Intravascular Large B-Cell Lymphoma as Mono-Neuritis Multiplex
Renu Pokharna*, Souvik Sen and Candace Schaefer
Division of Neurology, Palmetto Health-University of South Carolina, USA
Submission: May 22, 2017; Published: July 6, 2017
*Corresponding author: Renu Pokharna, Division of Neurology, Palmetto Health-University of South Carolina, Columbia, SC, USA, Email: renu.pokharna@palmettohealth.org
How to cite this article: Renu P, Souvik S, Candace S. Intravascular Large B-Cell Lymphoma as Mono-Neuritis Multiplex. Open Access J Neurol Neurosurg. 2017; 4(4): 555644. DOI: 10.19080/OAJNN.2017.04.555644
Abstract
Intravascular Lymphoma (IVL) is an uncommon disease, which can rarely manifest as Mono Neuritis Multiplex (MNM) and must be considered in the differential diagnosis of Lymphoma. We report a case of a 75 year old female diagnosed with MNM who was shown to have IVL very late in her disease course by a nerve biopsy. We propose that IVL should be considered in the differential diagnosis of MNM. Awareness of the presentation of this chronic asymmetric progressive, disabling, and potentially fatal disease may be facilitated by early diagnosis and early treatment after the biopsy.
Keywords: Intravascular Lymphoma (IVL); Mono Neuritis Multiplex (MNM) or Multifocal Mono Neuropathy; Hemophagocytic Lymphohistiocytosis (HLH)
Introduction
Intravascular lymphoma (IVL) is a rare type of extra-nodal lymphoma with an aggressive clinical course characterized by proliferation of large lymphoma cells within the lumina of small vessels. Diagnosis of IVL is extremely difficult because of its varied clinical symptoms and the absence of lymphadenopathy, which requires histological confirmation. We report a case of a patient with Mono-Neuritis Multiplex (MNM) who admitted to our hospital in Oct 2016. MNM is a painful, asymmetrical, asynchronous sensory motor axonal peripheral neuropathy, which randomly damages many separate nerves bilaterally, distally, or proximally. MNM becomes more symmetrical rather than multifocal as the condition progresses. Damage is commonly caused by decreased blood flow, which causes lack of oxygen to the nerve. There is inflammation of blood vessels and epineurial artery vessel wall destruction and lumen occlusion. In her case, MNM was found to be secondary to IVL, which was diagnosed by a nerve biopsy. Early diagnosis and prompt treatment with rituximab-based chemotherapy could have produced a favorable response. It is proposed that tissue biopsy be done early, which may alter the course of events for patients.
Case Report
We report a 75 year old Caucasian female in excellent health who developed progressive weakness and numbness following blood transfusions for new-onset anemia one year ago. Patient was worked up for neuropathy, progressive functional decline, dizziness, fever, night sweats, gait instability, left foot drop, weakness in both hands, numbness/tingling in both hands and feet continuing up to her knee in the right leg, difficulty with ADLs, RLE shooting pain, decreased appetite, weight loss, rare dysphagia for solids, bladder and bowel incontinence. LP in May was unremarkable. EMG results were consistent with MNM, for which she received Prednisone for 4 weeks.
Patient had a past medical history of rheumatoid arthritis, psoriasis/rash, dyspnea, lymphedema in the right leg, cold intolerance, fatigue, weight loss, persistent headaches, tremor, decreased memory, dizziness, and abdominal discomfort. The patient's grand-daughter was diagnosed with Hodgkin lymphoma. Outside records showed anemia/iron deficiency (severe, requiring transfusions), mild leukocytosis, hyperferritinemia (786 -April 2016), hyperbilirubinemia, hyperlipidemia, elevated LDH, hypertriglyceridemia, and mild hypercalcemia. ANA positivity, negative panel, an ESR of 37, elevated serum of 281, &unremarkable SPEP were reported. Previous PET-CT was negative, brain MRI showed small infarct, & TTE showed non-specific changes. She had an abnormal chest CT with a left chest wall mass and breast nodule with no biopsy done. Electrodiagnostic evidence was suggestive of MNM, with spontaneous activity with polyphasia and a decreased recruitment pattern distally, which was asymmetrical. Proximal muscles were normal without any electrodiagnostic evidence of AIDP, CIDP, or polyradiculopathy.
The patient continued to decline and was referred for further care. Patient presented to the hospital with progressive weakness, sensory loss and failure to thrive. During physical exam the patient was found to have mild BLE edema, bilateral progressive motor and sensory symptoms and signs with both UMN and LMN features. Hemophagocytic Lymphohistiocytosis (HLH) was considered because of the patient's current rash, fever (101.6°F), altered mental status, monocytosis, hypertriglyceridemia, elevated LDH, hyperferritinemia and past history of rheumatoid arthritis. Post-transfusional CMV was considered, which can trigger secondary HLH, but tested negative. Pan-culture and LP were also negative. Labs after admission showed anemia of chronic disease/inflammation, iron deficiency, mild thrombocytopenia. Peripheral blood smear showed normocytic normochromic anemia, basophils, immature cells, slight monocytosis, no blastocyst or atypical lymphocytes. Labs also showed Ferritin of 1990ng/mL, Fe of 24 ug/dL, TIBC of 168ug/dL, ESR of 67mm/hr, albumin of 2g/dL, Pre-albumin of 7.7, Indirect bili of 0.8 mg/dL, Procalcitonin of 0.71ng/mL, LDH of 631 U/L, CRP of 66.2mg/L, TAG of 362mg/dL, dsDNA+ of 130IU/mL, antihistone+ of 187AU/mL. SPEP showed biclonal bands with a small-IgG peak of 0.5 and an IgM peak of 0.1, as well as a monoclonal band in the gamma region. Hepatitis panel, RPR, HIV, CMV IgM, glycoprotein antibodies, serum IgG, C3, C4, cyclic citrullinated peptide AB, Purkinje cell/neuronal nuclear IgG, MAG IgM Ab, Azo, HSV 1&2, Parvovirus, cyroglobulin, paraneoplastic panel (anti-ANNA, anti-PCCA), serum anti-CCP, anti-CV2/CRMP5, repeat ANA, C and P ANCA, ACE, CCP Ab, RF, anticardiolipin antibodies, Lupus-anticoagulant, autoimmune serology-scleroderma, DNA antibody, Smith antibodies, RNP antibody, centromere antibody, anti-Jo, anti-SSA/SSB, myeloperoxidase antibody, serine protease 3 were all within normal limit. Cervical, thoracic and lumbar spine MRI showed a T8 compression fracture. Chest, abdomen, and pelvis CT showed splenomegaly. Thyroid US showed multinodular goiter.
Biopsies
Bone marrow biopsy: Hypercellular (55%) with Trilinage maturation, hemophagocytosis, no dysmorphic features, plasmacytosis with lambda seen, no atypical lymphoid, no increase in blasts by flow. adequate iron. no ring sideroblasts. Although no definitive monoclonal plasma cell noted. the inverted K:L ratio with predominance of Lambda+ plasma cells by ISH is suggestive of possible low level involvement by a plasma cell neoplasm. Bi-clonal plasma cell populations with different light chains could prove difficult or impossible to identify with light chain ISH staining alone. Alternately, if the patient were to be diagnosed with a B-cell non-Hodgkin lymphoma, this could account for M-protein.
Skin biopsy report: Atypical B-cell lymphoid infiltrate and histiocytes showing increased phagocytosis was noted, as seen in figure 1. These cells tested to be CD20 positive. HLH can be seen with lymphoma, plasma cell neoplasm, or other malignancies. Malignancy, possibly lymphoma, was hypothesized, but no clearly pathologic lymphadenopathy noted. Mild splenomegaly was seen; however, this by itself would be unlikely to account for her symptoms. POEMS syndrome and Plasma cell dyscresias were also considered, but were unlikely because small monoclonal protein with 10 percent marrow plasmacytosis was seen. Mast cell activation syndrome was also considered, but there was no skin manifestation such as urticaria or recurrent allergies.
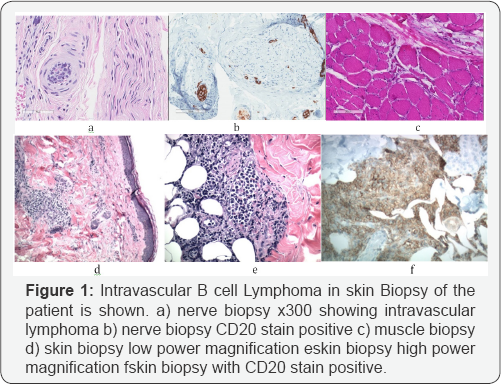
Right sural nerve biopsy: Intravascular non-germinal center type large B-cell lymphoma and severe anoxal loss with evidence of mild active degeneration was noted with CD20 positive stain.
Right gastrocnemius muscle biopsy: Intravascular large B-cell lymphoma was noted.
Final Diagnosis
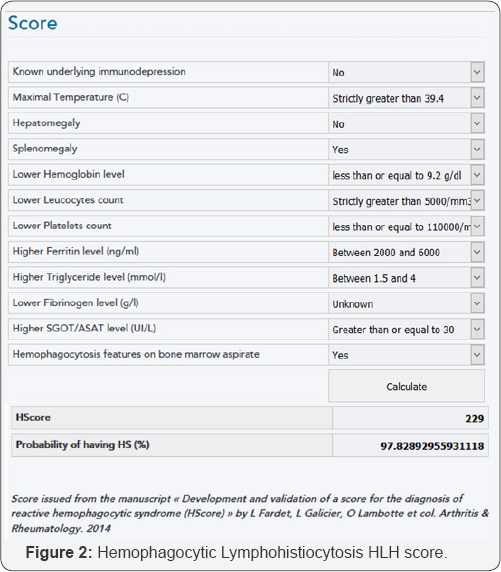
The final diagnosis was intravascular large B-cell lymphoma, presented as Mono-Neuritis Multiplex. Episodic fevers and worsening anemia are thought to be related to episodes of Hemophagocytic Lymphohistiocytosis (HLH) triggered by her underlying lymphoma. She met a sufficient number of diagnostic criteria outlined in the HLH-2004 Trial including Fever >101.3, Splenomegaly, Cytopenia (especially anemia and thrombocytopenia), Hemophagocytosis on bone marrow biopsy report, Ferritin > 500 (close to 3000), and hypertriglyceridemia. The patients HLH score, as seen in figure 2, was 97.83 percent. The positive ANA and dsDNA are most likely a paraneoplastic phenomenon and not an indicator of actual autoimmune disease. The patient succumbed to her illness before treatment could be initiated. Treatment should be targeted at the underlying lymphoma, but it poses significantly greater than average risk of treatment related complications and mortality.
Discussion
IVL is a rare large B cell Lymphoma, also known as intravascular lymphomatosis, angiotropic large cell lymphoma, and malignant angioendotheliomatosis, which rarely can also be T cell phenotype. IVL occurs in less than one per million people [1]. IVL affects capillaries and venules producing symptoms of the organ involved, without causing an extra vascular tumor, which used to be recognized at autopsy [2,3]. Lately with more frequent biopsies being done, IVL has been able to be diagnosed earlier, allowing for earlier treatment, which has the potential for a better prognosis after chemotherapy. There have even been rare cases of untreated long-term survivors.
Constitutional B symptoms include fever, night sweats, and weight loss [2]. The clinical presentation appears to differ by country of origin. In Western countries, patients commonly present with central nervous system symptoms, such as dementia, stroke, and peripheral neuropathy, which can rarely present as Mono-Neuritis Multiplex, as in our case [2]. IVL can also present with skin lesions and less commonly present with bone marrow, spleen and liver. In Asia, neurological symptoms and cutaneous lesions are less common while bone marrow, spleen and liver are more common [2].
IVL may present as secondary HLH, which is a hemophagocytic syndrome due to systemic macrophage activation, associated with constitutional symptoms and hemophagocytosis of erythrocytes, leukocytes, and platelets [4,5]. Eighty to 90 percent of patients with HLH have a rise in serum lactate dehydrogenase and beta 2-microglobulin, 65 percent are anemic and 43 percent have signs of inflammation with an elevated sed rate [2]. About 15 to 20 percent have abnormal liver, kidney, and thyroid functions and 14 percent have the presence of a serum monoclonal protein [2].
Treatment can include Anthracycline-based chemotherapy with either CHOEP (cyclophosphamide, Adriamycin, Oncovin, prednisone, etoposide) or MACOP-B (methotrexate, Adriamycin, cyclophosphamide, Oncovin, prednisone, Bleomycin) and followed by consolidation high-dose chemotherapy supported by autologous stem cell transplantation (ASCT) appeared to be the best mode of treatment [6,7]. Chemotherapy, surgery, radiation can be combined to improve survival.
Conclusion
In general, IVL is a rare and lethal disease that is difficult to diagnose and rarely presents as MNM. IVL should be included in the differential diagnosis of MNM in order to obtain an earlier diagnosis, which is dependent upon a tissue biopsy. This would allow for earlier treatment and a better prognosis for patients.
Acknowledgement
I am thankful to Dr. James Dollar and Dr. Harry Kellermire for providing pathological Slides. I also wish to thank Miles Reese, Medical Student with formatting of the script.
References
- Linnik Y, Rand J, Kaur P, Liu, X (2017) Intravascular large B cell lymphoma diagnosed in random duodenal biopsies. A case report and a literature review. Virchows Archiv: 1-3.
- Freedman A, Aster J, Böer-Auer A (2015) Intravascular large cell lymphoma. In Alan G Rosmarin (Ed.), UpToDate. Retrieved.
- Roux S, Grossin M, De Bandt M, Palazzo E, Vachon F, et al. (1995) Angiotropic large cell lymphoma with mononeuritis multiplex mimicking systemic vasculitis. J Neurol Neurosurg Psychiatry 58(3): 363-366.
- Janka G, Imashuku S, Elinder G, Schneider M, Henter JI (1998) Infection- and malignancy-associated hemophagocytic syndromes: secondary hemophagocytic lymphohistiocytosis. Hematology/oncology clinics of North America, 12(2): 435-444.
- Han AR, Lee HR, Park BB, Hwang IG, Park S, et al. (2007) Lymphoma- associated hemophagocytic syndrome: clinical features and treatment outcome. Annals of hematology 86(7): 493-498.
- Ponzoni M, Ferreri AJ, Campo E, Facchetti F, Mazzucchelli L, et al. (2007) Definition, diagnosis, and management of intravascular large B-cell lymphoma: proposals and perspectives from an international consensus meeting. J Clin Oncol 25(21): 3168-3173.
- Ferreri AJ, Campo E, Seymour JF, Willemze R, Ilariucci F, et al. (2004) Intravascular lymphoma: clinical presentation, natural history, management and prognostic factors in a series of 38 cases, with special emphasis on the 'cutaneous variant'1. Br J Haematol 127(2): 173-183.






























