Positive Impact of Ultrasound In Management of Acute Appendicitis In Children
Raffaele Alessandro1* and Parigi Gian Battista2,3
1Department of Pediatric Surgery Unit, IRCCS Policlinico “S.Matteo”, Italy
2 Faculty of Pediatric Surgery Unit, Parigi Gian Battista, FEBPS, University of Pavia and IRCCS Policlinico “S.Matteo”, Italy
Submission: May 05, 2017; Published: August 04, 2017
*Corresponding author: Raffaele Alessandro, Department of Pediatric Surgery Unit, University of Pavia, UOC Chirurgia Pediatrica Fondazione IRCCS Policlinico “S.Matteo” Viale Golgi 1927100 Pavia, Italy.
How to cite this article: Raffaele A, Parigi G B. Positive Impact of Ultrasound In Management of Acute Appendicitis In Children. Acad J Ped Neonatol. 2017; 5(3): 555720. DOI: 10.19080/AJPN.2017.05.555720
Abstract
The impact of Ultrasound Scan (US) in the diagnosis of suspected acute appendicitis directly at presentation in the Emergency Department has been reviewed. Out of 327 patients assessed for acute abdominal pain, 145 (44,4%) were examined also with US. A total of 154 patients underwent surgery, of which 67 (43,6%) after US scan and 87 (56,4%) with no US. Differences in surgical timing and procedure, histologic findings and length of stay in the two groups were analyzed. In the US group the time gap between first examinations in ED to surgical intervention almost halved; operative time was shorter and total length of stay reduced. Our study confirms the highly positive value of US evaluation in the initial assessment of abdominal pain in children.
Keywords: Acute Appendicitis, Ultrasound, Early Diagnosis, ED Assessment
Objective
Acute appendicitis presents with a cohort of symptoms sometimes of difficult interpretation [1]. Variations in the appendix position, patient’s age and degree of inflammation make clinical presentation of appendicitis somewhat inconsistent, while an accurate diagnosis is mandatory to avoid complications from an inappropriate or delayed surgical management. It has been demonstrated that a diagnostic approach based only on history and clinical examination leads to an unacceptably high percentage of negative appendectomy rate (between 9.2% and 35%) [2,3]. Clinical signs as McBurney, Rovsing and Blumberg are not always present, and sometimes are not of any help; the same applies also for laboratory tests.
Imaging modalities were therefore developed to increase diagnostic accuracy: according to some Authors, CT is the most sensitive and specific method to investigate the presence of acute appendicitis [4]. However, pediatric patients are particularly sensitive to ionizing radiation and 30% of all pediatric CT examinations are unlikely to benefit the individual or could be easily and effectively replaced by a non-ionizing imaging technique [5]: among them, UltraSonography (US) has gained more and more momentum [6,7], but its overall impact is not always properly appreciated. In our study we tried to quantify the impact of US in the diagnosis and general management of acute appendicitis in children.
Materials and Methods
Medical records of 327 children(188 males, 139 females, M:F ratio 1:0.7) referred to the Pediatric Emergency Department(ED) of ”S.Matteo” Research Hospital between 1st January 2013 and 31st December 2014 for abdominal pain and suspected appendicitis were retrospectively reviewed.
182 patients (55.6%; M:F ratio 1:0.4) underwent clinical evaluation only, while in 145 children (44,4%; M:F ratio 1:1.3) clinical evaluation was integrated with an abdominal US examination performed directly in the ED. In no cases CT scan was performed. Decision to integrate clinical and laboratory diagnosis with US imaging in the ED was related to confuse clinical picture at admission or relapsing abdominal pain. Higher risk of ovarian pathology suggested a more generous utilization in girls, while in boys with a clear-cut clinical and laboratory picture US was usually deemed unnecessary for the diagnosis.
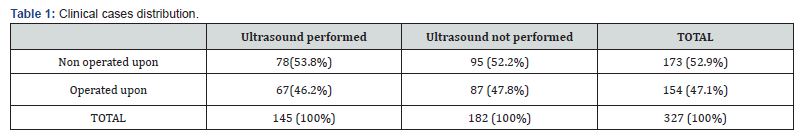
In the non-US group 95children (52,2%) were sent home, while 87 (47,8%), admitted for further examinations, were thereafter operated upon. In the US group 78 children (53,8%) were sent home, while 65(44,8%) turned out to be positive for acute appendicitis and immediately operated upon. In the remainder 2 cases (1,4%) diagnosis was still uncertain after US and children were operated only one day after. These data are summarized in Table 1.
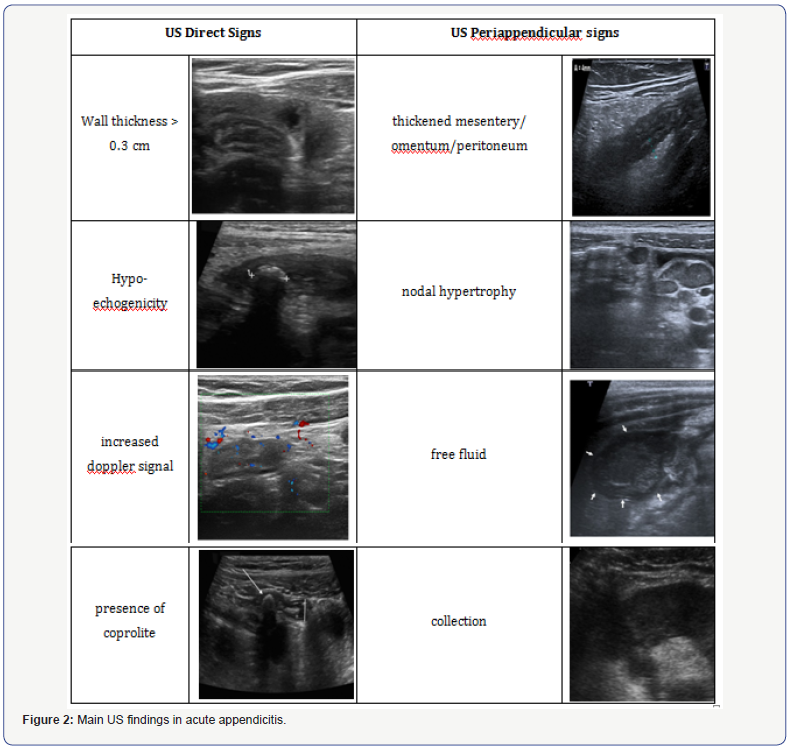
In 56 out of 65 US positive cases (86,1%)the scan showed direct signs of appendicular inflammation, namely wall thickness >0.3 cm, hypo-echo genicity, increased Doppler signal and/or presence of a coprolite; in the remainder 9 cases (13,9%) appendix was not appreciable, but periappendicular signs as thickened mesentery, nodal hypertrophy and free fluid or collection were present.
The study was then conducted on the two groups of patients undergoing appendectomy, those not examined with US (87 children) and those examined with US (67 children), comparing for each group surgical timing and procedure, histopathology findings, total length of stay.
Chi-square analysis was utilized to compare results.
Results
Surgical timing
Delay between ED evaluation and entrance in the operating room (ED-ORΔT) was 442±297’ for US group and 815±742’ for non-US group (p <0.0001).
Operative room time (OR ΔT) – calculated as time elapsed from the entrance in the OR to the end of the anesthesia awakening phase- was 93±28’ for the US group and 109±41’for the non-US group (p<0.003). Duration of surgery (from initial incision to skin suture) turned out to be 61±27’ for the US group and 72±36’ for the non-US group (p=0.04).
Surgical procedure
Primary surgical approach utilized in all 154 operated cases was Trans Umbilical Laparoscopic Assisted Appendectomy (TULAA). In 126 cases (81,8%) appendectomy was performed without need to conversion (51.6% US group, 48.4% non-US). In 20 cases (13.0%; 2 in US group, 18 in non-US group) a conversion to multi-trocar laparoscopy was required, while in the remainder 8 cases (5.2%, all non-US group; p<0.0001) conversion to open appendectomy was needed. Intra operative conversion rate was therefore 3.0% in the US group and 30.2% in non-US group. No further intra operative complications were recorded in both groups.
Postoperative period
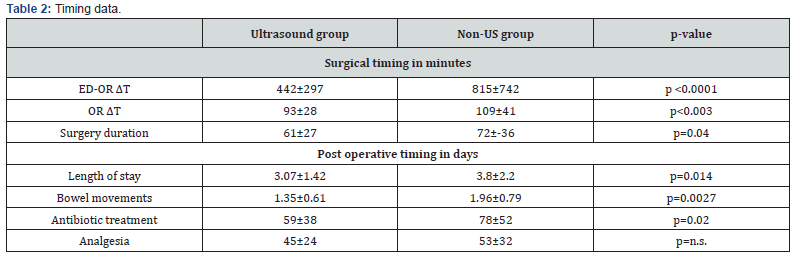
Postoperative length of stay in the ward was 3.0±1.4 days in US group vs 3.8±2.2 days in non-US group (p=0.014).Bowel movements appeared 1.35±0.61 days in US group and 1.96±0.79 days in non-US group (p=0.0027). Antibiotic therapy was administered for 59±38 hours in US group and for 78±52 hours in non-US group (p=0.02), while analgesia respectively for 45±24 hours and 53±32 hours. Timing data are summarized in Table 2.
Histopathology
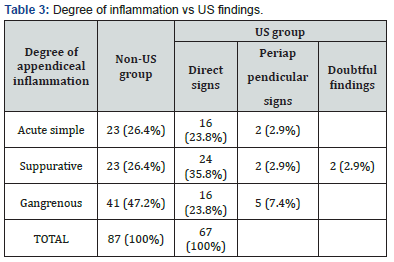
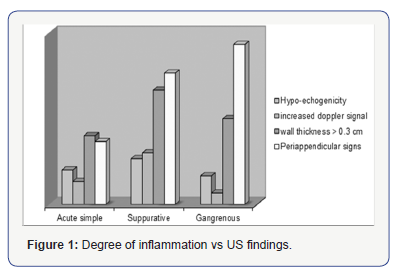
Relative incidence of degree of inflammation vs US signs is summarized in Table 3 and illustrated in Figure 1
Histopathology examination showed higher prevalence of gangrenous appendicitis in non-US vs US group (47.2% vs 31.2%). 17 out of the 154 operated cases (11.0%) showed histological diagnosis of chronic or exacerbation of chronic appendicitis, with hyperplasia of the mucosa-associated lymphoid tissue and signs of fibrin-granulocyte. Comparing histology with US findings, when direct signs were present appendicitis was in most cases suppurative, while the presence of periappendicular signs–even if the appendix was not identifiable - was related to a higher prevalence of gangrenous appendicitis. Main US patterns are depicted in Figure 2.
Discussion
Acute appendicitis diagnosis can be challenging, but nevertheless an accurate diagnosis is mandatory for the proper surgical management to avoid complications. Even if abdominal pain is nearly a universal symptom, it may be difficult to assess in very young children; older children can give a history of their illness, toddlers and young school-aged children need a caregiver to communicate their history and this may not necessarily be accurate, because each caregiver may have a different perspective on the condition of the child [8]. Clinical findings in acute appendicitis may vary a lot showing a fair to moderate interrater reliability [9], hence the need of a more reliable imaging diagnostic tool.
Comparing the diagnostic performances of both US and CT scan for the diagnosis of appendicitis, Doria et al. reported sensitivity and specificity of US in children at around 88% and 94% respectively, while the pooled sensitivity and specificity for CT in children was 94% and 95% [4]. A recent study by Elikashvili et al. showed a 60% sensitivity of bedside ultrasound in pediatric appendicitis (95% CI=46% to 72%) and a specificity of 94% (95% CI=88%to 97%) [10]. In some other series, slightly higher sensitivity of 83% was reported [11,12]. Despite this very high accuracy in detecting appendicitis, CT carries some nonnegligible problems, particularly in children: actually, interest in emphasizing the risks of ionizing radiations is increasing [13], thus increasing as well the interest given to the US-assisted diagnosis of appendicitis [14] that prompted us to perform this study.
Main criticism that can be moved to it is the lack of a formal randomization of children to be submitted to US in the ED. On the other hand - once accepted some bias such as the wider adoption of US in girls- the relatively long span of time in which the study was performed, the variety of clinical pictures and of clinicians examining children suffering of abdominal pain and requesting an US in a 24/7 ED inflow, allow to consider our series sufficiently randomized, although informally
Or study confirmed that adoption of US as a ED diagnostic tool allows a faster diagnostic workup and management: actually, US examined children underwent surgery in half of the time needed in non-US patients. This resulted also in shorter duration of surgery and in faster discharge from the hospital.
The first consequence of a decreased ED-OR ΔT after US evaluation turned out to be a significant reduction in the length of surgery , as a consequence of a shorter pre-operative time interval resulting in a lower incidence of conversions, typically ensuing a long-lasting inflammatory process. Post-operative length of stay as well was significantly shorter in US group as a result of the virtuous cycle triggered by a faster diagnosis and a faster indication to surgery, ultimately resulting in a timely interruption of the inflammatory process.
Moreover, false negative ratio after an US assessment was practically nil, with none of the children discharged undergoing surgery in the following two years.
Conclusion
Our study allows to conclude supporting the concept that, given the described unquestionable benefits, US should be employed in a widespread manner in the initial assessment of all children presenting with suspected acute appendicitis, directly in the ED, being a useful device able to differentiate between common causes of abdominal pain in children and thus expediting an appropriate clinical management [15].
References
- Becker T, Kharbanda A, Bachur R (2007) A typical clinical features of pediatric appendicitis. Acad Emerg Med 14(2): 124-129.
- Chandrasegaram MD, Rothwell LA, An El, Miller RJ (2012) Pathologies of the appendix: a 10-year review of 4670 appendicectomy specimens. ANZ J Surg 82(11): 844-847
- Seetahal SA, Bolorunduro OB, Sookdeo TC, Oyetunji TA, Greene WR, et al. (2011) Negative appendectomy: a 10-year review of a nationally representative sample. Am J Surg 201(4): 433-437.
- Doria AS, Moineddin R, Kellenberger CJ, Epelman M, Beyene J (2006) US or CT for Diagnosis of Appendicitis in Children and Adults? A Meta- Analysis. Radiology 241(1): 83-94.
- Larson DB, Rader SB, Forman HP, Fenton LZ (2007) Informing parents about CT radiation exposure in children: it’s OK to tell them. AJR Am J Roentgenol 189(2): 271-275.
- Marin JR, Lewiss RE American Academy of Pediatrics, Committee on Pediatric Emergency Medicine; Society for Academic Emergency Medicine, Academy of Emergency Ultrasound; American College of Emergency Physicians, Pediatric Emergency Medicine Committee; World Interactive Network Focused on Critical Ultrasound (2015) Point-ofcare Ultrasonography by pediatric emergency medicine Physicians. Pediatrics 135(4): 1113-1122.
- Russell WS, Schuh AM, Hill JG, Hebra A, Cina RA, et al. (2013) Clinical practice guidelines for pediatric appendicitis evaluation an decrease computed tomography utilization while maintaining diagnostic accuracy. Pediatr Emerg Care 29(5): 568-573.
- Bundy DG, Byerley JS, Liles EA Perrin EM, Katznelson J, et al. (2007) Does this child have appendicitis? JAMA 298(4): 438-451.
- Kharbanda AB, Stevenson MD, Macias CG, Sinclair K, Dudley NC,et al. (2012) Interrater reliability of clinical findings in children with possible appendicitis. Pediatrics 129(4): 695-700.
- Inna Elikashvili DO, Ee Tein Tay, James W. Tsung (2014) The Effect of Point-of-care ultrasonography on Emergency Department Length of Stay and Computed Tomography Utilization in Children With Suspected Appendicitis. Academic Emergency Medicine 21(2): 163-170.
- Sivitz AB, Cohen SG, Tejani C (2014) Evaluation of acute appendicitis by pediatric emergency physician sonography. Ann Emerg Med 64(4): 358-364
- Zielke A, Hasse C, Sitter H, Kisker O, Rothmund M (1997) Surgical ultrasound in suspected acute appendicitis. Surg Endosc 11(4): 362-365
- Pearce MS, Salotti JA, Little MP, McHugh K, Lee C, et al. (2012) Radiation exposure from CT scans in childhood and subsequent risk of leukaemiaand brain tumours: a retrospective cohort study. Lancet 380(9840): 499-505.
- Mittal MK, Dayan PS, Macias CG, Bachur RG, Bennett J, et al. (2013) Performance of ultrasound in the diagnosis of appendicitis in children in a multicenter cohort. Acad Emerg Med 20(7): 697-702.
- Sanchez TR, Corwin MT, Davoodian A, Stein-Wexler R (2016) Sonography of Abdominal Pain in Children: Appendicitis and Its Common Mimics. J Ultrasound Med 35(3): 627-635.






























