Excellence in Primary Health Care for Children: The case of the North Alentejo Local Health Unit, Dr. José Maria Grande Hospital, Portugal
Brito Sílvio1*, Deolinda Pinto2 and Jerónimo Elsa3*
1 Departamental of Social Science Unit, Polytechnic Institute of Tomar, Portugal
2North Alentejo Local Health Unit, Urgence Service, Jose Maria Grande Hospital, Portugal.
3Sociology Research Center, ISCTE, Universitary Institute of Lisbon, Portugal
Submission: February 11, 2020; Published: February 28, 2020
*Corresponding author: Brito Sílvio, Social Science Departamental Unit, Polytechnic Institute of Tomar, Portugal
How to cite this article: Brito Sílvio, Pinto Deolinda, Jerónimo Elsa. Excellence in Primary Health Care for Children: The case of the North Alentejo Local Health Unit, Dr. José Maria Grande Hospital, Portugal. Acad J Ped Neonatol. 2020; 9(2): 555815. DOI: 10.19080/AJPN.2020.09.555815
Abstract
Background: Take care of children implies an enormous responsibility to families and essentially to health services that have the mission to care, prevent pathological consequences, and protect all childhood community. So the local health units are inprescindible for a search for excellence in this type of service.
Methods: Were observed, 19712 children, through the Manchester Screening System (MSS) and the Medical Specialties Chart of Jose Maria Grande Hospital, during the 2019 year, according to the database provided by the hospital, in order to decrease the use of urgency to take care the children and empower the primary health care and, undoubtedly, the quality of service.
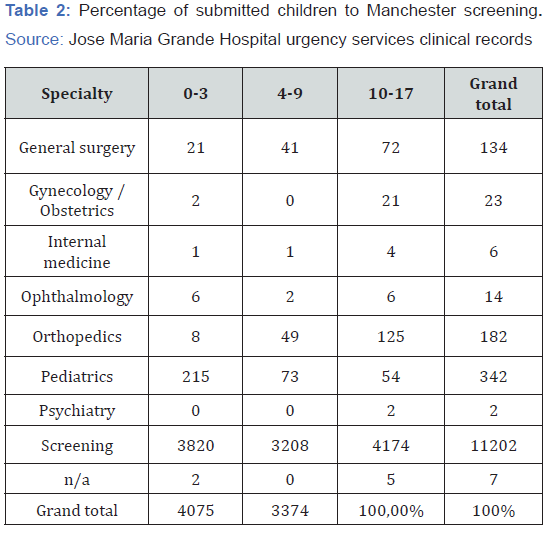
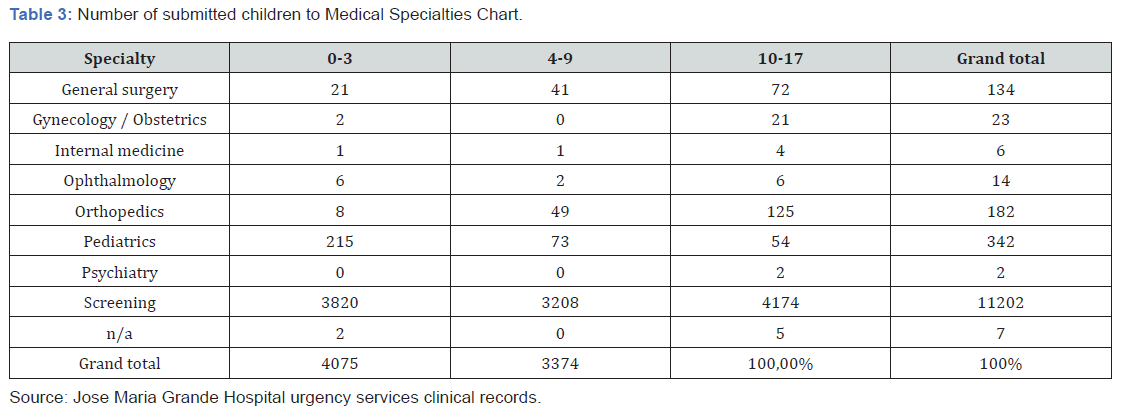
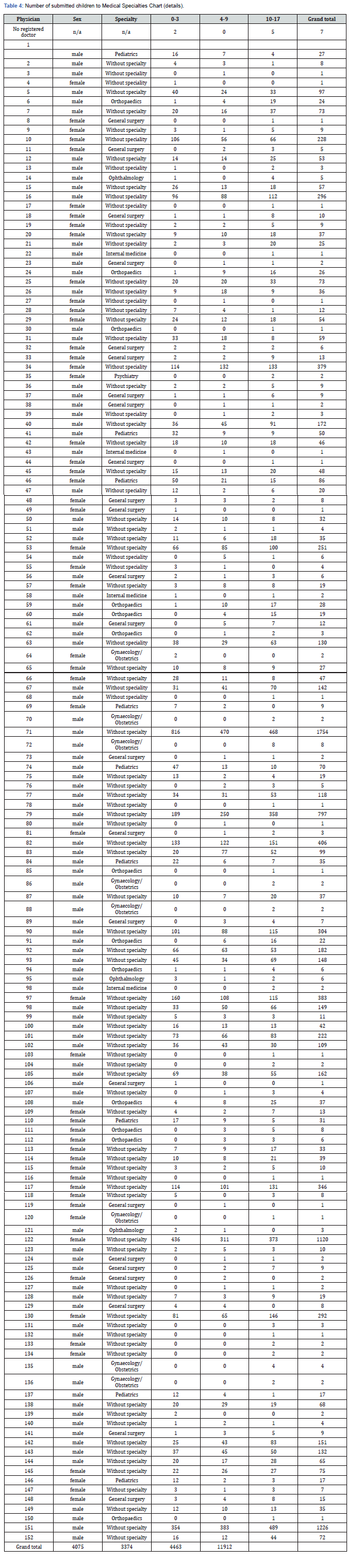
Results: The medical specialties chart shows that most children were discharged from the hospital, by the screening doctor and not by a specialist doctor. From 19712 children who attended the screening (without specialty) during 2019, only 7800 were observed and were discharged through the specialist doctor, that is only 11912 children had contact with an undifferentiated screening doctor.
Conclusion: The medical specialties chart showed that most children were discharged from the hospital by the screening doctor and not by a specialist. We could see that there is no need to resort to emergency services, as the primary care units are able to provide them to children, by not exposing them to unnecessary infections caused by waiting time in the hospital.
Keywords:Children; Primary health care; Screening; Specialties; Exposure; Urgency
Introduction
Preoccupation with the children is a prerogative to parents and health services in all the world and make part of the social cognitive influence on parents’ decision making and cognitive empowerment experience of medical staff [1]. Programs about this matter are diverse but with a high coherence level and transversal capacity, namely child abuse risk prevention [2] empowering and transforming health centres in wellness centres [3]. The primary health care is responsible for maternal and child health programs and for chronical disease attendance, based on a health state’s prevention and maintenance perspective, representing the first contact between families, citizens and health services [4]. For that, they build an important service, being strongly advised, its evolution and adaptation, in accordance with the population health characteristics and needs, over time [5]. The health centres have, as general objectives, ensure all population coverage health care in timely access [6] and health care maintenance valuing the relationship patient-doctor [7]. The primary health care is responsible for providing long-term care, with continuity and support at an individual and familiar levels [8] This continuity suggests a longitudinal relationship between patients and those who take care of them and are responsible about their preventive and coordinative care [9], noteworthy that this continuous and long term relationship, it’s fundamental to create trust between health professionals and patients and constitutes one of the great health care services advantages [10]. So, the health systems that ensure a good organization based on primary health care services are recognized for the present more satisfactory results, from citizens, to obtain more equity, health gains, and better health conditions [11].
Material and Methods
Several bacteria and fungus can cause nosocomial infections. These can be caused by acquired microorganisms from another person in the hospital (cross-infection) or been caused by the patient’s own flora (endogenous infection). Some microorganisms can be acquired trough inanimate objects or recently contaminated substances from another human source (environmental infection) [12]. This leads us to ask the following question:
a) There will be a need to expose children to increased risk of infection resorting to hospital emergency, with primary health care covering the entire hospital area.
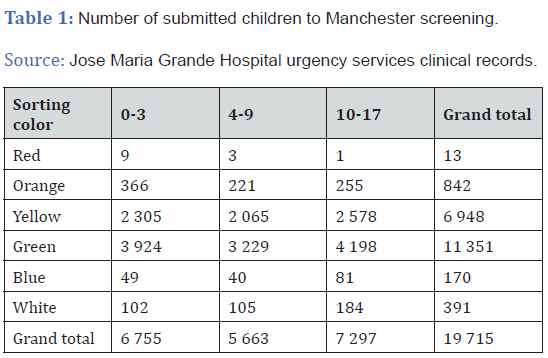
So, we proceed to observe all universe of children patients that recurred to Jose Maria Grande Hospital emergency services, and there were submitted to Manchester Screening and Medical Specialties Chart, during the year of 2019. This clinical record data was obtained by Alert Software System (ASS) used by the hospital urgency services. The Manchester Screening System (MSS) was implemented and developed in Manchester Hospital in 1997 [13], and its implementation and dissemination occurred in several countries, predominantly, in Ireland, Portugal, Span, Italy, Germany, Sweden Holland, Japan, and the Hong. Kong city. Portugal was adopted as national policy, in function in many hospitals since 2000, through Portuguese Triage Group (PTG) [14], with the support by Health Ministry, Physicians Order (PO), and the Nurses Order (NO). The MSS is a five priority categories scale (in Portuguese system six), developed by an emergency specialist multidisciplinary care group which category received a number and a name, and color, and a target time, for initial medical observation:
a) Emergent, red color, 0 minutes.
b) Very urgent, orange color, till 10 minutes.
c) Urgent, yellow color, till 60 minutes.
d) Little urgent, green color, till 120 minutes.
e) Not urgent, blue color, till 240 minutes.
f) Nothing urgent, white color, more than 240 minutes.
This method made the priority screening and identifies severity criteria, in an objective and systematized form that indicates a clinical priority with which the patient should be treated (based on identified problems) and the recommended time target till the beginning of the first clinical observation. It is not a question of establishing diagnoses. The Health Ministry, through 2nd February Dispatch n.º 1057/2015, determined that all health units who haven’t implemented the MSS should proceed to its implementation till 31st December 2015. We also used the ALERT software alert to extract the urgency of children’s clinical records. This software is used by the Portuguese National Health Service. The children arrived at pediatric urgency and the nurse, based on observation and verbalized complaints, in an objective and systematized form, used the MSS and inputted the color, being the children attended by a nonspecialty physician (screening physician).
Patients Children
Discussion
Reporting to data we see the following:
a) The green, white and blue screenings considered a not urgent situation with 120 to 240 minutes and more, if we see the percentual that sits above 59%.
b) The medical specialties chart translated to us that the majority of the patient’s children were discharged from the hospital by a screening physician hand, not by a specialist.
c) Reporting to the 19712 screening submitted children during the year of 2019, from these only 7800 were observed and discharged by a specialist physician, that is only 11912 had contact with a without specialty physician.
d) There`s no need to expose children to an unnecessary exposure risk once in the hospital area there are primary health services units that avoid hospital urgency services recurse.
The specialties that observed the children with green, blue, or white colors that went to urgency by indication of a specific physician, are those that they are in the specialty chart where it was verified that 11912 were discharged from the urgency through the screening physician and not through the specialist.
Conclusion
The Portuguese State, in the last decade, has led a reformat at Health Public Service Level with the objective to bring citizens closer to Health Centres in an attempt to relieve hospitals from the abnormal influx of users, reducing costs, and redirect resources to another more demanding types of health cares that cannot be delegated to Health Centres, in attempt to a health culture promotion proximity and continuity care. So, towards the Portuguese State investment on this health care delivery reformulation, it matters to know if the citizen’s behaviours followed the political option trend or, by the contrary, they still choose the hospitals. In this sense, it’s important to question us: What Portugal citizens choose with respect to child health care? The studied data reveal the answer to that question, the Portuguese don’t see each other in the political reformulation and still continuing to choose the hospital health care. Nevertheless, when they do, they subject the children to virus and bacteria contamination environment, superior to the environment in a health centre, if do not get care from specialist physicians, and if the literature doesn´t present any advantage evidence to this type of health answer, a derived question it matters: why the citizens still prefer the hospital health care, instead choose the health care in local health units? What there is in a hospital environment that conditions the citizens choose and what can be done to health policy will be a success in its implementation? If those citizens expectative who appeal to hospital, to access a child health care is pediatric, thus one of the reformative options can be the paediatric physician’s mobility through local health units. In the same form, the diagnosis of complementary means access also can condition the citizens to choose and, in this sense, on this type of service inclusion in local health units, can increase the citizen’s preference. Another option as “mentoring” or “telemedicine” could be equated, but this will be an open window for further investigations.
References
- Janicke David M, Finney Jack W (2003) Children's Primary Health Care Services: Social-Cognitive Factors Related to Utilization.J PediatrPsychol 28(8): 547-557.
- Leach T (2019) Featured counter-trafficking program: H.E.A.L.T.H. Clinic of Ottawa. Child Abuse Negl.
- Ved RR, Gupta G, Singh S (2019) India’s health and wellness centres: realizing universal health coverage through comprehensive primary health care. WHO SouthEast Asia J Public Health8(1):18-20.
- Hing E, Hooker RS, Ashman JJ(2011) Primary Health Care in Community Health Centres and Comparison with Office-Based Practice. J Community Health 36(3):406-413.
- PolitzerR, Regan J, Shi L, Starfield B, Xu J (2003) Primary care quality: community health centre and health maintenance organization. South Med J 96(8): 787-795.
- Mohamed EY, Sami W, Alotaibi A, AlfaragA, Almutairi A, et al. (2015) Patients’ satisfaction with primary health care centres’ services, Majmaah, Kingdom of Saudi Arabia. Int J Health Sci (Qassim) 9(2): 163-170.
- OseiFrimpong K (2016) Examining the effects of patient characteristics and prior value needs on the patient-doctor encounter process in healthcare service delivery.International Journal of Pharmaceutical and Healthcare Marketing 10(2): 192-213.
- Amado CA, dos Santos SP (2009) Challenges for performance assessment and improvement in primary health care: the case of the Portuguese health centres. Health policy 91(1): 43-56.
- Saultz JW (2003)Defining and measuring interpersonal continuity of care. Ann Fam Med1(3): 134-143.
- Arthur KC, Mangione-Smith R, Burkhart Q, Parast L, Liu H, et al. (2018)Quality of care for children with medical complexity: An analysis of continuity of care as a potential quality indicator. Acad Pediatr 18(6): 669-676.
- Gava GB, Dias H (2018) A reforma dos Cuidados de Saúde Primários: êxitos e desafios da experiência portuguesa. NAU Social 9(16): 19-39.
- DucelG, Fabry J, Nicolle L (2002) Prevention of hospital-acquired infections: a practical guide. Prevention of hospital-acquired infections: a practical guide.2nd
- Riley PA, Cooksey CJ, JohnsonCI, Land E J, LatterAM, et al. (1997) Melanogenesis-targeted anti-melanoma pro-drug development: effect of side-chain variations on the cytotoxicity of tyrosinase-generated ortho-quinones in a model screening system. Eur J Cancer 33(1): 135-143.
- Martins HMG, Cuña LDCD, Freitas P (2009)Is Manchester (MTS) more than a triage system? A study of its association with mortality and admission to a large Portuguese hospital. Emerg Med J26(3): 183-186.






























