Spontaneous Pneumopericardium in a Term Newborn
Peter Krcho1 and Steven M Donn2*
1Department of Pediatrics (Neonatology), Pavol Jozef Šafárik University, Kosice, Slovakia
2Division of Neonatal-Perinatal Medicine, C.S. Mott Children’s Hospital, Michigan Medicine, University of Michigan, Ann Arbor, Michigan, USA
Submission: November 20, 2021; Published: December 03 2021
*Corresponding author: Steven M Donn, Division of Neonatal-Perinatal Medicine, 8-621 C.S. Mott Children’s Hospital, 1540 E. Hospital Drive, Ann Arbor, MI, USA Acad
How to cite this article:Peter Krcho, Steven M. Donn. Spontaneous Pneumopericardium in a Term Newborn. Acad J Ped Neonatol 2021; 11(1): 555860. 10.19080/AJPN.2021.11.555860
Abstract
We present the case of a term newborn who developed cardiopulmonary distress at 15 minutes of age secondary to a spontaneous pneumopericardium. Diagnostic and therapeutic considerations are addressed.
Keywords: Newborn, Pneumopericardium, Pneumothorax, Transillumination, Pericardiocentesis
Case Report
A term male infant was born at 40 weeks’ gestation to a 37-year-old primigravida mother. The pregnancy was achieved through in vitro fertilization. The mother was treated with Enoxaparin during the pregnancy for thrombophilia. Labor was complicated by failure to progress, and a Cesarean section was performed. The baby was macrosomic (4210 g) and required forceps to assist the delivery during the Cesarean section. The baby transitioned without difficulty. Apgar scores were 8 and 10 at one and five minutes, respectively.
At 15 minutes of age the infant suddenly developed pallor and a fall in pulse oximetery. On auscultation, heart sounds were barely perceptible.
Vital signs were heart rate 80 beats per minute, respiration 58 breaths per minute, and blood pressure 71/45 with a mean of 53 mmHg. An arterial blood gas at 20 minutes of age revealed pH 7.10, pCO2 58.8 torr, BE -13.9 mEq/L, lactate 4.7 mmol/L and glucose 68 mg/dL. Over the next 90 minutes, the infant continued to deteriorate. Mean blood pressure fell to 35 mmHg but improved to 52 after administration of dopamine. The baby was moved to the neonatal intensive care unit, sedated, intubated and placed on mechanical ventilation. He required a maximal FiO2 of 0.8 but was able to be weaned to 0.25 by 16 hours.
A chest radiograph (Figure1) demonstrated a pneumopericardium, which was confirmed on transillumination (Figure 2). A follow-up radiograph showed the presence of a pneumothorax as well. A needle thoracentesis removed 40 mL of air.
The infant was successfully extubated after two days. He received three days of antibiotic treatment for suspected sepsis, but all cultures remained negative. All the air leaks resolved, and the infant was discharged at 7 days.
Discussion
Air leak syndrome in the newborn is usually manifested as pneumothorax (PTX) and/or pneumomediastinum (PM) in the term infant and by PTX and/or pulmonary interstitial emphysema (PIE) in the preterm infant. Pneumopericardium (PPC) is a rare complication of thoracic air leaks (TALs) in the newborn [1-5]. In general, air leaks seen in neonates with RDS frequently occur in situations where a delay in stabilization of the respiratory status leads to the development of heterogeneous lung disease and poor distribution of gas flow within the lung.
Thoracic air leaks can lead to catastrophic complications inflluencing not only respiratory function but also cardiac performance, especially during transition [6]. Pneumopericardium in term infants is uncommon but does occasionally occur in nonventilated infants or in those undergoing active resuscitation, those with aspiration syndromes, or as a complication of dyssynchronous mechanical ventilation [7]. Pneumopericardium is one of the rarest forms of TALs. Air accumulates in the pericardial sac and may lead to cardiac tamponade. PPC is more common in premature infants with a history of respiratory distress requiring mechanical ventilation and is rarely observed in term infants.
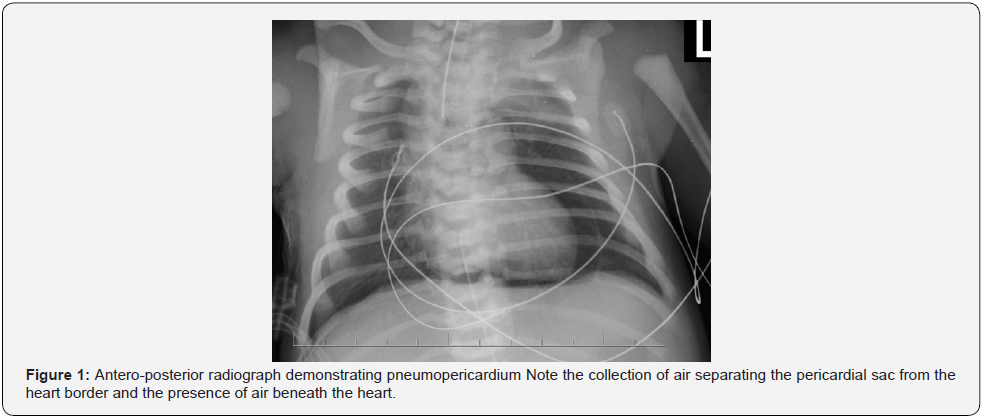
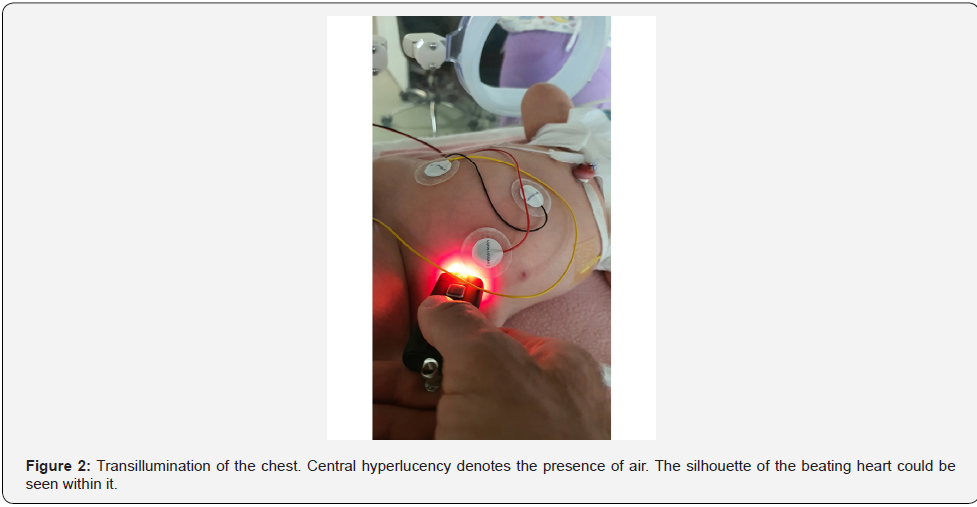
It is unclear if it is related to complicated extraction or difficult delivery or after lung recruitment in the delivery room using positive pressure ventilation. In this case, it is possible that a difficult delivery led to aspiration of amniotic fluid with a subsequent TAL. Thoracic air leaks occur when alveoli or terminal airways are overdistended and rupture into the perivascular bundle. Escaping air tracks toward the hilum of the lung causing PM, PTX, PPC, and subcutaneous emphysema. In premature infants the interstitium is less dissectible, and the air will remain in the perivascular sheath causing PIE. In term infants, inspired air may not be completely exhaled during expiration in situations where there is increased resistance or inadequate time for expiration, such as aspiration syndromes.
Pneumopericardium is a rare but potentially serious complication caused by dissection of leaked air through the great vessels. The trapped air in the pericardial space can quickly cause tamponade of the heart, decreasing venous return and cardiac output. This should be suspected when the pulse pressure is narrow and when heart sounds are muffled on auscultation [8]. The diagnosis of TALs are generally made by plain chest radiography.
PPC appears as free air completely surrounding the heart but not extending beyond the aorta or pulmonary artery into the upper mediastinum. It is sometimes difficult to distinguish from a PM, but if the air is between the heart and diaphragm, it is diagnostic for PPC. On the lateral view, PM generally appears as an accumulation of air in a retrosternal location, while the anteroposterior view may show the “bat wing” sign, as the thymus is pushed anterior and cephalad by the accumulating air. Transillumination of the chest with a fiberoptic light source can also assist in the diagnosis of PPC [9]. The central chest will appear hyperlucent and the silhouette of the beating heart can be seen within the lucent area. Treatment of PPC is dictated by the clinical manifestations. If the infant is hemodynamically stable and does not show signs of impaired perfusion, observation and supportive therapy may be attempted. On the other hand, if there is evidence of cardiac tamponade or altered cardiopulmonary function, the air will need to be evacuated. Initially, pericardiocentesis may be attempted.
If the PPC is recurrent or continuous, a pericardial tube may need to be inserted and placed to underwater seal. Again, transillumination may be a helpful adjunct. Cabatu and Brown described transillumination guidance of pericardial tube placement [10]. The prognosis of PPC depends upon its severity. Clinical manifestations vary widely from asymptomatic to lifethreatening. Older literature reported an 86% mortality with untreated cardiac tamponade, but more current diagnostic and therapeutic techniques should greatly lower this figure [11].
References
- Brans YW, Pitts M, Cassady G (1976) Neonatal pneumopericardium. Am J Dis Child 130(4): 393-396.
- Burt B, Lester PD (1982) Neonatal pneumopericardium. Radiology 142(1): 81-84.
- Walker TL, Shannon DA, (2017) Pneumopericardium in the neonate. Neonatal Netw 36(6): 368-373.
- Garvey A, Filan P (2019) Neonatal pneumopericardium. Arch Dis Child Fetal Neonatal Ed 104(5): F479.
- Kataria Hale J, Fernandez CJ, Speer ME (2020) Pneumopericardium in the neonate: a case report. Perfusion 35(4): 360-362.
- Varano LA, Maisels MJ (1974) Pneumopericardium in the newborn: diagnosis and pathogenesis. Pediatrics 53(6): 941–945.
- Suresh P, Tagare A, Kadam S, Vaidya U, Pandit A, et al. (2011) Spontaneous pneumopericardium in a healthy full-term neonate. Indian J Pediatr 78(11): 1410-1411.
- Al Tawil K, Abu Ekteish FM, Tamimi O, Al Hathal MM, Al Hathiol K, et al. (2004) Symptomatic spontaneous pneumothorax in term newborn infants. Pediatr Pulmonol 37(5): 443-446.
- Donn SM, Kuhns LR (1983) Pediatric Transillumination. Book Medical Publishers, Chicago, USA.
- Cabatu EE, Brown EG (1979) Thoracic transillumination: aid in the diagnosis and treatment of pneumopericardium. Pediatrics 64(6): 958-960.
- Lawson EE, Gould JB, Tauesch HW (1980) Neonatal pneumopericardium: current management. J Pediatr Surg 15(2): 181-185.






























