Biological Regeneration of Tissues - Latest Therapeutic Approach Using Platelet Rich Plasma
Abha Singla and Monica Jain*
Department of Oncopathology, Delhi State Cancer Institute, India
Submission: February 25, 2017; Published: April 03, 2017
*Corresponding author: Dr. Monica Jain, Department of Oncopathology, Delhi State Cancer Institute, India, Email: drmonical23@gmail.com
How to cite this article: Abha S, Monica J. Biological Regeneration of Tissues - Latest Therapeutic Approach Using Platelet Rich Plasma. Blood Res Transfus J. 2017; 1(1) : 555553.
Abstract
Regeneration of cells and tissues is a new therapeutic approach for treatment of various diseases. Earlier, prolotherapy was practiced all over using hypertonic solutions, but later on Platelet Rich Plasma therapy was introduced to stimulate wound healing. Initially, large quantity of blood requirement and expensive equipment precluded its use, but PRP therapy was revolutionized in 1990, when small quantity of autologous patient's blood and portable machines extended its use from dental surgeries to orthopedics and cosmetics. Various methods of preparing HD-PRP are known. Then these platelet concentrates are activated and injected locally at the target site. These activated platelets release various growth factors and cytokines on degranulation, which act by chemo attraction and matrix deposition and accelerate wound healing. This mode of therapy is further advanced by injecting embryonic (prenatal stem cells and adult postnatal stem cells) along with PRP. Outcomes and evidence of its utility so far is encouraging and positive. However, more research needs to be done to refine these techniques and provide larger patient trial and long term benefits.
Keywords: Platelet rich plasma; High density platelet rich plasma; Prolotherapy
Abbreviations: EGF: Epidermal Growth Factor; IGF: Insulin Like Growth Factor; PDGF: Platelet Derived Growth Factor; PD-EGF: Platelet Derived Epidermal Growth Factor; PDAF: Platelet Derived Angiogenesis Factor; PF-4: Platelet Factor 4; TGF-β: Transforming Growth Factor; VEGF: Vascular Endothelial Growth Factor; ECGF: Endothelial Cell Growth Factor; FGF: Fibroblast Growth Factor; SDF-1α: Stromal Cell Derived Factor 1α
Introduction
Regenerative Medicine is a new therapeutic approach characterized by biological regeneration of the cells and tissues instead of their replacement. Platelet Rich Plasma (PRP) therapy, like prolotherapy is a method of injection designed to stimulate healing. "Prolotherapy, started in 1930, with injection of solutions which were primarily hypertonic dextrose or saline based, when Dr. Earl Gedney, an osteopathic surgeon, accidently injured his thumb and could repair it fully by injecting these irritating solutions [1]. Prolotherapy is practiced worldwide, and has been proved to be effective in treating many musculoskeletal conditions such as tendinopathies, back pain, tennis/golfers elbow, joint laxity and knee pain [2]. Platelet rich plasma is defined as "autologous blood with concentrations of platelets at least five times above baseline levels, (1000X109/L) and contains around seven growth factors" [3].
History of PRP Therapy and Prolotherapy
Use of PRP has been reported from 1970's but initially, large quantity of patient's blood (450ml), expensive large equipment, limited the use of this mode only in large scale surgeries. In 1990, the preparation of PRP revolutionized, making its use broad based, by using only 30-40ml of patient’s blood taken in a syringe and processed in small, portable and affordable machines [4]. The use of this PRP in clinical practice ranged from maxillofacial, dental, periodontal surgery to cosmetic surgery and skin grafting [5]. By year 2000, its use included orthopedics in healing of bone grafts and fractures, and with encouraging results, expanded its further use for connective tissue repair in sports medicine and chronic tendon problems in athletes in year 2006 [6]. Now-a-days, PRP is being used in treatment of more than 30 diseases including tissue engineering and research, cardio-vascular surgery, gastroenterology, urology, cosmetic and ophthalmology. PRP is considered in stem cell technology in recent years [7]. PRP is successfully added into the medium to culture several kinds of stem cells. It can be used as an alternative to fetal bovine serum for cultivating mesenchymal stem cells [8]. The latest developments in this field are use of HD-PRP in stem cell proliferation and transplantation, fetal type (embryonic) which are pluripotent cells and give rise to any type of cells and adult type which are multi-potent, partially differentiated but still can give rise to multiple lineages [9].
Preparation of PRP Therapy
Platelets are small, non nucleated bodies constituting 6% of whole blood which contain alpha granules and dense bodies. These alpha granules have several growth factors and cytokines that enhance proliferation, recruitment and differentiation of cells in tissue regeneration. Preparation of PRP is done in the department of transfusion medicine using standard preparation techniques from patient's own blood. 20-100ml of blood is drawn from the patient's vein with a syringe, transferred to an anti-coagulated test tube with citrate phosphate dextrose adenine (CPDA) in a ratio of 1:9 to the blood. Further, there are three techniques for preparation of PRP [4,10].
a. Gravitational platelet sequestration (GPS) technique.
b. Standard cell separators
c. Autologous selective filtration technology (plateletpheresis)
i. The GPS is a table top centrifuge system in which 60ml plastic centrifuge tube is used and 12 minute spin at 3200rpm is done. PRP volume of about 5ml can be collected.
ii. Standard cell separators operate on a full unit of blood using a continuous flow centrifuge bowl or a continuous flow disc separation technique involving hard (fast) spin and soft (slow) spin yielding two-four times of platelets. However, a discontinuous technique with a cell separator produces fivefold increase in platelet count in which one 10minute centrifugation at 2000rpm separates blood into three layers-RBCs, platelets and platelet poor plasma. Then RBC layer is drawn from the tube and the remainder is agitated for several seconds and undergo a second centrifugation again at 2000rpm for 10minutes. Now, it gets separated into two layers, upper supernatant which is platelet poor plasma constituting about three fourth of the sample and residual one fourth contains platelet concentrate which is around 5ml.
iii. Plateletpheresis follows the principle of single use disposable filter designed to concentrate platelets from whole blood without need of centrifugation producing platelet fraction enriched with platelets and growth factors [11].
Cell ratios in average circulating whole blood contain only 6% platelets, but in these high density PRP preparations, the concentration of platelets achieved is around 94%. If platelet count is around 1000X109/L, is considered ideal for therapeutic PRP [12].
Further processing of PRP to activate platelets
In a 10ml syringe, 10% calcium chloride is integrated with PRP in a ratio of 6:1 (6ml of PRP, 1ml of calcium chloride and 1ml of air), and air which acts as a mixing bubble. The syringe is pushed for 10 minutes to initiate clotting and this leads to platelet activation, resulting in release of growth factors from alpha granules [13]. 70% of stored growth factors are released within 10minutes of PRP activation and nearly 100% within one hour which continues for 8-10 days [7]. Another method of activation of PRP is by mixing PRP and calcium chloride solution in ratio of 10:1 using a dual syringe system. The PRP is drawn into a 10ml syringe and activating solution in 1ml syringe. Both the syringe plungers are connected to make a motion in concert with both the ports connected to a dual spray applicator tip which allows both the solutions to be mixed as they are given to the surgical bed. The benefit of this method is that since the alpha granules quickly release their contents on activation, there is no delay in delivery and hence no loss of secretary proteins [14].
Various therapeutic platelet products [15]
a. Platelet Rich Plasma-Platelet concentrates obtained after two centrifugations.
b. Platelet Gel- Platelets are exposed to agonist to induce activation with release of intrinsic substances that are applied to the target area to accelerate wound healing.
c. Platelet Leukocyte Gel- It has additional antimicrobial properties.
Mechanism of Action of PRP Therapy
The alpha bodies of platelets in PRP degranulate on activation and release cytokines, signal proteins and various growth factors which actually initiate and accelerate tissue regeneration by cellular chemo attraction and deposition of extracellular matrix (Table 1) [16].
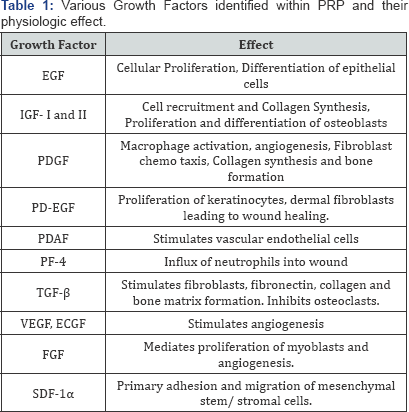
EGF: Epidermal Growth Factor; IGF: Insulin Like Growth Factor; PDGF: Platelet Derived Growth Factor; PD-EGF: Platelet Derived Epidermal Growth Factor; PDAF: Platelet Derived Angiogenesis Factor; PF-4: Platelet Factor 4; TGF-β: Transforming Growth Factor; VEGF: Vascular Endothelial Growth Factor; ECGF: Endothelial Cell Growth Factor; FGF: Fibroblast Growth Factor; SDF-1α: Stromal Cell Derived Factor 1α
Indications of PRP therapy
a. Musculo-skeletal diseases- Ligament sprains, tendonitis, intra-articular injuries, knee meniscus repair. PRP therapy is a new revolutionary treatment which relieves pain and denies or postpones surgery [15].
b. Cosmetic surgery- For esthetic purposes such as fine wrinkles, acne, scars, hair transplantation and change of colour. Local therapy of PRP is also effective tool for mucosal lesions caused by graft versus host disease (GVHD) involving dermis or oral mucosa [15].
c. Maxillofacial surgeries-PRP is considered standard treatment of bone defects, implants, reconstructions and augmentation [15].
d. Wound Healing-PRP is applied topically around injury. For chronic wounds, twice weekly, up to ten dressings and for injuries, maximum three injections within six months, at a gap of two to three weeks. Recovery occurs usually after second injection [13].
e. Ophthalmology-PRP has been used for dry eye, fast healing of corneal ulcers and ocular surgeries [17].
f. Others-In Cancer, Ischemic damage to nerves and various muscle atrophies and degenerations [15].
Since PRP is prepared from autologous blood, there are minimal risks for disease transmission, cancer or hypersensitivity reaction. There have been no reports of side effects of PRP injection [18].
Contraindications of PRP therapy
a. Absolute- Platelet dysfunction syndrome, severe thrombocytopenia, septicemia, local site infection, hemodynamic instability
b. Relative- Persistent NSAID intake within 2 days, local corticosteroid injection or systemic use of steroids, recent fever, Hb less than 10g/dl, platelet level less than 100X109/L [16].
Conclusion
PRP is a natural biological product which can be used as a drug in wound healing, as an adjuvant in stem cell transplantation and a differentiating factor and stimulator in stem cell culture. Prolotherapy is like planting seeds in a garden; while PRP therapy is planting seeds with fertilizers.
References
- Alderman D (2009) A history of the American College of Osteopathic Sclero therapeutic Pain Management, the oldest prolotherapy organization. Journal of Prolotherapy 1(4): 200-204.
- Rabago D, Best T, Beamsley M, Patterson J (2005) A systematic review of prolotherapy for chronic musculoskeletal pain. Clin J Sport Med 15(5): 376-380.
- Hall MP, Band PA, Meislin RJ, Jazrawi LM, Cardone DA (2009) Platelet- rich plasma: Current concepts and application in sports medicine. J Am Acad Orthop Surg 17(10): 602-608.
- Kevy S, Jacobson M (2004) Comparison of methods for point of care preparation of autologous platelet gel. Journal Extra-Corpor Technol 36(1): 28-35.
- Garg AK (2000) The use of platelet rich plasma to enhance the success of bone grafts around dental in plants. Dent Implantol Update 11(3): 17-21.
- Mishra A, Pavelko T (2006) Treatment of chronic elbow tendonosis with buffered platelet-rich plasma. Am J Sports Med 34(11): 17741778.
- Hara G, Basu T (2014) Platelet-rich Plasma in regenerative medicine. Biomedical Research and Therapy 1(1): 25-31.
- Pham PV, Vu NB, Pham VM, Truong NH, Pham TL, et al. (2014) Good manufacturing practice-compliant isolation and culture of human umbilical cord blood-derived mesenchymal stem cells. J Transl Med 12: 56.
- Pittenger M, Mackay A, Beck SC, Jaiswal RK, Douglas R, et al. (1999) Multi-lineage potential of adult human mesenchymal stem cells. Science 284(5411): 143-147.
- Dhurat R, Sukesh MS (2014) Principles and Methods of Preparation of Platelet-Rich Plasma: A Review and Author's Perspective. J Cutan Aesthet Surg 7(4):189-197.
- Saran RK (2003) Blood components preparation and uses. Transfusion Medicine Technical Manual (2nd edn), Ministry of Health & Family Welfare Govt of India, India, pp. 193-228.
- Marx RE, Kevy SV, Jacobson MS (2008) Platelet rich plasma (PRP): A primer. Pract Pain Manag 8(2): 46-47.
- Singh R, Rohilla RK, Dhayal RK, Sen R, Sehgal PK (2014) Role of local application of autologous platelet-rich plasma in the management of
- Man D, Plosker H, Winland-Brown JE (2001) The use of autologous platelet-rich plasma (platelet gel) and autologous platelet-poor plasma (fibrin glue) in cosmetic surgery. Plast Reconstr Surg 107(1): 229-237.
- Rozman P, Semeni D, Smrke DM (2011) The Role of platelet gel in Regenerative Medicine. Advances in Regenerative Medicine DOI: 10.5772/26130.
- Foster TE, Puskas BL, Mandelbaum BR, Gerhardt MB, Rodeo SA (2009) Platelet Rich Plasma (PRP) from basic sciences to clinical application. Am J Sports Med 37(11): 2259-2272.
- Freire V, Andollo N, Etxebarria J, Hernaez-Moya R, Duran JA, et al. (2014) Corneal Wound Healing Promoted by 3 Blood Derivatives: An In-Vitro and In-Vivo Comparative Study. Cornea 33(6): 614-620.
- Alderman DD, Alexander RW (2011) Advances in Regenerative Medicine: High-density Platelet rich plasma and Stem cell prolotherapy for Musculo skeletal Pain. Practical Pain Management 11(8).






























