Self-Efficacy-an Important Arthritis Pain Correlate and Possible Treatment Factor General Review and Commentary
Ray Marks*
Department of Health and Behavior Studies, Columbia University, USA
Submission: August 18, 2017; Published: September 08, 2017
*Corresponding author: Ray Marks, Department of Health and Behavior Studies, Department of Health, Physical Education & Gerontological Studies and Services, City Universityof New York, Teachers College, New York, USA, Tel:202-606-1211; Email: rmarks@york.cuny.edu
How to cite this article: Ray M. Self-Efficacy-an Important Arthritis Pain Correlate and Possible Treatment Factor General Review and Commentary. Nov Tech Arthritis Bone Res. 2017; 1(5) : 555574 DOI: 10.19080/NTAB.2017.01.555574
Background
Self-efficacy, a well-established psychological construct denoting an individual’s confidence to successfully carry out a specific activity or behavior was initially discussed in the 1970 as a potential disease mediator. This brief focuses on the salience of the link between having adequate confidence to deal with arthritis pain and its relationship to the pain experience, which is normally an unpleasant one and the most profound manifestation of arthritis. Originally propounded by Dr. Albert Bandura, the psychological variable of self-efficacy was proposed to explain the discrepancy between having knowledge about a skill and the actual performance of this skill. It was also predicted to influence motivation levels that might mediate the capacity and willingness to elicit behaviors that promote health despite disconfirming experiences [1-4]. Moreover, Bandura’s research depicted how self-efficacy judgments might determine the extent to which a person will or will not perform the adaptations needed to deal with chronic illnesses [2].
The finding that the degree of self-efficacy tended to predict how much effort might be expended on a task-and for how long- in the face of obstacles and negative situations, such as pain, was a further especially insightful research observation, especially in the context of arthritis care [4]. Indeed, in 1997, Bandura [4] argued these personal beliefs were fundamental to many desirable health related behaviors and practices, in the context of influencing health outcomes among people with chronic illnesses such as arthritis, a term referring to over one hundred forms of pain-provoking joint and muscle-related disorders that continue to pose an immense burden on both the affected individual, as well as society [5].
Indeed, with no prevailing cure for any form of arthritis, the importance of any understandings about the disease, especially understandings about modifiable factors that might be harnessed to reduce or minimize disability and maximize independence and life quality of the affected individual cannot be underestimated in this regard. In particular, given the link between a variety of human behaviors and several prevalent disease consequences of arthritis [6] such as pain, and between how people cope with chronic pain and disability [7], a key role for continuing to examine the role of self-efficacy in the context of efforts to reduce arthritis disability and optimize its outcomes has emerged [8].
But is there sufficient contemporary evidence to support the specific idea that self-efficacy perceptions for managing arthritis pain is a significant determinant of the severity of any prevailing arthritis pain, per se, and if so, what efforts should be forthcoming to more ably assist, enhance or promote the wellbeing of the arthritis client in this regard, other than efforts to directly.
To address these questions, this brief overview focuses on some relevant past and current research concerning the link between behavior specific arthritis self-efficacy beliefs and pain, the most important feature of arthritis. It also reviews selected processes for enhancing self-efficacy directly, as well as vicariously in the context of efforts to minimize arthritis pain.
In short, the present overview specifically examines:
i. If there evidence of a consistent association between the magnitude of one’s arthritis self-efficacy beliefs and arthritis pain, and/or between the extent of pain and the subject’s confidence beliefs for managing pain.
ii. If it is possible to increase arthritis pain self-efficacy and if so, what approaches other than isolated pain relieving interventions appear most promising.
Methods
All relevant publications in the PUBMED data base covering the years January 1980-August 2017 were sought. To be included, only English language publications concerning arthritis disability and pain self-efficacy were deemed acceptable, with few exceptions. The specific studies retrieved to address the study question one were categorized as either descriptive correlation or prospective studies. Management approaches were examined separately. Some of the author's observations are added to solidify the arguments. The key search terms used were 'arthritis' and ‘self-efficacy’ or 'pain self-efficacy’. Studies detailing instrumentation processes related to the topic were excluded. Studies that examined other forms of self-efficacy, rather than pain self-efficacy, as well as those that did not assess pain eg [9-12] were generally excluded, as were general selfefficacy studies eg, Brembo et al. [13].
Results
Among the 1135 articles housing the key words, 665 dealt specifically with pain self-efficacy topics, with 243 of these being published in the last 5 years. Many listings however, bore no relationship to the present questions of interest, and included efficacy studies, among those that matched the search criteria there were more correlation than prospective studies. Bearing in mind other data bases or key search terms may house or yield additional data, it is possible some works were overlooked, the majority of currently reported studies appear highly representative of this topic.
Correlation studies
Among the fair numbers of related cross-sectional studies that have examined some aspect of pain related self efficacy, the findings of these depicted in Table 1 imply a possible important relationship between arthritis pain self-efficacy and the extent of prevailing pain does exist. This relationship implies that the relationship is an inverse one between pain self-efficacy and pain experiences, and tends to prevail across different forms of this condition, even if the study designs differ and are not robust [14], negative studies may be missing or unpublished, and assessment approaches and samples studied preclude synthesis [Marks Knee Prop].

Abbreviations: OA=osteoarthritis; RA=rheumatoid arthritis; SE=self-efficacy
Indeed, while not all authors would agree in this respect eg [15-18], among those that support the view that pain related self-efficacy and pain are related in some way include Blamey et al. [19]. who found having low self-efficacy for taking care of, or for handling pain, not only correlated with increases in pain, but also with depression, anxiety levels, regular use of analgesics, fatigue and greater physical impairment. Self-efficacy scores also correlated with reported pain ratings [20], psychological thriving [21], and general perceptions about functional ability [22] among people with arthritis, regardless of level of physical function. Other findings shown in Table 1 indicate similar trends.
Consequently it seems plausible to infer that in addition to attempts to reduce pain directly, efforts to optimize self-efficacy for managing pain or both are likely to yield more favorable outcomes in the context of an arthritic condition, than not, despite the paucity of data, and considerable limitations in this body of cross sectional related literature[23-35].
Prospective studies linking pain self efficacy to arthritis outcomes
While there few prospective studies that have shown parallel trends between self-efficacy measurement scores and pain among arthritis patients, Holman, Mazonson & Lorig [36]. found arthritis patients who demonstrated long term postintervention self-efficacy improvements for managing pain, also demonstrated consistent significant early and sustained clinical improvements that seemed closely linked to changes in the participant's self-efficacy scores for pain and managing fatigue. Strong support for self-efficacy as a salient outcome predictor was later observed by Lorig, Mazonson & Holman [37]. as well as several independent researchers, for example, Yip et al. [38].
In accord with study results of Braden et al. [39] and Lorig & Holman [40], Allegrante et al. [41] who conducted a selfefficacy theory approach to enhancing short-term outcomes for persons with disabling knee osteoarthritis. This group found the interventions reduced pain levels, and improved arthritis self efficacy for managing pain, even though a one-year follow-up study [42] showed a much diminished carry-over effect.
Taal et al. [43] who attempted to help arthritis participants adjust to their exercise, rest and medication regimens, plus the cyclic nature of the disease, reported significant positive postintervention improvements in functional disability, and selfefficacy for overall function and knowledge. Although pain selfefficacy was not examined directly, these positive results, still evident 14 months after implementation, denoted a possible reduction in pain severity or an improved ability to cope with pain.
In another study, after combining the principles of selfmanagement, adult learning, case management and self-efficacy enhancement in an interdisciplinary program that integrated group and individualized treatment, Alderson et al. [44] reported significant increases in self-efficacy among 57 persons diagnosed as having arthritis who participated in such a program. These improvements were noted immediately following the program, and were sustained for up to six-months after the program. Disability and pain also decreased over the follow-up period.
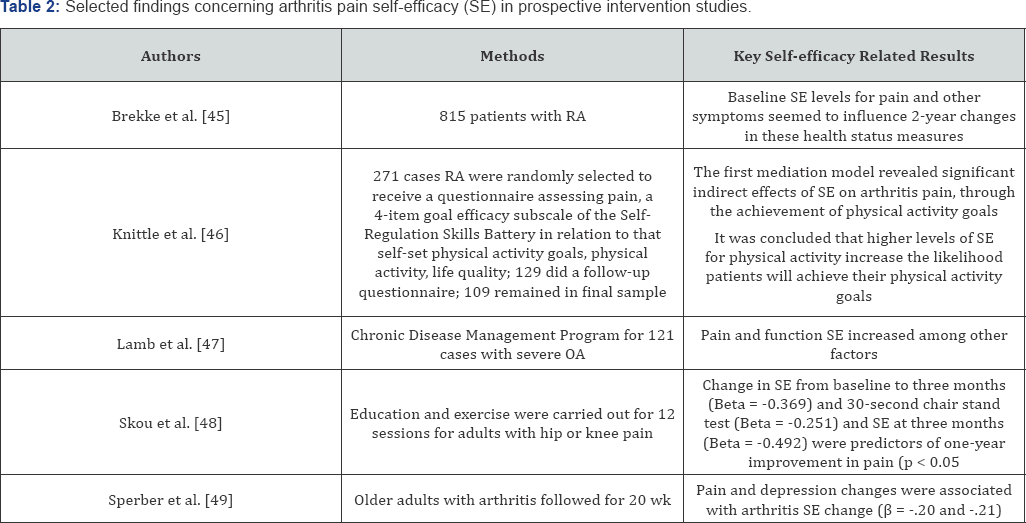
Similarly Brekke et al. [45] who conducted a longitudinal observational study of 306 patients with rheumatoid arthritis over a five year period showed that changes in self-efficacy regarding pain as well as other symptoms, were positively related to changes in perceived health status. This study also revealed that high levels of self-efficacy at baseline were positively related to improved pain perception after five years, and that mental distress at baseline was related to reduce selfefficacy after five years [45-50] (Table 2).
Self-efficacy enhancing approaches
Among a wide array of methods that may favourably impact arthritis pain self-efficacy, aquatic programs [50], cognitive behavioural self-help interventions [51], exercise and dietary weight loss approaches [52], exercise and education [53], online cognitive-behavioural self-management group therapy with weekly telephone support [54], tai-chi [55] and yoga [56] have been shown to be efficacious.
As well, self-management programs, combined with adaptive pain coping skills training interventions and social emotional support to strengthen self-efficacy expectations [57] have been found to enhance self-efficacy cognitions, plus the physical and psychological status of individuals with arthritis [28]. Educating spouses, significant family members and care-givers may also impact upon a patient's expectancies about their ability to control arthritis-related symptoms, such as pain and functional limitation in a positive way [58].
According to Bandura [1,4] and Strecher et al. [59], clinicians interested in
Heightening a patient's pains self-efficacy should attempt to:
i. Identify and reinforce the patient's past and present successes/ accomplishments in dealing with pain.
ii. Direct the patient to observe the successful pain control related behaviors of others.
iii. Provide positive feedback for the patient's efforts and/ or encourage people in the patient's social network to do this as well.
iv. Help patients to correctly interpret how and what they are feeling.
In particular, given that Jia et al. [60] found pain belief content to be a significant moderator in controlling pain, perhaps identifying the specific belief of the individual and targeted this will prove especially helpful. As outlined by Marks et al. [15], there are several sub-domains within the most well established self-efficacy tool for assessing arthritis self-efficacy, which do not yield consistent within-subject responses, and because these and their item or sub dimensions do not necessarily correlate perfectly, it might be especially helpful to pinpoint aspects of self-efficacy that need to be improved versus those that are adequate.
In addition, because self-efficacy is strengthened by actually performing the task in question, rather than just discussing this [61], helping the novice patient to carry out the actual task requirements in a step by step fashion is advocated. In addition, keeping adequate records, and offering positive reinforcement and encouragement as the new skill is learned is potentially of high import outlined by Alderson et al. [44].
Resnick [62] who conducted research to better understand the factors that influence efficacy beliefs dentified 11 major themes that might be useful in a rehabilitation plan including: fostering motivation and verbal encouragement, providing exposure to positive role models, having patients deal effectively with past experiences as well as current aversive physical sensations.
Additional research reveals that for purposes of enhancing pain self-efficacy:
a. The clinician should assess the extent of pain experienced by a patient during a demanding activity.
b. They should train the individual in pain reduction skills through relaxation, distraction or imagery.
c. They should have the patient repeat the demanding activity while applying the acquired pain reduction skills and monitor the improvements in pain that result [63].
In addition educating patients to better manage pain, cope with disease flares and any disease progression, as well as helping them to understand why and how emotional reactions can affect their disease status may be of additional value [24]. Moreover, structuring treatments in such a way that mastery experiences and positive feedback are maximized is indicated [64].
In addition, to ensure sustainability of results [65], coping skills training and related educational interventions, plus building and maintaining a sound patient-therapist relationship that permits mutual inquiry, information-giving, and the negotiation of activity goals important to the patient may be helpful. Identifying barriers to desired goals and solutions for overcoming these, setting short-term, rather than long-term goals for some desired achievement [66,67], implementing a series of modest progressive behavioral changes, each over short time periods, may likewise improve the ability of the individual to make successive changes that can reduce pain [68].
Breaking goals into achievable steps, starting with a task that will be easy to undertake and will most likely be successful, plus practicing these in different venues may further facilitate the success of any pain self-efficacy enhancing intervention approach [69]. However, because an individual is less likely to perform an activity they feel less than confident of, a discussion about how to overcome any perceived barriers in this respect may be required [70].
Benefits likely to accrue as a consequence of a well- designed tailored set of intervention strategies to enhance pain management self-efficacy are depicted below.
Discussion
Self-efficacy, denoting anindividual’s perception ofconfidence to deal with negative situations or carry out desirable behaviors, which has been studied for more than 50 years, appears to be an important determinant of the overall pain experience of the arthritic patient [71] Commonly measured using a self-reported rating on a 0-10 or 10-100 scale, a small number of prospective studies that specifically assessed aspects of pain self-efficacy appear to confirm that regardless of numbers of affected joints, joint sites, or arthritis diagnosis, continuing to explore the role that self-efficacy perceptions play in the arthritis-pain cycle may have important clinical implications, regardless of disease stage. In particular, bolstering a patient's pain self-efficacy may not only help to reduce pain directly, but may help patients to maintain an optimal level of physical function, despite the progressive nature of most of these arthritic diseases [eg., 72], even if general selfefficacy is found unrelated to pain disability [34].
Although it is unclear what the specific approach is likely to prove optimal in heightening an individual's arthritis patient’s pain self-efficacy level, sufficient research indicates the clinician should select the intervention method(s) that will most closely achieve the desired outcomes for a given individual, and concentrate on those patients whose self-efficacy is found to be low to moderate, rather than satisfactory [73]. Given that theory based interventions are in general, more efficacious in the longterm than those that are a theoretical,, careful application of the steps enumerated in this brief for directly enhancing self-efficacy may produce more far reaching results than relying on vicarious self-efficacy improvements that eminate from the application of a variety of physical modalities and others.
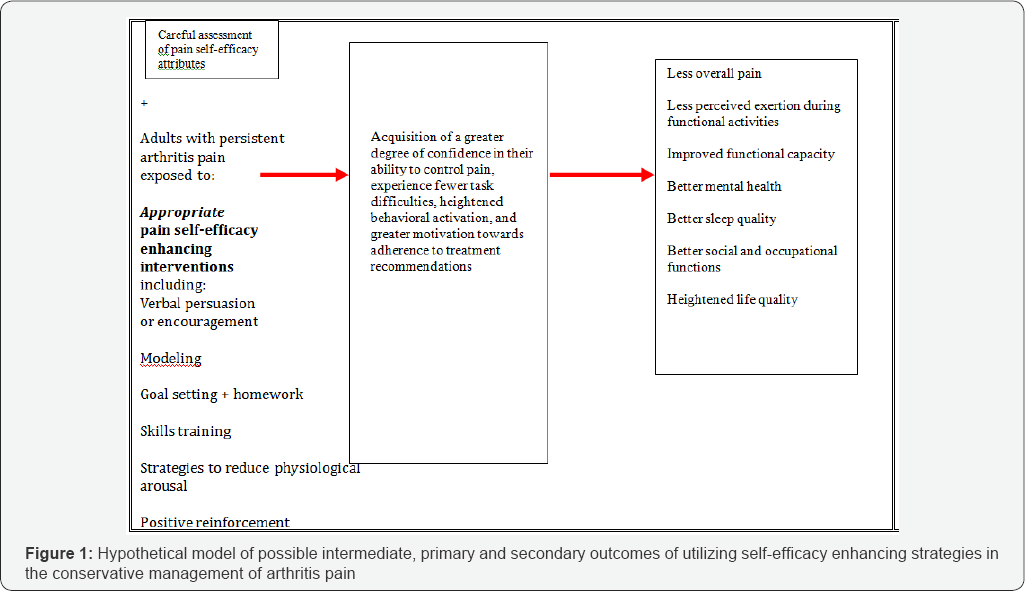
To reduce pain, as outlined inFigure 1, the desired strategies must be carefully construed and implemented on the basis of a sound comprehensive assessment of the clinical status of the patient, including recognition of the impact of age, mental health status, actual pain levels, and general capacity towards self generated pain control efforts. Keeping adequate progress notes may help to detect patterns of import to guide further treatment suggestions both for the patient in question, as well as future patients, as may detailed personal journals that focus on the patients’ daily activities, and nature of any pain flare up. These activities could also be extended to include any emotional, mental, social, and work related issues that might enable a pattern to emerge. Based on available data, it can be anticipated that patients will probably suffer less, and begin to feel more in Although it is unclear what the specific approach is likely to prove optimal in heightening an individual's arthritis patient’s pain self-efficacy level, sufficient research indicates the clinician should select the intervention method(s) that will most closely achieve the desired outcomes for a given individual, and concentrate on those patients whose self-efficacy is found to be low to moderate, rather than satisfactory [73]. Given that theory based interventions are in general, more efficacious in the longterm than those that are a theoretical,, careful application of the steps enumerated in this brief for directly enhancing self-efficacy may produce more far reaching results than relying on vicarious self-efficacy improvements that eminate from the application of a variety of physical modalities and others. control, while reducing their dependence on pharmaceutical drugs. Even if surgery is contemplated, the ability to confidently deal with post-operative pain situations will possible assist in furthering the well-being of the patient.
Since there is presently no cure for any form of arthritis, and the literature is increasingly turning to cognitive factors that mediate or moderate arthritis symptoms and disease severity, it appears research to specifically differentiate those forms of arthritis or stages of arthritis that may be most favorably influenced by well designed pain self-efficacy enhancing interventions may prove highly beneficial. Comparative studies to examine whether self-efficacy theory based approaches to reduce pain do so to a greater extent than educational or other therapeutic interventions alone, which has not been well examined, also deserves evaluation. Similarly, because results presently observed in the available arthritis studies may have inadvertently have underestimated the precise nature of the factors that undermine a particular patient's pain related coping confidence, or have been too short in duration to permit significant and desirable changes to emerge, more contemporary behavior specific approaches to assessing this variable, along with objective pain and performance measures, plus the implementation of diverse interventions over extended time periods also deserves attention.
In the interim, short-term self-efficacy enhancing interventions may still yield significant early and sustained treatment benefits including the ability to manage arthritis pain [70]. Importantly, these observed improvements are likely to be commensurate with those obtained by arthritis medications, while reducing utilization of, and dependency upon, health care services [40]. However, it is possible that important benefits that could be derived will be overlooked if the clinician as well as the researcher continue to examine the concept of pain self-efficacy solely as an aggregate psychological factor, rather than also examining item responses, or assessing pain relative to aspects of behavior that are not directly pain related.
In the following example of the magnitude of self-efficacy perceptions with respect to pain and other symptoms management scores as outlined by Lorig et al. [74], where a 10 represents low confidence or certainty and 100 represents high confidence or certainty for 5 and 6 subscale items is depicted alongside other variables over time. The single sample was an elderly community dweller with mild to moderate knee osteoarthritis undergoing an exercise intervention program. As shown below, the aggregate scores on the pain self-efficacy scale are depicted over time, and comprise 5 items that examine:
i. Certainty about one's ability to decrease pain substantively.
ii. Certainty about one's ability to continue activity.
iii. Certainty about one's ability to control pain to be able to sleep.
iv. Certainty about one’s use of methods other than medication to relieve pain.
v. Certainty of benefits for making large pain reduction with methods other than medication.
In this example-we may note firstly that the self-efficacy average score for managing pain is clearly in the low range, and less profound than that expressed for the subject's self-efficacy perceptions regarding the ability to function, suggesting that pain self-efficacy is not only an important highly important correlate in its own right in this particular case, but that different self-efficacy domains and dimensions cannot be used interchangeably to infer another. Moreover, even though a comprehensive intervention program, including exercise, was diligently delivered and pursued for more than three months, and function was heightened considerably, neither rain nor self-efficacy for managing pain, or function was heightened. In addition, certain item scores on the pain self-efficacy scale were lower post-treatment, even though others improved or were maintained.
In terms of the application of this data, a similar analysis made on a case by case basis at the outset for any individual client, as well as at the closure of treatment. This approach might not only indicate where no specific intervention is required, but might also depict other dimensions of pain related perceptions where self-efficacy is less than optimal and might hence warrant interventions that are more targeted and dimension specific than generic. Such an approach might also foster a better understanding of intervention results and what else in needed to assist the patient to progress optimally in the realm of pain control, as well as health status, rather than to regress [75-78] (Table 3).

*5 Pain Items embedded in the Self Efficacy of the Arthritis Self-Efficacy Scale Instrument of 3 Domains that include the certainty about one's ability:
1. To decrease pain substantively
2. To continue activity
3. To control pain to be able to sleep
4. To use of methods other than medication to relieve pain
5. To make large pain reductions with methods other than medication
**Other Symptoms Self Efficacy Items include certainty about one's ability:
1. To control fatigue
2. To be active without aggravating condition
3. To be able to do something to help oneself feel better if feeling blue
4. To be able to manage pain compared to others with arthritis
5. To be able to manage symptoms so as to enjoy things of value
6. To be able to deal with frustration of arthritis
*76 year old community dwelling female weighing 68 kg with a 7 year history of radiographically confirmed grade one degree right knee osteoarthritis and a history of hypertension who underwent intensive rehabilitation in a group along with an individualized exercise regimen 3 times a week for 3 months Self-efficacy for managing arthritis pain appears to be an important possible predictor or mediator of disease outcomes among people with various forms of arthritis. Linked to other problems that impact pain and disability, such as depression, and fear of movement, the assessment of pain self-efficacy and efforts to heighten this where deficient may serve as an important treatment target that has not been readily exploited to date, especially in the context of arthritic diseases other than rheumatoid arthritis [79, 80].
However, data do suggest that efforts to examine specific attributes of self-efficacy that underpin pain management and its control are more likely than generic approaches to assist arthritis patients in exercising better control over their disease, while lowering their sense of helplessness. In turn, those patients with high perceived self-efficacy scores are more likely to experience better health outcomes, especially in the realm of controlling excessive pain [75], regardless of intervention mode or disease stage.
While some individuals with arthritis may clearly be sufficiently confident to cope with certain aspects of controlling their pain, they should still be examined closely at the outset to garner if they perceive they may be less than highly confident in their ability to undertake recommended self-management strategies and others. After that, ascertaining where the patient is less than optimally confident is specifically recommended in efforts to successfully increase their confidence and to help them adapt successfully to their condition in face its many deleterious and disabling consequences. Adequately assessing this variable, which is easy to measure and interpret, and thereafter intervening accordingly using self-efficacy theory, rather than less strategic approaches is especially indicated.
These theory-based strategies include but are not limited to:
i. Exposing the patient to salient role models who have succeeded in managing pain over the course of their disease.
ii.Taking a skills-based approach.
iii. Encouraging graduated behavioral and therapeutic practices.
iv. Encouraging salient reinterpretation of pain experiences.
v. Applying timely feedback, and practice opportunities.
vi. Promoting decision-making and problem-solving.
vii. Helping patient to set and attain achievable valued short-term, rather than long-term goals.
viii. Providing frequent follow-up and consultation opportunities and an empathetic approach.
ix. Rewarding experiences of success and achievement of desired outcomes.
References
- Bandura A (1977) Social Learning Theory. Englewood Cliffs, NJ Prentice Hall 2(3): 247.
- Bandura A (1986a) Social Foundations of Thought and Action: A Social Cognitive Theory. Englewood Cliffs, NJ Prentice Hall.
- Bandura A (1986b) Self-efficacy mechanism in physiological activation and health promoting behavior. Madden J, Matthysse S, Barchas J (Eds.), Adaptation, Learning and Affect, Raven Press, New York, USA.
- Bandura A (1997) Self efficacy: The exercise of control. W H Freeman and Company, New York, USA, p. 3.
- Baruth M, Wilcox S, Schoffman DE, Becofsky K (2013) Factors associated with disability in a sample of adults with arthritis. Disabil Health J 6(4): 377-384.
- Pells JJ, Shelby RA, Keefe FJ, Dixon KE, Blumenthal JA, et al. (2008) Arthritis self-efficacy and self-efficacy for resisting eating: Relationships to pain, disability, and eating behavior in overweight and obese individuals with osteoarthritic knee pain. Pain 136(3): 340-347.
- Arnstein P (2000) The mediation of disability by self efficacy in different samples of chronic pain patients. Disabil Rehabil 20(17): 794-801.
- Sharma L, Cahue S, Song J, Hayes K, Pai YC, et al. (2003) Physical functioning over three years in knee osteoarthritis: role of psychosocial, local mechanical, and neuromuscular factors. Arthritis Rheum 48(12): 3359-3370.
- Zhaoyang R, Martire LM, Sliwinski MJ (2017) Morning self-efficacy predicts physical activity throughout the day in knee osteoarthritis. Health Psychol 36(6): 568-576.
- Moe RH, Grotle M, Kjeken I, Olsen IC, Mowinckel P, et al. (2016) Effectiveness of an integrated multidisciplinary osteoarthritis outpatient program versus outpatient clinic as usual: a randomized controlled trial. J Rheumatol 43(2): 411-418.
- Quicke JG, Foster NE, Ogollah RO, Croft PR, Holden MA (2017) Relationship between attitudes and beliefs and physical activity in older adults with knee pain: secondary analysis of a randomized controlled trial. Arthritis Care Res 69(8): 1192-1200.
- Schulz S, Brenk-Franz K, Kratz A, Petersen JJ, Riedel-Heller SG, et al. (2015) Self-efficacy in multimorbid elderly patients with osteoarthritis in primary care--influence on pain-related disability. Clin Rheumatol 34(10): 1761-1767.
- Brembo EA, Kapstad H, Van Dulmen S, Eide H (2017) Role of selfefficacy and social support in short-term recovery after total hip replacement: a prospective cohort study. Health Qual Life Outcomes 15(1): 68.
- Maly M, Costigan P, Olney S (2005) Contribution of psychosocial and mechanical variables to mobility outcome measures in knee OA. Phys Ther 85(12): 1318-1328.
- Marks R (2007) Physical and psychological correlates of disability among a cohort of individuals with knee osteoarthritis. Can J Aging 26(4): 367-377.
- Benyon K, Hill S, Zadurian N, Mallen C (2010) Coping strategies and self-efficacy as predictors of outcome in osteoarthritis: a systematic review. Musculoskeletal Care 8(4): 224-236.
- Thompson DP, Moula K, Woby SR (2016) Are fear of movement, selfefficacy beliefs and fear of falling associated with levels of disability in people with osteoarthritis of the knee? A cross sectional study. Musculoskeletal Care doi: 10.1002/msc.1167.
- Maly MR, Robbins SM (2014) Osteoarthritis year in review 2014: rehabilitation and outcomes. Osteoarthritis Cartilage 22(12): 19581988.
- Blamey R, Jolly K, Greenfield S, Jobanputra P (2009) Pattern of analgesic use, pain and self-efficacy: a cross-sectional study of patients attending a hospital rheumatology clinic. BMC Musculoskelet Disord 10: 137.
- Rejeski WJ, Craven T, Ettinger WH, McFarlane M, Shumaker S (1996) Self -efficacy and pain in disability with osteoarthritis of the knee. J Gerontol B Psychol Sci Soc Sci 51: 24-29.
- Sirois FM, Hirsch J K (2013) Associations of psychological thriving with coping efficacy, expectations for future growth, and depressive symptoms over time in people with arthritis. J Psychosom Res 75(3): 279-286.
- Mendes de Leon CF, Seeman TE, Baker DI, Richardson ED, Tinetti ME (1996) Self-efficacy, physical decline, and change in functioning in community-living elders: a prospective study. J Gerontol B Psychol Sci Soc Sci 51(4): S183-190.
- Ahlstrand I, Vaz S, Falkmer T, Thyberg I, Björk M (2017) Self-efficacy and pain acceptance as and men with rheumatoid arthritis. Clin Rehabil 31(6): 824-834.
- Barlow JH, Cullen LA, Rowe I F (2002) Educational preferences, psychological well-being and self-efficacy among people with rheumatoid arthritis. Patient Educ Counsel 46(1): 11-19.
- Buescher KL, Johnston JA, Parker JC, Smarr KL, Buckelew S P, et al. (1991) Relationship of self-efficacy to pain behavior. J Rheumatol 18(7): 968-972.
- Dogan N, Gôriç S, Demir H (2016) Levels of pain and self-efficacy of individuals with osteoarthritis. Agri 28(1): 25-31.
- Helminen EE, Sinikallio SH, Valjakka AL, Väisänen Rouvali RH, Arokoski JP (2016) Determinants of pain and functioning in knee osteoarthritis: a one-year prospective study. Clin Rehabil 30(9): 890-900.
- Keefe F J, Lefebvre JC, Maixner W, Salley AN, Caldwell DS (1997) Self-efficacy for arthritis pain: Relationship to perception of thermal laboratory pain stimuli. Arthritis Care Res 10: 177-184.
- Lefebvre JC, Keefe FJ, Affleck G, Raezer LB, Starr K, et al. (1999) The relationship of arthritis self efficacy to daily pain, daily mood, and daily pain coping in rheumatoid arthritis patients. Pain 80(1-2): 425-435.
- Packham JC, Hall MA, Pimm TJ (2002) Long-term follow-up of 246 adults with juvenile idiopathic arthritis: predictive factors for mood and pain. Rheumatology (Oxford) 41(12): 1444-1449.
- Porter LS, Keefe FJ, Wellington C, de Williams A (2008) Pain communication in the context of osteoarthritis: patient and partner self-efficacy for pain communication and holding back from discussion of pain and arthritis related concerns. Clin J Pain 24(8): 662-668.
- Sinikallio SH, Helminen EE, Valjakka AL, Väisänen-Rouvali RH, Arokoski JP (2014) Multiple psychological factors are associated with poorer functioning in a sample of community-dwelling knee osteoarthritis patients. J Clin Rheumatol 20(5):261-267.
- Somers TJ, Shelby RA, Keefe FJ, Godiwala N, Lumley MA, et al.(2010) Disease severity and domain-specific arthritis self-efficacy: relationships to pain and functioning in patients with rheumatoid arthritis. Arthritis Care Res (Hoboken) 62(6): 848-856.
- Schulz S, Brenk-Franz K, Kratz A, Petersen JJ, Riedel-Heller SG, (2015) Self-efficacy in multimorbid elderly patients with osteoarthritis in primary care--influence on pain-related disability. Clin Rheumatol34(10): 1761-1767.
- Wallis JA, Webster KE, Levinger P, Fong C, Taylor NF (2014) A preoperative group rehabilitation programme provided limited benefit for people with severe hip and knee osteoarthritis. Disabil Rehabil 36(24):2085-2090.
- Holman H, Mazonson P, Lorig K (1989) Health education for selfmanagement has significant early and sustained benefits in chronic arthritis. Trans Assoc Am Phys 102: 204-208.
- Lorig K, Mazonson PD, Holman H (1993) Evidence suggesting that health education for self-management in patients with chronic arthritis has sustained health benefits while reducing health care costs. Arthritis Rheum 36(4): 439-446.
- Yip YB, Sit JW, Wong DY, Chong SY, Chung LH (2008) A 1-year follow-up of an experimental study of a self-management arthritis programme with an added exercise component of clients with osteoarthritis of the knee. Psychol Health Med 13(4): 402-414.
- Braden CJ, McGlone K, Pennington F (1993) Specific pyschosocial and behavioral outcomes from the systemic lupus erythematosus self-help course. Health Educ Q 20(1): 29-41.
- Lori K, Holman H (1993) Arthritis self-management studies: a twelve year review. Health Educ Q 20(1): 17-28.
- Allegrante JP, Kovar PA, Mackenzie CR, Peterson MG, Gutin B (1993) A walking education program for patients with osteoarthritis of the knee: Theory and intervention strategies. Health Educ Q 20(1): 63-81.
- Sullivan T, Allegrante JP, Peterson MG, Kovar P A, MacKenzie CR (1998) One -year follow up of patients with osteoarthritis of the knee who participated in a program of supervised fitness walking and supportive patient education. Arthritis Care Res 11: 228-233.
- Taal E, Riemsma R, Brus H, Seydel E, Rasker J, et al. (1993) Group education for patients with rheumatoid arthritis. Patient Educ Couns 20(2-3): 177-187.
- Alderson M, Starr L, Gow S, Moreland J (1999) The program for rheumatic independent self-management: A pilot evaluation. Clin Rheumatol 18(4): 283-292.
- Brekke M, Hjortdahl P, Kvien TK (2003) Changes in self-efficacy and health status over 5 years: A longitudinal observational study of 306 patients with rheumatoid arthritis. Arthritis Rheum 49(3): 342-348.
- Knittle KP, De Gucht V, Hurkmans EJ, Vlieland TP, Peeters AJ, et al.(2011) Effect of self-efficacy and physical activity goal achievement on arthritis pain and quality of life in patients with rheumatoid arthritis. Arthritis Care Res (Hoboken) 63(11): 1613-1619.
- Lamb SE, Toye F, Barker KL (2008) Chronic disease management programme in people with severe knee osteoarthritis: efficacy and moderators of response. Clin Rehabil 22(2): 169-178.
- Skou ST, Simonsen ME, Odgaard A, Roos EM (2014) Predictors of longterm effect from education and exercise in patients with knee and hip pain. Dan Med J 61(7): A4867.
- Sperber N, Hall KS, Allen K, Devellis BM, Lewis M, et al. (2013) The role of symptoms and self-efficacy in predicting physical activity change among older adults with arthritis. J Phys Act Health 11(3): 528-535.
- Guo L, Yang H, Malkin MM (2009) Self-efficacy and arthritis impact on health: the effect of an Arthritis Foundation Aquatic Program. Am Recreational Ther 8: 9-19.
- Garnefski N, Kraaij V, Benoist M, Bout Z, Karels E, et al. (2013) Effect of a cognitive behavioral self-help intervention on depression, anxiety, and coping self-efficacy in people with rheumatic disease. Arthritis Care Res (Hoboken) 65(7): 1077-1084.
- Focht BC, Rejeski WJ, Ambosius WT, Katula JA, Messier SP (2005) Exercise, self-efficacy, and mobility performance in overweight and obese older adults. Arthritis Rheum 53(5): 659-665.
- Hopman RM, Westhoff MH (2000) The effects of a health educational and exercise program for older adults with osteoarthritis of the hip or knee. J Rheumatol 27(8): 1947-1954.
- Shigaki CL, Smarr KL, Siva C, Ge B, Musser D, et al. (2013) RAHelp: An online intervention for individuals with rheumatoid arthritis. Arthritis Care Res (Hoboken) 65(10): 1573-1581.
- Waite Jones JM, Hale CA, Lee HY (2013) Psychosocial effects of Tai Chi exercise on people with rheumatoid arthritis. J Clin Nurs 22(21-22): 3053-3061.
- Evans S, Moieni M, Lung K, Tsao J, Sternlieb B, et al. (2013) Impact of iyengar yoga on quality of life in young women with rheumatoid arthritis. Clin J Pain 29(11): 988-997.
- Taal E, Rasker JJ, Seydel ER, Wiegman O (1993) Health status, adherence with health recommendations, self-efficacy and social support in patients with rheumatoid arthritis. Patient Educ Counsel 20(2-3): 63-76.
- Martire LM, Schulz R, Keefe F J, Starz TW, Osai TA, et al. (2003) Feasibility of a dyadic intervention for management of osteoarthritis: a pilot study with older patients and their spousal caregivers. Aging Ment Health 7(1): 53-60.
- Strecher VJ, DeVellis BM, Becker MH, Rosenstock IM (1986) The role of self -efficacy in achieving health behavior change. Hlth Educ Quart 13: 73-92.
- Jia X, Jackson T (2016) Pain beliefs and problems in functioning among people with arthritis: a meta-analytic review. J Behav Med 39(5): 735756.
- Blazer DG (2002) Self-efficacy and depression in late life: a primary prevention proposal. Aging Ment Health 6(4): 315-324.
- Resnick, B (2002) Geriatric rehabilitation: the influence of efficacy beliefs and rehabilitation. Rehabil Nurs 27(4): 152-159.
- O'Leary A, Schoor S, Lorig K, Holman HR (1988) A cognitive-behavioral treatment for rheumatoid arthritis. Health Psychol 7(6): 527-544.
- Jerome GJ, Marquez D X, McAuley E, Canaklisova S, Snook E, et al. (2002) Efficacy effects on feeling states in women. Int J Behav Med 9(2): 139-154.
- Hammond A, Freeman K (2006) Community patient education and exercise or people with fibromyalgia: A parallel group randomized controlled trial. Clin Rehabil 20(10): 835-846.
- Bandura A, Schunk DH (1981) Cultivating competence, self-efficacy, and intrinsic interest through proximal self-motivation. J Personality Soc Psychol 41(3): 586-598.
- Jensen GM, Lorish CDP (1994) Promoting patient cooperation with exercise programs. Linking research, theory and practice. Arthritis Care Res 7(4): 181-189.
- Bandura A, Simon KM (1977) The role of proximal intentions in selfregulation of refractory behavior. Cognitive Therapy and Research 1(3): 177-198.
- Lorig K (1986) A short guide to self-efficacy. Arthritis Health Professional Association 21st Annual Scientific Meeting, New Orleans Louisiana 3-7.
- Barlow JH, Turner AP, Wright CC (1998) Long-term outcomes of an arthritis self-management programme. Brit J Rheumatol 37(12): 1315-1319.
- Urquhart DM, Phyomaung PP, Dubowitz J, Fernando S, Wluka AE, et al. (2015) Are cognitive and behavioural factors associated with knee pain? A systematic review. Semin Arthritis Rheum 44(4): 445-455.
- Brassington GS, Atienza AA, Perczek RE, DiLorenzo TM, King AC (2002) Intervention-related cognitive versus social mediators of exercise adherence in the elderly. Am J Prev Med 23(2): 80-86.
- Makelainen P, Vehvilaainen-Julkunen K, Pietil A (2009) Change in knowledge and self-efficacy of patients with rheumatoid arthritis: a six-month follow-up study. Int J Nurs Practice 15(5): 368-375.
- Lorig K, Chastain RL, Ung E, Shoor S, Holman HR (1989) Development and evaluation of a scale to measure perceived self efficacy in people with arthritis. Arthritis Rheum 32(1): 37-44.
- Heiberg T, Kvein TK (2002) Preferences for improved health examined in 1,024 patients with rheumatoid arthritis: pain has highest priority. Arthritis Rheum 47(4): 391-397.
- Marks R (2014) Self-efficacy and arthritis disability: an updatedThis work is licensed under Creative Commons Attribution 4.0 License synthesis of the evidence base and its relevance to optimal patient care. Health Psychol Open 1(1): 2055102914564582.
- Marks R (2014) Perceived health status of women with knee osteoarthritis: a cross-sectional study of the relationships of age, body mass, pain and walking limitations. Open Orthop J 8: 255-263.
- Adegoke BOA, Boyinde OH, Odole AC, Akosile CO, Bello AI (2017) Do self-efficacy, body mass index, duration of onset and pain intensity determine performance on selected physical tasks in individuals with unilateral knee osteoarthritis? Musculoskelet Sci Pract 32: 1-6.
- . Brand E, Nyland J, Henzman C, McGinnis M (2013) Arthritis selfefficacy scale scores in knee osteoarthritis: a systematic review and meta-analysis comparing arthritis self-management education with or without exercise. J Orthop Sports Phys Ther 43(12): 895-910.
- Orengo C, Wei S, Molinari V, Hale D, Kunik M (2001) Functioning in rheumatoid arthritis: the role of depression and self-efficacy. Clin Gerontol 23(3-4): 45.






























