Recurrent Late-Onset GBS Sepsis in the NICU
Charles M Roitsch, DO and Joseph B Philips III, MD*
Division of Neonatology, Department of Pediatrics, University of Alabama at Birmingham, USA
Submission: February 04, 2020; Published: February 12, 2020
*Corresponding author: Joseph B Philips III MD, Division of Neonatology, Professor of Pediatrics, University of Alabama at Birmingham, 176F Ste 9380 1700, 6th Ave South Birmingham, USA
How to cite this article: Charles M Roitsch, DO, Joseph B Philips III, MD. Recurrent Late-Onset GBS Sepsis in the NICU. Acad J Ped Neonatol. 2020; 9(1): 555812. DOI: 10.19080/AJPN.2020.09.555812
Abstract
We present a case series of three premature infants with aggressive late-onset GBS disease in the Neonatal Intensive Care Unit (NICU) requiring an additional course of antibiotics for long-term clearance of infection. This illustrates the association of late-onset GBS disease with serious illness and potential for resistance to initial treatment. We propose that treatment of late-onset GBS sepsis or meningitis with penicillin or ampicillin should be lengthened to at least a 21day course.
Keywords: Group B streptococcus; Late-onset sepsis; Penicillin; Ampicillin; Neonatology
Abbreviations: GBS: Group B streptococcus; NICU: Neonatal Intensive Care Unit; IAP: Intrapartum antimicrobial prophylaxis; DOL: Day of life; NGTD: No growth to date; CSF: Cerebrospinal fluid; VLBW: Very low birth weight (1000-1500g); ELBW: Extremely low birth weight (<1000 g); PTL: Preterm labor; NEC: Necrotizing enterocolitis
Introduction
Group B streptococcus (Streptococcus agalactiae, or GBS) is a gram positive coccus with significant pathological potential in the neonate and young infant causing bacteremia, pneumonia, meningitis and other systemic and focal infections. Intrapartum antimicrobial prophylaxis (IAP) for GBS has made a dramatic impact on vertical transmission of early-onset GBS disease in newborns. However, late-onset GBS disease (onset between 7-89 days) has remained unchanged, afflicting approximately 0.4 per 1000 births [1]. Among those infants with late-onset GBS disease, mortality is high (21.9% [2]). If an infant develops culture proven GBS sepsis or meningitis, the current recommendation is to treat with a 10 or 14day course of penicillin G, respectively. For late-onset GBS disease, penicillin (450,000 to 500,000 U/Kg/day) is the drug of choice, but ampicillin (300 mg/kg/day) is an appropriate alternative [3]. We present three premature infants with recurrent GBS disease despite treatment with a regimen deemed appropriate.
Case Reports
The infants presented initially with increased apnea and bradycardia events and/or respiratory distress requiring positive pressure ventilation. These general signs of worsening clinical status prompted an evaluation for sepsis and meningitis including blood and cerebrospinal fluid (CSF) cultures.
Case 1 (Table 1) was a male infant born at 30 weeks gestation who was diagnosed with late-onset GBS sepsis on day of life 24 and completed a 14-day course of ampicillin (300 mg/kg/day). One week later, he developed apneic events which prompted an infection workup that revealed GBS sepsis and meningitis. After a 21-day course with penicillin G (450,000U/kg/day) including 5 days of gentamicin (5mg/kg/day) for synergy, repeat CSF and blood cultures were negative. Culture of mother’s breast milk did not grow GBS.
Case 2 (Table 1) was a female infant born at 26 weeks gestation who developed late-onset GBS meningitis at day of life 12 and completed 21 days of ampicillin (300mg/kg/day). On the last day of treatment, CSF and blood cultures were obtained and had no bacterial growth. Subsequently, she developed recurrent GBS meningitis two weeks later and completed another 21 day course of ampicillin (300mg/kg/day). Repeat blood and CSF cultures were negative after the second course of treatment.Case 3 (Table 1) was a female infant born at 22 weeks gestation whose course was complicated by necrotizing enterocolitis with spontaneous bowel perforation on day of life 6 necessitating emergent peritoneal drain placement. Vancomycin, tobramycin and metronidazole provided antimicrobial coverage for 18 days, and these were discontinued after the peritoneal drain was removed. On Day of Life 47, respiratory decompensation prompted drawing blood cultures which grew GBS. CSF cultures grew Staphylococcus capitis, which was thought to likely be a contaminant from normal skin flora. 14days of ampicillin (300mg/kg/day) were completed for sepsis treatment. Two sets of blood cultures were obtained after completion of course and had no bacterial growth. On day of life 82, she developed abdominal distention and tachycardia. Lumbar puncture did not yield enough fluid for culture, but blood cultures grew GBS, so she then completed a 21 day course of ampicillin (initially started at 200mg/kg then increased to 300mg/kg on treatment day 6). Blood cultures after completion of antibiotics were negative. Mom’s breast milk was tested; no growth of GBS was identified.
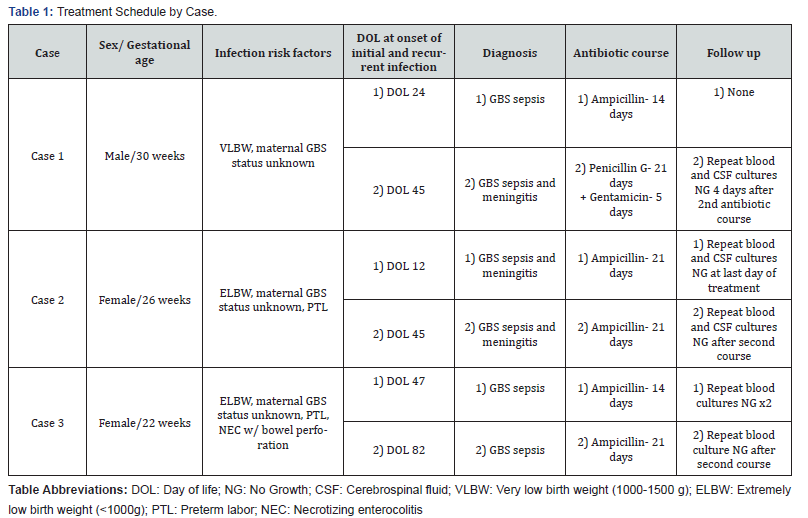
Case 3 (Table 1) was a female infant born at 22 weeks gestation whose course was complicated by necrotizing enterocolitis with spontaneous bowel perforation on day of life 6 necessitating emergent peritoneal drain placement. Vancomycin, tobramycin and metronidazole provided antimicrobial coverage for 18 days, and these were discontinued after the peritoneal drain was removed. On Day of Life 47, respiratory decompensation prompted drawing blood cultures which grew GBS. CSF cultures grew Staphylococcus capitis, which was thought to likely be a contaminant from normal skin flora. 14days of ampicillin (300mg/kg/day) were completed for sepsis treatment. Two sets of blood cultures were obtained after completion of course and had no bacterial growth. On day of life 82, she developed abdominal distention and tachycardia. Lumbar puncture did not yield enough fluid for culture, but blood cultures grew GBS, so she then completed a 21 day course of ampicillin (initially started at 200mg/kg then increased to 300mg/kg on treatment day 6). Blood cultures after completion of antibiotics were negative. Mom’s breast milk was tested; no growth of GBS was identified.
Conclusion
Late-onset sepsis (LOS) remains a serious illness in the NICU affecting approximately 25% of singleton very low birth weight (VLBW) infants [4,5]. Among those infants affected with LOS, approximately 28% will experience 2 or more episodes of sepsis after their initial infection [5]. GBS is responsible for about 2% of VLBW infant late-onset sepsis [4,5] and has a mortality rate of almost 22% [5]. Of those affected by GBS disease, approximately 50% have been shown to be directly related to maternal colonization [2]. Two of the three infants had their mother’s milk cultured for GBS revealing no growth. Therefore, even without culture proven evidence of GBS from breastmilk, infection can recur due to other means such as inadequate clearance of initial infection, continued colonization followed by invasive disease, and horizontal transmission. Our three premature infants with late-onset GBS disease were treated initially according to the current recommendations of GBS management. They had an adequate course of either penicillin or ampicillin and temporarily improved clinically. However, each infant developed recurrent sepsis and/or meningitis and were then treated successfully with a 21day course of antibiotics with long term clinical improvement [6]. We propose that the treatment of late-onset GBS sepsis or meningitis with penicillin or ampicillin should be lengthened to at least a 21day course, rather than the standard 14-21day course. Furthermore, an aminoglycoside can act synergistically and aide in GBS clearance, although treatment length has yet to be established[6]. Late-onset GBS disease can recur and proof of cure by blood and/or CSF cultures should be obtained post therapy [3]. Further research regarding treatment length and follow up of these infants is needed
Conflict of Interest
The authors declare no conflict of interest.
References
- Jordan HT, Farley MM, Craig A, Mohle-Boetani J, Harrison LH, et al. (2008) Revisiting the need for vaccine prevention of late-onset neonatal group B streptococcal disease: a multistate, population-based analysis. PediatrInfect Dis J 27(12): 1057-1064.
- Dillon HC Jr, KhareS, Gray BM (1987) Group B streptococcal carriage and disease: a 6-year prospective study. J Pediatr110 (1):31-36.
- (2015) Group B Streptococcal Infections. In: Kimberlin DW, Brady MT, Jackson MA, Long SS, eds. Red Book®: 2015 REPORT OF THE COMMITTEE ON INFECTIOUS DISEASES. American Academy of Pediatrics 745-750.
- BoghossianNS, Page GP, Bell EF, Stoll BJ, Murray JC, et al. (2013) Late-onset sepsis in very low birth weight infants from singleton and multiple-gestation births. J Pediatr 162(6):1120-1124.
- Stoll BJ, Hansen N, FanaroffAA, Wright LL, Carlo WA, et al. (2002) Late-onset sepsis in very low birth weight neonates: the experience of the NICHD Neonatal Research Network. Pediatrics110(2 Pt1):285-2
- SchaufV, DeveikisA, Riff L, SerotaA (1976) Antibiotic-killing kinetics of group B streptococci. J Pediatr 89(2):194-198.






























