Congenital Candidiasis - A Rare Cause of Skin Eruption
Diana Reis Monteiro*, Ana Bernardo Ferreira, Liliana Quaresma, Inês Ferreira, Margarida Azevedo and Teresa Andrade
Neonatology Unit, Pediatrics/Neonatology Department, Centro Hospitalar Entre Douro e Vouga, Portugal
Submission: June 13, 2021; Published: October 07 2021
*Corresponding author: Diana Reis Monteiro, R. Dr. Cândido Pinho 5, 4520-211 Santa Maria da Feira, Portugal
How to cite this article: Diana R M, Ana Bernardo F, Liliana Q, Inês F, Margarida A, et al. Congenital Candidiasis - A Rare Cause of Skin Eruption. Acad J Ped Neonatol 2021; 10(4): 555853. DOI: 10.19080/AJPN.2021.10.555853
Abstract
Congenital candidiasis is an extremely rare condition that results from vertical transmission of an infection by Candida species. It can produce a wide spectrum of disease ranging from a diffuse skin eruption to severe systemic infection with high morbidity and mortality, particularly in low birth weight and extremely low birth weight infants. We report a case of a full-term neonate who presented at birth with a generalized skin eruption, characterized by erythematous macules and papules diffusely distributed through the body surface, with palms and soles involved. The pregnancy was uneventful except for several episodes of candida vulvovaginitis. During the first day of life an aggravation of the exanthema was progressively observed, associated with fever, signs of respiratory distress, hemodynamic instability, and an increase in inflammatory laboratory parameters. Treatment with Liposomal Amphotericin b was initiated and later a positive result for Candida Albicans in skin scrape and urine analysis was found. Our patient showed a progressively clinical improvement and after 21 days of antifungal therapy he was medically discharged. We discuss clinical features, risk factors, diagnosis and treatment based on a review of previous published literature.
Keywords: Congenital Disorders, Candidiasis, Newborn, Exanthema
Abbreviations: CC: Congenital Candidiasis; NICU: Neonatal Intensive Care Unit
Introduction
Congenital candidiasis (CC) is an extremely rare condition that results from an intrauterine infection by Candida species and usually manifests itself at birth or during the first days of life [1,2]. It can produce a wide spectrum of disease ranging from a diffuse skin eruption to severe systemic infection with high morbidity and mortality, particularly in low birth weight and extremely low birth weight infants [1-6]. The clinical variability of CC can make it a challenging diagnostic and its similarity to more common causes of skin eruptions in the newborn can delay the diagnosis and increase the risk for adverse sequelae [1].
We report a case of a full-term neonate with CC and discuss clinical features, risk factors, diagnosis and treatment based on a review of previous published literature.
Case Report
We report a case of a male patient, born to a 30-year-old gravida 3 para 2 woman, whose results from the third trimester analysis were negative for venereal disease research laboratory, human immunodeficiency virus, types B and C hepatitis tests, as well as immune to rubella and not immune to toxoplasmosis. Throughout pregnancy were reported several episodes of vaginal infections, some of them described as candida vulvovaginitis, treated accordingly. Cardiotocography monitoring showed no signs of fetal distress and spontaneous membranes rupture occurred 8 hours before labor.
Our patient was a full-term neonate, 3670gr, born by spontaneous vaginal delivery, with Apgar scores of 9 and 10 at 1 and 5 minutes, respectively. On the first physical examination there was a well-developed newborn, with good vitality status, that presented a generalized skin eruption, characterized by erythematous macules and papules diffusely distributed through the entire body surface except for mucosae, with palms and soles involved, without nail disorder, as shown in Figures 1, 2 and 3. There were not any other abnormalities in the remainder examination.
Figure 1 to 3: Generalized skin eruption, characterized by erythematous macules and papules.
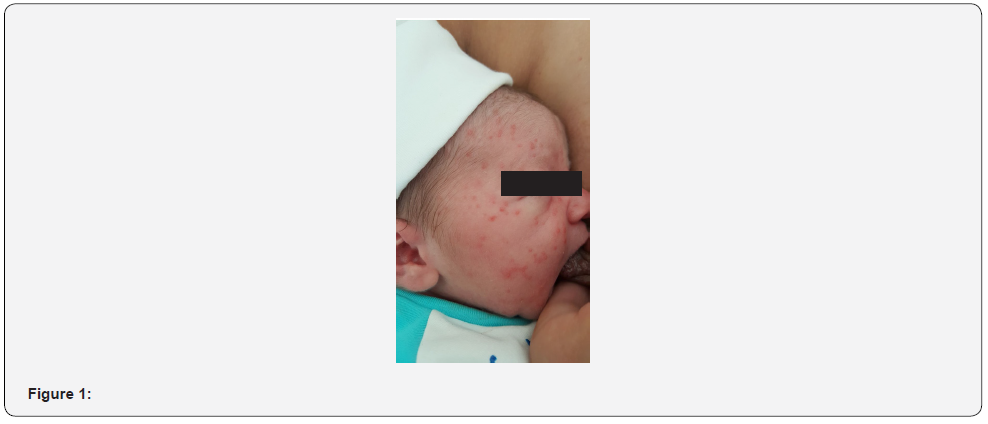
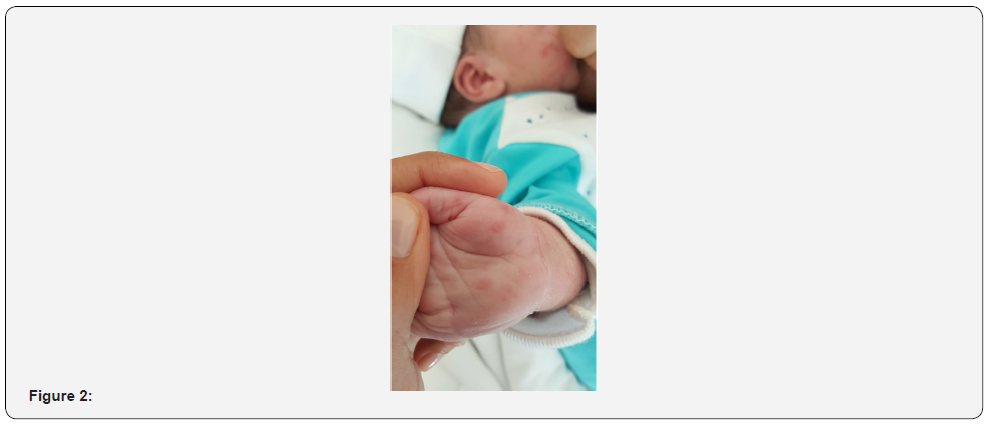
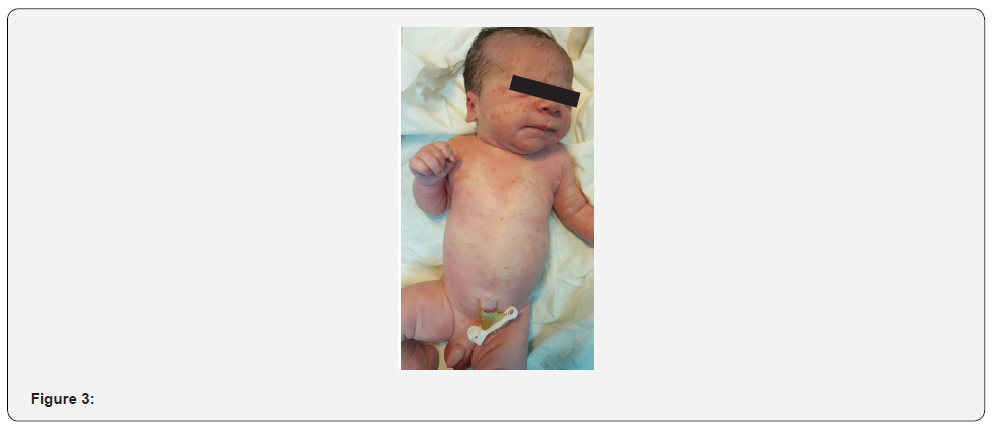
Initial laboratory tests showed no relevant findings, with a total leukocyte count of 11,100/mm3, procalcitonin of 0.49 ng/mL (reference values in the first 6 hours of life < 2ng/mL), and c-reactive protein of 4.8 mg/L (reference values 0.8-15.8 mg/L). Due to the normal overall status, normal feeding tolerance and the lack of abnormal findings in laboratory tests, the newborn stayed initially in the nursery with his mother. However, during the first 19 hours of life, an aggravation of the exanthema was progressively observed, associated with fever and an increase in inflammatory laboratory parameters, with a c-reactive protein of 12.7 mg/L and a procalcitonin of 2.79 ng/mL. The newborn was admitted in Neonatal Intensive Care Unit (NICU). At this point our patient presented an aggravated maculopapular exanthema, widely distributed, with erythematous base, involving palms, soles, and skin folds, non-desquamative, non-petechial, sparing mucosae (Figures 4 and 5).
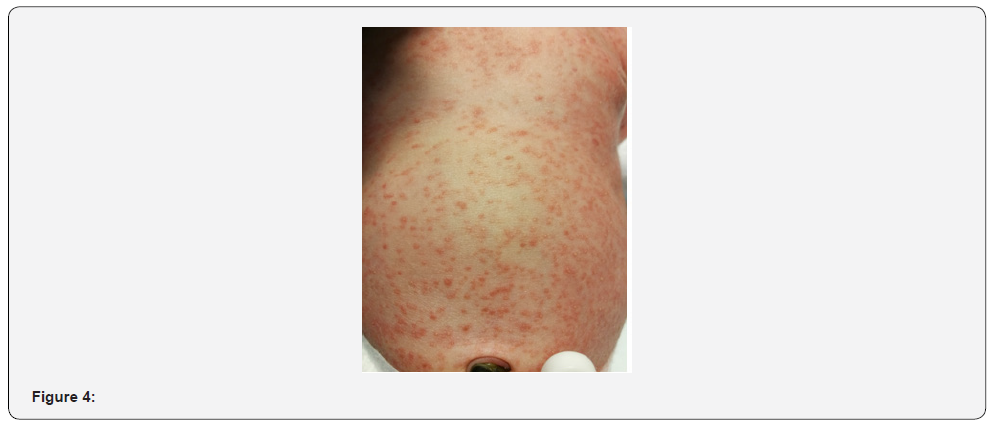
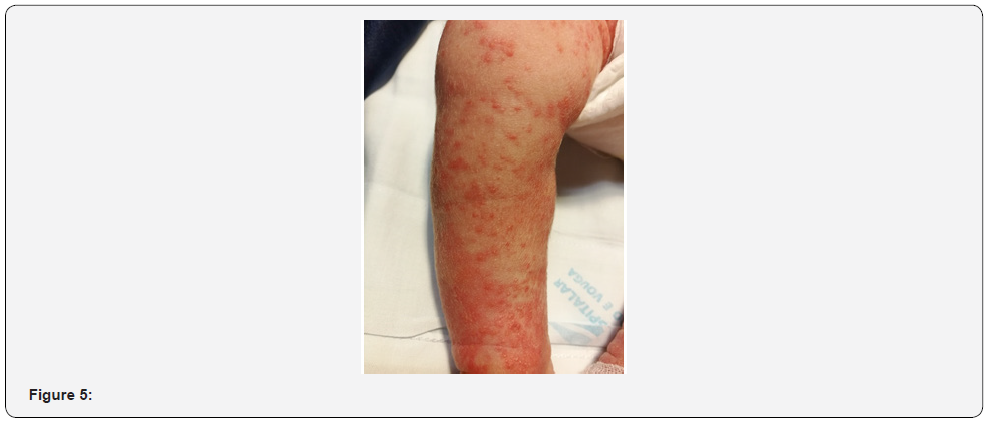
Figure 4 and 5: Aggravated maculopapular exanthema.
A short time after the admission in the NICU, he started showing signs of respiratory distress as well as hemodynamic instability. Ventilation support was not necessary, however ionotropic treatment was needed for 3 days. Chest radiography showed a heterogeneous pulmonary infiltrate, and initial blood and urine cultures were negative. It was decided to initiate antibiotics for suspected neonatal sepsis with Ampicillin and Gentamicin. After 48 hours of treatment there was no improvement of the symptoms. In fact, the number of cutaneous lesions was increasing, the exanthema was worsening and developing a more humidified aspect, especially in skin folds (Figures 6 and 7).
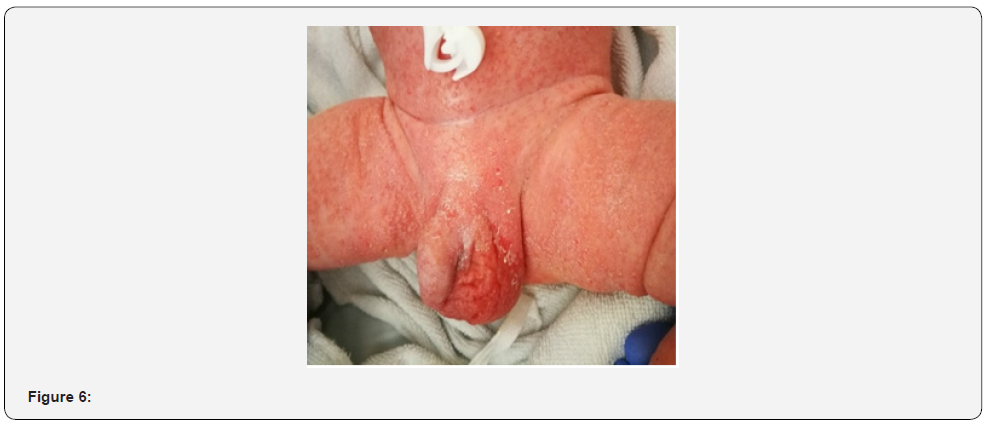
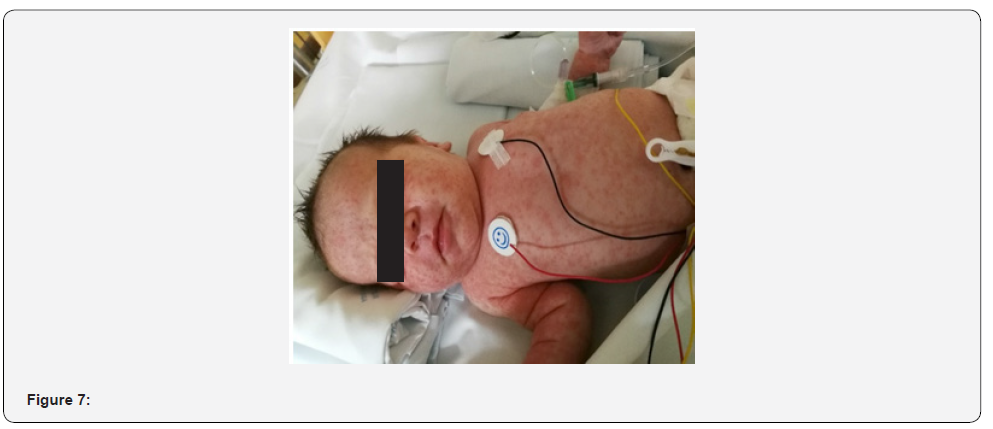
Figure 6 and 7 Exanthema with humidified aspect, especially in skin folds.
Given the extensive exanthema, the laboratory evidence of sepsis, the lack of improvement with antibiotic treatment in course, as well as the history of several episodes of vaginal candidiasis documented throughout the pregnancy, the possibility of an infection by Candida species with systemic involvement seemed the most probable. After blood and urine cultures were repeated, and skin scrape analysis was performed, empiric treatment with Liposomal Amphotericin b was started.
Later, a positive result for Candida Albicans in skin scrape and second urine analysis was found, while the second blood culture was negative. To complement the evaluation, renal, vesical and transfontanelar ultrasounds were performed, all with normal results, as well as an ophthalmologic observation, also without abnormal findings. Neurological examination was performed regularly, and the evaluation was always normal.
Throughout admission, laboratory tests showed a maximum of 15,8 mg/L c-reactive protein and 2,79 ng/mL procalcitonin, with liver enzyme function always within the normal values.
Placenta analysis showed signs of ascending infection as severe acute chorioamnionitis and funiculitis with abscesses, with necrotizing fetal response and white-yellow plaques on the umbilical cord.
Our patient showed a progressively clinical improvement, with skin lesions gradually reducing, and after 21 days of antifungal therapy he was medically discharged.
Discussion
The clinical variability of CC can make it a challenging diagnostic [1]. Its most frequent presentation is a generalized eruption, with erythematous macules and papules, that may progress to vesicular and pustular stages [1,5-9], with palms and soles involved [6-10], and skin folds and extensor surfaces described as areas of greater involvement [2], but there are also published cases that presented with peeling, flaking and dry cracking rashes. [1] It usually appears within the first 24 hours of life [5], but there are reports of a delayed onset (≤7 days) [1,2,6,8,9,11,12]. The acute phase is then followed by a desquamation phase [2,5,8,9,11].
Usually, full-term neonates show a benign infection while preterm patients are more vulnerable to present an exuberant infection or even systemic spread, which might be explained by their immature mucocutaneous barrier and systemic host defenses [2,6,12]. Besides lower gestational age [1,3-5,10,11,13] and low birth weight [3,5,6,10,11,13] other risk factors for fungal infection have been considered, such as maternal candida vulvovaginitis [1,2,10-12] the use of large spectrum antibiotics [1,3,6,12-14] length of parenteral nutrition and presence of central catheter [4,11,13]. Although vaginal candidiasis is common during pregnancy, only in a small percentage of patients occurs vertical transmission [14], with Candida on the fetal surface of less than 1% of placentas [2,10-12]
In terms of diagnosis, skin scraping analysis and cultures of blood, urine and cerebrospinal fluid should be obtained if an infection by Candida is suspected, however, its sensitivity to detect infection is poor [1-3,5-8,11] As a result, a positive result of Candida isolated from any normally sterile body fluid should be treated as evidence of systemic disease [3,8]. The diagnosis of central nervous system involvement is also challenging as normal cerebrospinal fluid parameters may be present in infants with candidal meningitis [3]. In our case, lumbar puncture was not performed because the rash was present over the back. Systemic infection is defined by a positive result of blood, urine, or cerebrospinal fluid cultures, nevertheless, those patients with burn-like dermatitis, respiratory distress, altered liver enzymes as well as laboratory evidence of sepsis should be considered systemically infected until proven otherwise [2,6,8,10].
Concerning the histological evaluation of the placenta and umbilical cord, the appearance of whitish nodules is characteristic of fungal infection [1,2,7-12,14] but can also appear in infection caused by Listeria monocytogenes [2].
The list of differential diagnosis can be very extensive and includes a range of diseases, from benign eruptions to serious and life-threatening conditions, since CC should be distinguished from other more common causes of neonatal eruptions [5,8,12]. It should include non-infectious benign entities, such as erythema toxicum, neonatal acne, milliaria, transient neonatal pustular melanosis, acropustulosis of infancy, eosinophilic pustular folliculitis; non-infectious but potentially serious entities such as acrodermatitis enterophatica, incontinentia pigmenti, epidermolysis bullosa, Langerhans cell histiocytosis, Herpes gestationis, pemphigus vulgaris neonatal; and infectious diseases, whether they are mild like scabies or neonatal candidiasis, or potentially serious infections such as bacterial (Clamydia, Escherichia coli, Hemophilus Influenza, Klebsiella Pneumoniae, Pseudomonas Aeruginosa, Staphilococcus Aureus, Listeria monocytogenes, Group A beta-hemolytic Stretococcus), fungal (congenital candidiasis) and viral (herpes simplex, varicella, cytomegalovirus). [1,2,5,6,11]
Regarding treatment, there is different opinions among authors. Some authors claim that antifungal topical treatment may be used for exclusively cutaneous infections to decrease the number of viable organisms and lower the risk of systemic spread [2,6,11] However, others state that once there are skin findings neonatal biopsies have demonstrated that CC is an invasive fungal infection with involvement of the epidermis and dermis that requires systemic treatment [1]. Systemic empiric treatment should be initiated promptly, not only in cases of a positive blood, urine, or cerebrospinal fluid analysis, but as soon as Candida is suspected in patients with “burn-like” dermatitis, respiratory distress in early neonatal period, laboratory evidence of sepsis and extensive cutaneous involvement. [2,6,8] Therapy options for candidiasis include Fluconazole 12 mg/kg/day, Amphotericin B deoxycholate 1 mg/kg/day, Liposomal amphotericin B 5 mg/kg/day and Micafungin 10 mg/kg/day. [1,3,6,13] There is no consent when it comes to choose the best drug and the duration of the treatment. Among Polyenes, studies show that both Amphotericin B deoxycholate and amphotericin B lipid products were efficient in the treatment of candidiasis [3] Fluconazole is an alternative therapy, proved to be safe and effective in the treatment of invasive candidiasis, with hepatotoxicity as its most concerning side effect [3]. Micafungin is an alternative for candidiasis treatment in neonatal period, but only if endophthalmitis was previous excluded since this drug doesn´t penetrate the vitreous [3]. Regarding the duration of the treatment, it is acceptable a minimum of 14 to 21 days in case of suspected invasive disease [1,6], nevertheless additional studies are recommended to document microbiologic clearance [3]. If cultures continue to be positive by day 7, the addition of a second agent should be considered [3].
In cases of invasive disease, previous publications registered a 11-50% mortality rate [3,7,15], as well as the possibility of neurocognitive impairment [3,4,13], especially in preterms and extremely low birth weight infants, as full-term patients usually follow a benign course and recover without long-term sequelae [2,8]. The early recognition and diagnosis of systemic infection by Candida species is essential to start prompt treatment and improve outcome and survival rates [1-3,10]. Neurocognitive evaluations should be performed as part of the follow-up of these patients, to identify those at risk and give intervention support if needed [3]
Conclusion
CC is an uncommon cause of skin eruption in the newborn that presents as a variable rash and can affect both preterm and term infants. This case highlights the importance of the clinical evaluation and reminds us to consider this entity as part of the differential diagnosis when a newborn presents with an exanthema at birth with palms and soles involved. As a rare but potentially serious disease, its early recognition and clinical intervention is essential to decrease the likelihood of complications.
References
- Kaufman DA, Coggins SA, Zanelli SA, Weitkamp J (2017) Congenital Cutaneous Candidiasis: Prompt Systemic Treatment Is Associated with Improved Outcomes in Neonates. Clin Infect Dis 64(10): 1387-1395.
- Darmstadt GL, Dinulos JG, Miller Z (2000) Congenital Cutaneous Candidiasis: Clinical Presentation, Pathogenesis, and Management Guidelines. Pediatrics 105(2): 438-444.
- Greenberg RG, Benjamin DK (2014) Neonatal Candidiasis: diagnosis, prevention, and treatment. J Infect 69(1): 19-22.
- Benjamin DK, Stoll BJ, Gantz MG, Walsh MC, Sánchez PJ, et al. (2010) Neonatal Candidiasis: Epidemiology, Risk Factors, and Clinical Judgment. Pediatrics 126(4): 865-873.
- Araújo T, Schachner L (2006) Benign vesicopustular eruptions in the neonate. An Bras Dermatol 81(4): 359-366.
- Jagtap SA, Saple PP, Dhaliat SB (2011) Congenital cutaneous candidiasis: a rare and unpredictable disease. Indian J Dermatol 56(1): 92-93.
- https://www.uptodate.com/contents/treatment-of-candida-infection-in-neonates
- Rolim S, Figueirinha J, Miguel C, Lopes S, Rocha F, et al. (2021) Congenital Candidiasis – A Diagnostic Challenge. Nascer e Crescer - Birth and Growth Medical Journal 30(1): 48-51.
- Colantonio S, Hedin E, Oi-Yee Li H, Gavigan G (2019) Management of congenital cutaneous candidiasis in a healthy term baby: A case report. SAGE Open Med Case Rep 7: 1-3.
- Mandal S, Banerjee M, Mallick A K (2019) Congenital Candidiasis. Pediatr Oncall J 16: 49-50.
- Tiraboschi ICN, Niveyro C, Mandarano AM, Messer SA, Bogdanowicz E, et al. (2010) Congenital candidiasis: confirmation of mother-neonate transmission using molecular analysis techniques. Medical Mycology 48(1): 177-181.
- Siriratsivawong R, Pavlis M, Hymes SR, Mintzer JP (2014) Congenital candidiasis: an uncommon skin eruption presenting at birth. Cutis 93(5): 229-232.
- Botero-Calderon L, Benjamin DK, Cohen-Wolkowiez M (2015) Advances in the treatment of invasive neonatal candidiasis. Expert opinion on pharmacotherapy. 16(7): 1035-1048.
- Fernández-Ruiza M, Mosqueda-Peña R, Pérez-Ayala A, Blázquez-Gamero D (2020) Congenital cutaneous candidiasis associated with maternal peripartum candidemia. Rev Iberoam Micol 37(2): 68-71.
- Zaoutis TE, Heydon K, Localio R, Walsh TJ, Feudtner C (2007) Outcomes Attributable to Neonatal Candidiasis. Clin Infect Dis 44(9): 1187-1193.






























