Neonatal Group B Streptococcal Sepsis: Retrospective Study from a Tertiary Level Hospital
Malak Al-Samnan and Zakariya Al-Salam*
Neonatal Medicine-Department of Pediatrics, Prince Sultan, Military Medical City, Saudi Arabia
Submission: September 10, 2016; Published: August 24, 2017
*Corresponding author: Zakariya Al-Salam, Neonatal Medicine-Department of Pediatrics, Prince Sultan Military Medical City, Postal Code: 11159, PO Box 7897, Riyadh-Saudi Arabia.
How to cite this article: M Al-Samnan, Z Al-Salam. Neonatal Group B Streptococcal Sepsis: Retrospective Study from a Tertiary Level Hospital. Acad J Ped Neonatol. 2017; 5(4): 555724. DOI: 10.19080/AJPN.2017.05.555724
Abstract
Background and objective:Group B Streptococcus (GBS) is one of the commonest pathogens that may lead to lethal neonatal sepsis. This can be prevented by screening and intrapartum antibiotic prophylaxis. However, maternal GBS screening is not practiced routinely in our hospital. Moreover, in order to implement such program, local data about the status of neonatal GBS infection is needed. The objective of this study was to estimate the prevalence of invasive early onset GBS infection, identify neonatal and maternal characteristics.
Methods:We conducted a retrospective review of our database, medical charts and laboratory results of all newborns and their mothers who were admitted to neonatal intensive care unit throughout the period of 2004-2012 at Prince Sultan Military Medical City, Riyadh, Saudi Arabia.
Results:Among 87246 live births, 9114 newborns were admitted to NICU. Fifty of them were diagnosed to have GBS invasive infection, five out borns were excluded. Therefore, the prevalence was estimated to be 0.52/1000 live births. The mean gestational age was 37±5 weeks, and mean birth weight of 2708±910 gm, 49% were males and 9% died before discharge. Thirteen percent of their mothers were carriers of GBS while the rest were not screened or tested negative. Respiratory complications were observed as follow: 18% respiratory distress syndrome, 9% pulmonary hemorrhage, 4%, persistent pulmonary hypertension, 2% bronchopulmonary dysplasia, 2% pneumothorax and 2% congenital pneumonia. In addition to antibiotics, the following treatments were given: surfactant (18%), inhaled nitric oxide (4%), postnatal dexamethasone (2%) and hypotension required treatment (16%). Patients spent mean of 4±10 days on mechanical ventilators, 5±12 days on CPAP and 7±20 days on oxygen.
Conclusion:GBS infection is not uncommon and can be lethal. Majority of mothers were not screened or negative. We recommend antenatal screening and intrapartum antibiotic prophylaxis.
Keywords:Early onset sepsis; Group b streptococcus; Morbidity
Introduction
Neonatal sepsis is a very common cause for admission in both term and preterm infants. Group B Streptococcal (GBS) infection is one of the most common causes of early-onset-sepsis. It may result in acute deterioration in the form of respiratory failure due to severe pneumonia, pulmonary hypertension that may even require ECMO. Severe cases are complicated by multi-organ dysfunction and ultimately death. Survivors may suffer from adverse neurodevelopmental sequalae [1-3].
Screening pregnant women for GBS colonization has been recommended with the ultimate goal to prevent neonatal GBS sepsis by identifying and providing intrapartum antibiotic prophylaxis for those at risk [4]. In our region, the practice of routine GBS screening and intrapartum prophylaxis is not consistently implemented. This may result in avoidable morbidity and mortality [5]. However, there is limited data from our region that address this very important infection in neonates in the first days of life (early-onset-sepsis). Therefore, we designed this study to review all patients who were admitted to our neonatal intensive care unit over 9-years period (2004-2012) due to early-onset invasive GBS infection. We also attempted to estimate the prevalence of GBS invasive infection and its complications.
Methods
This is a retrospective study of all neonates who were admitted to our Neonatal Intensive Care Unit (NICU) and diagnosed to have invasive GBS sepsis (positive blood or cerebrospinal fluid culture) between January 2003 and December 2012, Prince Sultan Military Medical City, Riyadh-Saudi Arabia. Our unit is considered a standard tertiary NICU and referral center as well. It is supported by various subspecialties including pediatric infectious diseases team. Out borns were excluded from the study to estimate the prevalence more accurately.
The diagnosis of invasive GBS was identified from our database that was collected over the years upon each patient discharge. Further information was collected from the maternal and neonatal files that included discharge and death summaries, mortality logbook, laboratory and imaging systems. From these we identified maternally and neonatal characteristics, GBS infection presentations, complications/co-morbidities and treatment.
The data were presented as mean±standard deviation and range (minimum-maximum) for continuous variables and frequency and percentage for categorical variables. Epi Info 3.4.3 was used for data collection while SPSS 20 for analysis.
Results
Among 87236 total live births in our hospital during 9 years, 9114 of them were admitted to NICU. Fifty of them were diagnosed to have GBS infection. We excluded 5 babies who were delivered outside our hospital. 38% were admitted from postnatal ward. Estimated prevalence was 0.52 per 1000 live births.
We noticed that the maternal age was presented in broad range (16-43 years old). The parity also ranged from primigravida to multipara. Thirty eight percent were delivered by cesarean section. Nine percent presented with prolonged rupture of membrane. Only 13% of them were known as GBS positive carrier and only 4% had received intrapartum antibiotic. Unfortunately, one IVF case was included. Seven percent were unbooked to our hospital.
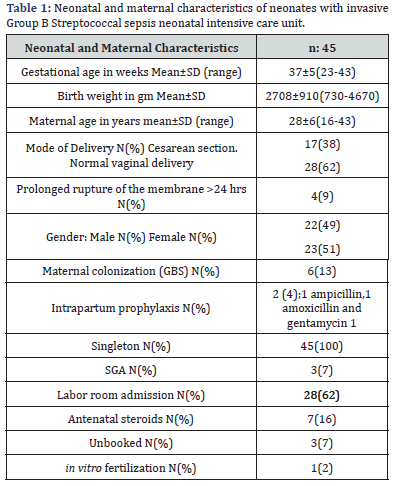
Mean gestational age was 37±5 weeks which was including extreme premature (23 weeks) and post-term (43 weeks). Mean birth weight was 2708±910 gm. Forty nine percent were males. The mortality was 9% (Table 1).
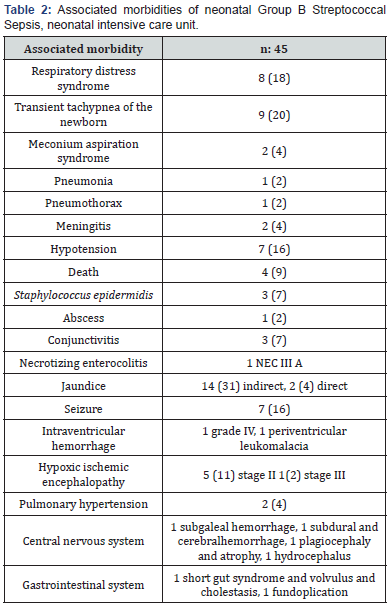
We noticed some association morbidities in a form of respiratory distress syndrome (18%), pulmonary hemorrhage (9%), persistent pulmonary hypertension (4%), bronchopulmonary dysplasia (2%), pneumothorax (2%) and congenital pneumonia (2%) (Table 2).
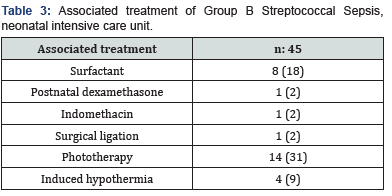
In addition to antibiotics, the following managements were provided: surfactant 18%, inhaled nitric oxide 4%, postnatal dexamethasone 2%, hypotension required treatment 16%. Babies spent mean of 4±10 days on mechanical ventilation, mean of 5±12 days on CPAP and 7±20 days on oxygen supplement (Table 3).
Discussion
Early onset neonatal sepsis in our hospital is not uncommon. The prevalence of 0.52 per 1000 could be explained by high number of deliveries in our hospital. There was high mortality among GBS infected babies (9%). As 13% of mothers were GBS positive, most of pregnant women were not screened or GBS negative. The explanation of this is that there is lack of awareness about the prevalence and seriousness of this infection among healthcare staff and pregnant women. Also absence of solid policy for prevention in our hospital. As the prevalence of early GBS infection in our hospital is exceed internationally published reports, serious measures have to be undertaken to tackle this issue including: antenatal screening and intra-partum antibiotic prophylaxis, screen all mothers at 35-37 weeks gestation and administer intra-partum prophylaxis accordingly and based on risk factors if screening was not done [6-8] or not available and to establish educational campaign about GBS sepsis for healthcare providers and mothers [9].
This study has some strength and weakness aspects. It depends on large database and probably the first in the country and Gulf Countries. It is limited to inborns. However, it is a retrospective study and some patients could have been missed or not diagnosed or presented to emergency department or other hospitals. In addition, we couldn’t find the type of bacterial serotyping which can be consider as infirm.
Conclusion
GBS sepsis is not uncommon in our health facility in Riyadh. Majority of mothers were not screened or negative and not received intrapartum prophylaxis and GBS sepsis was associated with significant mortality and major cardio-respiratory morbidities. We recommend antenatal screening and intrapartum antibiotic prophylaxis according to the result of screening or risk factors.
References
- Stoll BJ, Hansen NI, Sánchez PJ, Faix RG, Poindexter BB, et al. (2011) Early onset neonatal sepsis: the burden of group B Streptococcal and E. coli disease continues. Pediatrics 127(5): 817-826.
- Phares CR, Lynfield R, Farley MM, Mohle-Boetani J, Harrison LH, et al. (2008) Epidemiology of invasive group B streptococcal disease in the United States, 1999-2005. JAMA 299(17): 2056-2065.
- Almuneef M, Alalola S, Ahmed S, Memish Z, Khan MY, et al. (2000) The Changing Spectrum of Group B Streptococcal (GBS) Infection in Infants of Saudi Arabia. J Chemother 12(1): 48-52.
- Porta K, Rizzolo D (2015) Preventing group B streptococcal infections in newborns. JAAPA 28(3): 24-29.
- Heath PT, Balfour GF, Tighe H, Verlander NQ, Lamagni TL, et al. (2009) Group B streptococcal disease in infants: a case control study. Arch Dis Child 94(9): 674-680.
- Schuchat A, Oxtoby M, Cochi S, Sikes RK, Hightower A, et al. (1990) Population-based risk factors for neonatal group B streptococcal disease: results of a cohort study in metropolitan Atlanta. J Infect Dis 162 (3): 672-677.
- Polin RA, Committee on Fetus and Newborn (2012) Management of neonates with suspected or proven early-onset bacterial sepsis. Pediatrics 129(5): 1006-1015.
- Puopolo KM, Draper D, Soora Wi, Newman TB, Zupancic J, et al. (2011) Estimating the probability of neonatal early-onset infection on the basis of maternal risk factors. Pediatrics 128(5): e1155.
- Ahmadzia HK, Heine RP (2014) Diagnosis and management of group B streptococcus in pregnancy. Obstet Gynecol Clin North Am 41(4): 629- 647.






























