Accuracy of Assessing Magnification in Total Hip Arthroplasty Radiographs Utilizing a Two-Ball Bearing Marker
Andrew W Mack1, Olivia J Bono*2, Kevin Krasinski3, Addison Wilson4, David Whiddon5, James V Bono2
1 Walter Reed National Military Medical Center, Bethesda, MD, USA
2 New England Baptist Hospital, Boston, MA
3EmergeOrtho, Burlington, NC, USA
4 Beaufort Naval Hospital, Beaufort, SC, USA
5Orthopedic Associates of West Florida, Clearwater, Florida
Submission: June 01, 2018; Published: June 13, 2018
*Corresponding author: Olivia J Bono, New England Baptist Hospital, Boston, MA.
How to cite this article: Andrew W M, Olivia J B, Kevin K, Addison W, David W, James V B. Accuracy of Assessing Magnification in Total Hip Arthroplasty Radiographs Utilizing a Two-Ball Bearing Marker. Nov Tech Arthritis Bone Res. 2018; 3(1): 555605. DOI: 10.19080/NTAB.2018.03.555605
Abstract
This study evaluated the accuracy of a two-ball bearing radiographic marker on assessing the true magnification of post-operative total hip arthroplasty (THA) films. The effects of body mass index (BMI) and height on the measured error rates were also examined. We retrospectively reviewed 211 consecutive THA films. The implanted hemispherical acetabular component size was used to calculate the actual magnification. The average film magnification was 118.7%. There was a mean measured error rate of 1.27% (SD = 3.32) for this marker. No significant difference was found between measurements on consecutive post-operative films (n=52). BMI and height did not demonstrate any effect on error rate. These results support the use of this two-ball bearing marker as a reliable instrument for assessing x-ray magnification in pre-operative templating.
Introduction
Preoperative planning is paramount to successful total hip arthroplasty. It is well established that implanting undersized or oversized components for a given patient’s anatomy may lead to several complications including implant subsidence, early loosening, intraoperative fracture, and leg length discrepancy [1-7]. Templating of preoperative radiographs assists the surgeon in choosing appropriately sized femoral and acetabular components, as well as helping to develop a plan to reconstruct leg length, offset, and version through optimal component positioning [2,4,6,8,9,12-15].
Variation in the degree of magnification on a given x-ray is related to the changes in the distance of the object of interest from the x -ray plate. Due to this phenomenon, objects positioned closer to the x-ray plate will appear smaller than objects further away. This is analogous to the variation in the size of a shadow projected from a light source at a constant distance from a wall when one moves the object of interest closer to and further away from the wall. To perform accurate templating, it is critical to account for the degree of magnification of the x-ray image in order to make precise measurements and component size predictions [11, 12]. This holds true whether the surgeon utilizes a digital templating system or acetate overlays on a hardcopy film.
Therefore, radiographs used for templating need to be scaled to determine their true magnification. This requires the use of a radiographic marker of a known length or diameter. However, placement of a radiographic marker, by itself, does not ensure an accurate estimation of the x-ray magnification. Rather, the position of the marker in relation to the area of interest (i.e., hip joint) is vital to determining the magnification of the osseous structures [3,15,17].
Prior studies have examined the accuracy of a variety of radiographic markers in assessing magnification [2-5,8-10,13]. At our institution, a radiographic marker consisting of two ball bearings, spaced 100 mm apart, housed in a Plexiglas rectangular column has been used (Figure 1A-B). The objective of our study was to assess the accuracy of this 100mm marker in assessing the magnification of post-operative total hip arthroplasty films. Although the use of this marker has been described previously, no study to our knowledge has determined its accuracy [3].

Materials and Methods
Study design
A retrospective study of 237 consecutive patients undergoing primary total hip arthroplasty between June 15, 2005 and September 26, 2006 was performed. Prior approval was obtained from the hospital institutional review board (IRB). Only hips with hemispherical acetabular components, and therefore a uniform outer diameter, were examined. Those patients with non-hemispherical acetabular implants, 21 patients, or those without the radiographic marker visualized in its entirety on x-ray, 5 patients, were excluded from this study. Therefore, 211 patients (115 females, 96 males) were included for data analysis. A chart review was performed to determine acetabular component sizes and implant demographics from operative reports and implant sheets, as well as height/weight data. The implants analyzed included 161 Trident Hemispherical (Stryker, Kalamazoo, Ml), 31 Pinnacle® and 19 Duraloc® Option (Depuy, Warsaw, IN) acetabular components.
Radiographic Technique
The marker consists of two metal, spherical ball bearings, each 7.5 mm in diameter, spaced apart at a fixed distance of exactly 100 mm, encased in a radiolucent plastic rectangular column. The radiographic marker was affixed by the x-ray technician with tape to the patient’s lateral thigh at the level of the greater trochanter and in line with the longitudinal axis of the femur (in the coronal plane of the hip joint). The lower extremity was internally rotated 10 degrees to account for femoral anteversion and to bring the greater trochanter in the coronal plane of the hip joint. The x-ray beam was positioned 40 inches (101.6 cm) from the plate to obtain the AP hip postoperative x-rays.
Measurement and Calculations
Measurements of the marker and the acetabular component were made on each film utilizing the digital ruler tool on the IMPAX digital radiograph software (AGFA HealthCare, Greenville, SC). Measurements were performed by a single investigator blinded to the true acetabular component size. The hemispherical acetabular component on the AP hip x-ray was measured at its widest outer diameter (Figure 2).

The measured acetabular component size was compared with the true diameter of the implant obtained from the medical record. This ratio of measured component size to actual component size represents the true magnification of the film, as the acetabular component is in the plane of interest, the hip joint.
True Magnification Ratio = (measured cup size) / (actual cup size)
Once calculated, the true magnification ratio could be applied to the marker measurement to obtain a % error of the radiographic marker. For example, if the marker was placed in the correct coronal plane of the hip joint, the magnification of the marker would be 100% of the true magnification, and if the marker were placed anterior to the hip joint for the AP hip radiograph, the magnification would be greater than 100% of the true magnification (positive % error).
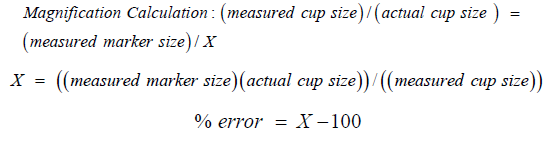
A body mass index (BMI= weight (kg)/height(m)2) for each patient was calculated based on the height and weight recorded in their chart at the time of surgery. The patients’ BMI were analyzed to determine if there was any correlation with the calculated % error of the radiographic marker.
Results
The 211 postoperative AP hip radiographs demonstrated a mean radiographic marker error of 1.27% (SD= 3.32). The mean film magnification was calculated to be 18.66% (SD= 5.90) as compared to the true size of the implanted acetabular component. The relationship between % error of the radiographic marker and patient BMI was evaluated using Pearson correlation and scatterplots. The Pearson correlation was 0.045 (P = 0.520) indicating no significant correlation between the two sets of data. Scatterplots also failed to demonstrate a relationship between % error and BMI. This held true when using linear, quadratic and cubic fit lines (Figures 3-5). Eliminating one outlier (% error> 10%) did not alter the results. Height was also not found to be associated with % error when it was examined as an independent variable with a Pearson correlation 144 of 0.11(P = 0.289).



Of the 211 patients, 52 had two consecutive post-op visits where radiographic marker x-rays were obtained, allowing for the evaluation of consistency of the % error rates between serial post-operative films. The mean radiographic marker error in this group of patients with a second post-operative x-ray was 1.75% (SD= 3.60). There was no significant difference found between the calculated % errors for the first and second post-operative films in the same patient, Pearson correlation -0.224 (P = 0.111). The 52 patients with second post-op films were also evaluated for any relationship with patient BMI. Again, no correlation was found, Pearson correlation 0.193 (P = 0.171).
Discussion
Pre-operative templating is an integral part of preparation for successful total hip arthroplasty. By preoperatively evaluating and calculating the leg length discrepancy, femoral offset, and hip center of rotation, the optimal biomechanics of the hip can be reconstructed intraoperatively.
Many acetate overlays traditionally used for templating assume a 120% magnification. However, assuming the magnification of a hip radiograph without knowing the actual magnification can lead to significant errors in templating. Prior studies have shown that by assuming a 120% magnification of an x-ray film, a surgeon can encounter up to an 11% inaccuracy in templating measurements, which may contribute to component oversizing or undersizing. Component oversizing can be a significant problem, and has been attributed to having a role in causing intraoperative periprosthetic fracture (3-25% incidence) in numerous studies [1,3,6,7,10,14]. Undersizing may lead to significant complications as well, resulting in component instability, loosening or subsidence, requiring revision surgery to correct [1,2,5,6,7,8,10].
Radiographic markers aid the surgeon in determining the actual magnification of a film. Other studies have examined the accuracy of radiologic markers in assessing magnification. A coin, calipers and a radiodense sphere have all been examined [2,4,5,14,16]. Although the columnar two-ball bearing marker used in this study has been described previously, to our knowledge it has not been studied for accuracy in assessing magnification. The two-ball-bearing radiographic marker, based on our data, is a reliable instrument to assess radiograph magnification and is comparable to other templating marker devices studied in the literature. Wimsey et al [2]. reported an error margin of 1.12% with a coin marker and 6.99% with a caliper. Similarly, The et al. reported a 1.5% margin of error with a 28mm femoral head marker [5]. Our study demonstrated a mean margin of error of 1.27% (average accuracy rate of 98.73%) which is consistent with prior published findings of these other radiographic markers [2-5,8,15-17]. This study also demonstrated the reproducibility of this marker by showing no significant difference between % error measurements in the same patient on consecutive post-operative x-rays. No other study in the literature, to our knowledge, specifically examined this consistency when evaluating other markers. The failure to establish a correlation between % error and BMI was somewhat unexpected. There are many variables in the process of taking an accurate and reproducible x-ray of a hip after arthroplasty surgery.
The distance of the x-ray source from the plate, patient positioning, marker location and technician technique may all play a role in introducing variability in the results. Our radiographic protocol is to place the radiographic marker on each of the patients’ lateral thighs in the coronal plane of the hip joint with the hip internally rotated, which brings the lateral position of the marker in-line with the hip joint. This technique may have helped to mitigate the effect of increasing thigh girth (using increased BMI as a surrogate) on altering the % error in hip film magnification. These findings support the use of this two-ball bearing radiologic marker as a reliable instrument to accurately assess x-ray magnification and consistently scale films for total hip arthroplasty templating.
References
- Schwartz JT, Mayer JG, Engh CA (1989) Femoral fracture during noncemented total hip arthroplasty. J Bone 193 Joint Surg Am 71: 1135- 1142.
- Wimsey S, Pickard R, Shaw G (2006) Accurate scaling of digital radiographs of the pelvis. J Bone Joint Surg Br 88:1508-1512.
- Gorski JM, Schwartz L (1986) A device to measure x-ray magnification in preoperative planning for cementless arthroplasty. Clin Ortho Relat Res 202: 302-306.
- Conn KS, Clarke MT, Hallet JP (2002) A simple guide to determine the magnification of radiographs and to improve the accuracy of preoperative templating. J Bone Joint Surg Br 84(2): 269-272.
- The B, Diercks RL, Stewart RE, van Ooijen PMA, van Horn JR (2005) Digital correction of magnification in pelvic x-rays for preoperative planning of hip joint replacement. Medical Physics 32(8): 2580-2589.
- Della Valle AG, Padgett DE, Salvati EA (2005) Preoperative planning for primary total hip arthroplasty. J Am Acad Orthop Surg 13(7): 455-462.
- Davidson D, Pike J, Garbuz D, Duncan CP, Masri BA (2008) lntraoperative Periprosthetic Fractures During Total Hip Arthroplasty: Evaluation and Management. J Bone Joint Surg Am 90(9): 2000-2012.
- Carter LW, Stovall DO, Young TR (1995) Determination of accuracy of preoperative templating of noncemented femoral prostheses. J Arthroplasty 10: 507-513.
- Knight JL, Atwater RD (1992) Pre-operative planning for total hip arthroplasty: quantitating its utility and precision. J Arthroplasty 7: 403-409.
- Gonzalez Della Valle A, Slullitel G, Piccaluga F, Salvati EA (2005) The precision and usefulness of preoperative planning for cemented and hybrid primary total hip arthroplasty. J Arthroplasty 20(1): 51-58.
- Clarke IC, Gruen T, Matos M, Amstutz HC (1976) Improved methods for quantitative radiographic evaluation with particular reference to total hip arthroplasty. Clin Orthop 121: 83-91.
- Linclau L, Dokter G, Peene P (1993) Radiological aspects in preoperative planning and postoperative assessment of cementless total hip arthroplasty. Acta Orthop Belg 59(2): 163-167.
- Unnanuntana A, Wagner D, Goodman SB (2009) The accuracy of preoperative templating in cementless total hip arthroplasty. J Arthroplasty 24(2): 180-186.
- Iorio R, Siegel J, Specht LM, Tilzey JF, Hartman A, Healy WL (2009) A comparison of acetate vs digital templating for preoperative planning of total hip arthroplasty: is digital templating accurate and safe? J Arthroplasty 24(2): 175-179.
- Gamble P, de Beer J, Petruccelli D, Winemaker M (2010) The accuracy of digital templating in uncemented total hip arthroplasty. J Arthroplasty 25(4): 529-532.
- Oddy MJ, Jones MJ, Pendegrass CJ, Pilling JR, Wimhurst JA (2006) Assessment of reproducibility and accuracy in templating hybrid total hip arthroplasty using digital radiographs. J Bone Joint Surg Br 88(5): 581-585.
- Crooijmans HJ, Laumen AM, van PuL C, van Mourik JB (2009) A new digital preoperative planning method for total hip arthroplasties. Clin Orthop Relat Res 467(4): 909-916.






























