The Role of Surgical Ligation of Patent Ductus Arteriosus in Very Preterm Infants: A Mini Review and Case Report
Brenton R Robison1*, J Radha Krishnan2 and Robert Arensman1
1Department of Pediatric Surgery, Presence Saint Joseph’s Hospital, USA
2J Radhakrishnan Professor of Pediatric Surgery, University of Illinois at Chicago, USA
Submission: November 30, 2016; Published: December 21, 2016
*Corresponding author: Brenton R Robison, Department of Pediatric Surgery, Presence Saint Joseph’s Hospital, 2800 North Lake Shore Drive, Chicago, IL 60657, USA, Email:brentr01@gmail.com
How to cite this article: Brenton R R, J Radha K, Robert A. The Role of Surgical Ligation of Patent Ductus Arteriosus in Very Preterm Infants: A Mini Review and Case Report. Acad J Ped Neonatol. 2016; 2(4): 555591
Abstract
Patent ductus arteriosus (PDA) in the very low birth weight premature newborn (VLBWPN) is currently treated with medical therapy or by surgical ligation. The objective of this mini-review and brief case report is to highlight the potential side effects of medical therapy (indomethacin or ibuprofen) including bronchopulmonary dysplasia (BPD), necrotizing enterocolitis (NEC), intraventricular hemorrhage (IVH), bowel perforation, pulmonary edema and bleeding, retinopathy, thrombocytopenia, and decrease in renal function and present an example of a patient frequently encountered in the neonatal intensive care unit that dramatically improved with prompt surgical intervention. Secondary objective is to support a more proactive approach toward early surgical ligation and highlight factors in VLBWPN who might be at the greatest risk and might benefit from earlier intervention. Currently PDA ligation is generally performed in the cases in which indomethacin or ibuprofen medication is unsuccessful or contraindicated. Given the side effects of indomethacin or ibuprofen medical therapy, it is important to recall the risks of nonoperative management of VLBWPN and to consider earlier utilization of surgical ligation.
Introduction
Patent ductus arteriosus (PDA) is a serious condition frequently seen in the neonatal intensive care unit in premature low-birth-weight infants. The reported incidence of PDA among premature babies less than 28 weeks and 1000 grams is as high as 70%, and the rate of spontaneous closure in very low birth weight premature newborns (VLBWPN) is about 34% [1]. Patent ductus arteriosus (PDA) in preterm infants is an important entity to diagnose since it is well established to be associated with increased mortality and morbidities such as bronchopulmonary dysplasia (BPD), necrotizing enterocolitis (NEC), and intraventricular hemorrhage (IVH); however, a causal relationship has not been definitively established [2]. Patent ductus arteriosus, which leads to significant hemodynamic, pulmonary, gastrointestinal, cerebrovascular, and retinal problems, can be medically or surgically treated; although, there has been an ongoing debate on which method should be preferred [1]. However, studies show that PDA closure rates with medical treatment are still low in VLBWPN. Failure of medical intervention occurs in 40% to 50% of VLBWPN necessitating surgical intervention [3,4]. In patients with a bleeding diathesis, necrotizing enterocolitis (NEC) or where nonsteroidal anti-inflammatory drugs (NSADs) are contraindicated surgical intervention is the only available option [4]. Given the side effects of indomethacin or ibuprofen medical therapy such as necrotizing enterocolitis, bowel perforation, pulmonary edema and bleeding, retinopathy, thrombocytopenia, and decrease in renal function [1] it is prudent to seriously consider an alternative to nonoperative management of VLBWPN.
Case Report
Patient was a fourteen day old female born premature at 24 weeks gestation. She was born via caesarian section due to preterm premature rupture of membranes and fetal intolerance to labor with a birthweight of 490 grams. She was noted to have Apgar scores of 5 and 8 and required immediate neonatal resuscitation with intubation for respiratory distress syndrome (RDS). She subsequently was admitted to the neonatal intensive care unit (NICU) for closer monitoring. At the time of consultation, she was tolerating feeds and weighted 560 grams but continued to require mechanical ventilation with inability to wean Fi02 (upper 40%). A transthoracic ECHO cardiogram was performed in the immediate postpartum period and found to be consistent with a large PDA with left to right shunting.
The patient subsequently underwent attempted medical therapy for closure of PDA with two courses of indomethacin. Repeat transthoracic echocardiogram on day of life eleven was found to be consistent with persistent moderate PDA with continued left to right shunting with a gradient of 25-30mmHg across the PDA. Other pertinent past medical history was significant for questionable germinal matrix bleed, extreme prematurity and respiratory failure. Other imaging included serial daily chest x-rays consistent with RDS with bilateral fluid overload that was unresponsive to Lasix.
Surgery was performed in the NICU; the patient was positioned in the right lateral decubitus position and all pressure points were padded. The left chest was prepped and draped. A posterior lateral thoracotomy was performed with Bovie electrocautery just inferior to the tip of the scapula and blunt dissection was preformed down to the subcutaneous tissues; the latissimus dorsi muscle was divided. The serratus muscle was then retracted anteriorly and the third interspace was identified. The electrocautery was further used to divide the intercostal muscles and the left chest was entered. The aorta, recurrent laryngeal nerves, subclavian artery, and the ductusarteriosus were identified; grossly normal anatomy was noted. Dissection was then carried out inferiorly and superiorly to the patent ductus arteriosus after the overlying pleura was opened. A test clamp was then preformed which she tolerated well. A medium clip was applied to the ductus, and it was noted to occlude completely. The lung was reinflated and the ribs reapproximated “with two 3-0 interrupted Vicryl sutures. Likewise the muscles were reapproximated and finally the skin was closed in a subcuticular fashion. The postoperative chest x-ray showed the clip in good position and the lungs adequately reexpanded. The immediate postoperative course was uneventful and the postoperative day one chest X-ray revealed dramatic resolution of bilateral pulmonary infiltrates (Figure 1). The Fi02 was quickly weaned to the low 30s without difficulty. The neonate resumed feedings on postoperative day one.
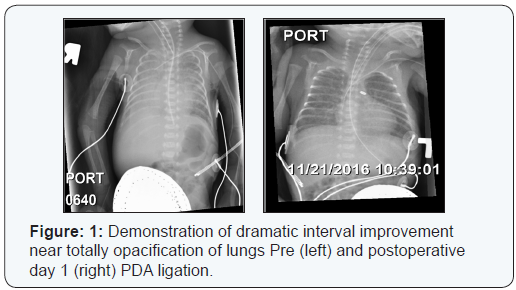
Discussion
Surgical PDA ligation is generally utilized after medical therapy with indomethacin or ibuprofen has been unsuccessful at closure. Thoracotomy (eventually done bedside in the neonatal unit to avoid transport) has been the standard of care for treating large, symptomatic, or persistent PDAs since its inception in 1938 [3]. In a study by Trust et al, they found for infants under 800 g, the failure rate for PDA closure with indomethacin was found to be as high as 40%-50% [5]. In addition, indomethacin treatment in VLBWPN has numerous severe side effects such as necrotizing enterocolitis, bowel perforation, pulmonary edema and bleeding, retinopathy, thrombocytopenia, and decrease in renal function [1]. Furthermore, other studies have clearly shown that the incidence of NEC and the duration of TPN were significantly decreased in premature infants with early surgical ligation of symptomatic PDA that was refractory to medical treatment [6].
As highlighted by Weisz et al, it is important to note that many of the observational studies on the treatment of PDA do not adequately account for confounding by indication [7]. In other words, it may be that PDA ligation is a surrogate marker for increased illness severity, as “sicker” infants may be more likely to be referred for ligation and therefore surgical ligation is generally not considered until medical treatment has failed or was contraindicated [7]. Studies to date have inadequately addressed this confounding by indication.
The results from previous studies by Grosfeld et al and Cassady et al support an opinion, that VLBWPN should undergo early surgery as the treatment of choice [8,9]. The defined interval from failed medical management in the VLBWN to surgical ligation has not been defined and is likely multifactorial in nature. Therefore, a brief period of conservative medical management for VLBWN with PDA may be a reasonable approach, but without rapid resolution and success with drugs, surgical closure of PDA, generally assured and complete with one attempt, remains the gold standard of treatment and should not be delayed.
References
- Avsar MK, Demir T, Celiksular C, Zeybek C (2016) Bedside PDA ligation in premature infants less than 28 weeks and 1000 grams. J Cardiothorac Surg 11(1): 146.
- Sung SI, Chang YS, Chun JY, Yoon SA, Yoo HS, et al. (2016) Mandatory Closure Versus Nonintervention for Patent Ductus Arteriosus in Very Preterm Infants. J Pediatr 177: 66-71.e1.
- Lam JY, Lopushinsky SR, Ma IW, Dicke F, Brindle ME (2015) Treatment Options for Pediatric Patent Ductus Arteriosus: Systematic Review and Meta-analysis. Chest 148(3): 784-793.
- Teixeira LS, Shivananda SP, Stephens D, Van Arsdell G, McNamara PJ (2008) Postoperative cardiorespiratory instability following ligation of the preterm ductus arteriosus is related to early need for intervention. J Perinatol 28(12): 803-810.
- Trus T, Winthrop AL, Pipe S, Shah J, Langer JC, et al. Optimal management of patent ductus arteriosus in the neonate weighing less than 800 g. J Pediatr Surg 28(9): 1137–1139.
- Lee JH, Ro SK, Lee HJ, Park HK, Chung WS, et al. (2014) Surgical Ligation on Significant Patent Ductus Arteriosus in Very Low Birth Weight Infants: Comparison between Early and Late Ligations. Korean J Thorac Cardiovasc Surg 47(5): 444-450.
- Weisz DE, McNamara PJ (2014) patent ductus arteriosus ligation and adverse outcomes: causality or bias? J Clin Neonatol 3(2): 67-75.
- Grosfeld JL, Chaet M, Molinari F, , Engle W, Engum SA, et al. (1996) Increased risk of necrotizing enterocolitis in premature infants with patent ductusarteriosus treated with indomethacin. Ann Surg 224(3): 350-357.
- Cassady G, Crouse DR, Kriklin JW, Strange MJ, Joiner CH, et al. (1989) A randomized controlled trial of very early prophylactic ligation of the ductusarteriosus in babies who weighed 1000 g or less at birth. N Engl J Med 320(23): 1511-1516.






























