Recurrent Bilateral Breast Abscess in Immunocompetent Women: A Case Report and Literature Review
Hiyam AL Haddad1*, Hend AL Shamsi2 and Najla AL Askar2
1Department of surgery, King Fahad Hospital of the University, Saudi Arabia
2lmam Abdulrahman Bin Faisal University, Saudi Arabia
Submission: February 15, 2018; Published: March 26, 2018
*Corresponding author: Hiyam Al Haddad, Consultant Breast surgeon, Department of surgery, King Fahd hospital of the University, Saudi Arabia, Email: dr_hiyam@yahoo.com
How to cite this article: Hiyam A H, Hend A S, Najla A A. Recurrent Bilateral Breast Abscess in Immunocompetent Women: A Case Report and Literature Review. Open Access J Surg. 2018; 8(4): 555745. DOI: 10.19080/OAJS.2018.08.555745.
Introduction
Breast abscess is a localized pocket of infection containing pus tissue; that commonly affects women of reproductive years with age ranging from 18-50 years. It is divided into a lactation and non-lactation infection. It can affect overlying skin as a primary event or secondary to a lesion such as sebaceous cyst [1]. Breast abscesses are typically caused by bacteria, most commonly Staphylococcus aureus. Other causes include mycobacterial and fungal infections [2]. There have been few reports of different infections caused by Salmonella spp. in recent years and a single case of bilateral breast abscess caused by E. coli and few by Proteus mirabilis, to our knowledge, there were no cases reported with recurrent breast abscesses caused by Kocuria kristinae. We present an unusual case of recurrent bilateral breast abscess caused by multiple organisms in an immunocompetent non-lactating patient.
Case Report
A 41-year-old Non Diabetic Saudi single female presented through the emergency department October 2015 complaining of progressive breast pain for 15 days' duration and a lump in the left breast. The patient denied history of fever, nipple or skin changes. On physical examination, she was cachectic and had left breast erythema, and tender mass. Admitted under the impression of mastitis with abscess. Further history taking was insignificant (negative history of fever, night sweats, smoking, alcohol or illicit drug use, trauma, nipple piercing, insect bite, nor swimming in public pools), apart from repeated visit to GIT clinic for weight loss and anorexia. She also denied history of ever being sexually active. In her family history, her aunt suffered from breast cancer. Laboratory investigations revealed elevated white blood cells (lymphocytes), total bilirubin, & ESR. She was managed with IV antibiotic & incision drainage done. The culture isolated Pseudomonas aeruginosa (Table 1).

She noted flu like symptoms prior to each attack. She noticed that her attacks were mostly when her weight decreases since she's underweight with history of weight loss and decreased appetite over the last few years. Her height is 156.5cm and her weight varies between 37-47kg making her average BMI= 17 which is considered underweight (She currently weighs 38kg). She was investigated thoroughly for the decrease in appetite and weight loss and nothing found except positive H Pylori stool antigen each time. Hepatitis profile, HIV test, and TB tests were negative as well as cancer screening. IgG, IgM, IgE, are normal level. Anti endomysial antibodies and Antigliadin antibodies are negative. Breast biopsy was negative for cancer or chronic inflammatory condition.
Discussion
The main concern of most of the women presenting with breast symptoms, including lumps, is likelihood of cancer, however, most breast masses are benign including fibrodenomas, fibrocystic condition, intraductal papilloma and breast abscesses [1]. WHO report on mastitis in 2000 clearly indicates that mastitis and abscesses are more common in lactating versus non-lactating women and NHS choices website article on breast abscesses, stated that "Breast abscesses are very uncommon in women who are not producing milk." Non-lactational breast abscesses can be divided into two broad groups, Peripheral and Areolar.
Breast abscess in non-lactating women had limited data in the literature [4]. the most significant risk factor for non- lactating breast abscess is diabetes mellitus (DM), smoking and immune suppression which was not identified as a risk factors in our case. Granulomatous mastitis another underlying diagnosis with high recurrence rate. Most common microorganism isolated from breast abscess is Staph [21-23]. Aureus other rare bacteria species can be found in immunocompromised patent. In our case, the identifiable organisms were Salmonella sp., Pseudomonas arignosa, E. coli, Proteus mirabilis, Klebsiella pneumoniae, Citrobacter species and Kocuria kristinae in different occasions.
Salmonella typhi bacteremia is occasionally associated with extra intestinal disease. It is capable of forming abscesses in various organs such as liver, subcutaneous tissue, muscles and skin. The pathogenesis of abscess formation is not well established [24]. The possible causes may be infective bile from carriers, hematogenous spread from distant site, and lym-phatic spread from gastrointestinal tract. Bilateral breast ab-scesses due to Salmonella typhi are a rare presentation. However, the present case was not associated with a detectable bacteremia in the past [3]. It is well known that the most common cause of community-acquired urinary tract infection is E. coli.
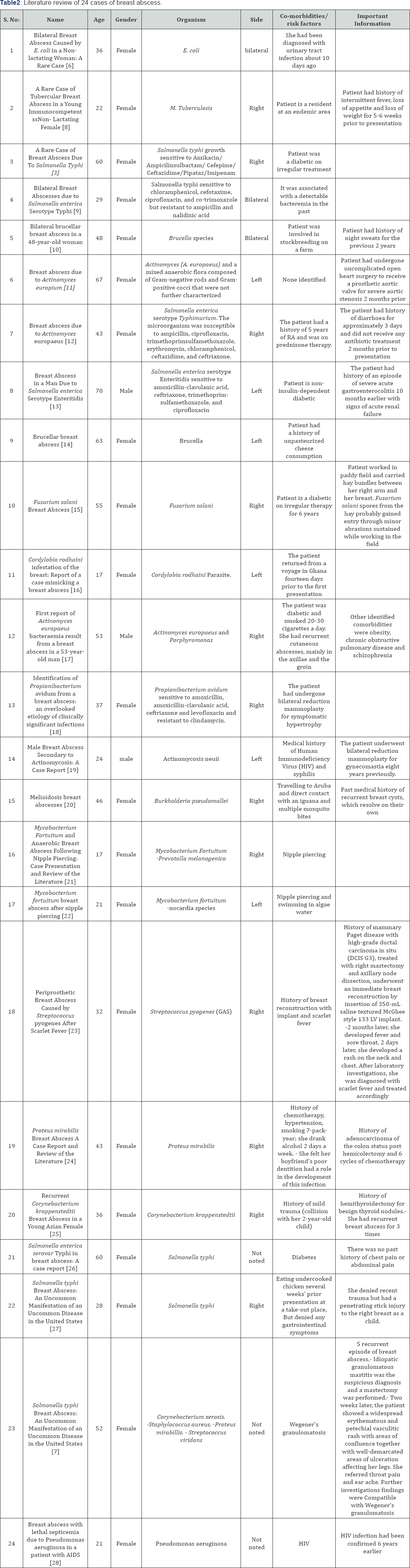
However, it is a rare occurrence of a breast abscess caused by E. coli. Proteus mirabilis is most often associated with infections of the genitourinary tract. Breast abscess formation with Proteus mirabilis is uncommon. This infection is more common in diabetic patients who also have an increased risk of abscess recurrence [9]. The treatment of breast abscess during the non- lactating period is controversial in the literature, especially regarding such rare infections. For an early abscess presenting as an indurate mass, a course of antibiotics may suffice. For a mature abscess (e.g., fluctuant mass), surgical intervention along with antibiotics is indicated. The following table summarizes literature review of 24 cases of breast abscess of Non Staph [25]. Aureus rare microorganisms in Non lactating woman, however, almost all of them have identifiable risk factors which lack in our case (Table 2).
Conclusion
Any case of a recurrent breast abscess in a non-lactating female must be heavily evaluated, in terms of clinical, laboratory and imaging assessment for any possible under lying risk factors can be identified. Keeping in mind the absence of such risk factors does not rule out rare or recurrent breast infections as it is the case in our patient whom after thorough investigation we could not find any identifiable risk factor.
The combination of medical and surgical management helps in such a case when supported by a microbiological culture and sensitivity report.
References
- Dixon JM (1994) ABC of breast diseases. Breast infection BMJ 309 (6959): 946-949.
- Nancy F, Crum Cianflone, Fadi A, Haddad, George Sakoulas (2013) A Breast Abscess, an Unusual Manifestation of Coccidioidomycosis? Infect Dis Clin Pract 21(4): 263-264.
- Murugesan N, Alagar Samy R, Viswanathan MS, Anbazhagan A (2016) A rare case of breast abscess due to salmonella typhi. Int J Cur Res Rev 8(5): 10-12.
- Rizzo M, Gabram S, Staley C, Peng L, Frisch A, et al. (2010) Management of breast abscesses in nonlactating women. Am Surg 76(3): 292-295.
- Şimjek, G, GündeŞ E, Tekin Ş, Tavli Ş (2014) Bilateral Breast Abscess Caused by E. coli in a Non-lactating Woman: A Rare Case. J Breast Health 10(3): 174-176.
- Malhotra S, Sharma S, Bhatia NJK, Sharma S, Hans C (2015) A Rare Case of Tubercular Breast Abscess in a Young Immunocompetent Non-Lactating Female. Clin Microbiol 4: 190.
- Singh G, Dasgupta M, Gautam V, Behera A, Ray P (2011) Bilateral breast abscesses due to Salmonella enterica serotype typhi. J Global Infect Dis 3(4): 402-404.
- Ibis C, Albayrak D, Yagci M (2009) Bilateral brucellar breast abscess in a 48-year-old woman. Annals of Saudi Medicine, 29(2): 158.
- Silva WA, Pinheiro AM, Jahns B, Bo'gli-Stuber K, Droz S, et al. (2011) Breast abscess due to Actinomyces europaeus. Infection 39(3): 255258.
- Irmak Baran, Neriman Aksu, Altan Aksoy (2016) Breast abscess due to Salmonella typhimurium in a patient with rheumatoid arthritis: a case report. BMC Infect Dis 16: 348.
- Brnčić N, Gorup L, Strcic M, Abram M, Mustac E (2011) Breast Abscess in a Man Due to Salmonella enterica Serotype Enteritidis. J Clin Microbiol 50(1): 192-193.
- Erdem G, Karakas H, Yetkin F, Alkan A, Firat A, et al. (2006) Brucellar breast abscess. Breast 15(4): 554-557.
- Anandi V, Vishwanathan P, Sasikala S, Rangarajan M, Subramaniyan C, et al. (2005) Fusarium solani breast abscess. Indian J Med Microbiol 23(3): 198.
- Grassi V, Butterworth JW, Latiffi L (2016) Cordylobia rodhaini infestation of the breast: Report of a case mimicking a breast abscess. International Journal of Surgery Case Reports 27: 122-124.
- Nielsen H (2015) First report ofActinomyces europaeus bacteraemia result from a breast abscess in a 53-year-old man. New Microbes New Infect 7: 21-22.
- Kritikos A, Pagin M, Borens O, Voide C, Orasch C (2015) Identification of Propionibacterium avidum from a breast abscess: an overlooked etiology of clinically significant infections. New Microbes New Infect 4: 9-10.
- Mahendiran SA, Leibman AJ, Kommehl AS (2016) Male Breast Abscess Secondary to Actinomycosis: A Case Report. J Clin Diagn Res 10(4): TD05-TDO7.
- Mickail N, Klein NC, Cunha BA, Schoch PA (2012) Melioidosis breast abscesses. Journal of Infection 64(4): 434-435.
- Bengualid V, Singh V, Singh H, Berger J (2008) Mycobacterium fortuitum and Anaerobic Breast Abscess Following Nipple Piercing: Case Presentation and Review of the Literature. Journal of Adolescent Health 42(5): 530-532.
- Abbass K, Adnan MK, Markert RJ, Emig M, Khan NA (2014) Mycobacterium fortuitum breast abscess after nipple piercing. Can Fam Physician 60(1): 51-52.
- Persichetti P, Langella M, Marangi GF, Vulcano E, Gherardi G, et al. (2008) Periprosthetic Breast Abscess Caused by Streptococcus pyogenes After Scarlet Fever. Ann Plast Surg 60(1): 21-23.
- Labalo S, Saravolatz LD (2015) Proteus mirabilis Breast Abscess. Infectious Diseases in Clinical Practice 23(3): 126-127.
- Goh Z, Tan AL, Madhukhumar P, Yong WS (2015) Recurrent Coryne bacterium kroppenstedtii Breast Abscess in a Young Asian Female. The Breast Journal 21(4): 431-432.
- Kumar ES, Selvam RE, Ramesh SS (2012) Salmonella enterica serovar Typhi in breast abscess: A case report. Indian J Pathol Microbiol 55(4): 608-609.
- Vikram Vattipally V, Thatigotla B, Nagpal K, Saraiya R, Henry M, et al. (2011) Salmonella typhi Breast Abscess: An Uncommon Manifestation of an Uncommon Disease in the United States. Am Surg 77: E133-135.
- Comas AG, Diana CA, Crespo CC, Cebollada MM, Linan MA, et al. (2010) Wegener's granulomatosis presented as recurrent breast abscess. The Breast Journal 16(1): 82-84.
- Rizzo M, Peng L, Frisch A, Jurado M, Umpierrez G (2009) Breast abscesses in nonlactating women with diabetes: clinical features and outcome. Am J Med Sci 338(2): 123-126.
- Roca B, Vilar C, Perez EV, Saez Royuela A, Simon E (1996) Breast abscess with lethal septicemia due to Pseudomonas aeruginosa in a patient with AIDS. Presse Med 25(17): 803-804.






























