Cavernous Sinus Syndrome Secondary to Internal Carotid Aneurysm
El Hadji Malick Sy*, Aissatou Aw, Lamine Ndiaye, Soda Mbaye, Mohamed Ndiaye, Ousmane Ndiaga Senghor, Serigne Sohibou Gaye and Papa Amadou Ndiaye
Abass Ndao Hospital Eye Center, Cheikh Anta University of Dakar, Senegal
Submission: January 23, 2024; Published: February 14, 2024
*Corresponding author: El Hadji Malick SY, Abass Ndao Hospital Eye Center, Cheikh Anta University of Dakar, Senegal
How to cite this article: El Hadji Malick S, Aissatou A, Lamine N, Soda M, Mohamed N, et al. Cavernous Sinus Syndrome Secondary to Internal Carotid Aneurysm. JOJ Ophthalmol. 2024; 10(4): 555791. DOI: 10.19080/JOJO.2024.10.555791
Abstract
Purpose: The goal of this work is to share a rare case of cavernous sinus syndrome diagnosed in our department and to highlight the challenges in managing this condition in our department.
Observation: It was a 48-year-old known hypertensive patient who presented with a sudden decrease in visual acuity associated with a drooping of the right upper eyelid over the past month. The ophthalmological examination revealed a visual acuity limited to 1/10th, severe ptosis, complete ophthalmoplegia, decreased corneal sensitivity, areflexic mydriasis, and papillary edema in the right eye. The left eye showed no particularity. Angio-MRI revealed a partially thrombosed aneurysm of the right internal carotid artery, causing compression of the vascular and neural elements due to mass effect. The patient treatment required a transfer to the Neurosurgery Department.
Discussion: Internal carotid artery aneurysm is a rare cause of cavernous sinus syndrome. The diagnosis is primarily clinical, and neuroimaging confirms the origin of the condition. Endovascular treatment has revolutionized management, which depends on the size, location, and integrity of the aneurysm.
Conclusion: The cavernous sinus syndrome is a diagnostic and therapeutic emergency. Its management is delicate and relies on embolization. The prognostic of this condition remains reserved in our countries, even with the advent of new revolutionary techniques.
Keywords: Cavernous sinus; Aneurysm; MRI; Embolization; Ophthalmoplegia
Abbreviations: CSS: Cavernous Sinus Syndrome; CT: Computed Tomography; MRI: Magnetic Resonance Imaging
Introduction
Involvement of the cavernous sinus can simultaneously lead to involvement of one or several cranial nerves because it is an anatomical crossroads. When this involvement of the cranial nerves is associated with that of the sympathetic chain and/or the optic nerve, it is referred to as cavernous sinus syndrome (CSS) [1]. It can be secondary to pathological conditions such as tumors, trauma, infection, malformation, or inflammation, but also vascular conditions like fistulas or aneurysms [1]. In the case of an aneurysm of the cavernous portion of the internal carotid artery, it is often responsible for compression of various adjacent structures, leading to the observed signs. Vascular involvement of the cavernous sinus is most often spontaneous, progressive, and associated with risk factors such as arterial hypertension, age, and smoking [1]. The diagnosis of cavernous sinus syndrome (CSS) is essentially twofold, involving clinical suspicion and radiological confirmation. Computed tomography (CT), magnetic resonance imaging (MRI), and/or arteriography are essential for highlighting these involvements [2,3]. Therapeutic management has significantly advanced with the advent of interventional neuroradiology. However, in case of failure of endovascular treatment, surgery remains a therapeutic alternative [3]. In this study, we report a case of cavernous sinus syndrome in a young woman secondary to an aneurysm of the internal carotid artery.
Observation
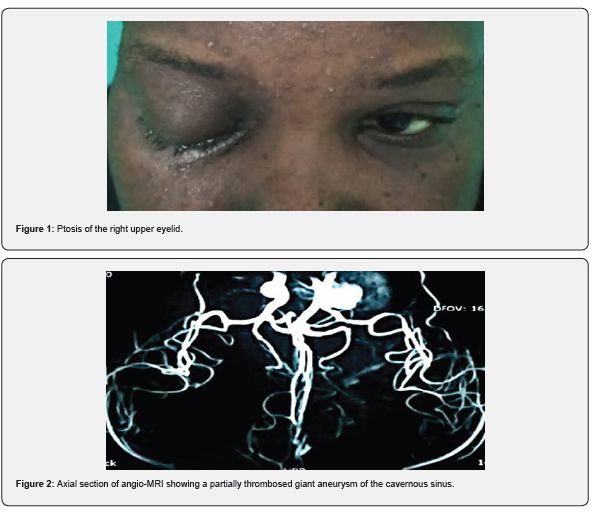
It was a 48-year-old hypertensive patient under known treatment, without reported history of trauma, presenting with a sudden decrease in visual acuity associated with a rapidly progressive drooping of the right upper eyelid over the past month without improvement. Ophthalmological examination revealed a visual acuity limited to 1/10th on the right, severe ptosis (Figure 1), complete ophthalmoplegia, decreased corneal, eyelid, and forehead sensitivity. An areflexic mydriasis was also noted, and fundoscopy showed vascular tortuosity and stage 1 papillary edema. The left eye showed no particularity. Given these symptoms strongly suggesting involvement of the cavernous sinus, an orbito-cerebral angio-MRI was requested and revealed a giant aneurysm of approximately 16.5x10 mm in the right internal carotid artery in its intra cavernous portion with thrombosis, causing compression by mass effect on the vascular and neural elements of the cavernous sinus (Figure 2). After the diagnosis was established, a transfer to Neurosurgery was decided for better management. From an ophthalmological perspective, cosmetic surgery for neurogenic ptosis was considered after neurosurgical treatment. However, while awaiting scheduling for neurosurgery, the patient was lost to follow-up.
Discussion
The cavernous sinus, being an anatomical crossroads, serves as the passage for significant vasculo-nerve bundles destined for the orbital region. Their partial or total compression is responsible for cavernous sinus syndrome. It is a rare condition, representing 5% of all ophthalmoplegias, which is the main symptom in cavernous sinus syndrome [4]. In addition to ophthalmoplegia due to paralysis of the oculomotor nerves (III, IV, and VI), cavernous sinus syndrome involves ptosis, hypoesthesia of the trigeminal nerve territory, and sometimes exophthalmos due to compression of the ophthalmic veins [5]. This clinical description was found in our patient with the onset of symptoms over approximately one month. According to some authors, the onset of symptoms in cavernous sinus syndrome strongly depends on the etiology [1,2]. The etiologies of cavernous sinus syndrome are generally diverse and varied, although dominated by traumas, tumors, and vascular conditions (fistulas, aneurysms). The intra-cavernous internal carotid aneurysm is a rare cause of cavernous sinus syndrome and represents 3 to 5% of intracranial aneurysms [6]. The occurrence of these aneurysms is often correlated in the literature with risk factors such as hypertension, age, smoking, alcohol, tumors, and genetics [1]. In our patient, a history of hypertension over several years was found. Although not reported, craniofacial trauma could be a risk factor since trauma accounts for 75% of carotid-cavernous aneurysms or fistulas, and the onset of cavernous sinus syndrome can occur remotely from the trauma [3]. Presumption of cavernous sinus syndrome is clinical; however, diagnostic confirmation is essentially radiological. Cerebral arteriography, orbito-cerebral angio-MRI, and angio-CT have revolutionized the diagnosis of cavernous sinus syndrome [2,4]. In our patient, angio-MRI allowed for a definite diagnosis by showing an unruptured giant aneurysm of the internal carotid artery in the cavernous portion, compressing the vascular and neural elements of the cavernous sinus. The management of aneurysms depends on their size, location, and integrity (ruptured or not). These aneurysms are less noisy, and the risk of rupture is relatively low [1]. Interventional neuroradiology has revolutionized the treatment of this condition by allowing selective cerebral arterial embolization aiming at closing the aneurysm.
It is a true neuro-ophthalmological emergency because untreated cases can jeopardize life by causing ruptures resulting in cerebral or subarachnoid hemorrhages, sudden epistaxis. Functional prognosis is also at stake with the risk of ocular hypertension, optic atrophy, and decreased visual acuity [3]. The decrease in visual acuity observed in our patient was mainly due to neurogenic ptosis despite stage 1 papillary edema. The challenge in managing these cases in our regions lies in the lack of equipment for rapid treatment of patients given the urgency of the clinical picture, which slightly worsens the prognosis. Our patient was awaiting neurosurgical intervention, and the fact that she was lost to follow-up could be related to the onset of complications or the occurrence of death due to delayed management. From an ophthalmological perspective, ptosis treatment was considered for aesthetic purposes. However, this surgical indication would depend on the condition of the elevator muscle [5].
Conclusion
Cavernous sinus syndrome is a diagnostic and therapeutic emergency. The etiologies are multiple, including carotid aneurysm thrombosis, requiring a multidisciplinary approach. The prognosis is reserved in our regions.
References
- Clermont VC, LAMIRAL C (2020) Neuro-ophtalmologie pratique. Rapport SFO, Elsevier, Paris, pp. 332-334.
- Giles K, Moukouri EN, A, Mballa JCA, Tsimi Mvilongo C, Ebana CM (2013) Syndrome de l’Apex Orbitaire: à propos de Deux Cas au CHU de Yaoundé. Health Sciences and Disease 14(3).
- Boukili K, Loubna E, Bouchra A, Asma E (2021) Exophtalmie unilatérale révélant un grand anévrysme de la carotide interne: à propos d´ un caso. Pan Afr Med J 39(1): 196.
- Toro J, Lisseth Estefania B, Saúl R, Paulo B (2015) Cavernous sinus syndrome: need for early diagnosis. BMJ Case Rep 2015: bcr2014206999.
- Louis M, Goga D, François P (2013) Ptosis révélant un méningiome du sinus caverneux. J Fr Opthamol 36(10): 197-200.
- Bodla Ali A, Ablett M, Andrew I (2007) Bilateral intracavernous carotid artery aneurysms presenting as progressive cranial nerve palsies. Clin Exp Optom 90(3): 207-208.






























