Rhomboid Flap: Best Option for Skin Defects of All Sizes? A Comprehensive Review of Literature
Ajaipal S. Kang, MD FACS and Kevin S Kang BS
1MD FACS, Department of Surgery, UPMC Hamot, United States
2BS, Geisel Dartmouth Medical School, United States
Submission:March 05, 2020; Published: April 03, 2020
*Corresponding author:Ajaipal S. Kang, MD FACS, Chairman, Department of Surgery, UPMC Hamot, Erie, Pennsylvania, USA
How to cite this article:Kang A S, Kang K S. Rhomboid Flap: Best Option for Skin Defects of All Sizes? A Comprehensive Review of Literature. Open Access J Surg. 2020; 11(4): 555817. DOI:10.19080/OAJS.2020.11.555817.
Abstract
Surgical resection remains the mainstay treatment for cutaneous malignancies resulting in skin defects. Traditionally, the concept of the reconstructive ladder suggests that primary closure and skin grafting should be considered first in reconstruction. However, these techniques may lead to increased likelihood of dehiscence, distortion of key structures, poor cosmetic outcomes and less-than-total graft acceptance. To overcome these limitations, various local skin flaps and tissue rearrangement techniques have been developed, including rhomboid flap. This flap is quickly and easily designed, does not require any special instruments and provides excellent contour, texture, thickness, color match, long-term good cosmesis and high patient satisfaction. The following article presents a comprehensive review of rhomboid flaps in the English literature. Nearly 100 years after it was first described by AA Limberg in 1928, the time has come to embrace this simple and elegant flap as the preferred method of reconstruction of cutaneous defects of any size and any part of the body.
Keywords:Rhomboid flap; Limberg reconstruction; Skin cancer; Cutaneous defect; Transposition; Local flap
Abbreviations: RSTL: Relaxed Skin Tension Lines
Introduction
Traditionally, the concept of the “reconstructive ladder “suggests that primary closure of a defect should be considered first in reconstruction. However, a considerable number of cases are not eligible for primary closure. In these circumstances, local flaps become the best option. Although defect size is a limiting factor, the texture, pliability and color match of a local flap favor its use. Of local flaps, a rhomboid flap is a popular flap that can be used to reconstruct defects in any part on the body [1].
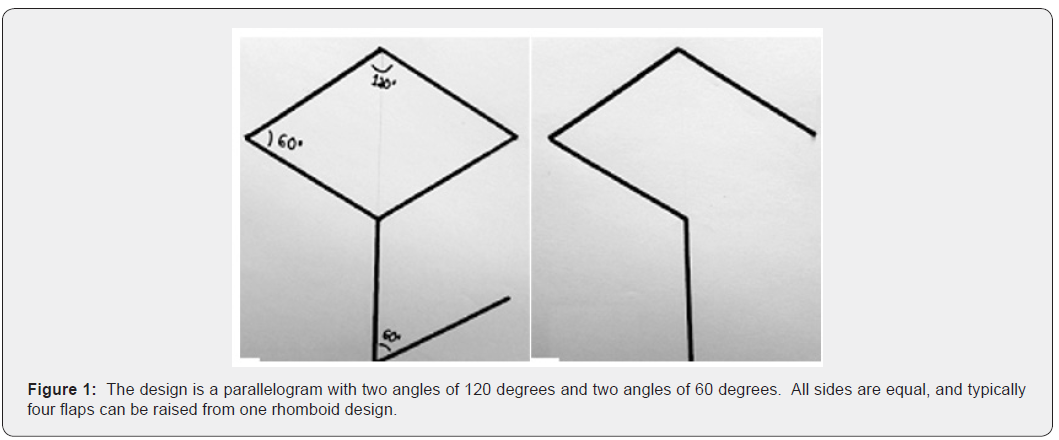
The rhomboid flap design was first described by Professor Alexander Alexandrovich Limberg of Leningrad in 1928. The first description in English language was a chapter in Modern Trends in Plastic Surgery in 1963 [2]. The design is a parallelogram with two angles of 120 degrees and two angles of 60 degrees. All sides are equal, and typically four flaps can be raised from one rhomboid (Figure 1). The technique of elevation is simple. The application of this flap has been described in almost all parts of the body with extreme safety and good cosmetic result [3]. Flaps are full thickness cutaneous local flaps with random blood supply. Typically, they rely on dermal-subdermal plexus of blood supply [4]. The final quality of the scar is related to the underlying tension. When a scar is parallel to Relaxed Skin Tension Lines (RSTL), tension is exerted along its axis, and new collagen is oriented in this direction. Ultimately, this results in a narrower scar. Less tension at 3 weeks results in an improved scar [5].
Over the years, several modifications have been reported. The “diamond” flap modification was shown to be employed with no complications and no hypertrophic scars in 44 patients [4]. Claude Dufourmental [6] proposed a modification which widens the pedicle width and increases flap safety [6]. Quaba [7] proposed a modification to cover circular defects in 1987 [7].
Rhomboid flaps can be used anywhere, without any limitations that are due to defect etiology, age or other patient factors. This flap has been described in head and neck regions, and reconstruction, breast reconstruction and pilonidal sinus reconstruction [1].
Discussion
History
While AA Limberg’s first publishing on the innovative rhomboid transposition flap was in 1928, his first treatise in English was a chapter in Modern Trends in Plastic Surgery, edited by Thomas Gibson in 1963 [3]. Since that time, rhomboid flap has been widely used worldwide in clinical practice. The term flap originates from the Dutch word “flappe”, meaning something suspended extensive and loose, attached only by one side, referring to keeping its blood supply by the pedicle [8]. Defect closure by primary intention and grafts may offer satisfactory outcomes for some locations. But rhomboid flap is easy to learn and relatively simple to perform and can be used at any site on the body surface [9]. For a plastic surgeon, it embodies the artistic eye meeting the science of cutaneous biomechanics [10].
Flap design and orientation
The rhomboid flap is a flap of skin and subcutaneous tissue that is rotated around a pivot point into an adjacent defect [11]. Traditionally, as many as four flaps can be raised from one rhomboid, if required [3]. The flap’s pedicle maintains subpapillary and sub-dermal vascular plexuses to provide superior results when compared to skin grafts of similar size and location [10,12]. A reduction in tension on the flap decreases the likelihood of necrosis of the donor tissue [13]. The flap should be positioned in the direction of minimal tension and maximum extensibility. Placement of incisions parallel to Relaxed skin tension lines (RSTL) allows the resulting scar to fall within the creases of the skin along line of maximal extensibility [9,14-19].
Primary closure versus rhomboid flap
A lesion should be excised as necessary without considering the shape of the defect produced [7]. Although reconstructive ladder provides a basic framework, there are no established guidelines for reconstruction of tissue defects. For any given defect, a host of closure techniques are available; experience and personal preference must be the deciding factors [20-23]. After excision, primary closure should be considered but if that would lead to distortion and contour deformity of key structures, a local flap should be considered [24].
Although a very common pattern of management of skin tumors is fusiform elliptical excision and primary closure, there are several problems with this technique. The major issue is central depression leading to a flat contour, and unsightly dog ears with peaking on both ends. If the dog ears are excised, it leads to a longer scar [7,25,26]. In addition, to avoid dog-ear deformity, length to width ratio of 3:1 is needed but leads to a much longer linear scar and also leads to loss of reconstructive options [24]. Direct primary closure can result in scars that are 3-4 times longer than the original length of the lesion. According to another study, compared with original defect size, a mean of 130% of healthy skin is wasted in an elliptical design [27,28]. These problems are even more exacerbated in areas of insufficient skin redundancy and more tension, such as near the joint [7,25,26]. Considering the tension of the skin, primary closure can cause an increase in dehiscence and infection in defects. Also, the longer conspicuous scars may have considerable impact on the quality of life of the patient [29].
These are some of the problems that have led to the development of local flaps as an alternative to fusiform excision of small skin lesions [25,26,30]. Rhomboid flaps have shown great effectiveness over primary closure in the literature [31,32]. One explanation for superiority of rhomboid flap closure versus elliptical excision and direct closure is better distribution of tension in the former. The tension at point of maximum tension is less in rhomboid flap because it allows the surrounding skin to participate in closure [7]. Also, the line of donor closure is placed along line of maximal extensibility leading to less tension on the flap [24]. Studies reveal that the pilonidal surgical procedures that healed with tension-free primary closure had greater disadvantages than wounds that healed using the rhomboid flap [33,34].
Another explanation is avoidance of distortion of key structures. Rhomboid flaps allow the tension force to be cancelled on the medium portion of the defect, minimizing the risk of distortion of the anatomic architecture [10,22]. If the defect is close to a structure or an organ, the flap design should consider appearance and function of the organ [16,35,36]. Borges suggested that in facial reconstructions, even for small lesions, cutaneous flaps are preferable to primary closure and/or grafting, with the purpose of avoiding distortions of adjacent structures and breaks in scar lines [37,38].
The only landmark article for comparison of rhomboid flap and primary closure was published as a meta-analysis of randomized controlled trials. The authors used the defect left behind after excision of sacrococcygeal pilonidal disease. 641 patients were included with rhomboid flaps demonstrating statistically significant trend towards lower wound infection and dehiscence. Primary wound closure resulted in significant wound tension resulting in wound dehiscence and final conclusion was that the rhomboid flap was superior to primary closure [39]. These considerations lead Chasmar [3] to propose that the rhomboid flap, single or multiple, can be applied with extreme safety and should be the “first choice for many full thickness defects” [3].
Advantages of Rhomboid Flap
The local flaps are often preferred due to their similarity in skin characteristics to the adjacent defect. The local flaps entail transposition or rotation flap designs. Local rhomboid flap is an example of such a transposition flap and has historically been used in small defects [15]. Flaps are developed to protect the function of surgical area, reduce the tension and postoperative complications and beautify the appearance [16].
A well-planned rhomboid flap with scars parallel to tension lines maintains continuity of texture, color, thickness and vascularity with the surrounding tissue, eliciting the most successful functional and aesthetic outcome [15,17,18]. This single flap design can be used to close defects almost anywhere on the body [3]. While certain closure techniques are invasive and involved, rhomboid flaps are associated with a good prognosis and rapid healing time [19]. The technique of its elevation is simple. Its minimally invasive, quick to perform, and suitable to be easily performed in a single stage under local anesthesia [18]. The elevated flap requires sufficient subcutaneous fat, and dissection must be carried past its base to prevent an elevated bump when it is transposed [3].
Also, the resultant scar is geometric broken lines that is less noticeable than longer linear primary closures [10,20,21]. The scar’s acute “broken” angles, make the risk of scar complications, such as trapping and hypertrophy, extremely low. This makes it an attractive option for pediatric patients and/or those with a history of pathological scarring [15,22].The position of the scars resulting from the flap transposition is highly foreseeable and the secondary defect scar can be hidden in a relaxed skin tension line (RSTL), making it less apparent [18,21]. The advantages are closure of defects that otherwise close under high tension or distort the nearby structures leading to functional or aesthetic impairment. The rhomboid flap has a low rate of complications, including epitheliolysis with partial necrosis of the flap, hematoma and bacterial infection [18,22]. Such advantages are a common reason why these flaps are one of the first techniques used by surgeons [3]. Chasmar [3] reports on the versatility of Rhomboid flaps and demonstrates how a single flap can be used to close defects almost anywhere on the body [3].
Where is a Rhomboid Flap Used?
It can be used in virtually any part of the body, and it is widely used in facial and breast reconstruction, neurosurgery, hand surgery, ophthalmology, and proctology [3]. Rhomboid flaps can be used anywhere, without any limitations that are due to defect etiology, age or other patient factors [1,3,15]. Tumor resections is the primary etiologic factor for this flap and this flap is commonly used in hand, breast and pilonidal sinus reconstruction [1].
Chasmar [3] gives examples of its application in skin cancer, lupus, cystic acne, spina bifida. The special application for eyelid, floor of nose, alar rim and chin defects are highlighted [3,15]. Alvarez et al. [15] reports the face was the most commonly affected, followed by the lumbosacral region, and by the dorsal, inguinoscrotal regions, anterolateral arm, thorax, shoulder, and supraclavicular region [15]. Another study shows success of local flaps in thigh, upper arm, forearm and back [22,25]. The Rhomboid flap has shown to be one of the quickest and least complicated treatments for wound healing in pilonidal sinus surgery [40,41]. Tissiani et al. [28] reports a series of this flap used for reconstruction of face, trunk, lower limb and upper [28]. Its commonly agreed that skin defects of extremities are difficult to cover. Therefore, these flaps are used for reconstruction for extremity defects [42].
Rhomboid and Local Flap Series in Literature
Becker stated that skin flaps have become the preferred method of facial reconstruction [14,20]. There are numerous reports in the literature reporting use of rhomboid flap for closure of small to large defects in several anatomical areas, achieving satisfactory results. Aydin et al reports a series indicating that rhomboid flaps can be safely used to reconstruct small to moderately sized skin defects [1]. Quaba [7] in his rhomboid flap series of 400 patients, calls this versatile flap the “workhorse for facial reconstructions” [7].
The predictability, high safety degree, low complication rate and tension free closure, makes rhomboid flap the first option for great majority of reconstructions [15,22]. A single institution experience in 70 patients treated for facial malignancies, revealed local flaps gave the best results and were the first choice of reconstruction of the face. The study notes that smooth contour and scar quality are very important for Plastic Surgery patients. The proper execution does require considerable technical skills and expertise [41,43-45].
Li et al. [30] published a series of 48 patients, 25 cases of benign pigmented nevi, with defect diameters of 0.9cm to 11cm which were treated with local flaps where 41 patients achieving satisfactory postoperative results [30]. Another series of 21 patients, with small benign skin lesions with defect diameters of less than 1 cm were treated with local flaps with all patients achieving satisfactory postoperative results [30]. A series of 27 patients who underwent a medial canthal reconstruction with a rhomboid flap showed healing with no major complications and re-operations [21].
Alvarez et al states that the great number of facial reconstructions in the temporal-zygomatic and malar regions (44% of the facial defects) demonstrates the versatility of the rhomboid flap in this area, and that it is the preferable technique in these facial units. There were very few complications in this study, which demonstrates the safety of the rhomboid flap for the most varied reconstructions of defects [15].
A series of 35 flaps for reconstruction after cutaneous malignancy resection, revealed excellent outcomes.44 A series of 30 patients of rhomboid flaps healed without any significant complications [13]. Tissiani et al. [28] published a series of 45 double transposition flap used for reconstruction of face, trunk, lower limb and upper limbs revealed a 15% complication rate. Small defects accounted for 70% of the cases and major defects constituted 11% of cases with largest defect being 107 cm [28]. Another series of 175 reconstructions reported a complication rate of 9.1%. The more common complications included infection, hematoma, partial necrosis and partial dehiscence [7].
We believe every case should be approached in an individual manner as no two patients, nor two defects are the same [8]. Reconstruction of each defect should be tailored to the unique characteristics of the defect, patient expectations and surgeon experience [46]. Patients, particularly Plastic Surgery patients, have shown a tendency to focus on both cosmetic and functional outcomes after surgery, thus the choice of reconstructive technique should focus on cure while minimizing scars [47,48]. Of note, the senior author has extensive successful experience in using rhomboid flap design in reconstructing various sized defects on all parts of the body. We agree with other authors in literature that Rhomboid and local flap should be considered as the first line of reconstructive strategy for various sized defects and body locations for best patient satisfaction, reconstructive, cosmetic outcomes and minimal complications [3].
Conclusion
We believe that with proper patient selection, rhomboid flaps should be considered a first-line option for reconstruction of almost any defect caused by any etiology. In summary, the technical ease, aesthetic outcome, continuity of function, short operation time, matching skin texture and color, safety, early functionality, and fewer out-patient clinic visits are some of the reasons to justify extensive application of rhomboid flaps.
References
- Aydin OE, Tan O, Algan S, Kuduban SD, Cinal H, et al. (2011) Versatile use of rhomboid flaps for closure of skin defects. Eurasian J Med 43(1): 1-8.
- Gibson T (1964) Modern Trends in Plastic Surgery. Butterworths, London, United Kingdom.
- Chasmar LR (2007) The versatile rhomboid (Limberg) flap. Can J Plast Surg 15(2): 67-71.
- Tamborini F, Cherubino M, Scamoni S, Frigo C, Valdatta L (2012) A Modified Rhomboid Flap: The Diamond Flap. Dermatol Surg 38: 1851-1855.
- Sommerlad BC, Creasey JM (1978) The stretched scar: A clinical and histological study. British Journal of Plastic Surgery 31: 34-45.
- Dufourmentel C (1964) An L-shaped flap for lozenge shaped defects: Principle - technique – applications. Transact Third Int Congr Plast Surg 772-773.
- Quaba AA, Sommerlad BC (1987) A square peg into a round hole: a modified rhomboid flap and its clinical application. British Journal of Plastic Surgery 40: 163-170.
- Kister M, Borowska K, Gontarz M (2017) Modern approach to facial skin defects reconstruction. Our Dermatol Online 8(4): 477-482.
- Turan T, Kuran I, Ozcan H (1999) Geometric limit of multiple local Limberg flaps: A flap design. Plast Reconstr Surg Glob Open 104(6): 1675-1678.
- Rohrer TE, Bhatia A (2005) Transposition flaps in cutaneous surgery. Dermatol Surg 31(8): 1014-1023.
- Ng SG, Inkster CF, Leatherbarrow B (2001) The rhomboid flap in medial canthal reconstruction. Br J Ophthalmol 85: 556-559.
- Mathew J, Varghese S, Jagadeesh S (2007) The Limberg flap for cutaneous defects- a two-year experience. Indian J Surg 29: 184-186.
- Pirozzi N, Pettorini L, Scrivano J (2013) Limberg Skin Flap for Treatment of Necrosis and Bleeding at Haemodialysis Arteriovenous Angioaccess Puncture Sites. Eur J Endovasc Surg 46(3): 383-387.
- Becker FF (1979) Rhomboid Flap in Facial Reconstruction. Arch Otolaryngol 105: 569-573.
- Alvarez GS, Laitano FF, Siqueira EJ, Oliveira MP, Martins PDE (2012) Use of the rhomboid flap for the repair of cutaneous defects. Rev Bras Cir Plást 27(1): 102-107.
- Li Z, Jiang Y, Zhang JY (2017) Modified O-T advancement flap for reconstruction of skin defects. Int J Clin Exp Pathol 10(9): 9158-9163.
- Khan AAG, Shah KM (2012) Versatility of Limberg flap in head and neck. International Journal of Case reports and Images 3(6): 13-18.
- Corredor Osorio R (2017) Rhomboid flap: An option to medial canthal reconstruction Our Dermatol Online 8(3): 329-332.
- Shah A, Zoumalan R, Constantinides M (2008) Aesthetic Repair od Small to Medium-sized Nasal defect. Facial Plast Surg 24: 1.
- Townsend J (1993) A template for the planning of rhombic skin flaps. Plastic and Reconstructive Surgery 92(5): 968-971.
- Ng SGJ, Inkster CF, Leatherbarrow B (2001) The rhomboid flap in medial canthal reconstruction. Br J Ophthalmol 85: 556-559.
- Di Santis EP, Elias BL, Andraus EM (2015) Rhomboid Flap: An Option to Many Anatomical Regions. Journal of Advanced Plastic Surgery Research 1: 14-18.
- Review of Rhomboid Flaps and Their Modern Modifications (2016) Grammenos, Rivas, Thomas, Thomas.
- Shah AR, Zoumalan R, Constantinides MS (2008) Aesthetic repair of small to medium-sized nasal defects. Facial Plast Surg 24(1): 105-119.
- Kim DY, Choi JH, Moon SH (2017) Feasibility and aesthetic results of small bilateral V-Y advancement flaps in the extremities and back. Arch Aesthetic Plast Surg 23(3): 127-134.
- Brown MD (1999) Skin surgery: a practical guide. Arch Dermatol 135(5).
- Tilleman TR, Neumann MH, Smeets NW (2006) Waste of skin in elliptical excision biopsy of non-melanomatous skin cancer. Scand J Plast Reconstr Surg Hand Surg 40: 352-356.
- Tissiani LAL, Alonso N, Carneiro MH (2011) Versatility of the bilobed flap. Rev Bras Cir Plast 26(3): 411-417.
- Pepper JP, Baker SR (2013) Local Flaps: Cheek and Lip Reconstruction. JAMA Facial Plastic Surgery 15: 374-382.
- Ooshima M, Kochi M, Marioka D (2018) Bipedicled Mini V-Y Advancement Flap for Skin Defect of the Face. Modern Plastic Surgery 8: 15-20.
- Defektlerinin C, Rhomboid O, Cok F (2011) Versatile use of rhomboid flaps for closure of skin defects. Eurasian J Med 43: 1-8.
- Dass T, Zaz M, Rather A (2012) Elliptical Excision with Midline Primary Closure versus Rhomboid Excision with Limberg Flap Reconstruction in Sacrococcygeal Pilonidal Disease: A prospective, Randomized Study. Indian J Surg 74: 4.
- Muzi MG, Milito G, Cadeddu F (2010) Randominzed comparison of Limberg flap versus modified primary closure for the treatment of pilonidal disease. Am J Surg 200(1): 9-14.
- Tavassoli A, Noorshafiee R (2011) Comparison of excision with primary repair versus Limberg flap. Int J Surg 9(4): 343-346.
- Cho YK, Ryu DW, Chung HY (2015) Surgical managemnt of scalp infantile hemangiomas. J Craniofac Surg 26: 1169-1172.
- Ring A, Kirchhoff P, Goertz O (2006) Reconstruction of soft-tissue defects at the foot and ankle after oncological resection. Front Surg 3: 15.
- Borges AF (1981) The rhombic flap. Plast Reconstr Surg 67(4): 458-466.
- Okus A, Sevinc B, Karahan O (2012) Comparison of Limberg flap and tension-free primary closure during pilonidal sinus surgery. World J Surg 36: 431-435.
- Horwood J, Hanratty D, Chandran P (2012) Primary closure or rhomboid excision and Limberg flap for the management of primary sacrococcygeal pilonidal disease? A meta-analysis of randomized controlled trials. Colorectal Dis 14(2): 143-151.
- Tekin A (2005) A simple modification with Limberg flap for chronic pilonidal disease. J Surg Tech Case Rep 138: 951-953.
- Aital SK, Rajan CS, Reddy N (2003) Limberg flap for sacrococcygeal pilonidal sinus a safe and sound procedure. Indian J Plast Surg 75(4): 298-301.
- Penington AJ, Mallucci P (1999) Closure of elective skin defects in the leg with a fasciocutaneous V-Y island flap. British Journal of Plastic Surgery 52: 458-446.
- Rao Jk, Shende KS (2016) Overview of Local Flaps of the Face for Reconstruction of Cutaneous Malignancies: Single Institutional Experience of Seventy Cases. Journal of Cutaneous and Aesthetic Surgery (4): 220-225.
- Divya GK, Shilpa K, Sarvajnamurthy S (2016) Outcome of flap surgeries in dermatosurgical unit at a tertiary care center in india with a review of literature. J Cutan Aesthet Surg 9: 226-231.
- Lister GD, Gibson T (1972) Closure of rhomboid skin defects: the flap of Limberg and Dufourmentel. Br J Plast Surg 25: 300-314.
- Badshah I, Shaully O, Lui CG (2019) Nonmelanoma Facial Skin Cancer: A Review of Diagnostic Strategies, Surgical Treatment, and Reconstructive Techniques. Clin Med Insights: Ear, Nose and Throat 219: 12.
- Lee KS, Kim JO, Kim NG (2017) A comparison of the local flap and skin graft by location of Face in Reconstruction after resection of facial skin cancer. Arch Craniofac Surg 18(4): 255-260.






























