Formulation and Characterization of Glutathione-Loaded Bioadhesive Hydrogel for Ocular Delivery
Jingyuan Wen*, Teresa Hawke, Diana Wong, Jonathon Hwang, Katarina Jeftic, Min Hao Zhan and Jingyuan Wen
Department of Medical and Health Science, University of Auckland, New Zealand
Submission: February 20, 2019; Published: March 07, 2019
*Corresponding author: Jingyuan Wen, School of Pharmacy, Faculty of Medical and Health Science, University of Auckland, New Zealand
How to cite this article: Guanyu Chen, Teresa Hawke, Diana Wong, Jonathon Hwang, Katarina Jeftic, et al. Formulation and Characterization of Glutathione-Loaded Bioadhesive Hydrogel for Ocular Delivery. Academ J Polym Sci. 2019; 2(3): 555590.DOI: 10.19080/AJOP.2019.02.555590
Abstract
Glutathione may prevent age-related, oxidative damage to ocular tissues but has poor corneal penetration. Hydrogel formulations were investigated to determine an optimized ocular delivery system. The rheology and texture profile of formulations were investigated at 25°C. The 1% w/v glutathione was incorporated into systems demonstrating desirable characteristics for ocular vehicles and physical characteristics re-determined. In vitro cumulative glutathione delivery across the bovine cornea was measured over 8 hours at 32ºC in Franz diffusion cells. Carbopol-containing Poloxamer systems exhibited shear-thinning behavior desirable for ocular formulations whilst Polyvinyl alcohol (PVA) and Polyacrylic acid (PAA) systems exhibited Newtonian behavior. Of the glutathione-containing systems, 0.2% w/v Carbopol 1342 was the most viscous with a viscosity of 960cP at a shear rate of 100sec-1. All formulations significantly increased the amount of glutathione delivered across the cornea (relative to an aqueous solution of glutathione) with the exception of 0.1% w/v Carbopol 940 (p=0.12). Formulations containing 0.1% w/v Carbopol 934, 0.1% w/v Carbopol 1342 and 0.2% w/v Carbopol 940 improved penetration dramatically (ca. 30%); but were not significantly different from each other. Therefore, Carbopol and Poloxamer formulations demonstrated enhanced penetration of glutathione across the cornea. The 0.2% w/v C940-containing-Poloxamer formulation was determined to be the most promising for ocular delivery of glutathione.
Keywords: Glutathione; Hydrogel; Ocular delivery; Rheology; Newtonian behavior; Sustained release; Permeation
Introduction
Glutathione (γ-glutamyl-cysteinyl-glycine; GSH) is a highly hydrophilic thiol tri-peptide with a low-molecular weight of 307.4Da [1,2] The reduced form of GSH serves as a strong intracellular antioxidant [1,3] and plays an important role in the protection of the eye from oxidative stress [4]. In addition to its antioxidant activity, glutathione serves as a cofactor of enzymes involved in the degradation of peroxides, such as glutathione peroxidises. Moreover, as a component of NADPH pathway, it prevents cell components from being oxidized thus promoting DNA regulation and protein synthesis [3]. Franco et al [5] also reported glutathione’s role in the regulation of cell-cycle, signal transduction and immune response [5]. Given that all ocular tissues contain GSH as a primary antioxidant, replenishing the amounts of GSH in the eye could reduce the incidence of ocular diseases related to oxidative stress and aging, such as cataracts. The cornea is particularly susceptible to chemical insults and damage because it is the outer-most layer of the eye and therefore exposed to the harsh environment. GSH maintains normal hydration, protects the cellular membrane and degrades xenobiotic agents [4] in the cornea. Therefore, GSH may play a role in the treatment of keratitis and other corneal diseases [4].
Due to anatomical and physiological characteristics, the eye is uniquely shielded and a highly protected organ that presents many barriers to effective ocular drug delivery [6]. The main physical barriers shielding the eye are tear film and cornea, which protect the anterior of the eye, Tear film is a protective layer that prevents the entry of foreign molecules into the eye. The blood-retina barrier, which protects the back of the eye [7]. The cornea is the main barrier against drug penetration to the inner tissues of the eye due to its small surface area and relative impermeability [8]. In addition, many ocular enzymes in the cornea could degrade glutathione and prevent its therapeutic effect. These enzymes include endopeptidases (plasmin, collagenase) and exopeptidases, such as the hydrolytic aminopeptidase, which degrade amino acids [9].
The main advantages of stopical administration are its ease and convenience of use and localized drug effects, thus, reducing systemic absorption and avoiding enzymatic degradation through hepatic first pass metabolism [10]. However, the natural ocular defense mechanisms lead to poor bioavailability. Blinking increases the production of the tear film’s aqueous layer which in turn increases tear turnover to approximately 1μL/min, which is equivalent to 16% of the tear film turnover [11]. Both the removal of excess fluid and tear turnover reduce the extent of drug absorption. Conventional eye drops require frequent administration, with each drop being more than 30μl, which is estimated to be the maximum volume the eye can accommodate without overflow. Drainage of instilled solution occurs within 15-30 seconds after administration [12], therefore the majority of the drugs administered are removed before absorption. Although ocular ointments have the viscosity to increase pre-ocular drug retention time, they often cause irritability to the eye, resulting in lower compliance. In addition, their oily medium is not compatible with water soluble drugs such as GSH. Consequently, an ocular formulation with desirable characteristics that shows promising potential would be required to effectively deliver glutathione. This delivery system should prevent enzymatic degradation of glutathione, enhance its pre-corneal retention and penetration.
Hydrogels can be formed by dispersing polymers in an aqueous medium where they undergo swelling to produce a viscous gel capable of increasing pre-corneal retention time, prolonging contact time by increasing mucoadhesion and controlling drug release [12]. These properties increase trans-corneal absorption and hence the amount of drug reaching the anterior chamber of the eye. Poloxamers are non-ionic triblock copolymers comprised of ethylene oxide and propylene oxide, which are non-irritating to the ocular surface. With favorable characteristics such as strong hydrogen-bonding, high MW and sufficient flexibility to interact with the mucus network contribute to excellent mucoadhesion. Another defining characteristic include their ability to increased stability of drugs, Carbopol (CP) is a synthetic high-MW polymer comprised of acrylic acid that are cross-linked with either allyl ether of pentaerythritol or allyl sucrose [3]. They are anionic and therefore offer increased mucoadhesion hence contact time [13]. In addition, CP is reported to open the cellular tight junctions and could promote trans-corneal penetration of glutathione [14]. PVA has been used extensively in ocular formulations due to its ability to maintain ocular osmotic pressure while PAA has been widely used as a viscosity enhancer [2]. In this project, we developed a novel hydrogel formulation which composed of CP, PAA and PVA, and used as a carrier system for ocular delivery of GSH. This delivery system is aimed to enhance the permeation of the GSH over the cornea, thus, to maximize the bioavailability of GSH via ocular administration.
Materials and Methods
L-glutathione reduced≥99% was purchased from Sigma-Aldrich (USA). P407 and P188 were purchased from BASF (Germany). C934NF were from Noveon (USA) while C940NF and C1342NF polymer were purchased from Lubrizol (USA). PVA came from Applichem (Germany) and PAA was from Polyscience Inc (USA). Sodium hydroxide (NaOH) was from Scharlau (Spain). All other chemicals and solvents were of analytical grade. Bovine eyes were obtained from Auckland Meat Processors (New Zealand) and stored at20°C until required.
Methods
Preparation of Formulations
The CP formulations were prepared by adding the required amount of CP to 35mL of milli-Q water and were continuously stirred until the CP was completely dissolved. The solution was cooled to 4°C and the required amount of Poloxamer 407 (P407) and Poloxamer 188 (P188) were added with gentle stirring. The formulation was stored in the refrigerator and stirred every 30 minutes until the Poloxamers were completely dissolved. Milli-Q water was added to make up to a final volume of 50mL. The pH of the formulations was then adjusted to 7.4 by the addition of a small amount of 1M of NaOH. (Table 1) lists the samples prepared using the method mentioned above.
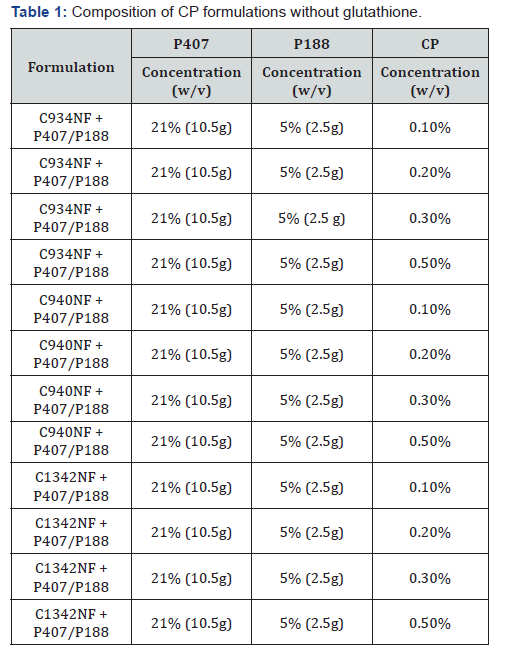
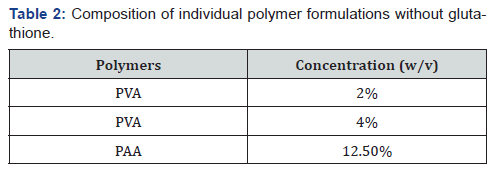
PVA formulations (Table 2) were prepared by adding the required amount (w/v) to 35mL of milli-Q water, which was then heated to 50°C under constant stirring until all PVA was dissolved and made up to 50mL with milli-Q water. The pH was adjusted to 7.4 by adding a small amount of 5M NaOH. The corresponding concentration of PAA samples were added according to (Table 2) and dilutions were made with milli-Q water. The control used in the screening of the formulations was milli-Q water.
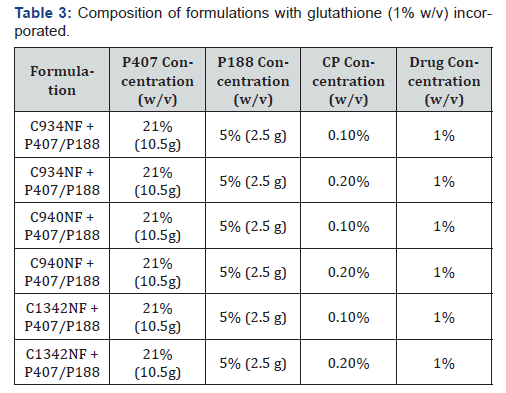
The polymer combinations were shown in (Table 3). The CP formulations containing glutathione were prepared by dissolving 0.5g of glutathione in milli-Q water. Once glutathione was dissolved, the required quantity of CP was added. The solutions were continuously stirred until CP was completely dispersed and the Poloxamers were prepared according to the method described above. The control for samples mentioned in (Table 3) was aqueous solution of glutathione. Simulated tear fluid (STF) was prepared based on the method used by Hagerstrom et al [15]. Based on the physical parameters obtained, several potential formulations with glutathione will be investigated in this study.
Characterization
Rheological Properties
The rheological properties were examined using the Brookfield DV-III+ rheometer (Brookfield Engineering Laboratories, Inc. USA) with spindle 40 for PVA and PAA samples and spindle 52 for the CP formulations. This was carried out in a temperature- controlled environment at 25±1°C to simulate average room conditions. Each sample went through 20-40 loops of shearing, in between which there was a 10 second delay. The speed of shearing increased by 5rpm at each loop and the torque was kept between 9 to 90% by manipulating the starting rpm to ensure accuracy of data. The range of rotational speed was between 1 and 394 rpm corresponding to a shear rate range between 2 and 788s-1.
Mechanical and Mucoadhesive Properties
TA-XT plus texture analyzer (Stable Micro Systems, UK) with a 5kg load cell at 25±1°C was used. Texture analyzer was calibrated. For the measurement of the mechanical properties, a 10mm diameter delrin cylinder probe was twice compressed into each formulation at the rate of 2 mms-1 to a depth of 5mm with a trigger force of 0.1g. A delay of 15 seconds was allowed between the compressions. Data collection and calculations were gathered from the Texture Exponent 3.0.5.0. The force-time plot measured mechanical properties such as hardness, compressibility, adhesiveness and cohesiveness. This experiment was conducted in triplicate.
Hardness is measured by the peak force of the first compression cycle. Compressibility is measured as the positive force area during the first compression of the probe [3,16]. Adhesiveness is the negative force area of the first compression [16]. Cohesive force of each sample is the ratio of the first and second positive force area of the two consecutive compressions.
Mucoadhesive force measurements were performed on freshly prepared bovine cornea using TA-XTplus texture analyzer (Stable Micro Systems, UK) with a 5kg load cell at 25±1°C. The cornea was stabilised on the mucoadhesion test rig. A small amount of sample was applied to the 10mm delrin cylinder probe surface, after which the probe was lowered at a constant speed of 2mms-1 and a trigger force of 5g. After 10 seconds of contact, the probe was moved away at a speed of 0.5mms-1, generating a curve. The area under the curve (AUC) was calculated by the Texture Exponent 3.0.5.0 program. The work of mucoadhesion was calculated through Equation 1[3]. Each measurement was conducted in triplicates.
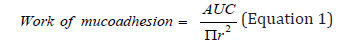
where πr² is the surface area of the cornea.
Permeability Studies
Ex-vivo drug permeation studies were performed by Franz diffusion cell (VTC 200, Logan Instrument Corp). The thermostat of the Franz diffusion cells was set at 32±1°C to mimic the ocular surface temperature. Bovine cornea is placed between the donor and the receptor chamber. Twelve mL of STF served as the dissolution medium in the receptor chamber which functioned as the reservoir. One mL of formulation was placed in the donor chamber and the cap was covered with parafilm to prevent evaporation. Samples (0.4mL) were collected at predeterminate time intervals and replaced by 0.4mL of STF for the first four hours, after which a greater amount of sample was withdrawn and replaced in order to maintain sink condition. UV spectrometer was blanked with STF at the wavelength of 215 nm and the absorbance of each sample was obtained. The absorbance for samples presented in Table 3 was measured and concentrations were calculated. In order to evaluate the penetration rate, the apparent permeability coefficient (Papp) was calculated, using the following equations:
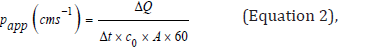
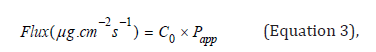
where ΔQ / Δt is the steady-state of the linear portion of the graph which presents the amount of drug in the receptor chamber versus time, A represents corneal area available for diffusion (1.766cm2), Co is the initial glutathione concentration in the donor chamber and 60 is the conversion factor from minute to second [2,17]. The linear branch of the permeation data was determined using correlation analysis. A minimum of six data points in the linear branch were taken to calculate the flux, J, (μg.cm-2s-1) by linear regression. The flux was then divided by the concentration in the donor (μg.cm-3) in order to calculate Papp (cm.s-1) [2,18].
Cryo-Scanning Electron Microscopy (Cryo-SEM)
Cryo-SEM was used to evaluate the hydrogel structure at swollen state. Images were obtained through Philips XL30S FEG (Field Emission Gun) SEM (Netherlands). Cryo unit, Gattan Alto 2500 was employed, including a fracture stage and a sputter coater, with a coating temperature of less than -120ºC. Samples were placed on a brass specimen holder and heated to allow thermogellation. The sample were frozen by using liquid nitrogen (-200ºC) and then cut and allowed to heat to -90ºC under vacuum. This allowed the frozen water in between gel pores to evaporate, generating the clear structure of polymer hydrogel. The surface of the sample was sputtered with gold for 4 minutes at -120ºC, to minimize any charge builds up, after which the samples were viewed under the cryo-SEM.
Statistical Analysis
Statistical data was analyzed using Microsoft Excel 2007, with two-way variance analysis (two-way ANOVA) and pair wise comparisons were performed using t-tests. p<0.05 indicates a significant difference.
Results
Characterization of Rheological Properties
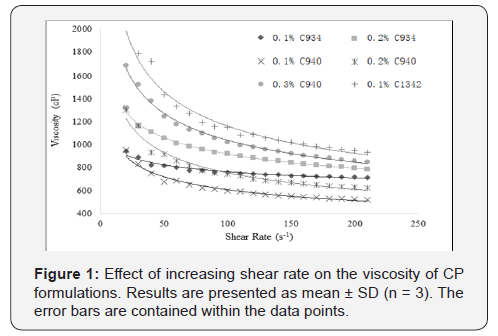
Hydrogel ocular formulations should ideally have a viscosity of around 1000-5000 cP in order to maximize pre-ocular retention time and the delivery of glutathione. Formulations with similar viscosities were plotted together for clear and apparent analysis. The 0.3% C1342 formulation was not included as it was too viscous and the method that was used to evaluate rheological properties was not suitable [19]. All CP dispersions exhibited non-Newtonian shear-thinning (pseudoplastic) behavior (Figure 1) i.e. decreasing viscosity with increasing shear rate.
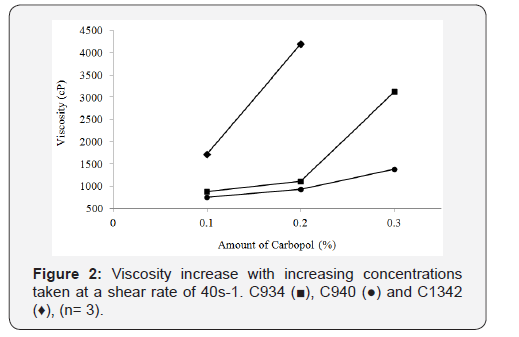
It was observed that the increase in viscosity with increasing CP concentration was proportionally similar at 0.1% and 0.2% for C934 and C940 at a shear rate of 40s-1. Conversely, C934 exhibited a much greater increase in viscosity at 0.3% compared to that of C940 (Figure 2). The viscosity difference appears to be proportional between 0.1% and 0.2% of C1342 and 0.2% and 0.3% C934 at the shear rate of 40s-1. Moreover, the 0.1% and 0.2% C940-containing formulations were the least viscous, while the respective C934 formulations appeared to be three-times more viscous than C940-containing formulations (Figure 2). The difference in viscosity between all formulations at different concentrations appears to be significant apart from that between 0.1% C934 and 0.2% C940 and between 0.1% C1342 and 0.3% C940.
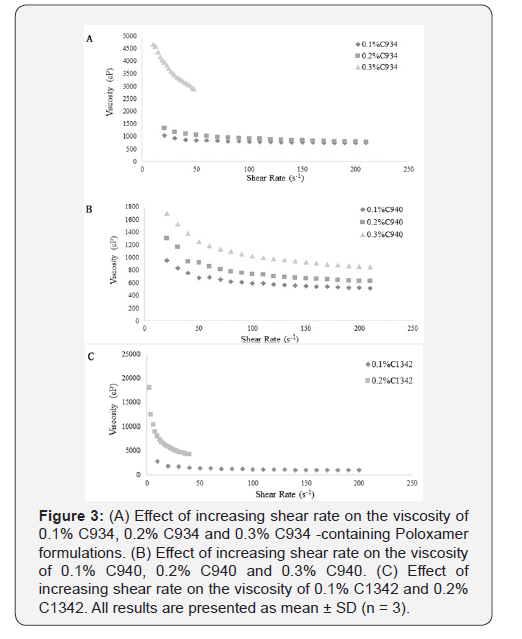
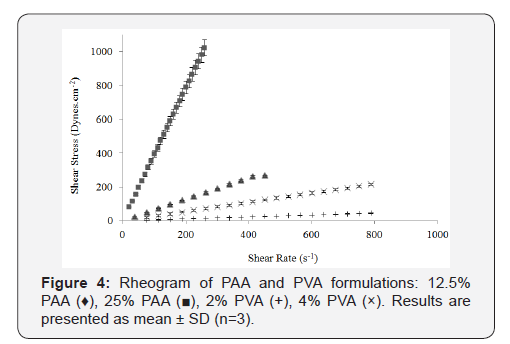
The difference in viscosity at different concentrations for each CP was statistically significant (p<0.05) (Figure 3A, 3B & 3C). The C940 exhibited the most proportional increase in viscosity with increasing concentration (Figure 3B); while the viscosities of C934 and C1342 appeared to have been more dramatically affected by the change in concentration. The rheological characteristics of PVA and PAA formulations are shown in (Figure 4). PVA and PAA results were analyzed separately from that of the CP formulations because their viscosity range was vastly different. The PVA and PAA formulations demonstrated Newtonian flow, where a linear relationship between shear rate and shear stress was evident (Figure 4) [7]. Furthermore, the Newtonian flow properties showed that the viscosity of these formulations remained constant despite increasing shear rate. The 25% PAA is approximately eight-times more viscous than the diluted 12.5% PAA and has a much higher shear stress than all the other three formulations. Similar to the CP systems, the viscosity of PAA and PVA also increased with increasing concentration. Again, there was a significant difference between the viscosities of these simple chain polymers where PAA appears to be more viscous than PVA. The 25% PAA displays a viscosity which is comparable to 0.1% C940-Poloxamer formulation after shearing (Figure 2).
Based on the optimal ocular formulation characteristic described by existing literatures available, the formulation demonstrating the most desirable rheological properties contains the 0.2% C940, it exhibited the lowest viscosity at the lowest shear rate investigated.
Characterization of mechanical and mucoadhesive properties
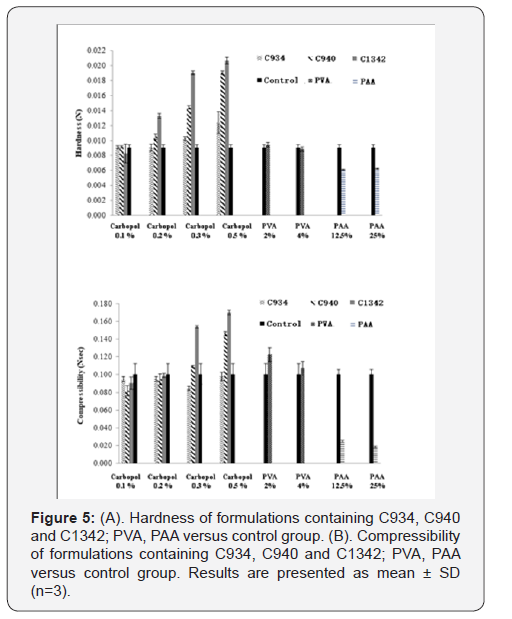
The hardness and compressibility of the hydrogel system during formulation screening increased with an increase in CP concentration. This trend can be observed for all CP-containing formulations (Figure 5A & 5B). Significant increase in hardness for C940 and C1342-containing systems was observed at concentration of 0.2% compared to concentration of 0.1% and there was significant difference compared to control (p<0.05). However, no significant differences between the CP systems and control at 0.1% (p>0.05) were observed. At 0.3% and 0.5%, all CP systems were significantly different, compared to control (p < 0.05). Conversely, PVA showed no distinctive change compared to control and no significant differences between the different concentrations was observed (p>0.05). PAA exhibited a significantly lower hardness compared to control (p<0.05), however, there was no difference when concentration was doubled. The hardness of the hydrogel in the presence of PVA was no different when it was compared to all 0.1% CP formulations (p>0.05). The results obtained were comparable to the previous literature data [20]. The compressibility of the hydrogel in the presence of C1342 at 0.3% and 0.5%, as well as C940 0.5%, was significantly different when compared against control (p<0.05). Similar to hardness, PAA showed a significantly lower compressibility in comparison to control (p<0.05).
A relationship exists between the increase in adhesion and a decrease in cohesion of formulations (Figure 6A & 6B), with a concentration increase. At 0.1%, C1342-containing formulations were significantly higher compared to control (p<0.05). However, adhesion of all CP-containing formulations increased with an increase in concentration. Conversely, for PVA and PAA formulation, no such trend can be observed with increase in concentration, and statistical analysis showed no significant difference when compared to control (p > 0.05). At 0.1%, 0.2% and 0.3% of C934 and C94 containing systems, the cohesive forces were significantly higher when compared to control (p<0.05), but this was not demonstrated at a concentration of 0.5% (p>0.05). Cohesion of 0.1% and 0.2% of C1342-containing formulations were significantly higher to control (p < 0.05). The cohesion forces of 0.1%, 0.2% and 0.3% of C934-containing formulations were significantly different compared to 0.5% of C1342, C940 and 0.1% of C940 respectively (p<0.05). The PVA and PAA formulations demonstrated higher cohesive forces than control (p<0.05) and showed a concentration dependent relationship similar to the CP formulations. There was no significant difference in cohesion between PVA and control (p>0.05), but both PAA concentrations had significantly lower cohesion compared to control (p<0.05).

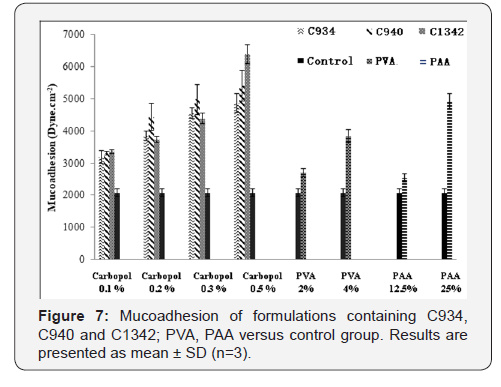
The measured apparent mucoadhesion showed a difference between the control and all formulations screened (Figure 7). It also showed a consistent increase in mucoadhesive force with increase in concentration, however, there was no significant difference between different CPs at concentrations 0.1% and 0.3%. At 0.2%, only apparent mucoadhesion of C940 was significantly different to that of other CPs. At 0.5% all CP formulations were significantly different from each other. PVA and PAA showed a similar trend, PAA at 25% obtained similar results to 0.5% C934 containing formulation.
Corneal permeability studies

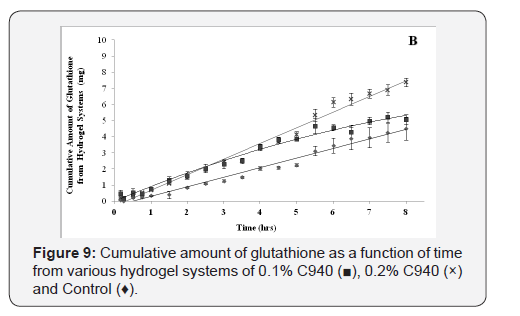
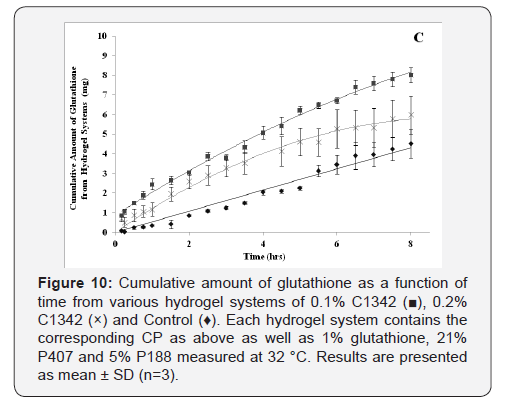
The cumulative diffusion profiles of each various hydrogel formulations of glutathione over eight hours are shown in (Figure 8-10). All of the hydrogel systems showed a linear diffusion trend and showed a significantly higher diffusion when compared to the control (p<0.05). The permeation of 0.1% C940 formulation was significantly less than 0.1% C934, 0.1% and 0.2% C1342 (p<0.05). The remaining formulations did not show any differences when compared to each other. The ranking order of the different formulation groups in their ability to promote glutathione diffusion across bovine cornea is: 0.2% C940 and 0.1% C1342 > 0.1% C934, 0.2% C1342 and 0.2% C934 > 0.1% C940 > Control.
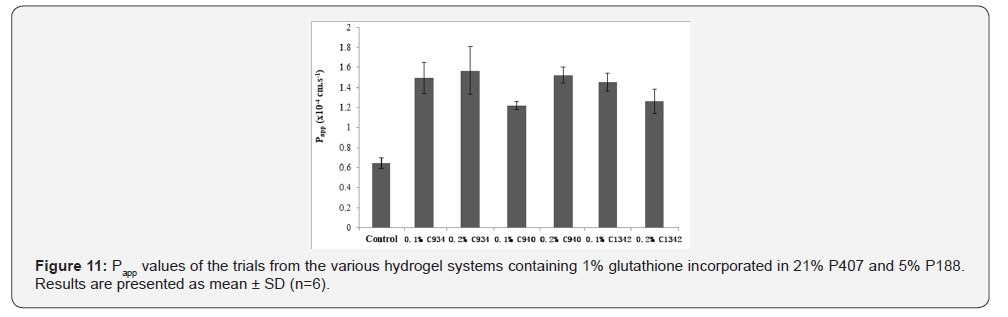
The apparent permeability coefficient (Papp) and Flux values were calculated and shown in (Figure 11). From the Papp of the different formulations measured, the permeability of glutathione was increased compared to water (p<0.01). The 0.2% C940 (p=0.03) and 0.1% C1342 (p=0.05) had an approximately 1.2-fold higher corneal permeability than 0.1% C940. All other hydrogel formulations did not show differences in their permeability (p > 0.05). The average Papp values of the hydrogels were in the range of 1.21-1.57 × 10-4 cm.s-1 compared to 0.64×10-4cm.s-1 produced by the control. This shows that the CP combinations enhance the permeability of drug by up to a 2.4-fold (p<0.05).
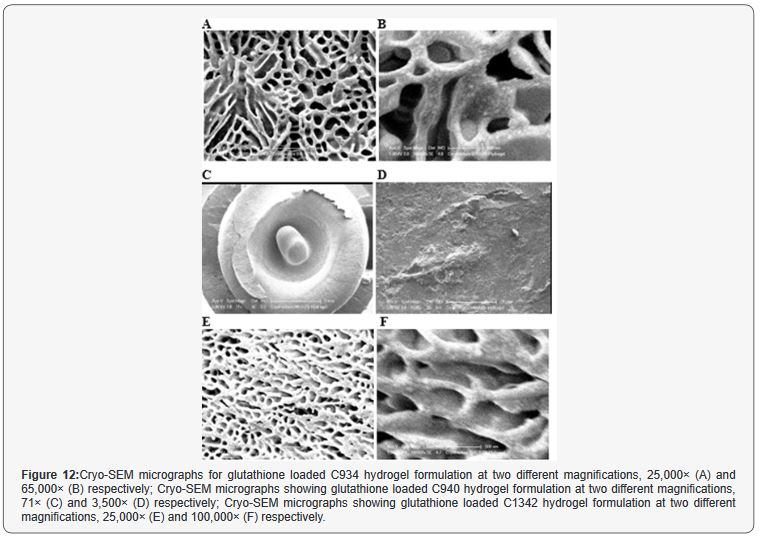
The Cryo-SEM images demonstrate the polymeric structure of the achieved CP hydrogel systems. Images of C934 and C1342 hydrogel systems with incorporated glutathione were obtained (Figure 12). Although, attempt was made to obtain images of C940 hydrogel structure, this could not be achieved due to experimental error. An air bubble was formed during preparation and, as it was cut, no formulation remained on the metallic rib for imaging; thus, the images of C940 hydrogel structure were not obtained and displayed.
Discussion
In order to increase the bioavailability of glutathione (and hence achieve post-corneal concentration), the pre-corneal residence time or penetration of the ocular formulation must be extended beyond that of the conventional formulations [21]. This may be achieved by increasing the viscosity, spreadability or mucoadhesion of the formulations; or by incorporating permeation enhancing materials into the formulation. The simplest approach is to enhance the viscosity because a two-fold increase in maximum bioavailability of a drug can be achieved. Therefore, viscosity is often considered as the major factor influencing ocular retention [12]. The increase in retention time of instilled formulations is apparent, once viscosity is greater than 10mPas but a very high viscosity results in ocular discomfort and epithelial damage can occur from blinking [22]. The difference in the effective number of polymers evaluated was likely the reason for the higher shear stress observed in this experiment. Upon the addition of NaOH solution to adjust pH to 7.4, carboxyl groups on the carbomers (pKa 3-5) are ionized, leading to electrostatic repulsion and dramatically increasing the rigidity of the formulation structure [23]. Thus, the ionized carboxylic groups could have also interacted with the small but very positive sodium ions, leading to a reduction in viscosity and shear stress. This theory could have been validated had the rheological characterization been carried out at both pH 5 and pH 7. Although Davies et al. [12] found the viscosity profile of PVA to be pseudoplastic in contrast to our findings; the conditions they used were extreme (85oC) and would not occur in the eye. Moreover, Davies et al. [12] prepared their PVA solution with PBS, introducing ions that possibly change the interactions between the molecules. Nevertheless, C934 was found to have greater viscosity-enhancing capability than PVA. Structurally, PAA are CPs without cross-link units and can be described as linear polymers (pKa~4.5) [24]. Although PAA has similar rigidity as the carbomers, it is less viscous because the strength provided by cross-links is much more robust.
The structures of hydrogels are highly dependent upon the interaction between the polymers and the swelling medium [25]. The mechanical properties of the hydrogel formulations were assessed through hardness, compressibility, adhesion and cohesion. The ability to prolong ocular contact time was measured through its strength of mucoadhesion [20,26,27]. The hardness is desired to be low in order for the formulation to be easily administered onto the ocular surface [27,28]. Therefore, lower concentrations of CP formulations (0.1% and 0.2%) are favoured. The “hardness” of anionic gels is dependent on the molecular network density and the degree of cross-linking, which is correlated to the polymer concentration, as well as viscosity [29-31]. C1342-containing hydrogels exerted the highest “hardness” out of all three CPs. This is likely to be due to increased cross-linking between its long alkyl methacrylate chain and allyl ethers of pentaerythritol and its high molecular weight compared to C934 and C940 [32]. Similarly, C934 with relatively lower molecular weight was the easiest formulation to deform due to its reduced rigidity. Additionally, surface molecules have a net inward force due to the cohesive forces being stronger than adhesive forces with the air, therefore a surface energy is created in parallel to the surface. This requires energy to break, which would have been measured as hardness [33-35]. The hardness of PAA was lower than the control. This may be explained through the accumulation of PAA molecules on the surface, which would push the liquid molecules into the bulk, leading to reduction in surface tension [33,34]. Compressibility claimed to measure the ease of spread of the formulations over the corneal surface; where a lower value was favorable. With increasing concentration, total resistance was greater hence more force was required as the parameter quantifies deformation under shear and compression [28]. The claimed “cohesion” is described as the spatial reformation of the hydrogel structure after successive compressions. It attempted to measure the relaxation of the polymers, which is dependent on time and the deformation [36]. The “cohesion” of the formulation hoped to examine the ability of the hydrogel to reform its structure after application to the ocular surface, where a high value was desired for maintenance of its structural integrity [27]. A general decline in cohesive force is shown with increase in concentration, which is due to the increase in mass of the polymers [37]. The adhesion is defined to be the interaction between different molecules within the hydrogel. This estimates the ability of the formulation to adhere to the target site [20]. At higher concentrations, there were more polymers present with greater capability to form chemical bonds [19]. The results showed a plateau at concentrations 0.3% and 0.5% for all CP-containing formulations. This may be explained by the high cohesive forces within the hydrogel structure to prevent adhesive forces forming with the probe [28]. The degree of mucoadhesion is dependent on the hydration, anionic charges, molecular weight and cross-linking of the polymer [32,38]. All CP-containing formulations were combinations of Poloxamers and CPs. This combination increased its mucoadhesive properties as the polyether components of Poloxamers were able to form tertiary carbon bonds with polyacrylic acid units of CPs, which may potentially expose different binding groups to increase mucoadhesive interactions [34,39]. Moreover, the CP-containing systems at 0.1% and 0.2% had a greater degree of swelling, therefore increased hydration. The polymers are flexible and free to diffuse to come in close contact with the corneal surface and interpenetrate with the mucus layer, to create a strong entangled network through non-covalent interactions [19,38].
The cumulative amount of glutathione that diffused across the cornea from the original administered dose (1mL), after eight hours ranged from 50.6% to 80.1% from the hydrogels compared to 45.0% from the control system. This is very high compared to the 5% or less, which is typically seen to reach the aqueous humour in living human eyes [40]. This is due to the absence of other ocular barriers such as tear turnover, tear dilution, lacrimation and nasal lacrimal drainage in the Franz diffusion cell apparatus [40]. The glutathione control group follows a linear trend across the corneal epithelial membrane and represents zero-order kinetics where diffusion was at a constant rate throughout the experiment. Conversely, the glutathione-loaded CP-containing hydrogels show a biphasic release profile. The initial phase was attributable to the release of glutathione from the outer pores of the gel surface and the second phase showed the sustained release of glutathione from the matrix of the polymer. This release profile shows benefits on application, rapid diffusion of glutathione through the corneal epithelial membrane will occur, followed by a sustained diffusion over time.
Conclusion
Glutathione is a potent anti-oxidant that is essential in the maintenance of tissue health. By replenishing the tissues with glutathione, it is hoped that the progression of ocular damages can be halted or even reversed. Hydrogels composed of CPPoloxamer, PAA and PVA were formulated and investigated as potential delivery systems for glutathione across the cornea. The CP-Poloxamer combinations exhibited favourable pseudoplastic behavior and cohesion/adhesion properties. These were further investigated for their ability to increase glutathione permeability across excised bovine corneas using a Franz diffusion cell. Penetration of glutathione across the cornea was significantly increased compared to the plain drug solution. The 0.2% C940- containing-Poloxamer formulation was determined to be the most promising for ocular delivery of glutathione. To study the efficacy of glutathione formulations on the reversibility of cataracts, in vivo tests can be performed in the future.
References
- Chen G, Wen J (2018) Poly (lactic-co-glycolic acid) based double emulsion nanoparticle as a carrier system to deliver glutathione sublingually. J Biomed 3: 50-59.
- Chen G, Wen J (2018) Poly (lactic-co-glycolic acid) based double emulsion nanoparticle as a carrier system to deliver glutathione sublingually. J Biomed 3: 50-59.
- Chen G, Bunt C, Wen J (2015) Mucoadhesive polymers‐based film as a carrier system for sublingual delivery of glutathione. Journal of Pharmacy and Pharmacology 67(1): 26-34.
- Ganea E, Harding JJ (2006) Glutathione-related enzymes and the eye. Current eye research 31(1): 1-11.
- Franco R, Schoneveld OJ, Pappa A, Panayiotidis MI (2007) The central role of glutathione in the pathophysiology of human diseases. Archives of physiology and biochemistry 113(4-5): 234-258.
- Gaudana R, Jwala J, Boddu SH, Mitra AK (2009) Recent perspectives in ocular drug delivery. Pharmaceutical research 26(5): 1197-1216.
- Martin AN (2006) Martin’s physical pharmacy and pharmaceutical sciences: physical chemical and biopharmaceutical principles in the pharmaceutical sciences: Lippincott Williams & Wilkins.
- Davies NM (2000) Biopharmaceutical considerations in topical ocular drug delivery. Clinical and experimental pharmacology and physiology 27(7): 558-562.
- Attar M, Shen J, Ling KH, Tang-Liu D (2005) Ophthalmic drug delivery considerations at the cellular level: drug-metabolising enzymes and transporters. Expert opinion on drug delivery 2(5): 891-908.
- Chen G, Li D, Jin Y, Zhang W, Teng L, et al. (2014) Deformable liposomes by reverse-phase evaporation method for an enhanced skin delivery of (+)-catechin. Drug development and industrial pharmacy 40(2): 260- 265.
- Wu G, Fang YZ, Yang S, Lupton JR (2004) Turner ND Glutathione metabolism and its implications for health. The Journal of nutrition 134(3): 489-492.
- Davies NM, Farr SJ, Hadgraft J, Kellaway IW (1991) Evaluation of mucoadhesive polymers in ocular drug delivery. I Viscous solutions. Pharmaceutical research 8(8): 1039-1043.
- Asane G, Rasal KB, Naik AA, Mahadik MS, Rao YM, et al. (2008) Polymers for mucoadhesive drug delivery system: a current status. Drug development and industrial pharmacy 34(11): 1246-1266.
- Hosmani AH, Thorat Y, Kasture P (2006) Carbopol and its pharmaceutical significance: a review. Pharmainfo net 4(1).
- Hägerström H, Paulsson M, Edsman K (2000) Evaluation of mucoadhesion for two polyelectrolyte gels in simulated physiological conditions using a rheological method. European Journal of Pharmaceutical Sciences 9(3): 301-309.
- Cevher E, Sensoy D, Taha MA, Araman A (2008) Effect of thiolated polymers to textural and mucoadhesive properties of vaginal gel formulations prepared with polycarbophil and chitosan. Aaps Pharmscitech 9(3): 953-965.
- Muchtar S, Abdulrazika M, Peryb JF, Benitaa S (1997) Ex-vivo permeation study of indomethacin from a submicron emulsion through albino rabbit cornea. Journal of controlled release 44(1): 55-64.
- Chen G, Svirskis D, Lu W, Ying M, Huang Y, et al. (2018) N-trimethyl chitosan nanoparticles and CSKSSDYQC peptide: N-trimethyl chitosan conjugates enhance the oral bioavailability of gemcitabine to treat breast cancer. Journal of Controlled Release 277: 142-153.
- Jones DS, Woolfson AD, Brown AF (1997) Textural analysis and flow rheometry of novel, bioadhesive antimicrobial oral gels. Pharmaceutical research 14(4): 450-457.
- Cevher E, Taha MA, Orlu M, Araman A (2008) Evaluation of mechanical and mucoadhesive properties of clomiphene citrate gel formulations containing carbomers and their thiolated derivatives. Drug Delivery 15(1): 57-67.
- Asane GS, Nirmal SA, Rasal KB, Naik AA, Mahadik MS, et al. (2008) Polymers for mucoadhesive drug delivery system: A current status. Drug development and industrial pharmacy 34(11): 1246-1266.
- Zhu H, Chauhan A (2008) Effect of Viscosity on Tear Drainage and Ocular Residence Time. Optometry and Vision Science 85(8): 715-725.
- Chen G, Svirskis D, Wen J (2015) Development and validation of a stability indicating isocratic HPLC method for gemcitabine with application to drug release from poly lactic‐co‐glycolic acid nanoparticles and enzymatic degradation studies. Journal of Pharmacy and Pharmacology 67(11): 1528-1536.
- Riley RG, John D Smart, John Tsibouklisa, Peter W Dettmarb, Frank Hampson, et al. (2001) An investigation of mucus/polymer rheological synergism using synthesised and characterised poly (acrylic acid) s. International journal of pharmaceutics 217(1-2): 87-100.
- Le Bourlais C, Acar L, Zia H, Sado PA, Needham T, et al. (1998) Ophthalmic drug delivery systems recent advances. Progress in retinal and eye research 17(1): 33-58.
- Yaprak Karavana S, Guneri P, Ertan G (2009) Benzydamine hydrochloride buccal bioadhesive gels designed for oral ulcers: Preparation, rheological, textural, mucoadhesive and release properties. Pharmaceutical Development and Technology 14(6):623- 631.
- Cevher E, Sensoy D, Taha MA, Araman A (2008) Effect of Thiolated Polymers to Textural and Mucoadhesive Properties of Vaginal Gel Formulations Prepared with Polycarbophil and Chitosan. AAPS PharmSciTech. 9(3): 953-965.
- Jones DS, Woolfson AD, Brown AF (1997) Textural, viscoelastic and mucoadhesive properties of pharmaceutical gels composed of cellulose polymers. International journal of pharmaceutics 151(2): 223-233.
- Jones DS, Woolfson AD, Djokic J (1996) Texture profile analysis of bioadhesive polymeric semisolids: mechanical characterization and investigation of interactions between formulation components. Journal of Applied Polymer Science 61(12): 2229-2234.
- Tamagawa H, Nogata F, Yagasaki K (2004) An interpretation of amphoteric gel hardness variation through potential and hardness measurement. Journal of colloid and interface science 275(1): 107- 112.
- McTaggart LE, Halbert GW (1993) Assessment of polysaccharide gels as drug delivery vehicles. International journal of pharmaceutics 100(1-3): 199-206.
- Blanco Fuente H, Anguiano Igea S, Otero Espinar FJ, Blanco Méndez J (1996) In-vitro bioadhesion of carbopol hydrogels. International journal of pharmaceutics 142(2): 169-174.
- Aulton ME (2007) Aulton’s pharmaceutics: the design and manufacture of medicines. Edinburgh; New York: Churchill Livingstone, USA, p. 717.
- Sinko PJ, Martin AN (2006) Martin’s physical pharmacy pharmaceutical sciences: physical chemical principles in the pharmaceutical sciences. (5th edn), Philadelphia: Lippincott Williams & Wilkins, USA, p. 795.
- Schwartz AM, Chatterjee PK, Gupta BS (2002) Chapter II Surface tension and surface energy, in Textile Science and Technology. Elsevier 13: 1-484.
- de Cindio B (1984) Stress relaxation of polymer melts subjected to large uniaxial tension. Polymer 25(7): 1049-1053.
- Jones DS, Woolfson AD, Djokic J, Coulter WA (1996) Development and mechanical characterization of bioadhesive semi-solid, polymeric systems containing tetracycline for the treatment of periodontal diseases. Pharmaceutical Research 13(11): 1734-1738.
- Ludwig A (2005) The use of mucoadhesive polymers in ocular drug delivery. Advanced drug delivery reviews 57(11): 1595-1639.
- Qi H, Chen W, Huang C, Li L, Chen C, et al. (2007) Development of a poloxamer analogs/carbopol-based in situ gelling and mucoadhesive ophthalmic delivery system for puerarin. International journal of pharmaceutics 337(1-2): 178-187. Gaudana R, Jwala J, Boddu SH, Mitra AK, (2009) Recent Perspectives in Ocular Drug Delivery. Pharmaceutical Research 26(5): 1197-1216.






























