosome 22 in all metaphases. The patient had multiple organ malformations consistent with previously documented cases of trisomy 22, with the addition of intrahepatic cholestasis, congenital hypothyroidism, absent gallbladder, and early onset seizures. To date, only 29 liveborn cases have been reported and none have reported liver and gallbladder disease in association with Trisomy 22.
Keywords: Trisomy 22, chromosomal abnormality, mosaicism, liveborn
Introduction
Trisomy 22 is a chromosomal disorder, which is one of the most common autosomal anomalies leading to early, spontaneous abortions. Greater than 96% of errors leading to trisomy 22 occur during oogenesis [1]. Non-mosaic trisomy is rarely associated with live-born infants, with few documented cases reported in the literature. Infants born with non-mosaic trisomy 22 have a poor prognosis, with prolonged survival being unusual [2]. It is important to differentiate non-mosaic from mosaic trisomy 22, as mosaic trisomy 22 is compatible with life and prolonged survival. Of the documented cases, survival of non-mosaic trisomy 22 has varied from a few minutes after birth to three years, with median survival of four days [3]. In utero, the most common feature associated with trisomy 22 is intrauterine growth restriction and oligohydramnios. Multiple organ malformations and fetal structural anomalies are typically seen but presentation can be variable [4] [5] [6].
Case Presentation
A single-live born, African-American, male was born to a 35-year-old G2P1001 at 38 and 3/7 weeks via spontaneous vaginal delivery (SVD). Mother was induced secondary to intrauterine growth restriction of the baby. Mother previously delivered a healthy term child. Mother had no major medical conditions and denied any use of tobacco, drugs, or alcohol. Mother’s only known medications were albuterol, escitalopram and loratadine. There was no consanguinity. Family history was unremarkable for previous genetic disorders.
Fetal trisomy 22 without mosaicism was confirmed via amniocentesis at 22 weeks’ gestation. Amniocentesis showed 47, XY, + 22 in all cells. Prenatal ultrasound identified multiple congenital defects, including congenital cardiac disease and genitourinary anomalies, along with oligohydramnios. Ultrasounds prior to birth were significant for estimated fetal weight (EFW) less than the second percentile, elevated dopplers, two vessel cord and decreased amniotic fluid, with an Amniotic Fluid Index of 11.5. The infant was also expected to have bilateral cleft lip with possible palatal involvement, questionable ambiguous genitalia, absent vs. left pelvic kidney and cardiac anomalies. Neonatal Intensive Care Unit (NICU) consultation and counseling was done prior to delivery in regards to the poor prognosis; however, parents wished to proceed with the pregnancy.
Infant was born at 38 and 3/7 weeks via SVD secondary to induction of labor and intrauterine growth restriction. APGAR at one and five minutes of life were three and five, respectively, with infant requiring brief positive pressure ventilation (PPV) before transitioning to continuous positive airway pressure (CPAP). Birth weight was 1570 grams, less than the third percentile, length was 41.5 cm, less than the third percentile, and head circumference was 27.5 cm, less than the third percentile. Infant transitioned to noninvasive positive pressure ventilation secondary to respiratory acidosis shortly after arrival to the NICU.
On exam, infant noted to have contractures of all extremities, microcephaly, orbital hypertelorism, down-slanting palpebral fissures, low-set ears with pits bilaterally, bilateral cleft lip involving nasal septum (palate intact), flattened nasal bridge, webbed neck, clinodactyly of fifth digit on bilateral hands, severe hypospadias, and imperforate anus. Echocardiogram was performed and significant for a large inlet ventricular septal defect, with anterior extension, a large, bidirectional patent ductus arteriosus, and a thickened, tri-leaflet and doming aortic valve. Left and right ventricular systolic function was mildly diminished. There was no surgical intervention for his cardiac defects due to his poor prognosis. Renal ultrasound was significant for a left ectopic pelvic kidney, with bilateral kidneys small for age. Patient had colostomy placed secondary to imperforate anus. Thyroid studies were consistent with hypothyroidism and patient was started on levothyroxine.
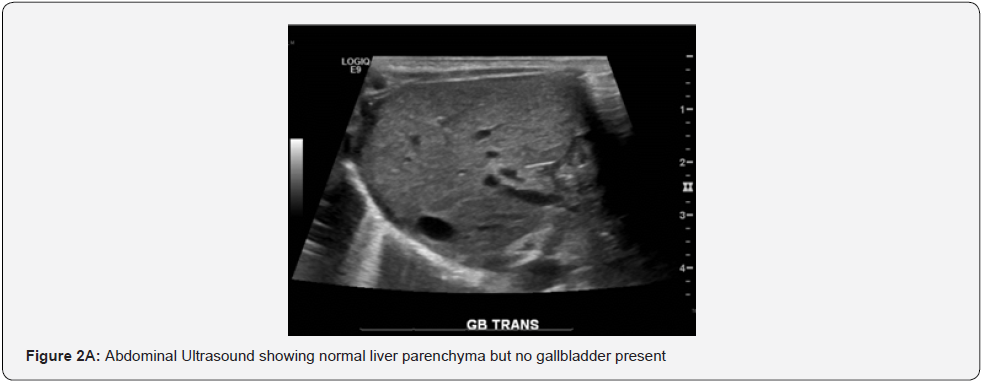
The infant was noted to develop an increasing direct hyperbilirubinemia, without transaminitis, on day of life (DOL) three. A formal gastroenterology and hepatology consult was placed on DOL four. Abdominal ultrasound was obtained and showed normal liver parenchyma, with concerns for biliary atresia versus neonatal hepatitis. Timing of biliary of atresia was too early in this infant and in the setting of normal liver parenchyma, neonatal hepatitis was less likely. HIDA scan was subsequently performed that showed intrahepatic cholestasis. Patient was started on Ursodiol on DOL seven.
Infant was discharged home on DOL 55 with home hospice. Shortly after discharge, the infant had new seizure activity while at home and had to be started on Levetiracetam. An EEG was later obtained and significant for the presence of left cortical dysfunction with nonspecific etiology.
Infant was re-admitted to the hospital following cardiac arrest requiring CPR at home on DOL 99. Patient was stabilized and discharged home on DOL 109, but readmitted three days later for acute, hypoxic respiratory failure. Due to patient’s worsening clinical status and poor prognosis, family opted for palliative care and infant died on DOL 112. Autopsy not performed as parents declined.
Cytogenic findings
After birth, Fluorescence in situ hybridization (FISH), with a panel of probes specific for detection of chromosomal trisomy: 13, 18, and 21, was performed on peripheral blood leukocytes of the patient. No evidence of aneuploidy was seen for these chromosomes. Peripheral blood leukocytes were then sent for full chromosomal analysis, with 20 metaphase spreads counted. GTGbanding was performed on the metaphase spreads, revealing 47, XY, +22 in all cells analyzed (see Figure 1). There was no evidence of mosaicism.
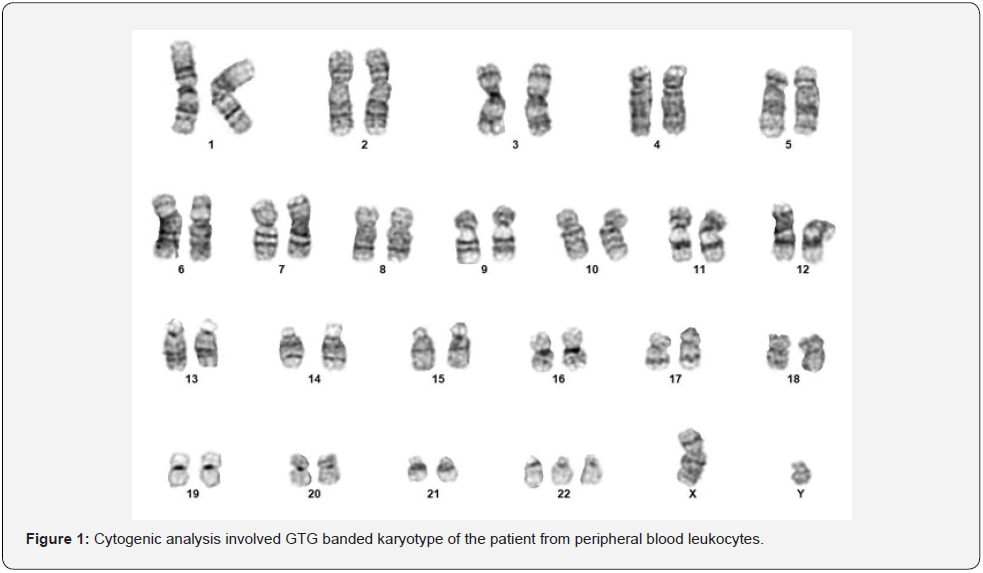
Discussion
Trisomy 22 (“complete” or “non-mosaic” Trisomy 22) is a rare chromosomal disorder. In contrast to mosaic trisomy 22, complete trisomy 22 is incompatible with life. Survival beyond the first trimester is rare. To date there are only 29 documented survivors and mean survival has been about four days. Our infant discussed here is now another documented survivor, with survival to four months of age. Typically, survived children have typical features of midface hypoplasia with flat/broad nasal bridge, ear malformation with pits or tags, cleft palate, increased distance between organs or bodily parts, unusually small head, congenital heart disease, genital abnormalities, and IUGR (NORD, 2021). Trisomy 16 occurs most frequently (1% of pregnancies) followed by trisomy 21 (0.4%) and trisomy 22 (0.5%) [7] [8].
In this report we describe the clinical presentation of a live born complete trisomy 22 diagnosed at 20 weeks’ gestation with confirmation of diagnosis postnatally. This infant is one of the rare cases known to survive up to four months of age. Presentation prenatally was typical according to previous reports of findings.
However, the infant presented with a direct hyperbilirubinemia as early as three days of life. The infant had a direct bilirubin of 1.6 on DOL one and total bilirubin of 6.1 that proceeded to increase to a direct bilirubin of 5.4 on DOL four with total bilirubin of 8.6. Infant initially had direct hyperbilirubinemia without elevated transaminases; however, at around two weeks of life, he developed elevated transaminases with ALT as high as 251 and AST 519. Infant was worked up to assess for the cause of the direct hyperbilirubinemia and a Gastroenterology and Hepatology consult was placed on DOL three.
Ultrasound findings presented normal liver parenchyma (see Figure 2A and 2B); however, this imaging could not rule out biliary atresia vs. Neonatal hepatitis. Timing was too early for the possibility of biliary atresia and infant had pigmented stools [9]. Neonatal hepatitis was initially excluded as a differential as initial transaminases were low; however as discussed earlier these peaked at around two weeks of life. Thyroid studies were obtained and significant for the diagnosis of congenital hypothyroidism. Infant was subsequently started on Levothyroxine, which may have been a possible etiology for his conjugated hyperbilirubinemia.
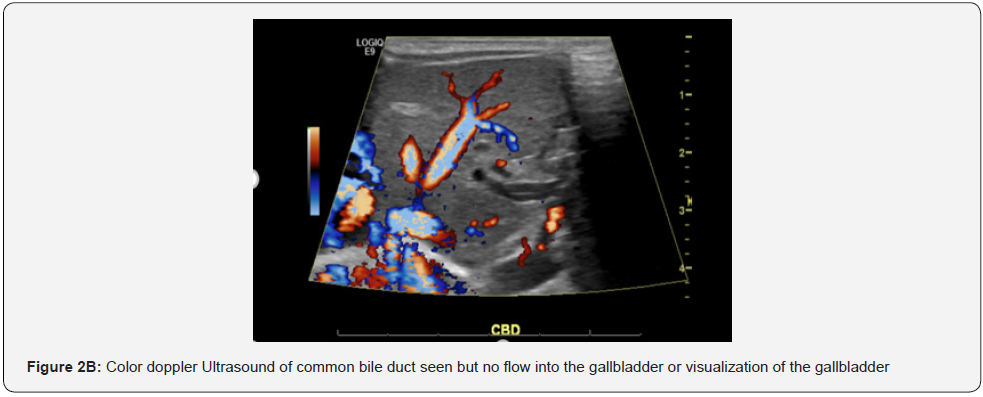
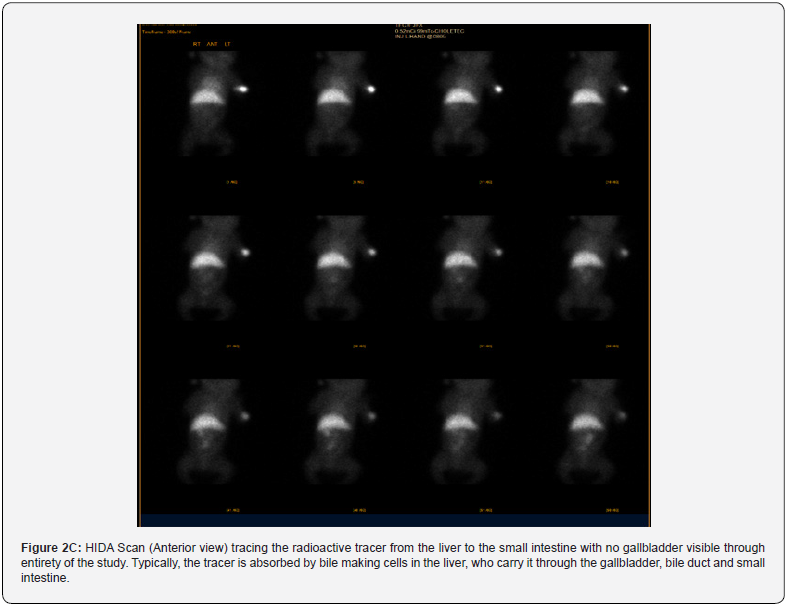
A HIDA (see Figure 2C) scan performed showed evidence of intrahepatic cholestasis; gallbladder was unable to be visualized on both abdominal ultrasound and HIDA scan. Interestingly, we found only one individual report of a complete trisomy 22 with thyroid isthmus agenesis and absent gallbladder; however, this infant was a feticide at 27 week’s gestation [10]. While it seems that congenital hypothyroidism presents in Mosaic Trisomy 22, there were no reports found in non-mosaic trisomy infants. Congenital hypothyroidism was seen in our case, along with report of absent gallbladder and development of direct hyperbilirubinemia, with findings of intrahepatic cholestasis.
Further workup included a newborn screen reported with elevated cystic fibrosis (CF) IRT, but with no CF mutations, as well as an amino acid profile above normal limits but with low risk of maple syrup urine disease. While Total Parenteral Nutrition (TPN) can be a differential for TPN associated cholestasis, the infant in our case developed direct hyperbilirubinemia prior to starting TPN [11]. Liver biopsy may have been an approach to provide a definitive explanation for the infant’s findings; however, after infant’s demise, autopsy was declined by parents.
Another rare development in our case is the development of seizure activity, requiring the patient to be started on Levetiracetam for control of his seizures. One previous case report identifies the development of seizures between the ages of three to five years in two trisomy 22 patients [12]. However, no other case reports have reported seizures in a complete trisomy 22 at an early age. Our patient developed seizures at around two months of age at home, which were described as bilateral upper extremity flexion that started and stopped over 15 minutes. Seizures resolved following administration of lorazepam. Infant was subsequently started on Levetiracetam by the palliative medicine physician.
Infant had a coding event at home requiring chest compressions and subsequently admitted to the PICU. With background of seizures, an EEG was obtained while infant was admitted that showed abnormalities due to the presence of left temporal asymmetry sharp and slow activity, which was suggestive of left cortical dysfunction with nonspecific etiology. At the time of admission infant was on palliative management and due to decompensation events through his hospital course, a MRI of the brain was never completed.
Conclusion
The infant presented in this clinical report provides new findings that may be associated with the diagnosis of Trisomy 22. Due to the rare survival of infants with non-mosaic Trisomy 22, most documented abnormalities are limited to findings seen prenatally via ultrasound or findings seen in the few documented live-born infants [13]. The prolonged survival of the patient in this case allowed for the discovery of congenital hypothyroidism, gallbladder agenesis, intrahepatic cholestasis, and early onset seizures. These findings in a non-mosaic trisomy 22 patient are uncommon or non-existent in the current literature. The severity of these anomalies, as well as the known severe congenital malformations are important factors to consider in the medical management of patients with non-mosaic trisomy 22. These factors also play a significant role when counseling families prenatally and postnatally [14] [15].
Declaration of Conflicting Interests
The authors declare that there are no conflicts of interest..
References
- Hall HE, Surti U, Hoffner L, Shirley S, Feingold E, et al. (2007) The origin of trisomy 22: evidence for acrocentric chromosome-specific patterns of nondisjunction. Am J Med Genet A 143A(19): 2249–2255.
- Bi-Qiu Xu, Xiao-Cui Jiang, Li Wan, Sha Wang, Yan-Dong Yang, et al. (2020) Prenatal diagnosis of trisomy 22 at the first trimester of pregnancy. J Obstet Gynaecol 40(3): 440-442.
- Tinkle BT, Walker ME, Blough-Pfau RI, Saal HM, Hopkin RJ (2003) Unexpected Survival in a Case of Prenatally Diagnosed Non-Mosaic Trisomy 22: Clinical Report and Review of the Natural History. Am J Med Genet A 118A(1): 90-95.
- Schwendemann WD, Contag SA, Koty PP, Miller RC, Devers P (2009) Ultrasound findings in trisomy 22. Am J Perinatol 26(11): 135-137.
- Fruhman G, El-Hattab AW, Belmont JW, Patel A, Cheung SW, et al. (2011) Suspected trisomy 22: modification, clarification, or confirmation of the diagnosis by aCGH. Am J Med Genet 155(2): 434-438.
- Henrich T, Nanda I, U Zollner, E Frieauff, J Wirbelauer, et al. (2012) Live-Born Trisomy 22: Patient Report and Review. Mol Sydromol 3(6): 262-269.
- Kehinde F, Anderson C, McGowan JE, Jethva RN, Wahab MA, et al. (2014) Co-Occurrence of Non-Mosaic Trisomy 22 and Inherited Balanced t(4;6) (q33;q23.3) in a Liveborn Female: Case Report and Review of the Literature. Am J Med Genet A 164A(12): 3187-3193.
- Scott F, Bonifacio M, Sandow R, Ellis K, Smet ME, et al. (2018) Rare autosomal trisomies: Important and not so rare. Prenat Diagn 38(10): 765-771.
- Lakshminarayanan B, Davenport M (2016) Biliary atresia: A comprehensive review. J Autoimmune 73: 1-9.
- Gangbo E, Lacombe D, Alberti EM, Taine L, Saura R, et al. (2004) Trisomy 22 with thyroid isthmus agenesis and absent gall bladder. Genet Couns 15(4): 311–315.
- Feldman AG, Sokol RJ (12) Neonatal Cholestasis: Update on Diagnostics, Therapeutics, and Prevention. NeoReviews 22(12): e819-e836.
- Shokier MH (1978) Complete Trisomy 22. Clin Genet 14(3): 139-146.
- Chen CP, Huang MC, Chern SR, Wu PS, Chen SW, et al. (2019) Mosaic trisomy 22 at amniocentesis: Prenatal diagnosis and literature review. Taiwan J Obstet Gynecol 58(5): 692-697.
- Leclercq S, Baron X, Jacquemont ML, Cuillier F, Cartault F (2010) Mosaic trisomy 22: five new cases with variable outcomes. Implications for genetic counselling and clinical management. Prenat Diagn 30(2): 168–172.
- Phung V, Dabagh S (2021) Complete Trisomy 22 and Congenital Heart Repair: The Impact of Shared Decision Making. Pediatrics 147(3_MeetingAbstract): 522. 10.1542/peds.147.3MA5.522a.






























