Unfolded Brain Tumor in A Young Child Presenting with Gastroenteritis: Lesson to Learn
Fatihi Hassan Soliman Toaimah1,2*, Mohammed H A Nasser Al-Amri1,2, Mohammad Hashim S Al shawagfeh1, Liju Skariah1, Ahmad Alshami1,2, Mohammad Munir Mohammad Aleter1 and Fysel Manthattil1
1Division of Pediatric Emergency Medicine, Department of Pediatrics, Hamad Medical Corporation, Qatar
2Department of Clinical Pediatrics and Clinical Emergency Medicine, Weill Cornell Medical College, Qatar
Submission: May 24, 2021; Published: October 05 2021
*Corresponding author: Dr. Fatihi Hassan Soliman Toaimah, MD, PhD: Pediatric Emergency Al-Sadd, Hamad Medical Corporation, PO Box 3050, Doha, Qatar
How to cite this article: Toaimah F H S, Al-Amri M H A N, Al shawagfeh M H S, Skariah L, Alshami A, et al. Unfolded Brain Tumor in A Young Child Presenting with Gastroenteritis: Lesson to Learn. Acad J Ped Neonatol 2021; 10(4): 555852. DOI: 10.19080/AJPN.2021.10.555852
Abstract
Craniopharyngiomas are generally slow-growing benign tumors, having its clinical picture and associated symptoms due to tumor compression on the adjacent neurological structures. We report a case of 4½-year-old boy who presented to the emergency department (ED) with the chief complaint of abdominal pain and vomiting with history of recurrent constipation for the last 5 months. The patient’s condition improved initially following intravenous (IV) fluid therapy, however, later he developed seizures and manifestations of raised intracranial pressure (ICP), requiring anticonvulsants and measures to reduce the raised ICP. Urgent CT scan of the head showed a midline complex solid and cystic mass lesion compatible with craniopharyngioma that compressed the third ventricle, causing obstructive acute hydrocephalus of both lateral ventricles. Hormonal assay done and showed central hypothyroidism and adrenal insufficiency. He has received IV hypertonic saline, dexamethasone and an external ventricular drain (EVD) was urgently implanted via right frontal approach, which drained cerebrospinal fluid and thus reducing ICP. Magnetic resonance imaging (MRI) showed a sellar and suprasellar retrochiasmatic adamantinomatous craniopharyngioma, with third ventricular extension. Almost complete surgical excision of the tumor was done using subfrontal approach with favourable outcome. The patient was discharged home in a good general condition on hormonal replacement therapy. This case report shows unfolding of a craniopharyngioma during the management of gastroenteritis.
Keywords: Craniopharyngioma, Gastroenteritis, Brain tumor; Intracranial pressure; Hydrocephalus
Introduction
Craniopharyngiomas are tumors arising from epithelial remnants of Rathke’s pouch along its line of development from the nasopharynx to the diencephalon. They are considered as a parasellar histologically benign tumors with solid or cystic/solid appearance near the pituitary stalk at the base of the skull [1,2]. These tumors usually grow slowly, and symptoms often are present for months or years, leading to late diagnosis until the compression effects become significant enough that leads to variable symptoms [3]. At the time of diagnosis, approximately 50% of cases have headache, and 20-50% have endocrine deficiencies, 62%–84% have visual disturbances [4,5].
The overall incidence rate is 1.86 cases per 1,000,000 persons/year, with a peak incidence rate occurring at 5-9 years of age in children and at 40-44 years in the adult population [6]. The hypothalamic-pituitary hormone dysfunction is generally common to some extent in most patients with craniopharyngioma. A complete and thorough endocrinologic evaluation is extremely important to identify and correct hormonal insufficiency [7,8]. Morbid obesity, epilepsy, growth failure and psychiatric conditions have all been documented as long-term complications [9]. The objective of this case report is to highlight new insights into the complexity of craniopharyngioma and its diverse clinical presentation.
Case Report
A 4½-year-old boy presented to the emergency department (ED) with vomiting and abdominal pain of three days duration, and lethargy for one day in the absence of fever, drug intake or trauma. He had been complaining of intermittent constipation of five months duration with multiple visits to ED, and was managed with laxatives, fleet enema and dietary modifications. He was able to attend the school, had a normal appetite, and appeared otherwise well.
The initial physical examination revealed an afebrile, little hypoactive boy, conscious, oriented and hemodynamically stable without focal neurological abnormalities. His initial vital signs showed temperature (T), 36.5 °C; heart rate (HR), 96 beats/min; respiratory rate (RR), 28 breaths/min; blood pressure (BP) 105/66 mm Hg; and oxygen saturation (SpO2), 100% on room air. He had dry lips with some dehydration, capillary refill time (CRT) of <2 seconds, and the remaining systemic examination were unremarkable. His height for age was 95 cm (-2.5 SD) and his weight was 14.7 kg (-1.6 SD).
He was admitted to the short-stay unit as gastroenteritis with dehydration and received intravenous (IV) fluids and ondansetron. Initial blood investigations were normal including complete blood count, electrolytes and blood gases. His symptoms were improved, tolerated oral fluids, however while leaving the ED following discharge, he developed a brief generalized clonic convulsion, which aborted by itself. The patient was connected to cardiac monitor that showed bradycardia with HR of 56 beats/min. However, other vital signs including neurologic assessments, blood sugar and electrolytes were found to be within the normal ranges. He had another generalized tonic-clonic seizures with dilated pupils for few minutes, which was aborted with IV diazepam. Fifteen minutes later, he developed muscle stiffening with decorticate posturing, with bradycardia that required further anticonvulsants, sedation and rapid sequence intubation. He received IV hyperosmolar therapy (3% saline), dexamethasone, other measures to reduce the raised intracranial pressure (ICP). The patient was stabilized and transferred to the intensive care unit.
Urgent CT scan of the head revealed midline complex solid and cystic mass lesion compressing the third ventricle and causing obstructive acute hydrocephalus of both lateral ventricles, with differential diagnosis of craniopharyngioma on top of the list (Figure 1).Urgent external ventricular drain (EVD) was inserted in the right side of the head with its tip in the body of the right lateral ventricle, after which his bradycardia resolved (HR 86/min) (Figure 2). Hypothalamic-pituitary hormones function were assessed, which revealed thyroid and adrenal insufficiencies (Table 1).
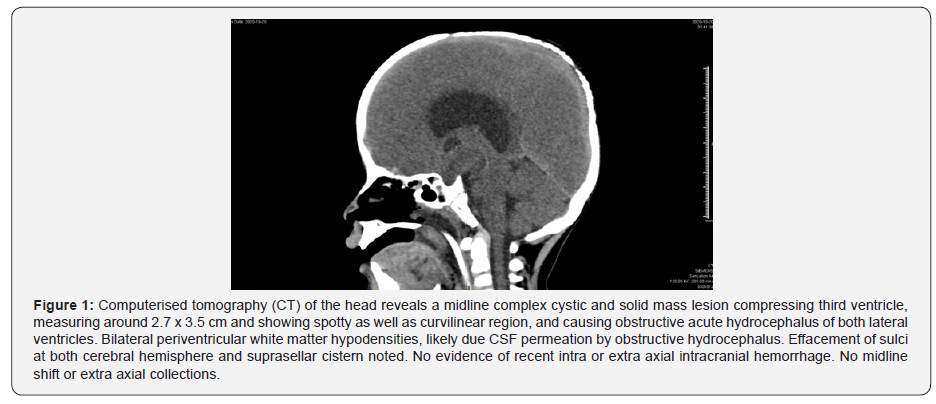
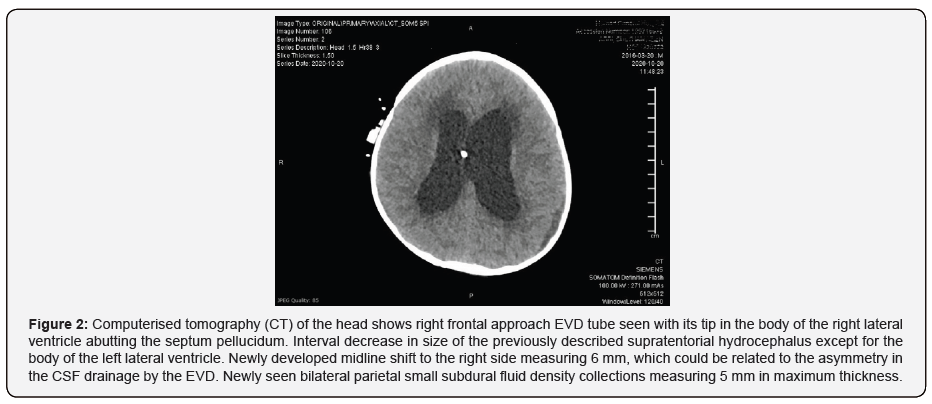
The patient was administered IV dexamethasone 2 mg every 6 hours and hypertonic 3% saline infusion for the initial 48 hours and kept on stress dose of hydrocortisone 7.5 mg every 6 hours for 1 week, followed by maintenance dose. On hospital day 3, his condition stabilized, off sedation with Glasgow Coma Scale of 15. His physical examination revealed a fully conscious and oriented child with no focal neurological deficits with normally reactive pupils, normal muscle power & tone and deep tendon reflexes.
Preoperatively, a magnetic resonance imaging (MRI) scan on the 3rd day of his hospital stay revealed a sellar and suprasellar likely adamantinomatous craniopharyngioma, retrochiasmatic with third ventricular extension. Right medial occipital area of focal parenchymal insult and a lumbar ventral epidural spinal lesion (Figure 3). On hospital day 4, debulking surgery of the lesion was performed via a subfrontal approach. Intraoperatively, the tumor was found to be large, rubbery mass displacing the chiasm superiorly. The patient underwent bifrontal craniotomy, subfrontal/anterior interhemispheric approach with debulking (90%) of sellar suprasellar tumor under neuronavigation. Smear preparations and frozen sections show large cellular fragments with basaloid features and cellular palisading forming, in many foci, a double cell layer. A relatively small amount of possible “wet keratin” is identified. The appearances are most likely those of an adamantinomatous craniopharyngioma.
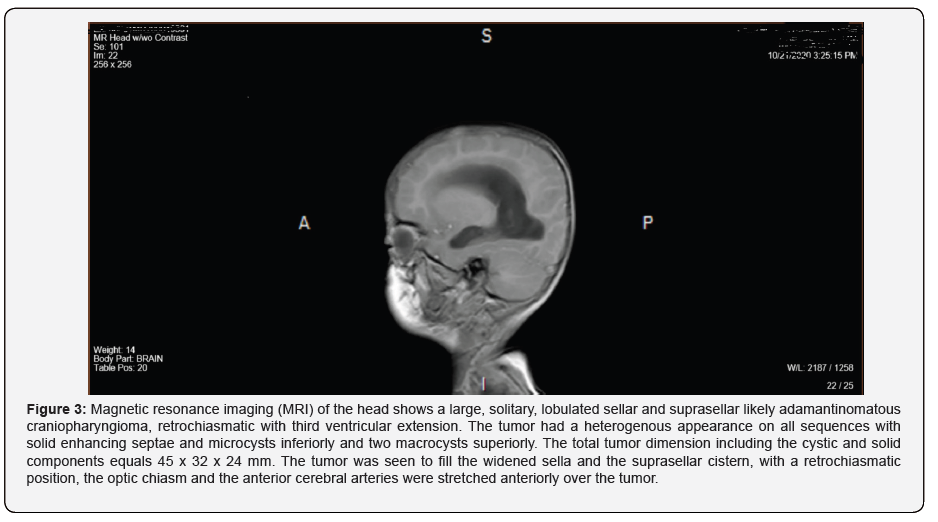
Postoperatively, the patient was noted to have right sided weakness and speech difficulty, requiring intensive rehabilitation programme, that has been resolved overtime. On follow‑up MRI, however, almost of the tumor area was found to be completely resected with an irregular non measurable possible residuum adherent to the posterior aspect of the optic chiasm and the right lateral wall of the third ventricle. On hospital day 8, hydrocephalus had resolved and EVD was removed. He also has had electrolyte abnormalities with sodium fluctuation, central diabetes insipidus, central adrenal insufficiency, central hypothyroidism and required prolonged hospital stay treatment with hormonal replacement therapy and fluid management. On hospital day 30, he was fully conscious, smart, interactive with remarkable improvement in his right sided weakness.
The patient was discharged home after one month of hospitalization in a stable condition to continue hormone replacement therapy, physiotherapy, occupational therapy, speech, and language therapy after educating the parents regarding his condition and plan of care. At the 3-month follow-up, he was in a good general condition.
Discussion
Craniopharyngiomas typically present with manifestations related to the compression of adjutant neurological structures [10]. The presenting manifestation of endocrine disorders are common (66 to 90%) in patients with craniopharyngioma. Signs and symptoms are usually present for prolonged duration before diagnosing the tumor, with an average of 9 to 24 months [11,12]. This generally allows enough time for detection and intervention before irreversible neurological deterioration.
Acute gastroenteritis remains a common cause of ED visits among pediatric population [13]. This is a rare case report of diagnosing craniopharyngioma while managing a young child with gastroenteritis. Craniopharyngiomas presenting with acute symptoms, although rare, are more frequently seen in children (13%) than adult patients [14]. Acute symptoms were defined as moderate or severe symptoms of abrupt onset occurring < 2 weeks before hospital admission, or sudden and severe worsening of pre-existing symptoms. Half of children with craniopharyngioma had hydrocephalus on presentation [14,15]. The IV fluid bolus of 0.9% saline used for rehydration of our patient may have contributed in decompensating and precipitating acute deterioration, which is a phenomenon that has been reported in another case of craniopharyngioma with increased ICP, leading to a rapid clinical deterioration due to acute brainstem herniation, with a fatal outcome [16].
Thyroid profile was evaluated earlier during his initial visits for constipation, 5 months prior to admission, and revealed borderline low T4 and normal TSH. Lately, during the admission when the craniopharyngioma was diagnosed, TSH and T4 were significantly decreased and consistent with central hypothyroidism. The slow growing nature of craniopharyngiomas may explain the gradual reductions of the thyroid function [17].
Although tumors located retrochiasmatically are associated with poorer outcomes, our patient has a good recovery at the three-month follow-up [18]. The fluctuations in medical, neurological, and neurobehavioral status should be anticipated throughout the lifetime, which makes the treatment for this type of tumor goes beyond the surgical excision [19]. This case report provides an acute presentation of a rare tumor which has got unmasked during the management of a patient with constipation and vomiting.
Conclusion
Gastroenteritis is one of the common complaints among paediatric population. We report a case of craniopharyngioma which got manifested during management of gastroenteritis in a pediatric patient. Unfolding an underlying brain tumor during the routine management of a common disease may be challenging. The patient improved following surgical removal of tumour and hormonal replacement therapy.
References
- Müller HL (2020) The diagnosis and treatment of craniopharyngioma. Neuroendocrinology 110(9-10): 753-766.
- Lubuulwa J, Lei T (2016) Pathological and topographical classification of craniopharyngiomas: a literature review. J Neurol Surg Reports 77: e121-e127.
- Daubenbüchel AMM, Müller HL (2015) Neuroendocrine Disorders in Pediatric Craniopharyngioma Patients. J Clin Med 4(3): 389-413.
- Huang C-C, Lin K-L, Wu C-T, Jung S-M, Wang C-J, et al. (2021) Clinical and Endocrinological Manifestations of Childhood-onset Craniopharyngioma Before Surgical Removal: A Report from One Medical Center in Taiwan. Pediatr Neonatol 62(2): 181-186.
- Khan RB, Merchant TE, Boop FA, Sanford RA, Ledet D, et al. (2013) Headaches in children with craniopharyngioma. J Child Neurol 28(12): 1622-1625.
- Müller HL, Merchant TE, Puget S, Martinez-Barbera J-P (2017) New outlook on the diagnosis, treatment and follow-up of childhood-onsetcraniopharyngioma. Nat Rev Endocrinol 13(5): 299-312.
- Asha MJ, Oswari S, Takami H, Velasquez C, Almeida JP, et al. (2020) Craniopharyngiomas: challenges and controversies. World Neurosurg 142: 593-600.
- Müller HL (2019) Management of endocrine disease: childhood-onset craniopharyngioma: state of the art of care in 2018. Eur J Endocrinol 180: R159-R174.
- Wijnen M, van den Heuvel-Eibrink, MM, Janssen JA, Catsman-Berrevoets CE, Michiels EM, et al. (2017) Very long-term sequelae of craniopharyngioma. Eur J Endocrinol 176(6): 755-767.
- Drapeau A, Walz PC, Eide JG, Rugino AJ, Shaikhouni A, et al. (2019) Pediatric craniopharyngioma. Childs Nerv Syst 35(11): 2133–2145.
- Müller HL (2018) Diagnosis and treatment of craniopharyngioma. Current Opinion in Endocrine and Metabolic Research 1: 29-35.
- Reddy GD, Hansen D, Patel A, Lin Y, Jea A, et al. (2016) Treatment options for pediatric craniopharyngioma. Surg Neurol Int 7: S174-S178.
- Hartman S, Brown E, Loomis E, Russell HA (2019) Gastroenteritis in Children. Am Fam Physician. 2019 Feb 1;99(3):159-165. Erratum in: Am Fam Physician 99(3): 159-165.
- Nielsen EH, Jørgensen JO, Bjerre PB, Andersen M, Andersen C, et al. (2013) Acute presentation of craniopharyngioma in children and adults in a Danish national cohort. Pituitary 16(4): 528-535.
- Chu CW, Su YF, LieuAS, Lin CL, Kwan AL, et al. (2017) Comparison study of clinical presentation and surgical outcome between children and adults with craniopharyngioma: a 22-year single-center experience in southern Taiwan. J Neurol Disord 5: 1e5.
- Weiss SL, Wegg-Uzunlar L, Bowman RM, Brannen ML (2011) Diagnosis of a craniopharyngioma after acute brainstem herniation in an emergency department. Pediatr Emerg Care 27(8): 747-750.
- Tan TSE, Patel L, Gopal-Kothandapani JS, Ehtisham S, Ikazoboh EC, et al. (2017) The neuroendocrine sequelae of paediatric craniopharyngioma: a 40-year meta-data analysis of 185 cases from three UK centres. Eur J Endocrinol 176(3): 359-369.
- Horn GJ, Lewis FD, Pepitone J (2017) Clinical challenges of craniopharyngioma: Neurobehavioral sequelae and complex outcomes. Neurol Disord Therap 1(2): 1-5.
- Guo Y, Wang Y, Ni M, Zhang Y, Zhong L (2019) Comparative evaluation of neuroendocrine dysfunction in children with craniopharyngiomas before and after mass effects are removed. J Pediatr Endocrinol Metab 32(2): 127e33.






























