Transient Evoked Otoacoustic Emissions and High Risk Register in Neonates
Nagwaa Hazzaa1, Dalia Mohamed Hassan1* and Asmaa Mostafa2
1Ain Shams University, Egypt
2Port Fouad hospital, Egypt
Submission: January 16, 2017; 2016; Published: February 20, 2017
*Corresponding author: Dalia Mohamed Hassan, Audiology Unit, ENT Dept, Faculty of Medicine, Ain Shams University, Abbassia Street, Cairo, Egypt, Tel: 0224821485; Email: daliamsg_audio@yahoo.com
How to cite this article: Nagwaa H, Dalia M H, Asmaa M. Transient Evoked Otoacoustic Emissions and High Risk Register in Neonates. Acad J Ped Neonatol. 2017; 3(2): 555606. DOI:10.19080/AJPN.2017.03.555606
Abstract
Objective: To document the frequency of risk factors for hearing loss in neonates undergoing the neonatal hearing screening program in Port Fouad primary health care centers and to imply their influence on the characteristics of transient evoked OAE (TEOAEs).
Study design: All neonates referred to port Fouad hospital for hearing screening program were included. The presence of risk factors for hearing loss was documented by using the High risk Registry 'HRR' Arabic checklist. The TEOAEs was done to all neonates and the responses were examined in two steps: First, screenings pass/refer criterion; second, the magnitude of TEOAEs responses for neonates with pass responses. The analysis of the responses targeted the presence and absence of HRR, the ear, gender and age effects.
Results: Five hundreds neonates (52% males, 48% females) were seen during the study period. Their mean age was 11.6 (±7.6) days. The HRR was present in 25% of neonates. Incubation in neonatal intensive care unit and cyanosis were the commonest factors. The screening TEOAEs showed 'pass' response in 94.8% of tested neonates. In neonates with high risk factors, 10.4% of neonates had 'refer' response. The mean of TEOAEs responses in the HRR group were lower in amplitude values than no HRR and reached statistical significance at 2 & 3 KHz. The TEOAEs amplitudes were larger in the right ear and in the female gender.
Conclusions: The TEOAEs provide important information on the operation of outer hair cell in newborns. The presence of risk factors affect the TEOAEs both in the pass /refer criteria or in the response values. Newborns with HRR require clinical monitoring and electrophysiological assessment to identify possible damage to the cochlea and auditory nerve cells, as well as to the development of auditory processing.
Keywords: Neonatal hearing screening; TEOAEs; High risk register
Introduction
The development and application of otoacoustic emissions in clinical practice marked the beginning of a new era in the field of screening for congenital hearing loss. In particular, transient evoked otoacoustic emissions (TEOAEs) have been widely adopted by many universal hearing screening (UNHS) programs. The test is quick, non-invasive, objective, sensitive, frequency specific, relatively cheap and can be performed in non-soundproofed facilities [1].
The Joint Committee for Infant Hearing 'JCIH' [2] published the risk factors of hearing loss in neonates and formally established a high-risk registry 'HRR', which listed ten risk factors for hearing loss. Risk factor registers are used to select which babies are target-ed for follow-up examinations [3]. The overall prevalence of unilateral and bilateral mild to severe hearing impairment in this high risk infant population is 10-100 times higher than in newborns without risk factors [4].
The risk factors for hearing loss include family history of permanent hearing loss in childhood, maternal infections during pregnancy or delivery, physical problems of the head/face/ ears/or neck, ototoxic medications given in the neonatal period, syndrome associated with hearing loss, admission to a neonatal intensive care unit 'NICU' greater than 5 days, prematurity (< 37 weeks), and hyperbilirubinemia [2].
Universal hearing screening in both well-baby and NICU newborn, yields a large amount of data on the presence and features of otoacoustic emissions measured in these groups. Most reports focus on the 'pass-fail' results of hearing screening testing [5]. However for Aidan et al. [6], one of the criteria to assess the actual status of the inner ear in neonates is the analysis of the intrinsic characteristics of this examination, such as the response magnitude of these emissions. The use of oto toxic drugs can cause lower amplitude response for otoacoustic emissions in neonates with preserved responses [7]. Basseto et al. [8] reported higher response amplitudes in full-term newborns when compared to preterm newborns.
One purpose of this study was to document the frequency of risk factors for hearing loss in neonates undergoing the neonatal hearing screening program in Port Fouad primary health care centers using the HRR. The value of HRR in this geographic area was highlighted. The other purpose was, to imply their influence on the TEOAEs of infants. The analysis of the signal/noise ratio can provide additional information on the functional status of the peripheral auditory system and the subsequent input to the central auditory nervous system.
Methodology
Subjects
The study included all neonates referred to port Fouad hospital from Port Fouad primary health care (PHC) offices (first and second) during the period January 2013 to March 2014. This was a regional part of the general screening program of ministry of health and population. The birth rate in port Fouad city is about 100 neonates per month. Referral for hearing screening was done in the same day for hypothyroidism screening. All neonates were tested in a single session. Informed consent signed by the parents of the neonate was obtained prior testing.
Procedures
All neonates were assessed using:
A. High risk registry checklist 'Arabic form' [9]. It focused on the presence of risk factors for hearing loss and was filled by the parents. It was composed of ten questions covering the known risk factors and the answers were categorized into yes, no, and I don't know. The scoring was calculated for each neonate out of 100, 'Yes' score 10, 'No' score 0, 'I don't know' score 5.A. High risk registry checklist 'Arabic form' [9]. It focused on the presence of risk factors for hearing loss and was filled by the parents. It was composed of ten questions covering the known risk factors and the answers were categorized into yes, no, and I don't know. The scoring was calculated for each neonate out of 100, 'Yes' score 10, 'No' score 0, 'I don't know' score 5.A. High risk registry checklist 'Arabic form' [9]. It focused on the presence of risk factors for hearing loss and was filled by the parents. It was composed of ten questions covering the known risk factors and the answers were categorized into yes, no, and I don't know. The scoring was calculated for each neonate out of 100, 'Yes' score 10, 'No' score 0, 'I don't know' score 5.A. High risk registry checklist 'Arabic form' [9]. It focused on the presence of risk factors for hearing loss and was filled by the parents. It was composed of ten questions covering the known risk factors and the answers were categorized into yes, no, and I don't know. The scoring was calculated for each neonate out of 100, 'Yes' score 10, 'No' score 0, 'I don't know' score 5.
B. Transient Evoked otoacoustic emissions (TEOAEs) using Smart TrOAE Intelligent Hearing System. To obtain reliable results, all neonates were tested either during natural sleep or calm in a relatively quiet test environment. Each ear was tested separately beginning with the right ear.
TEOAEs were elicited using click stimuli at 80 dB SPL with a rate of 20 per second. They were analyzed during the 20 milliseconds after the stimulus. A total of 1024 were averaged on each of two buffers (A and B), and above the automatic noise rejection level of the instrument.
The TEOAEs was done to all neonates and the responses were examined in two steps.
Step 1: screenings pass/refer results. By default, values were considered 'pass' when emissions present in a signal/noise ratio of 3dB in at least three consecutive frequency bands, including the 4,000 Hz band; 'refer' reflected absence of TEOAEs responses. The examination lasted 64 seconds, at most.
Step 2: All neonates with 'pass' response were included in this step. They were divided into two groups according to the presence of HRR. Group 1: HRR group, group 2: no HRR group. The analysis of the TEOAEs response magnitude targeted the variation between neonates in presence and absence of HRR; ear effect (between the right and left ears); gender effect (between males and females), and age effect. The TEOAE was measured in five frequency bands (1, 1.5, 2, 3, 4 KHz). The overall reproducibility and over all response in dB were also studied.
Statistical analysis of the data set was performed using statistical computer program (SPSS 12.0) for further evaluation and analysis. Quantitative data were described using mean and standard deviation. Association between categorical variables was tested using Chi-square test. Comparison between two independent variables was done using independent t-test. Correlations between quantitative variables were assessed using Spearman coefficient. The level of statistical significance (p-value) was set at 0.05, and 0.01. A statistician was used for guidance in the study.
Results
Five hundred neonates (52% males, 48% females) were seen during the study period. It was estimated to have larger number of neonates that should reach around 1400 considering the birth rate in this city. A high percent of drop out up to 62% was evident. This might be attributed to several factors as miss communication between PHC and Port Fouad hospital to follow the program, non motivated parents, busy PHC.
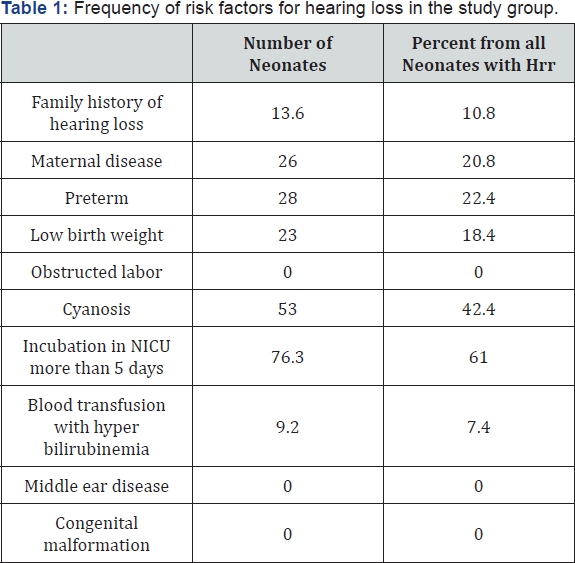
The mean age of studied neonates was 11.6 days (Standard Deviation SD ±7.6), range 1-30 days. The HRR checklist highlighted that the risk factors for hearing loss was present in 25% of neonates 'n=125'. More than one risk factor was seen in 14% 'n=70' while in the remaining neonates '11%; n=55' single factor was met. Table 1 showed the common risk factors seen in
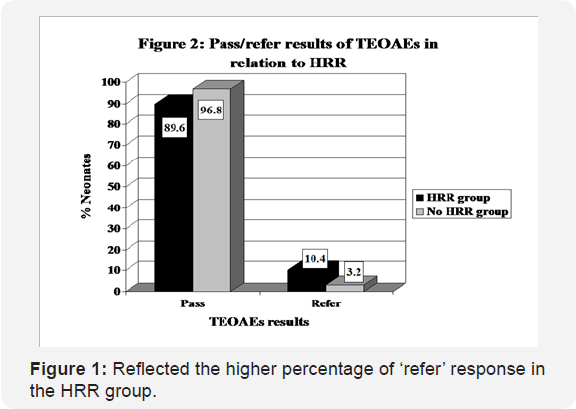
The relation between the risk factor score percentage and TEOAE pass/refer criteria was further studied using the chi square test (Table 2). It was found that as the HRR score increased denoting presence of more than one risk, the 'refer' response increased. This was statistical highly significant (p <0.001).
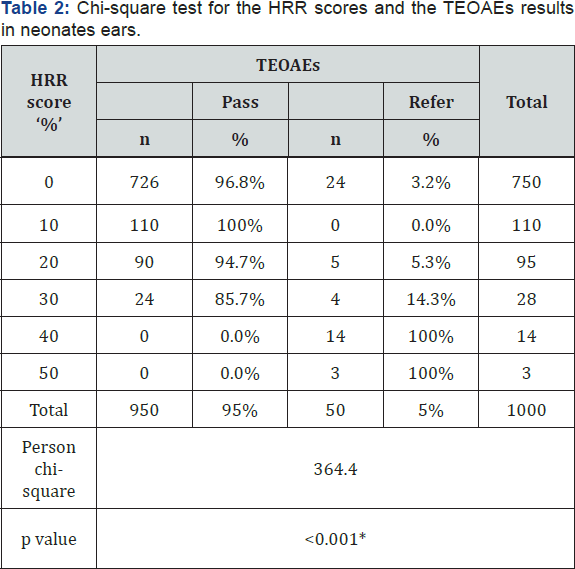
n = number of ears , *p< 0.05 statistically significant
From the above mentioned results the value of HRR checklist in neonatal hearing screening was highlighted. Studying the sensitivity and specificity of HRR checklist in relation to results of TEOAEs revealed that the sensitivity = 52.9%, specificity = 76.5%, positive predictive value = 10.8%, and negative predictive value=96.8%.
TEOAEs response analysis
The TEOAEs responses were analyzed and compared in the ears of the two groups. The mean of responses in the HRR group were lower in amplitude values than no HRR. These values reached statistical significance at 2 & 3 KHz. For both groups there was an increase of the response amplitude with increasing the frequency tested, except at 4 kHz (Table 3) The effect of each single risk factor on the TEOAEs responses was difficult to be studies as the majority of neonates had more than one risk factor in combination.
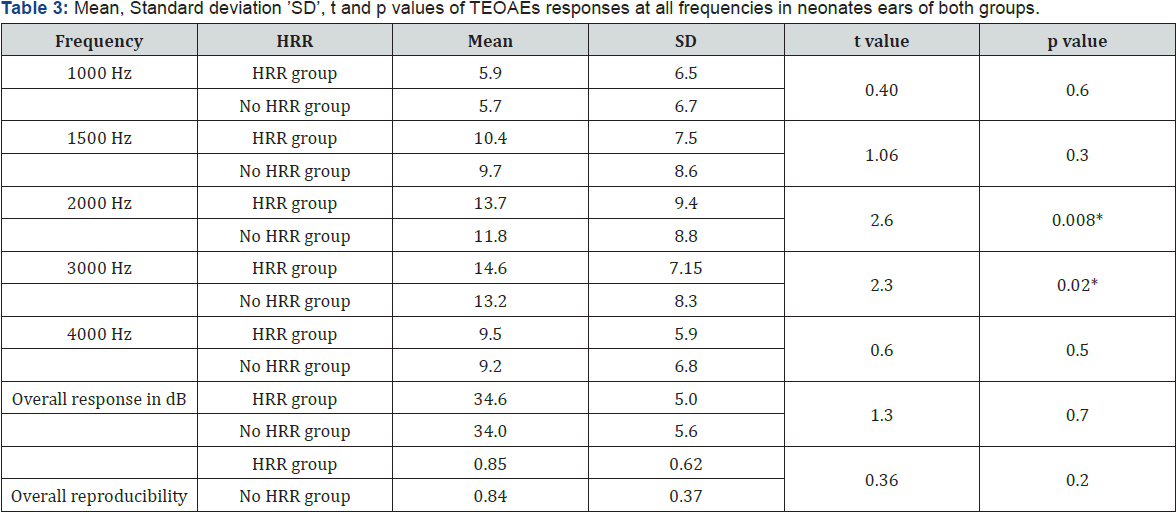
*p < 0.05 statistically significant; the shaded area highlighted the significant frequencies
Moreover, the TEOAEs amplitudes were larger in the right versus left ear in both groups. However, it reached statistical significance only in the HRR group at 3 & 4 KHz (Table 4). The female gender had higher TEOAEs response amplitudes in presence or absence of HRR with no statistical significant difference except at only 4 KHz in the HRR group (Table 5). The age of neonates was not statistically correlated with the TEOAEs either in the HRR group or no HRR group (Table 6).
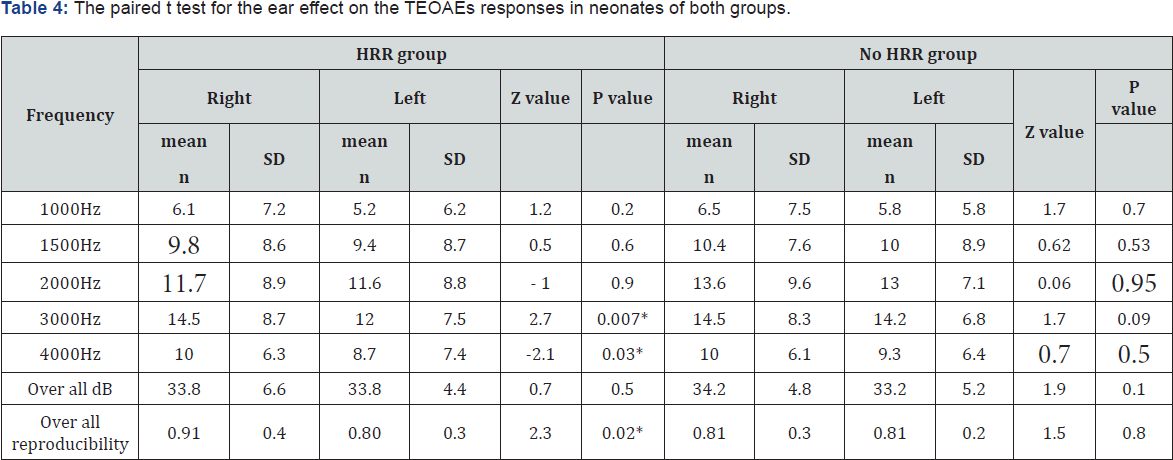
*p < 0.05 statistically significant; the shaded area highlighted the significant frequencies.

*p < 0.05 statistically significant, the shaded area highlighted the significant frequencies
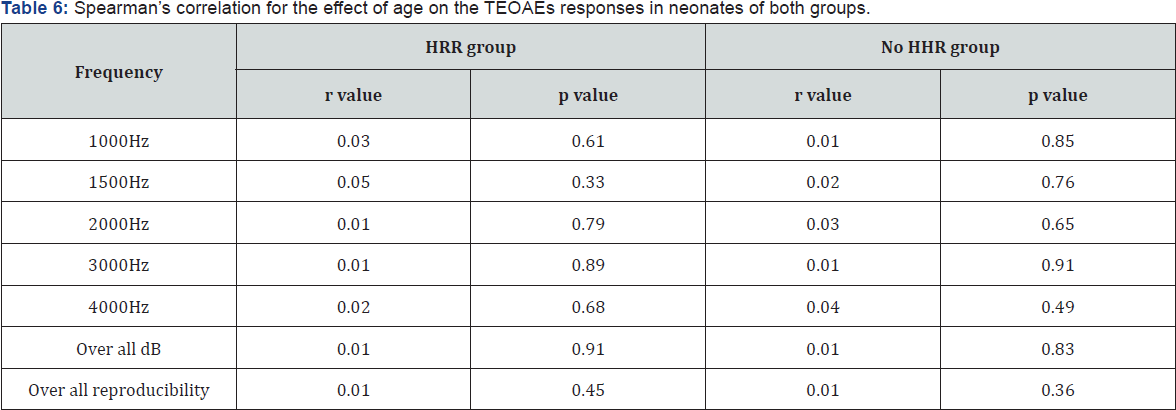
Discussion
One newborn every 500 -1,000 births present with hearing impair-ment which are greater incidence than the other incidence of diseases seen at birth [10]. In some populations incidence could be greater depending on different factors. In the current study, the results related to the presence of TEOAEs agree with several researches which observed 93% up to 97.0% of the tested neonates showed present responses [11,12].
The high rate of exposure to risk factor in developing countries increased the risk of hearing impairment [13]. Twenty- five percent of neonates in the present study had risk factors for hearing loss. In another Egyptian study, Hassan et al. [14] reported that the frequency of neonates with risk factors was 29%. A variety of risk factors for hearing loss were seen in the current study with incubation in NICU more than 5 days followed by cyanosis being the commonest. This agreed with Martinez-Cruz et al. [15] & Bielecki et al. [16]. Bielecki et al. [16] reported that the most frequent risk indicator for hearing loss was the use of ototoxic drugs (33.13%).
Obviously, the 'refer' responses were seen in neonates with HRR at a greater percentage (10.4%) compared to the no HRR group (3.2%). Similarly, Abdullah et al. [17] showed that 11.8% of the screened high-risk neonates in Malaysia failed the TEOAEs test. Wroblewska-Seniuk et al. [18] reported failure rate of TEOAEs in 24.9% of the high-risk registers. From the current study, as the risk factor score increased the percentage of passed ears decreased. In agreement, Bielecki et al. [16] highlighted that the greater the number of risk factors an infant is exposed, the probability of hearing impairment increases.
Furthermore, due to its high negative predictive value, the HRR could guide the neonatal screening process. It has the ability to exclude the neonates with hearing loss efficiently up to 96.8% and should be used as primary indicator for hearing loss in the screening program. However, its low sensitivity precludes its use as the primary indicator for screening newborn for hearing loss. It correctly identified neonates with 'refer' TEOAEs is only 53% while in well-baby nursery 50% of neonates with no known risk factors had hearing loss [2]. The sensitivity could be improved if HRR checklist categorized into 'no' risk, 'low' risk and 'high' risk as suggested by the authors.
A considerable number of neonates (89%) with HRR got 'pass’ response in TEOAEs. The low TEOAEs amplitude values across all frequencies in the HRR group suggested more vulnerability of outer hair cells in neonates with risk factors, even with the presence of response. This indicated the possibility of sub clinical damage to cochlear cells caused by tissue hypoxia, acidosis, and immature metabolic function, hyperbilirubinemia, ototoxic drugs, which are often administered to these newborns because of coexisting disease [19].
Jiang et al. [20] observed significantly lower amplitudes at frequencies of 1 kHz and 10 kHz in otoacoustic emission testing by distortion products in neonates with low Agar scores, suggesting cochlear impairment. Similarly, Ribeiro et al. [21] had evidenced low performance of outer hair cells in neonates who had perinatal asphyxia, which may affect the development of listening skills in this population. Korres et al. [1] showed that TEOAEs of very low birth weight newborns have lower reproducibility compared to normal newborns. Therefore, infants with risk factors should undergo serial follow-up, as proper development of auditory skills depends on the integrity of the peripheral auditory system and thus, parents should be informed.
In the current study, the TEOAE responses recorded from the neonates ears with and without HRR was larger in amplitude in the high frequency bands (2,3,4KHz) than low frequency bands ( 1,1.5 KHz). Kochanek et al. [22] stated that TEOAE responses increase as the frequency increase. Norton et al. [23] highlighted that the internal noise of the infant and the noise in the testing environment are affecting the signal to noise ratio particularly in the low frequency bands. They recommended screening only for higher frequencies as a time saving procedure. However high-frequency testing is less reliable, due to the standing-wave problem and the limitation of the electro-acoustic transducer.
The analysis of the magnitude of TEOAEs in relation to ear showed higher amplitudes in the right ear compared to left in both the HRR and No HRR groups. In a way, the findings described in this paper match the literature, as higher values were found for right ears that reached statistical significance at 3 kHz and 4 kHz only in the HRR group.
It is known that predominantly crossed medial olivocochlear system stimulation in the brainstem from contralateral auditory stimulation leads to reduced TEOAEs magnitude. Such suppression effect is present in neonates with increased suppression effect in right ears [24]. This same effect could grant right ears increased TEOAEs response. Increased right ear responses are assigned to sound processing at the level of the cochlea and the brainstem, possibly facilitating further hemispheric specialized development for the processing of certain sound types. Such specialization is attributed to the left auditory cortex [25].
As shown in this study, the difference in amplitude between both ears reached statistical significance only in the HRR group. The risk factors might impede the maturation of the peripheral auditory system altering the suppression effect in those neonates thus augmenting the difference between the two ears. A research on the effect of the suppression of the TOAEs in preterm infants with risk of hearing loss observed a trend of increase of the magnitude of suppression with the increase of the chronological age [4].
The newborn females of the present study had higher mean TEOAEs amplitudes when compared to male neonates. Significantly higher mean amplitudes were observed in females, with a predominance of the right ear was reported by others [6,26]. On the other hand, no difference between genders was reported when comparing the amplitude of the TEOAEs in preterm and term neonates [4], and in other surveys conducted by the same procedure [24]. Higher response levels in females may be associated with the gender's shorter cochlear length [27]. In spite of a few differences, some authors have found shorter cochlear length in females. In shorter cochleae, acoustic stimulation could get to the OHC more quickly, losing less sound energy, consequently eliciting better responses. Moreover, Cassidy & Ditty [26] explained the higher amplitudes in females can be due to attributed to increased sensitivity of the outer hair cells in females.
The detailed analysis of the characteristics of TEOAEs responses in the present study pointed to the importance of development of TEOAEs normative data in an attempt to maximize the usefulness and accuracy of this important tool. The authors suggest the following in TEOAEs data interpretation. Initial assessment of the noise floor to ensure it is sufficiently low for the correct analysis of the presence or absence of response. Secondly, to determine which category the recorded TEOAEs fall into:
A. 'present and normal' when meets the SNR criteria for detection and falls within the normal range
B. 'present, but abnormal' when meets the SNR criteria for detection, but is below the normal range
C. “absent” when does not meets the SNR criteria for detection.
Useful conclusions obtained from this study enabled use to confirm that the HRR is an important guide in the neonatal screening program. The TEOAE test provides indispensable information on the pe-ripheral auditory system of newborns. Because of the relative ease of record-ing, it is considered a method of choice in newborn hearing screening protocols for cochlear acuity assessment. It was obvious that the presence of risk factors affects the results of TEOAE both in the pass /refer criteria or in the response magnitude values.
It is recommended to use the HRR checklist to identify the presence of risk factor for hearing loss. Newborns with high risk registers require clinical monitoring and electrophysiological assessment to identify possible damage to the cochlea and auditory nerve cells, as well as to the development of auditory processing. Fortunately, the JCIH screening recommends that all infants with risk indicators should undergo periodic monitoring every 6 months for the first three years of life.
Acknowledgement
The contribution of the parents in this study was highly appreciated.
References
- Korres SG, Balatsouras DG, Nikolopoulos T, Korres GS, Ferekidis E (2006) Making universal newborn hearing screening a success. Int J Pediatr Otorhinolaryngol 70: 241-246.
- Joint Committee on Infant Hearing (2007) Year 2007 position statement: principles and guidelines for early hearing detection and intervention programs. Pediatrics 120(4): 898-921.
- Karaca 5, Oysu 5, Toros S, Naiboglu B, Verim A (2014) Is Hearing Loss in Infants Associated With Risk Factors? Evaluation of the Frequency of Risk Factors. Clin Exp Otorhinolaryngol 7 (4): 260-263.
- Ferreira D, Araújo N, Marques S, Miranda I, de Resende F, et al. (2014) Peripheral auditory maturation: analysis of the amplitudes of the distortion product otoacoustic emissions in preterm and term neonates. Audiol Commun Res 19(1): 25-32.
- Simonek MC, de Azevedo MF (2011) False-positive results in newborn universal hearing screening: possible causes. Rev CEFAC 13(2): 292298.
- Aidan D, Lestang P, Avan P, Bonfils P (1997) Characteristics of transient- evoked otoacoustic emissions (TEOEs) in neonates. Acta Otolaryngol 117(1): 25-30.
- Zorowka PG, Schmitt HJ, Gutjahr P (1993) Evoked otoacustics emissions and pure tone threshold audiometry in patients receiving cisplatinum therapy. Int J Pediatr Otorhinolaryngol 25(1-3): 73-80.
- Basseto MC, Chiari BM, Azevedo MF (2003) Transient evoked otoacoustic emissions (TEOAE): response amplitude in term and preterm neonates. Rev Bras Otorrinolaringol 69(1): 84-92.
- Kamal N, El Dessouky A (2005) Egyptian Neonatal Hearing Screening Program, children with special needs directorate, ministry of health and population, Egypt.
- Ohl C, Dornier L, Czajka C, Chobaut JC, Tavernier L (2009) Newborn hearing screening on infants at risk. Int J Pediatr Otorhinolaryngol 73(12): 1691-1695.
- Erturk B, Genc A, Ozkan S (2010) Comparison of hearing screening protocols for universal newborn hearing screening in Turkey. IAO 6(2): 223-230.
- Oliveira J, Rodrigues L, Aurélio F, Silva V (2013) Risk factors and prevalence of newborn hearing loss in a private health care system of Porto Velho. Northern Brazil 31(3): 299-305.
- Kamal N (1990) Profound hearing loss in Egyptian children. Egy J of Surg 9(2).
- Hassan D, El Mously M, El Gohary M, Ismail n, El-Dabaa M (2006) Universal neonatal hearing screening: Unpublished doctoral thesis, Audiology unit, E.N.T. Depatement, El-Azhar University, Egypt.
- Martinez Cruz CF, Poblano A, Fernandez Carrocera LA (2008) Risk factors associated with sensorineural hearing loss in infants at the neonatal intensive care unit: 15-year experience at the National Institute of Perinatology (Mexico City). Arch Med Res 39(7): 686-694.
- Bielecki I, Horbulewicz A, Wolan T (2011) Risk factors associated with hearing loss in infants: an analysis of 5282 referred neonates. Int J Pediatr Otorhinolaryngol 75(7): 925-930.
- Abdullah A, Hazim M, Almyzan A, Jamilah AG, Borhan L, et al. (2006) "Newborn hearing screening: experience in a Malaysian hospital”. Singap Med J 47(1): 60-64.
- Wroblewska Seniuk K, Chojnacka K, Pucher B, Szczapa J, Gadzinowski J, et al. (2005) The results of newborn hearing screening by means of transient evoked otoacoustic emissions. Int J Pediatr Otorhinolaryngol 69(10): 1351-1357.
- Uchoa N, Procianoy R, Lavinsky L, Sleifer P (2003) Prevalence of hearing loss in very low birth weight neonates. J Pediatr (Rio J) 79: 123-128.
- Jiang Z, Zang Z, Wilkinson A (2006) Distortion product otoacoustic emissions in term infants with a low Apgar score. Acta Otolaryngol 126: 1062-1066.
- Ribeiro G, Camargo da Silva D, Montovani J (2014) Assessment of levels of otoacoustic emission response in neonates with perinatal asphyxia. Rev Paul Pediatr 32(3): 189-193.
- Kochanek K, Sliwa L, Puchacz K, Pitka A (2015) Repeatability of Transient-Evoked Otoacoustic Emissions in Young Adults. Med Sci Monit 4(21): 36-43.
- Norton S, Gorga M, Widen J, Vohr B, Folsom R, et al. (2000) Identification of neonatal hearing impairment: transient evoked otoacoustic emissions during the perinatal period. Ear Hear 21(5): 425-442.
- Gkoritsa E, Korres S, Psarommatis I, Tsakanikos M, Apostolopoulos N, et al. (2007) Maturation of the auditory system: 1. Transient otoacoustic emissions as an index of inner ear maturation. Int J Audiol 46(6): 271276.
- Tognola G, Parazzini M, de Jager P, Brienesse P, Ravazzani P, et al. (2004) Cochlear maturation and otoacoustic emissions in preterm infants: a time-frequency approach. Hear Res 199(1-2): 71-80.
- Cassidy J, Ditty K (2001) Gender differences among newborns on a transient evoked otoacoustic emissions test for hearing. J Music Ther 38(1): 28-35.
- Morlet T, Lapillonne A, Ferber C, Duclaux R, Sann L, et al. (1995) Spontaneous otoacoustic emissions in preterm neonates: prevalence and gender effects. Hear Res 90(1-2): 44-54.






























