Neonatal Lung Abscess
Ujwal Kariholu*
Consultant Neonatologist, Plymouth hospitals NHS Trust, Derriford road, Plymouth
Submission: September 24, 2016; Published: October 07, 2016
*Corresponding author: Ujwal Kariholu, Consultant Neonatologist, Plymouth hospitals NHS Trust, Derriford road, Plymouth, UK, Tel:0044-7951925562; Emailujwalkariholu@nhs.net
How to cite this article: Ujwal K. Neonatal Lung Abscess. Acad J Ped Neonatol. 2016; 1(5): 555574.DOI: 10.19080/AJPN.2016.01.555574
Neonatal lung abscess
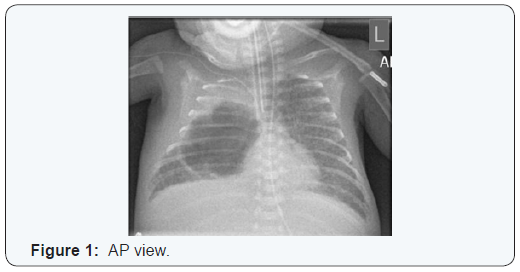
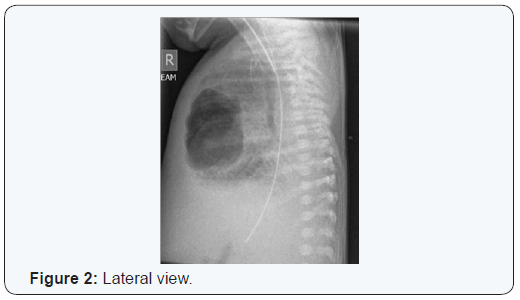
A baby girl was born at 23+4 weeks by precipitate delivery following spontaneous onset of labour and PROM of 121 hours. Mum had received a course of antenatal steroids. Following two unsuccessful trials of extubation on day 7 and 12, she had a significant cardio respiratory deterioration on day 14. She was started on second line antibiotics. Her CRP went up to 20 and her platelet count dropped to 51. Her chest x ray showed a large bullous emphysematous lesion occupying almost all of her right middle lobe (Figure 1 & 2). She became increasingly difficult to ventilate with worsening acidosis, hypotension and hyperglycemia despite maximizing intensive care support. Following discussion with her parents, her care was redirected to a palliative course. Post mortem examination of lungs revealed widespread collections of neutrophils / abscesses consistent with congenital pneumonia with abscess (seen as cavitating lesion on imaging). Her blood cultures did not reveal any growth.
Neonatal lung abscess is very rare [1] and is often of multibacterial etiology [2,3]. Predisposing factors include prematurity, assisted ventilation, congenital lung anomaly and aspiration. Given the range of potential pathogens, direct culture by percutaneous needle aspiration under either ultrasound [4] or CT guidance [2] is recommended to direct early appropriate intravenous medical therapy and hasten recovery, prevent further complications and obviate the need for surgery [4].
Competing Interests:
None.
Patient Consent:
Obtained.
References
- Siegel JD, McCracken GH (1979) Neonatal lung abscess. Am J Dis Child 133(9): 947-949.
- Levison J, Van Asperen P, Wong C, Harvey J, Halliday R (2004) The value of a CT-guided fine needle aspirate in infants with lung abscess. J Paediatr Child Health 40(8): 474-476.
- Tan TQ, Seilheimer DK, Kaplan SL (1995) Pediatric lung abscess: clinical management and outcome. Pediatr Infect Dis J 14(1): 51-55.
- Lee SK, Morris RF, Cramer B (1991) Percutaneous needle aspiration of neonatal lung abscesses. Pediatr Radiol 21(4): 254-257.






























