Infantilecortical Hyperostosis (Caffeydisease); Apossible Misdiagnosisas Osteomyelitis
Raneem Almadani1, Abdulqader Alhebshi2* and Zuha Rashidi1
1Taibah University, KSA
2Pediatric Department, Prince Mohammed Bin Abdul Aziz Hospital, Saudi Arabia
Submission: December 08, 2017; Published: January 09, 2018
*Corresponding author: Abdulqader Alhebshi, Pediatric Department, National Guard Health Affairs, Prince Mohammed Bin Abdul Aziz Hospital, Saudi Arabia, Tel: 966-14-8669999; Fax: 966-14-8669966, Email: habshi05@hotmail.com
How to cite this article: Raneem Almadani, Abdulqader Alhebshi, Zuha Rashidi. Infantilecortical Hyperostosis (Caffeydisease); Apossible Misdiagnosisas Osteomyelitis. Nov Tech Arthritis Bone Res. 2018; 2(4) : 555591. DOI: 10.19080/NTAB.2017.02.555591
Abstract
Infantile cortical hyperostosis (Caffey disease) is characterized by spontaneous episodes of subperiosteal new bone formation along one or more bones commencing within the first5 months of life. It is featured byacuteinflammationofperiosteumandoverlyingsofttissuewhichcausesfever. Sometimes it can present as fever without focus. Generally, the diagnosis may be delayed as this disorder mimics a wide range of diseases including osteomyelitis, hypervitaminosis A, scurvy, bone tumors and child abuse. The purpose of this casereport is to emphasize the high index of suspicion of this disease in our country, and remind the clinicians about How a full history is important to reach the diagnose.
Keywords: Caffey disease; Infantile cortical hyperostosis; Osteomyelitis
Introduction
Caffey’s disease is a rare genetic disorder that classically presents with a clinical trial of fever, irritability, and soft tissues welling, in an infant with a radio graphical picture of cortical thickening or bony expansion, bridging of bones across inter osseous membrane, marginal sclerosis, and hyperostosis of flat bones [1]. The mandible (75%), clavicles, and ulnae are the bones most frequently involved, others being long bones, lateral ribs and iliac bones, the skull being rarest [2]. Diaphyseal involvement and meta physeals paring of long bones is noted giving a spindleshaped appearance of bones. The clinical importance stems from the fact that certain pathological conditions such as osteo myelitis, bone tumors, scurvy, hypervitaminosis A, and battered baby syndrome can resemble the radiographic findings of Caffey’s disease, thus warranting exclusion.
Case Report
An 8th month-old Saudi boy presentedonJuly4,2017to the Emergency department of Prince Muhammad Bin Abdulaziz Hospital (National Guard Health affairs) Medina, Saudi Arabia, with a history of sudden painful right jaws welling for two days (Figure 1), nofeverno history of trauma or insect bite. By physical examination there was mild diffuse firm, fullness and tenderness on the right jaw, the over lying skin was normal and no discharging in us or localized lymphadenopathy. On general examination there was mild tenderness in the right upper limb maximum in for ear mother wise was normal. Plain X-ray of upper limbs how edno fracture line or bony abnormality. Patient was discharged home.


After three weeks the patient presented again to the ER with excessive crying, irritability and right fore arms welling with pain for three days (Figure 2). No history of trauma or fallen down.
On examination, the baby was alert but irritable. Vital signs were normal except for low grade fever. There was swelling in the right forearm with tenderness, hotness but normal range of movement on all joints. Other system ic examination was unremarkable.
He is a baby of medically free mother, full-term, product of uneventful pregnancy, normal vaginal delivery, his birth weight was 2.72kg, He was exclusively on breast feeding, normal growth and development, immunization up-to-date according to Saudi vaccination program. No history for recent travel. Family history was insignificant.
His initial Investigation done in the ER showed WBCs countof14.6, neutrophils 37.60%, Lymphocytes, platelets 743x10^9/L, Hgb10.3gm/dl, CRP141.2, ESR105mm/hr, alkaline phosphatase 323(normal). Other laboratory tests were within normal range. Blood culture revealed no growth.
X-ray marked ulnar & radial diaphyseal periosteal reaction sparing their metaphases& epiphyses, with soft tissue swelling around the forearm (Figure 3). However, there were no osteolyticlesions.

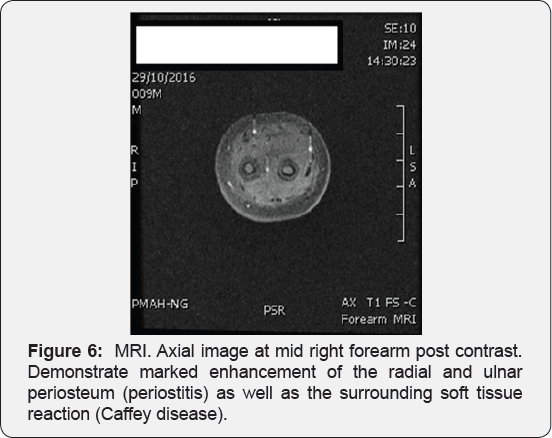
Orthopedic consultation done and advised to start empirical antibiotic for possible osteomyelitis. So, patient was admitted to hospital and started on amikacinand floxacillin after11 days of admission the patient still not improved, antibiotics changed to vancomycin and Ceftriaxone, and MRI of the right forearm pre & post contrast was done showed revealed marked radial & ulnar shaft periostitis with marked edematous /inflammatory changes in the surrounding structure (Figures 4-6). X-ray of the right mandible was done and it demonstrate marked periosteal reaction. Other skeletal survey to rule out child abuse showed no obvious periosteal reaction around the other flat bones (clavicle,scapula, ribs, clavicles or iliac bones). After what we found along with the non-improvement of the child condition we changed the diagnosis from osteomyelitisto Caffey's disease based on this clinical background (Bone biopsy and genetic study not done due to unavailability). The baby was discharged on Ibuprofen 10mg/kg PRN then here turned to pediatric clinic for follow up after four weeks of discharge with complete recovery


Discussion
Caffey disease, also known as Infantile Cortical Hyperostosis is a self-limiting disorder. It was first reported as a disease entity by Caffey and Silverman in 1945 [3]. The manifestations include irritability, swelling of the overlying soft tissue end cortical thickening of the underlying bones [1]. The swelling is painful with a wood like in duration but with no redness or warmth, thus suppuration is absent. There are usually noother signs and symptoms. Mandible is the most commonly involved site followed by scapula, clavicle, ribs and long bones. There are usually noother signs and symptoms [4-5]. The pain can be severe and canals result in pseudoparalysis. Other rare clinical findings included ysphagia, nasal obstruction and proptosis [6-8]. Laboratory findings include elevated ESR, and in some patient's high alkaline phosphatase, thrombocytosis, anemia and raised immunoglobulin levels [9,10].
The exactetiology of this condition is still unknown [11]. Most cases are sporadic, but a few familial cases with auto somal dominant and recessive patterns have been described [12]. Among the proposed causes are, infections, immunological defects and genetic abnormalities. Others studies discovery of a genelocus in 3 unrelated families with autosomal dominant inheritance (geneCOLIAL, 17q21)which encodesAlfa-1 chain of TypeI collagen, has raised some doubts whether some cases area type of Collagenopathy, like Osteogenesis imperfect [13,14]. Similar conditions have also been reported following prolonged treatment with Prostagl and in E1 for maintaining ductal patency in infants with cyanotic heart disease [15,16]. Two forms of Caffey disease have been described in literature, a classical mild infantile form (ICH) delineated by Caffey and Silver mananda severe form with prenatalonset. The incidence of the disease is unknown. Atotal of 44 cases have been reported with the severe prenatal on set of Cortical Hyperostosis [17].


Radiography is the most valuable diagnostic study in Caffey disease. Cortical new bone formation (Cortical Hyperostosis) beneath the regions of soft tissues welling in the diaphysis, sparing metaphysis and epiphysis is the characteristic feature [15]. While no laboratory tests are specific for diagnosis of ICH, the important differential diagnosis that are to be excluded are osteomyelitis, chronic hyper vitaminosis A, bone tumor, scurvy, child abuse and prolonged Prostagland in (PGE1) infusion [1519]. Consciousness of the presence of the Caffey disease is an uncommon condition but its regular clinical radiological outline will help patients. So, the Patients will no longer be forced to undergo needless investigation and medication Figures 7 & 8.
Conclusion
The condition should be taken under consideration when diagnosing this disease, that too with high level of uncertainty. A comprehensive history, clinical estimation, requisite laboratory inspection is needful to set aside the differential diagnoses. Plain radiography is adequate to assure the diagnosis in roughly every case.
References
- Kutty N, Thomas D, George L, John TB (2010) Caffey disease or infantile cortical hyperostosis: A case report. Oman Med J 25(2): 134-136.
- Phatak SV, Kolwadkar PK, Phatak MS (2004) Pictorial essay: Infantile cortical hyperostosis (Caffey's disease). Indian J Radiol Imaging 14: 185-186.
- CaffeyJ, Silverman WA (1945) Infantile cortical hyperostosis: preliminary report of a new syndrome. Am J Roentgenol 54: 1-16.
- Harris VJ, Ramilo J (1978) Caffey's disease: A case originating in the first metatarsal and review of a 12 year experience. AJR Am J Roentgenol 130(2): 335-337.
- Challapalli M, Cunningham DG, Varnado SC (1998) Infantile cortical hyperostosis and facial nerve palsy. Int J Pediatr Otorhinolaryngol 43(2): 175-178.
- Hall C (2005) Caffey disease Orphanet encyclopedia. accessed on April 3rd 2009.
- Sheppard JJ, Pressman H (1988) Dysphagia in Infantile corticalhy perostosis. Dev Med Child Neurol 30(1): 111-114.
- Faure C, Beyssac JM, Montague JP (1977) Predominant orbital and facial involvement in ICH. Pediatr Radiol 6: 103-106.
- Temperley IJ, Douglas SJ, Rees JP (1972) Raised immunoglobulin levels and thrombocytosis ininfantile cortical hyperostosis. Arch Dis Child. 47(256): 982-983.
- Kumar TS, Scott JX, Mathew LG (2008) Caffey disease with raised immunoglobulin levels and thrombocytosis. Indian J Pediatr 75: 181182.
- Restrepo S, Sanchez AM, Palacios E (2004) Infantile cortical hyperostosis of the mandible. Ear Nose Throat J 83(7): 454-455.
- Bernstein RM, Zaleska DJ (1996) Familial Aspects of Caffey Disease. Am J Orthop 24(7): 777-781.
- Glorieux FH (2005) Caffey disease: An unlikely collagenopathy. J Clin In vest 115(5):1142-1144.
- Caffey Diseasea type1 Collagenopathy, Current GGH 24(1) September 2005.
- Jao Fernando, Lourencode Almeida, Helio K, Luiz H, Hercowitz, et al. (2007) Cortical Hyperostosis secondary to prolonged use of prostaglandin. Clinics (Sao Paulo) 62(3): 363-366.
- Nadroo AM, Shivangi S, Garg M, Al-Sowaileen M (2000) Prostagl and in induced Infantile Cortical Hyperostosis. J Perinat Med 28: 447-452.
- Susan S, Rabih C, Comelia T, Katharina L, Stephan M, et al. (2003) Antenatal onset of cortical hyperostosis. Am J Med Genet A 120A(4): 547-552.
- Varma R, Johny VF (2005) Infantile cortical hyperostosis. Indian Pediatr 39(11):1057.
- Almada Rodriguez, Hugo D (2005) Non accidental injuries in Children- common pit falls accessed on 4th April2009.






























