Laparoscopic Versus Open Colectomies: Enhanced Surgical Skills And Rigorous Patient Selection May Improve Operative Times Without Compromising Outcomes
Konstantinos Stergios*1,2, Vasilios Pergialiotis2, Maximos Frountzas2, Prateek Nalwaya3, Konstantinos Kontzoglou2 and Shrabani Das Mohapatra3
1Watford General, west Hertfordshire Hospitals NHS Trust, UK
2National and Kapodistrian University of Athens, Greece
3Watford General, west Hertfordshire Hospitals NHS Trust, UK
Submission: May 01, 2017; Published: May 15, 2017
*Corresponding author: Konstantinos Stergios, Watford General, west Hertfordshire Hospitals NHS Trust, UK WD18 0GL, UK, National and Kapodistrian University of Athens, Greece, Tel: 0044(0)7599756871; Email: kostegios@gmail.com
How to cite this article: Konstantinos S, Vasilios P, Maximos F, Prateek N, Konstantinos K, et al.Laparoscopic Versus Open Colectomies: Enhanced Surgical Skills And Rigorous Patient Selection May Improve Operative Times Without Compromising Outcomes. Open Access J Surg. 2017; 4(3): 555636. DOI: 10.19080/OAJS.2017.04.555636
Abstract
Aim: The aim of our study was to compare the demographic characteristics, the intra- and postoperative outcomes of patients undergoing laparoscopic and open colorectal resections with or without stoma and with or without anastomosis.
Method: Our study includes 133 patients, who underwent laparoscopic and open colorectal resections for colonic and rectal disease.
Results: There was a statistically significant decrease of the operative duration time for the laparoscopic group [(182 min (103-341 min)] compared to the laparotomy group [(242 min (71-584 min)] (p=.006). The other parameters, such us age, BMI, blood loss, transfusion, leak, reoperation, 60-day mortality, wound infection, wound dehiscence, atelectasis, sepsis, ileus, UTI, first flatus and length of stay presented no difference.
Conclusion: The experience accumulated by the Colorectal surgeons and the careful selection of the patients seem to improve the operative duration and thus they provide both the surgeon and the patient with all the advantages of a short operation. On the other hand, the two techniques have no differences and the choice is made each time by the surgeon according to the indications and the patient status.
Keywords: Colorectal; Resection; Laparoscopic; Complications
Introduction
Colorectal cancer is the third most common cancer affecting both men and women, following breast, lung and prostate in the United States. The estimate number of colorectal cancer cases in the United States for 2017 is 95,520 new cases of colon cancer and 39,910 new cases of rectal cancer. The overall lifetime risk of developing colorectal cancer is about 1 in 21 (4.7%) for men and 1 in 23 (4.4%) for women [1]. In the US the overall Colorectal Cancer incidence in individuals over 50 years declined from 2009 to 2013. However, the incidence of rectal cancer in those ages 50 to 64 years was stable. On the other hand, the incidence of distal colonic and rectal cancer increases among adults of less than 50 years of age, by 22%. Colorectal cancer mortality rates also decrease by 34% for individuals above 50, but increase by 13% for those less than 50 years of age. In the United Kingdom, more than 40.000 new cases and more than 15.000 deaths on 2014, have been reported [2].
The treatment of choice by the means of cure, for the colorectal cancer is surgical resection of the affected segment, together with the relevant mesocolon/mesorectum, the supplying vascular pedicle and the included lymph nodes, laparoscopic or open [3]. Non-cancerous diseases are also treated surgically in some stage, like the diverticular disease and the Inflammatory Bowel Diseases [4]. While extensive and thorough studies are confirming the value of the laparoscopic operations for the colorectal cancer, the data about the resections of inflammatory masses are controversial [5-11].
Since its adoption the laparoscopic approach has gained enormous acceptance, mainly because of the equivalent surgical outcomes and the improved post-operative outcomes in terms of recovery and cosmesis. Costs and operative times, while higher in the past, are also improving, and especially the operative length is now similar to the open resections, fact which reflects the surgeon’s expertise and the strict selection of patients undergoing laparoscopy [12].
Materials and Methods
We retrospectively searched all patients that where operated in the Colorectal Department of The Princess Alexandra Hospital during 2013 and who underwent colorectal resections, for cancer and/or inflammatory diseases. All the operations were performed by expert Colorectal Surgeons were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments. Patients with synchronous malignant lesions were excluded from the present study as well as patients >90 years of age, patients with severe disability NYHA (New York Heart Association) status C and D (moderate and severe heart disease).
Statistical Analysis
Continuous variables are presented with median (range). The normality of the distributions was assessed with Kolmogorov-Smirnov’s test and graphical methods. Quantitative variables are presented with absolute and relative frequencies. Student’s t-test or nonparametric Mann-Whitney test were used to compare means between groups. For the comparisons of proportions chi-square and Fisher’s exact tests were used. All reported p values are two-tailed. Statistical significance was set at p<.05. All analyses were conducted using the SPSS statistical software (SPSS Inc. Released 2009. PASW Statistics for Windows, Version 18.0. Chicago: SPSS Inc.).
Results
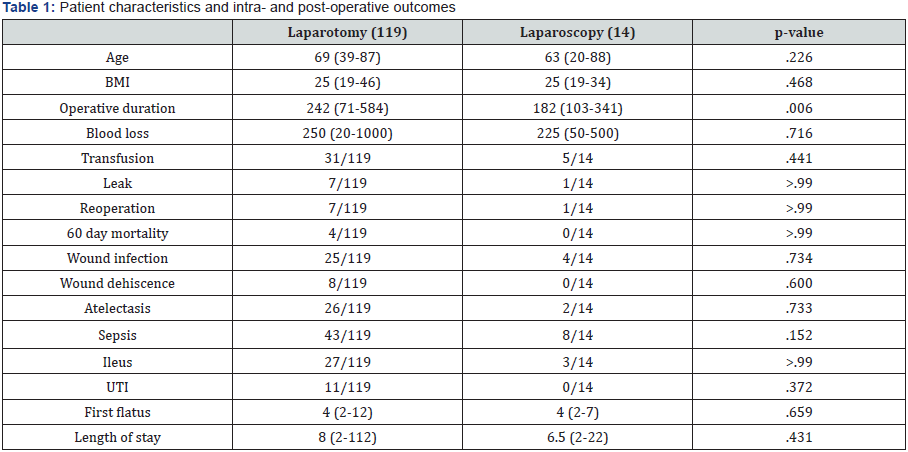
One hundred and thirty three patients who underwent laparoscopic and open colorectal resections for colonic and rectal disease where included. Most of the patients of the open group, were affected by advanced stage colorectal cancer, diverticular mass and complex Crohn disease. We evaluated 15 parameters and found them comparable. The patient`s age as well as BMI did not differ among the two groups. We did not observe significant differences in terms of intra- and postoperative complications. Interestingly, however, the intraoperative duration of laparoscopic operations was significantly decreased (p=.006) (Table 1). There was a statistically significant decrease of the operative duration time for the laparoscopic group [(182 min (103-341 min)] compared to the laparotomy group [(242 min (71-584 min)] (p=.006).
The other parameters, such us age, BMI, blood loss, transfusion, leak, reoperation, 60-day mortality, wound infection, wound dehiscence, atelectasis, sepsis, ileus, UTI, first flatus and length of stay presented no difference. The laparotomy group included patients with inflammatory masses and advanced stage of colorectal cancer, who were predicted to present more difficult dissection as a result of the inflammation and the locoregional spread of the primary tumor. While the advantages of the laparoscopy were confirmed, the operative length was shorter in confront to its size in the past. This decrease simultaneously revealed a significantly longer operative time for the laparotomies, fact which reflects both the improved surgical skills of the dedicated surgeons and the careful selection of patients undergoing some kind of colectomy.
Discussion
Colorectal Cancer is a common disease as per incidence and mortality and surgery is the curative method of choice, when possible. Both laparoscopic and open resections are equally safe and effective, but laparoscopic resections cost more and last longer [12-14]. The increasing experience of the Colorectal Surgeons, regarding their technical abilities and the selection of patients can minimize the operative time [4,15]. In our study all the resections were performed by expert Colorectal Surgeons and the open approach was reserved for diverticular masses, expected to be difficult because of the inflammatory sequels, as well as complex cases of Crohn disease, and advanced stages of colorectal cancer.
Many studies have been performed and published the last few years, emphasizing on the superiority of the laparoscopic surgery compared with the open surgery, with significant advantages of reduced blood loss, earlier recovery of intestinal motility, lower overall morbidity, and shorter duration of hospital stay [16,17]. These results have led to a general consensus on laparoscopic surgery as an equivalent alternative to open surgery for colorectal cancer and colonic pathologies of different nature [18,19]. The shorter hospital stay may also decrease the cost of the laparoscopic surgery for colorectal cancer, even if this is yet to be clearly defined, mainly due to the increasing cost over time, which in turn makes highly challenging the comparisons between studies conducted within a time frame of more than 10 years [20,21]. Drawbacks for a long time have been considered the higher costs and the longer operative time. However, despite the theoretical advantages of laparoscopic surgery, and the fact that today is considered, where there are available infrastructures and surgical expertise the standard treatment for colorectal cancer patients, the same concept does not apply in advanced staged cancer and inflammatory diseases, mainly due to technical limitations or the characteristics of the patients that may affect short and long term outcomes [22,23].
In our study we aimed to show that the duration of the operation can be importantly reduced, which reflects the overall improvement of surgical skills, but also that other factors, such as patient`s characteristics and nature of the underlying pathology maybe the cause of the longer operative time. This in our study is shown by the longer operative time of the laparotomies and their application in different diseases rather the colorectal cancer, at a favorable stage.
Nowadays, numerous studies conclude that the laparoscopic operations, performed for the same type of pathology last longer. Specifically there are studies evaluating operative time and outcome for the same stage of cancer and the specific segment of colon [24]. In particular the tumors of the transverse colon have been thoroughly studied, as representing a more challenging site with complex decision making management [25]. A certain number of studies also addressed the effectiveness of the application of the laparoscopic approach to diverticular disease and inflammatory bowel diseases compare to open, concluding that the laparoscopy takes longer [26]. However, there is a general acceptance of the fact that the laparoscopic operations are now lasting about half the time from the past and different studies confirm that [27]. This decrease of operating times has been attributed to the improved surgical skills and experience. In fact there are now studies showing a similar and even decreased operative time for the laparoscopic group for cancer or non-complex IBDs [28]. The operative time for a laparoscopic colorectal resections decreases with the increase of the operative skills of the surgeons and following careful selection of patients, excluding those who are predicted to undergo a difficult operation, based on patient`s characteristics and nature of disease can play a significant role in the best implementation of the laparoscopy in the surgical practice.
Conclusion
Colorectal Cancer is a common disease as per incidence and mortality. Surgery is the curative method of choice. Both laparoscopic and open resections are equally safe and effective, but laparoscopic resections cost more and last longer. The increasing experience of the Colorectal Surgeons, regarding their technical abilities and the selection of patients can minimize the operative time. In our study all the resections were performed by expert Colorectal Surgeons and the open approach was reserved for diverticular masses, expected to be difficult because of the inflammatory sequels, as well as complex cases of Crohn disease, and advanced stages of colorectal cancer [20]. More studies, including randomized control trials, are necessary for the laparoscopic approach to be proven faster in colorectal resections for cancer and inflammatory tumors.
References
- Rim SH, Seeff L, Ahmed F, King JB, Coughlin SS (2009) Colorectal cancer incidence in the United States, 1999-2004: an updated analysis of data from the National Program of Cancer Registries and the Surveillance, Epidemiology, and End Results Program. Cancer 115(9): 1967-1976.
- Siegel RL, Miller KD, Fedewa SA, Ahnen DJ, Meester RG, et al. (2007) Colorectal cancer statistics, 2017. CA: a cancer journal for clinicians.
- Fujii S, Tsukamoto M, Fukushima Y, Shimada R, Okamoto K, et al. (2007) Systematic review of laparoscopic vs open surgery for colorectal cancer in elderly patients. World journal of gastrointestinal oncology 8(7): 573-582.
- Di B, Li Y, Wei K, Xiao X, Shi J, et al. (2013) Laparoscopic versus open surgery for colon cancer: a meta-analysis of 5-year follow-up outcomes. Surgical oncology 22(3): e39-43.
- Bhakta A, Tafen M, Glotzer O, Canete J, Chismark AD, et al. (2016) Laparoscopic sigmoid colectomy for complicated diverticulitis is safe: review of 576 consecutive colectomies. Surgical endoscopy 30(4):1629-1634.
- Cirocchi R, Farinella E, Trastulli S, Sciannameo F, Audisio RA (2012) Elective sigmoid colectomy for diverticular disease. Laparoscopic vs open surgery: a systematic review. Colorectal dis 14(6): 671-683.
- de Campos-Lobato LF, Alves-Ferreira PC, Geisler DP, Kiran RP (2011) Benefits of laparoscopy: does the disease condition that indicated colectomy matter? The American surgeon 77(5): 527-533.
- Letarte F, Hallet J, Drolet S, Boulanger-Gobeil C, Bouchard A, et al. (2015) Laparoscopic versus open colonic resection for complicated diverticular disease in the emergency setting: a safe choice? A retrospective comparative cohort study. American journal of surgery 209(6): 992-998.
- Letarte F, Hallet J, Drolet S, Charles Gregoire R, et al. (2013) Laparoscopic emergency surgery for diverticular disease that failed medical treatment: a valuable option? Results of a retrospective comparative cohort study. Diseases of the colon and rectum 56(12): 1395-1402.
- Martel G, Bouchard A, Soto CM, Poulin EC, Mamazza J, et al. (2010) Laparoscopic colectomy for complex diverticular disease: a justifiable choice? Surgical endoscopy 24(9): 2273-2280.
- Umanskiy K, Malhotra G, Chase A, Rubin MA, Hurst RD, et al. (2010) Laparoscopic colectomy for Crohn’s colitis. A large prospective comparative study. Journal of gastrointestinal surgery 14(4): 658-663.
- Bayar R, Mzoughi Z, Djebbi A, Halek G, Khalfallah MT (2016) Laparoscopic colectomy versus colectomy performed via laparotomy in the treatment of non-metastatic colic adenocarcinomas. The Pan African medical journal 25: 165.
- Biondi A, Grosso G, Mistretta A, Marventano S, Toscano C, et al. (2013) Laparoscopic vs. open approach for colorectal cancer: evolution over time of minimal invasive surgery. BMC surgery 13 Suppl 2: S12.
- de’Angelis N, Alghamdi S, Renda A, Azoulay D, Brunetti F (2015) Initial experience of robotic versus laparoscopic colectomy for transverse colon cancer: a matched case-control study. World journal of surgical oncology 13: 295.
- Franklin BR, McNally MP (2017) Laparoscopy for Colon Cancer. Clinics in colon and rectal surgery 30(2): 99-103.
- Kannan U, Reddy VS, Mukerji AN, Parithivel VS, Shah AK, et al. (2015) Laparoscopic vs open partial colectomy in elderly patients: Insights from the American College of Surgeons - National Surgical Quality Improvement Program database. World journal of gastroenterology 21(45): 12843-12850.
- Kazama K, Aoyama T, Hayashi T, Yamada T, Numata M, et al. (2017) Evaluation of short-term outcomes of laparoscopic-assisted surgery for colorectal cancer in elderly patients aged over 75 years old: a multiinstitutional study (YSURG1401). BMC surgery 17(1): 29.
- Kim IY, Kim BR, Kim HS, Kim YW (2015) Differences in clinical features between laparoscopy and open resection for primary tumor in patients with stage IV colorectal cancer. OncoTargets and therapy 8: 3441-3448.
- Lee CZ, Kao LT, Lin HC, Wei PL (2015) Comparison of clinical outcome between laparoscopic and open right hemicolectomy: a nationwide study. World journal of surgical oncology 13: 250.
- Rinaldi L, Ouaissi M, Barabino G, Loundou A, Clavel L, et al. (2017) Laparoscopy could be the best approach to treat colorectal cancer in selected patients aged over 80 years: Outcomes from a multicenter study. Digestive and liver disease 49(1): 84-90.
- Yamaguchi S, Tashiro J, Araki R, Okuda J, Hanai T, et al. (2017) Laparoscopic versus open resection for transverse and descending colon cancer: Short-term and long-term outcomes of a multicenter retrospective study of 1830 patients. Asian J Endosc Surg
- Zeng WG, Liu MJ, Zhou ZX, Hou HR, Liang JW, et al. (2015) Outcome of Laparoscopic Versus Open Resection for Transverse Colon Cancer. Journal of gastrointestinal surgery 19(10): 1869-1874.
- Zimmermann M, Benecke C, Jung C, Hoffmann M, Nolde J, et al. (2016) Laparoscopic resection of right colon cancer-a matched pairs analysis. International journal of colorectal disease 31(7): 1291-1297.
- Lorenzon L, La Torre M, Ziparo V, Montebelli F, Mercantini P, et al. (2014) Evidence based medicine and surgical approaches for colon cancer: evidences, benefits and limitations of the laparoscopic vs open resection. World journal of gastroenterology 20(13): 3680-3692.
- Saiganesh H, Stein DE, Poggio JL (2015) Body mass index predicts operative time in elective colorectal procedures. The Journal of surgical research 197(1): 45-49.
- Schlussel AT, Lustik MB, Johnson EK, Maykel JA, Champagne BJ, et al. (2015) Do the advantages of a minimally invasive approach remain in complex colorectal procedures? A nationwide comparison. Diseases of the colon and rectum 58(4): 431-443.
- Zhao LY, Chi P, Ding WX, Huang SR, Zhang SF, et al. Laparoscopic vs open extended right hemicolectomy for colon cancer. World journal of gastroenterology 20(24): 7926-7932.
- Zheng Z, Jemal A, Lin CC, Hu CY, Chang GJ (2015) Comparative effectiveness of laparoscopy vs open colectomy among nonmetastatic colon cancer patients: an analysis using the National Cancer Data Base. Journal of the National Cancer Institute 107(3).






























