Screening for Retinopathy of Prematurity in Neonatal Unit - An Experience of a Tertiary Care Hospital in Bangladesh
Liton Chandra Saha1*, Md Mahbubul Hoque1 Dipak K Nag2 and MAK Azad Chowdhury1
1Department of Neonatal Medicine, Bangladesh Institute of Child Health, Bangladesh
2Department of Vitreo-Retina, National Institute of Ophthalmology & Hospital, India
Submission: January 23, 2017; Published: February 23, 2017
*Corresponding author: Dr. Liton Chandra Saha, Assistant professor, Department of Neonatal Medicine, Bangladesh Institute of Child Health (BICH), Dhaka Shishu (Children) Hospital, Sher-e-Bangla Nagar, Dhaka- 1207, Bangladesh, Email: sahaliton11@gmail.com
How to cite this article: Liton C S, Md Mahbubul H, Dipak K N, MAK Azad C. Screening for Retinopathy of Prematurity in Neonatal Unit - An Experience of a Tertiary ertiary Care Hospital in Bangladesh. Acad J Ped Neonatol. 2017; 3(3): 555612. DOI: 10.19080/AJPN.2017.03.555612
Abstract
Background: Retinopathy of prematurity (ROP) is a leading cause of childhood preventable blindness. Improved survival of preterm neonates has increased the incidence of retinopathy of prematurity (ROP).
Purpose: To determine the incidence of retinopathy of prematurity (ROP) in Neonatal Unit of a Dhaka Shishu (Children) Hospital (DSH) and assess the treatment requirements of these cases.
Materials and method: A ROP prospective screening survey was performed enrolling preterm neonates with a gestational age of 34 weeks or less and a birth weight of 1800 gram or less admitted to the SCABU and NICU of Dhaka (Shishu) Children Hospital from July 2013 to July 2014. Retinal evaluation was done by indirect ophthalmoscope and ROP was classified as type 1, type 2, APROP and retinal detachment (RD) groups. Infants who were found type 1 ROP, APROP (Aggressive posterior ROP) and RD were assigned for treatment.
Results: A total of 100 babies retinal evaluation were done. Among them 35 babies 70 eyes (35%) were found to have ROP (27 eyes 13.5% type1, 4 eyes 2.0% APROP, 5 eyes 2.5% retinal detachment and 34 eyes 17.0% were type 2). During the first screening 9 eyes had type 1, 52 eyes had type2, 4 eyes had APROP and 5 eyes were found to have retinal detachment. In the subsequent follow up another 18 eyes progressed to type 1 ROP from the type 2 group. In regards to treatment, 19 (52.8%) eye received laser, 10 (27.8%) eyes had received both laser and intra vitreal avastin, 2 eyes (2.6%) has got only intra vitreal avastin and 5 (13.9%) were advised for surgery.
Conclusion: The incidence of ROP is high in premature infants and more common in babies with gestational age less than 30 wks. Management of treatable ROP is also a time demanding issue.
Keywords: Retinopathy of prematurity (ROP); Prematurity; Incidence; Treatment; Bangladesh
Introduction
Retinopathy of prematurity (ROP) is a disease of low birth weight and premature infants, in which the retinal blood vessels fail to develop properly. This may result in rapidly progressive ocular abnormalities and causing childhood blindness from retinal detachment, macular dragging, strabismus and refractive error [1-4] with recent advances of care of very low birth weight infants, ROP is a serious problem among newborn babies. ROP may resolve without treatment by itself or can cause complications like moderate to severe visual impairments [5,6]. Preventive measurements are the best treatment, if disease occurs; it should be follow up very closely. The reported incidence of ROP in different regions of the world may varies from 10 to 46% among the low birth weight premature infants [7-9]. It seems that the incidence of this disease is quite high in premature infants in many countries [10]. Today, the survival rates for premature infants with low birth weight are improved. The prevention of disabling the disease is highly significant [11]. Several investigations have been carried out to follow up parents, meticulous neonatal care; screening and early treatment can reduce disability from this disease [10,12].
Earlier the Cryotherapy for Retinopathy of Prematurity (CRYOROP) demonstrated the decrease of incidence of adverse structural outcome and severe visual loss by 50% and latter on laser photocoagulation showed significantly better structural outcomes and visual function than Cryotherapy. At present anti vascular endothelial growth factors (Anti-VEGF) is also found an effective modality of treatment [13, 14].
Children of premature deliveries and low birth weights do not born with ROP. We know the natural history of ROP and we have effective treatment to prevent blindness from it. As such, ROP screening is now recommended by many international bodies [15]. Once upon a time ROP was the disease of developed countries but at present with the improvement of neonatal care in the developing countries most of the premature and low birth weight babies survived causing the risk of developing ROP and hence childhood blindness.
Despite its importance, very little data regarding the incidence as well as treatment requirements are available for future planning. The goals of this article are to report the incidence of ROP in a tertiary neonatal care center and to determine treatable cases to aware the health care professionals to address this issue in Bangladesh,
Materials and Methods
As part of the continuous ROP screening program at the neonatal Intensive care unit (NICU) and SCABU of Dhaka Shishu (Children) Hospital, we reported here those from July 2013 to July 2014 on first 100 babies, with a gestational age of 34 weeks or less and birth weight of 1800 gram or less. Babies with gestational age >34 weeks or birth weight >1800 gms were excluded from the study. Retinal evaluation was done by a ROP screening group headed by Dr. Dipak Kumar Nag, Department of Vitreo-Retina of National Institute of Ophthalmology and Hospital. ROP screening was done using indirect ophthalmoscope and 20D condensing lens after dilatation of commercially available eye drop which contained 0.8% tropic amide and 5.0% phenyl ephrine. ROP was classified as type 1, type 2 and APROP (Aggressive posterior ROP) groups.
Infants who were found type 1 ROP assigned for laser therapy. In case of APROP where laser can be applied satisfactorily was given laser, otherwise laser and intra vitreal avastin both were given simultaneously. However in some situation where pupil was not well dilated or fungus could not be visualized clearly due to vitreous haziness or in most posterior situations, only intra vitreal avastin was given as a rescue treatment. In cases with stage 4b and 5, vitrectomy was advised. First screening was done within the 30 days of birth but those came after that were also included in the study. Laser (double frequency Nd: YAG) and intra vitreal injection (0.0625 mg Bivacizumab) was given as treatment according to indication mentioned earlier in the retina operation theater of NIO under surface anesthesia (oxy buprocaine 0.4%) in presence of anesthesiologist or neonatologist if required. After laser a combination eye drop dexamethasone 0.1 % and tobramycin 0.3% and after intra vitreal injection only tobramycin 0.3 % were given for 7 days. Follow up was done on next day and 7 days after to see any adverse effect. Patients then followed up four weekly upto 40 weeks. Treatment outcome defined as good when on indirect ophthalmoscope retina appeared stable, no sign of active disease and child can follow the opto kinetic dram. Data was collected in a pre validated data sheet, zone and stages was drawn with colour pencil.
Results
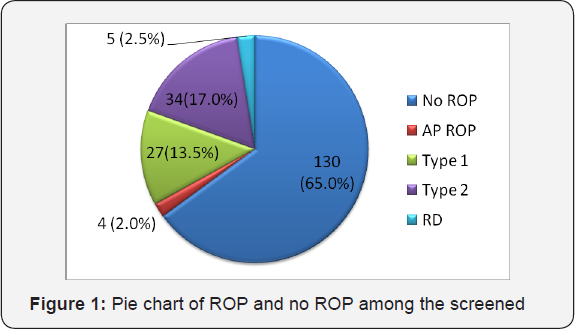
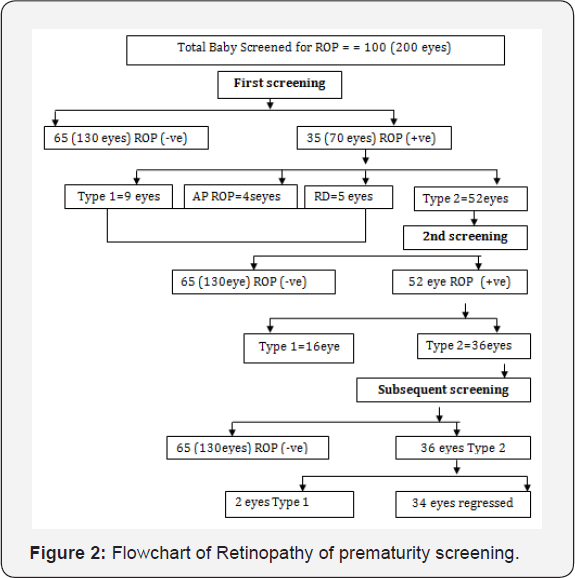
A total of 100 babies retinal evaluation were done. Among them 35 babies (Figure 1) 70 eyes (35%) were found to have ROP (27 eyes 13.5% type1, 4 eyes 2.0% APROP, 5 eyes 2.5% retinal detachment and 34 eyes 17.0% were type 2). (Table 1) shows the incidence of Retinopathy of prematurity according to gestational age. It is observed that who born <=28 weeks were at greater risk to develop ROP, 10 out of 11 (90.9%) and risk reduced to 14.3% (3 out of 21) if babies born > 32 weeks.
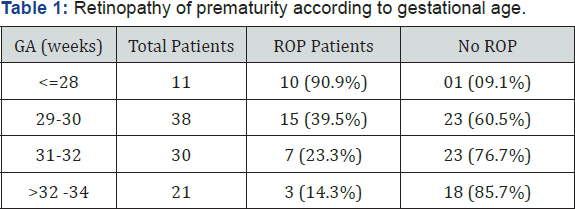
During the first screening 9 eyes had type 1, 52 eyes had type 2, 4 eyes had APROP and 5 eyes were found to have retinal detachment. In the subsequent follow up another 18 eyes progressed to type 1 ROP from the type 2 group (Figure 2).
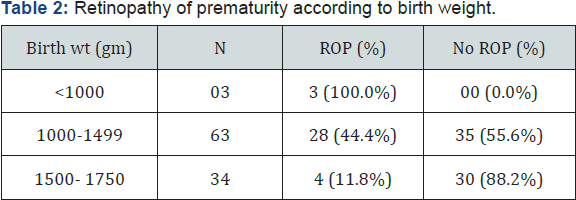
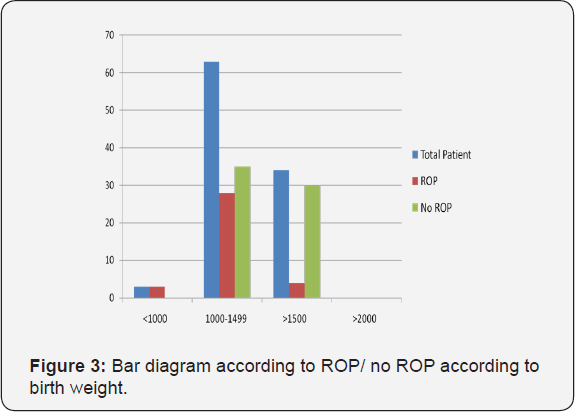
(Table 2) shows the incidence of retinopathy of prematurity according to the birth weight. It has been observed that all babies <1000g had ROP and the risk declined to approximately half (44.4%) if the birth weight was between 1000g to 1499g, and it was further reduced to nearly one tenth (11.8%) when the birth weight ≥ 1500g. (Figure 3) depicted the bar diagram according to ROP/ no ROP according to birth weight.
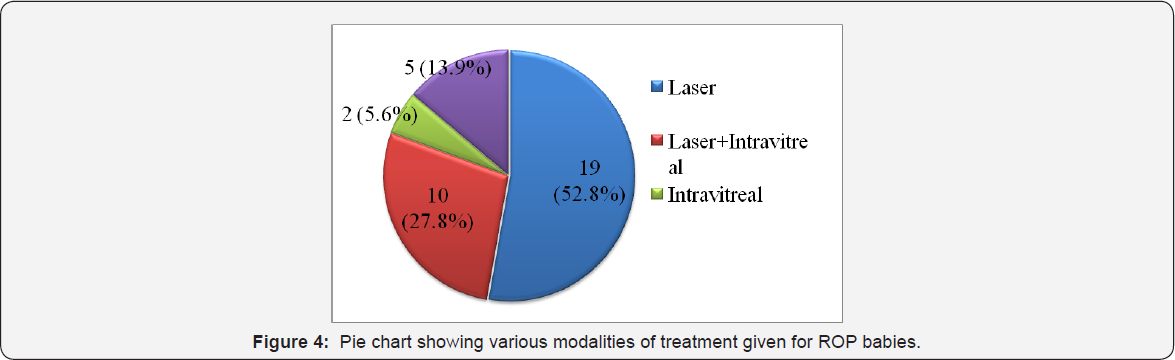
In regards to treatment, 19 (52.8%) eye received laser, 10 (27.8%) eyes had received both laser and intra vitreal bivacizumab, 2 eyes (2.6%) has got only intra vitreal bivacizumab and 5 (13.9%) were advised for surgery (Figure 4).
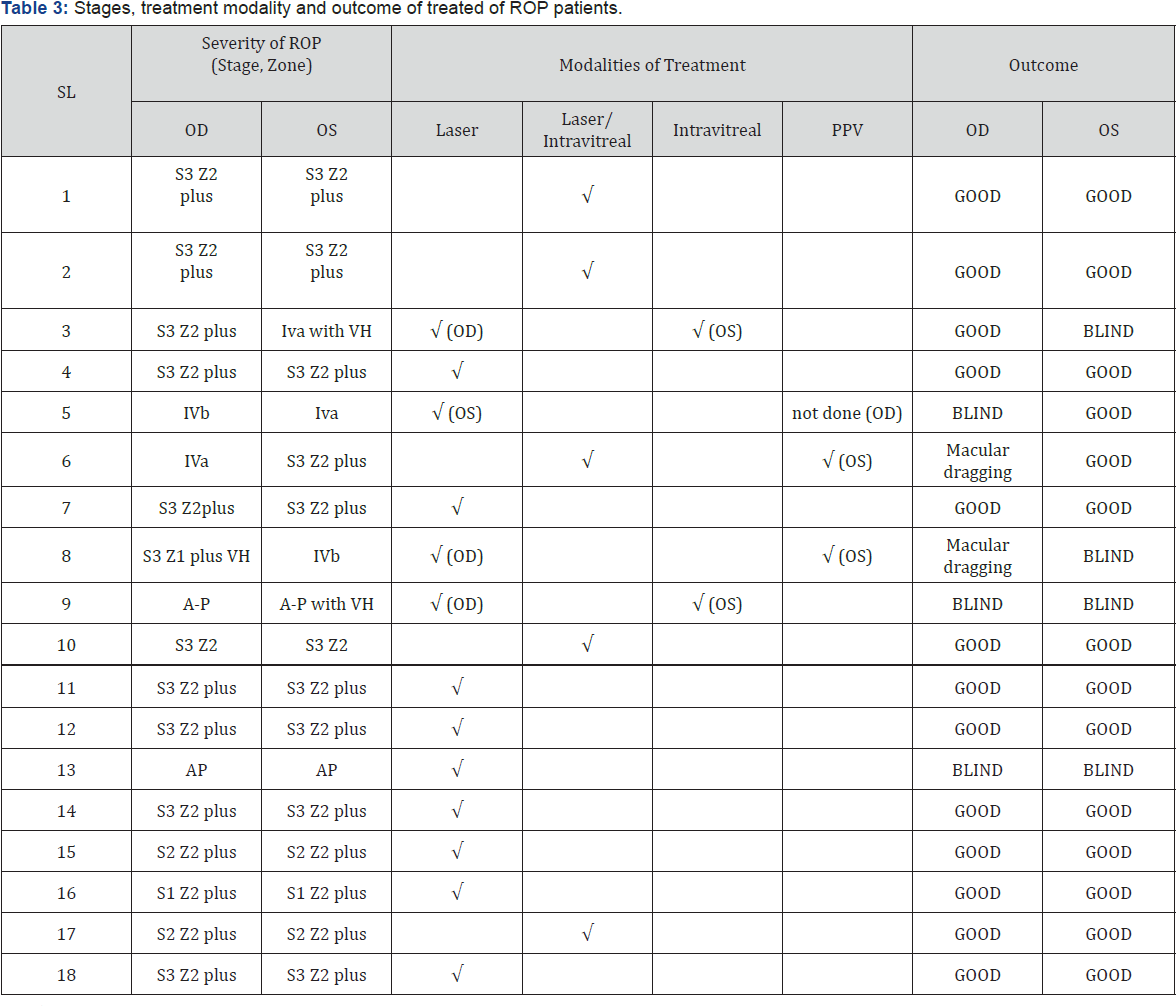
(S: stages of ROP; Z: zone of ROP)
Table 3 showed the Stages, zones, treatment modality and outcome of treated of ROP patient's up to forty weeks of follow up. Laser showed the effective choice of treatment where it can be given satisfactorily (among 19 eyes (52.8%), one eye got macular dragging, 2 eyes got blind). Combined treatment of laser and intra vitreal bivacizumab showed promising results (out of 10 eyes (27.8%), only one eye got macular dragging), On the other hand, only intra vitreal bivacizumab and pars plan a vitrectomy did not show good results in our study.
Discussion
Screening ofpremature low birth weight infants for retinopathy of prematurity is being carried out as a routine procedure in NICU and SCABU of Dhaka Shishu (Children) Hospital by the ROP team, National Institute of Ophthalmology since late 2013. We reported here result of the first 100 screened babies for the incidence of ROP and their treatment requirements. We have included the babies who were less than 34 weeks of gestational age and birth weight less than 1800 grams after a consensus meeting with the neonatologists, pediatric ophthalmologists and retina specialists forum on a strategic workshop on ROP screening held at the Ispahani Islamia Eye Institute & Hospital, Dhaka, Bangladesh in 2013.
Several studies have reported incidence rates ranging from 10% to 46% among low birth weight premature infants [8,9]. In our study have got 35% of the screened infants had ROP The incidence of ROP was highest among the low gestational age <=28 (90.9%) which steadily decreased with the increment of such ages. It has also been observed that low birth weight is the other most important risk factor for the development of ROP and found those babies who were <1000 gram had ROP in all of them. The development of ROP reduces with the increases of birth weight.
One of our important finding in this study is that we got most of the babies with ROP in first screening. That means, although we decided to do first screening within 30 days of birth, many children came after the time frame and as such, we had few babies in advanced stages (2.5%, five eyes with retinal detachment). This could be important news for the neonatologists who are basically the integral part of ROP screening procedure.
Another observation in this study was recognition of aggressive posterior retinopathy of prematurity (APROP) in the Bangladeshi children. There were 2.0% (4 eyes) babies had aggressive form of the disease, an uncommon, rapidly progressing and severe form of ROP APROP is characterized by its posterior location with prominence of plus disease, does not progress through classic stages from 1 to 3 and neovascularization may be flat and easily overlooked. In our study we did indirect ophthalmoscopy with the relative magnification of a 20 D condensing lens may aid in identifying this type of neo vascularization [16].
Treatment was necessary after diagnosis of ROP varies in different literature and found from 1.4% to 10.8% [17]. In this study, there was 18.0% babies (36 eyes) required treatment by different modalities. Why such a large number of babies required treatment is a question indeed. We looked for the answer of this question and assumed that most of the screened babies came to us in advanced stages due to irregularity and missing of follow- up. As per treatment modalities, laser was still remained the best option in the early stage. However, intra vitreal bivacizumab and pars plan a vitrectomy were disappointing in our setting may be because of the lack of sickness or advanced stage of the disease.
Conclusion
The observed incidence of retinopathy of prematurity is high among the infants with very low birth weight. The development of ROP was inversely proportional to the weight and gestational age at birth.
Recommendation
Data on ROP incidence and requirement of treatment is scarce in Bangladesh. We believe that this study would give clinical information and resources needed to combat the upcoming epidemic of ROP in the country
References
- Cryotherapy for Retinopathy of Prematurity Cooperative Group (1996) Multicenter trial of cryotherapy for retinopathy of prematurity. Snellen visual acuity and structural outcome at 51/2 years after randomization. Arch Ophthalmol 114(4): 417-424.
- Repka MX, Summers GC, Palmer EA (1998) The incidence of ophthalmologic interventions in children with birth weights less than 1251 grams. Results through 51/2 years. Cryotherapy for Retinopathy of Prematurity Cooperative Group. Ophthalmology 105(9): 1621-1627.
- Quinn GE, Dobson V, Kivlin J (1998) Prevalence of myopia between 3 months and 51/2 years in preterm infants with and without retinopathy of prematurity. Cryotherapy for Retinopathy of Prematurity Cooperative Group. Ophthalmology 105(7):1292-1300.
- Bremer DL, Palmer EA, Fellows RR (1998) Strabismus in premature infants in the first year of life. Arch Ophthalmol 116(3): 329-333.
- Haines L, A Fielder, H Baker, A Wilkinson (2005) UK population based study of severe retinopathy of prematurity: screening, treatment and outcome. A D C Fetal & Neonatal Edition 90(3): 240-244.
- Flynn J T (1992) A cohort study of transcutaneous oxygen tension and the incidence and severity of retinopathy of prematurity. N Engl J Med 326(16): 1050-1054.
- Rowlands E, Ionides AC, Chinn S (2001) Reduced incidence of retinopathy of prematurity. Br J Ophthalmol 85(8): 933-935.
- Cats BP, Tan KE (1985) Retinopathy of prematurity: review of a four- year period. Br J Ophthalmol 69(7): 500-503.
- Shohat M, Reisner SH, Krikler R, Nissenkorn I, Yassur Y, et al. (1983) Retinopathy of prematurity: incidence and risk factors. Pediatrics 72(2): 159-163.
- Karkhaneh R, S Z Mousavi, M Riazi-Esfahani, S A Ebrahimzadeh, R Roohipoor (2008) Incidence and risk factors of retinopathy of prematurity in a tertiary eye hospital in Tehran. British Journal of Ophthalmology 92(11): 1446-1449.
- Gibson D L, S B Sheps, S Hong, M T Schechter, A Q McCormick, et al. (1990) Retinopathy of prematurity-induced blindness: birth weight- specific survival and the new epidemic. Pediatrics 86(3): 405-412.
- Gilbert C (2008) Retinopathy of prematurity: a global perspective of the epidemics, population of babies at risk and implications for control. Early Human Development 84(2): 77-82.
- Hellen A, Mintz H, Ronald R (2008) Intravitreal injection of Bivacizumab (Avastin) for treatment of stage 3 retinopathy of prematurity in zone I or posterior zone II. Retina 28(6): 831-838.
- Hugo Q Maria A, Martinez C (2008) Antiangiogenic therapy with intravitreal bivacizumab for retinopathy of prematurity. Retina 28(3): 19-25.
- Fierson WM, Palmer EA, Petersen RA (2001) Screening examination of premature infants for retinopathy of prematurity. Pediatrics 108(3): 809-811.
- David K (2008) Focal points. Retinopathy of prematurity. AAO 12: 3.
- C Jandeck, MH Foerster (2007) Retinopathy of Prematurity: Clinical course and Treatment. Retinal Vascular Disease. Springer, p. 409.






























