Laryngeal Hamartoma Presenting as Congenital Stridor in Neonate: A Rare Entity
Nadzirah Dani1, Chian Yong Liu2, Yin Ping Wong3 and Bee See Goh1*
1Department of Otorhinolaryngology Head & Neck Surgery, Universiti Kebangsaan Malaysia Medical Centre, Malaysia
2Department of Anaesthesiology, Universiti Kebangsaan Malaysia Medical Centre, Malaysia
3Department of Pathology, Universiti Kebangsaan Malaysia Medical Centre, Malaysia
Submission: October 21, 2019; Published: October 31, 2019
*Corresponding author: Goh Bee See, Consultant Otorhinolaryngology, Department of Otorhinolaryngology and Head & Neck Surgery, Universiti Kebangsaan Malaysia Medical Centre (UKMMC), Kuala Lumpur, Malaysia
How to cite this article: Nadzirah Dani, Chian Yong Liu, Yin Ping Wong, Bee See Goh. Laryngeal Hamartoma Presenting as Congenital Stridor in Neonate: A Rare Entity. Acad J Ped Neonatol. 2019; 8(2): 555791.DOI: 10.19080/AJPN.2019.07.555791
Abstract
Hamartoma is uncommon to occur in the head and neck region, but it has been described. Laryngeal hamartoma is a rare entity to cause congenital stridor in neonate. A full term born neonate presented with stridor at birth which was aggravated upon on crying. Despite the child appeared to be not in respiratory distress, stridor noted on inspiration with suprasternal recession. Otherwise, child was breastfeeding well. Flexible nasopharyngolaryngoscopy demonstrated a pedunculated tubular mass at supraglottic region obstructing the airway during inspiration. We proceeded with direct laryngoscopy and excision in which the origin of the mass was confirmed to arise from ventricle. Histopathological examination was consistent of hamartoma. Laryngeal hamartoma should be kept in mind as one of the differential diagnosis in the case of congenital stridor despite its rare occurrence. Urgent assessment by otolaryngologist is mandatory. Complete excision of hamartomatous mass is crucial to provide airway and avoid recurrence.
Keywords:Hamartoma; Congenital stridor; Larynx; Benign tumour
Introduction
Stridor is high pitch musical sound which is produced as a result of turbulence of air when air flow through a narrowed space. Causes of paediatric stridor can be broadly classified into congenital or acquired and acquired can be further subclassified as febrile or afebrile cause. Most common cause of congenital stridor in neonate are laryngomalacia which accounts for 60% to 70% of cases, followed by vocal cord paralysis, laryngeal web, congenital subglottic stenosis, tracheomalacia and subglottic haemangioma [1]. Laryngeal hamartoma is a rare cause of congenital stridor. Hamartoma by definition, is a benign non-neoplastic lesion, composed of mixture of mature tissue elements that are endogenous to a particular site, but growing in a disorganised haphazard manner [2]. Most often sites of hamartoma development are in spleen, liver, lung, kidney or pancreas. Occurrence of hamartoma in the head and neck region is rare, but it has been described. Although uncommon, nasal cavity, paranasal sinus and nasopharynx are frequent site of hamartoma in head and neck region [3]. We herein report an unusual case of laryngeal hamartoma presenting as congenital stridor at birth.
Case report
A neonate who was born full term, presented with stridor at birth which was worsen with crying. There was no worsening of stridor on prone position. No cyanotic or choking episode was noted. The baby was otherwise breastfeeding well. Antenatal history was normal. It was an uneventful spontaneous vaginal delivery with birth weight of 3.37kg and Apgar score of 9/10 at 1 minute and 5 minutes. Postnatally, the baby had mild neonatal jaundice which resolved with phototherapy and not requiring neonatal intensive care unit admission. General examination revealed an active baby not in distress with good cry. There was suprasternal recession however no usage of other accessory muscle. Vital signs were all stable. Inspiratory stridor was audible and worsen with crying. Bedside flexible nasopharyngolaryngoscope showed a supraglottic pedunculated tubular mass partially obstructing the vocal cord. Bilateral vocal cord movement was normal. The baby was immediately posted for an examination under anaesthesia, direct laryngoscopy and excision of the mass. After adequate fasting time, the baby was induced with inhalational anaesthesia and muscle paralysis. Bagmask ventilation was initially uneventful but the airway became obstructed owing to the elongated mass that trapped itself into the larynx. By using endotracheal tube (ETT) size 3.0, the larynx was intubated by flipping the mass away with the ETT. Direct laryngoscopic examination showed a pedunculated and elongated supraglottic tubular mass, arising from the left ventricle
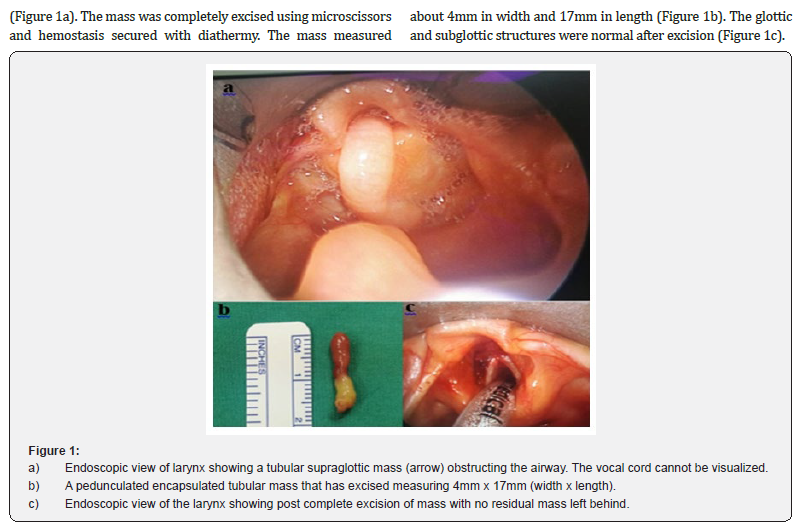

Histopathological examination of the ventricular mass revealed a well circumscribed polypoidal mass lined partly by nonkeratinising stratified squamous epithelium and respiratory type epithelium with underlying stroma (Figure 2a) composed of overgrowth of smooth muscle bundles, adipose tissue, blood vessels and seromucous glands that are haphazardly arranged (Figure 2b,2c). Final diagnosis of hamartoma is rendered. Post operatively, ETT was changed to size 3.5 and the baby was nursed in neonatal intensive care unit. The baby was subsequently extubated to nasal prong oxygen and was able to wean down to room air the following day. The baby was discharged well on post-operative day 2 with no immediate post-operative complications. Three months post excision, the baby was well with good weight gain to 3.8kg. No audible stridor heard. Flexible nasopharyngolaryngoscope was repeated at outpatient clinic and found no residual mass seen nor pooling of saliva.
Discussion
The term hamartoma is originated from the Greek word hamartánein first coined by Albrecht in 1904 which brings a meaning of “to go wrong” [3]. A hamartoma is a benign (noncancerous) tumour-like malformation which denotes a local developmental anomaly rather than a true neoplasm. Contrasting to true benign neoplasms, by definition, hamartomas are comprised of a mixture of mature cellular elements that are found in areas of body where abnormal growth occurs, but in a disorganised haphazard manner [4]. Laryngeal hamartoma was first described by Zapf et al in 1981 [5], in a 6-weeks old child presenting with stridor and sternal retraction [5]. The presentation of laryngeal hamartoma may varies from airway symptoms, feeding and swallowing symptoms, and failure to thrive. Systematic review by Windfuhr et al [6] reported only 26 cases of laryngeal hamartoma, among them 10 cases were in paediatric age group. Among those 10 paediatric cases, 3 of them presented in neonatal period with main presentation of stridor [6]. The other presentations include dysphagia, dyspnoea, hoarseness and choking episodes. Snoring as the main presentation was also documented. In this report by Noraziana Fadzilah et al [7], the location of hamartoma was at midline tongue base region and the mass was obstructing the oropharyngeal region [7]. Histologically, majority of laryngeal hamartomas are mesenchymal hamartoma which contains solely mesodermal elements (muscle, blood vessels and lymphoid cells) and lack epithelial components. Epithelial hamartoma, on the contrary, composed of not only the epithelial or glandular tissue but also the mesodermal components [3]. Hamartoma do not give rise to malignancy owing to the lack uncontrolled proliferation of the cell.
Other differential diagnosis of benign developmental lesions in the head and neck region among the paediatric age group are teratoma, choristoma, or epidermal cyst [3]. Epidermal cyst is usually superficially located ectodermal origin. Teratoma is a germ cell tumour that exhibit a mixture of mature and immature tissue elements derived from one or more germ cell layers. Choristoma or heterotopia, whereby is another form of developmental malformation where the abnormal proliferation of mature tissue elements are not indigenous to the site that they arise from [2]. As with other laryngeal lesion presenting as stridor, direct laryngoscopy should be performed for assessment of the origin and extent of tumour and to obtain biopsy for histopathological diagnosis. Hamartoma being a benign well encapsulated lesion can be completely excised with good prognosis in most cases. Rinaldo et all has observed a case of recurrence where incomplete excision adopted [8]. Surgical option include dissection using a micro laryngeal instruments or laser excision surgery. Zapf et al [5] has describe an interesting technique of using snare for removal of supraglottic lesion [5]. By far, none of the report describe a major post-operative complication except for one report a massive post-operative haemorrhage [9]. In conclusion, all congenital stridor needs endoscopic evaluation. Despite its rare occurrence, a physician should keep laryngeal hamartoma as one of the differential diagnosis. Complete excision provides a curative treatment with immediate relieve of stridor and good prognosis.
References
- Clark CM, Kugler K, Carr MM (2018) Common causes of congenital stridor in infants. JAAPA31(11): 36-40
- Kumar V, Abbas AK, Aster JC(2013) Robbins Basic Pathology. 9thEdn Elsevier.
- Leon Barnes (2001) Surgical Pathology of Head and Neck. 2ndEdn 1649-1668.
- Albrecht E (1904) Ueber hamartoma. Verhandlungen der DeutschenPathologischenGesellsc 7: 153-157
- Zapf B, Lehmann WB, Snyder GG 3rd (1981) Hamartoma of the larynx: an unusual cause for stridor in an infant. Otolaryngol Head Neck Surg 89(5): 797-799
- Windfuhr JP (2004) Laryngeal Hamartoma. Acta Otolaryngol 124(3): 301-308
- NorazianaFadzilah, Mawaddah Azman, Goh Bee See (2016) Congenital Midline Tongue Base Mass in An Infant: Lingual Hamartoma. J Clin Diagn Res 10(9): 01-03
- Rinaldo A, Minnara G, Fischer C, Ferlito A (1998) Hamartoma of the larynx: a critical review of the literature. Ann OtolRhinolLaryngol 107(3): 264-267
- Hosal AS, Hosal IN, Gungen Y, Onerci M (1998) Hamartoma of the larynx: a case of unusual bleeding after microlaryngoscopy. Ear Nose Throat J 77(11): 910-913






























