Flying Saucer Appearance: Antimalarial Drug Macular Toxicities
Ahmed Ghazza*, Brahim Madiq, Sarah Belghmaidi, Ibtissam Hajji and Abdeljalil Moutaouakil
Ophthalmology Service Military Hospital Avicenne, Morocco
Submission: January 30, 2020;Published: March 02, 2020
*Corresponding author: Ahmed Ghazza, Ophthalmology Service Military Hospital Avicenne, Marrakech, Morocco
How to cite this article:Ahmed G, Brahim M, Sarah B, Ibtissam H, Abdeljalil M. Flying Saucer Appearance: Antimalarial Drug Macular Toxicities. JOJ Ophthalmol. 2020; 8(2): 555735.DOI: 10.19080/JOJO.2020.08.555735
Keywords:Systemic lupus; Lupus nephropathy; Ophthalmological assessment; Orange yellow; Visual acuity; Retrofoveolar lesion; Flying saucer; Antimalarials
Opinion
We report the case of a 17-year-old woman followed in dermatology for acute systemic lupus with lupus nephropathy on hydroxy chloroquine for 5½ years. In addition, no ophthalmological assessment was carried out when starting treatment or during follow-up. On admission to ophthalmology, visual acuity was estimated at 6/10 P2 of the 2 eyes, with perception of a pericentral scotoma. The bio-microscopic examination was without particularity. The fundus found a round orange yellow retro foveolar lesion, with alteration of the retinal pigment epithelium giving a rosette appearance of the 2 eyes. Multimodal imaging of the 2 eyes including the first-line assessment including a visual field 10 degrees central objectified a tubular visual field with persistence of a central island. The macular OCT found an alteration of the ellipsoid line with a thinning and disappearance of the external retina in para-foveal giving a so-called “flying saucer” appearance (Figure 1). In second intention, a multifocal electroretinogram was carried out and objectified a significant reduction in the amplitude of the waves N1 P1 and N2 in the 2-15 central degrees. The conduct consisted of stopping synthetic antimalarials after consultation with internists and dermatologists.
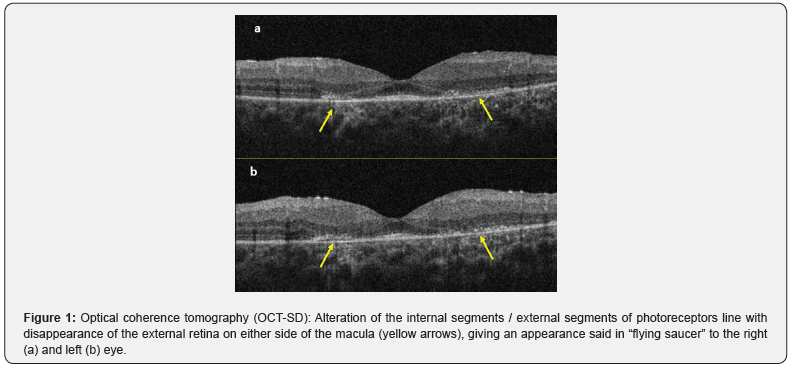
Discussion
Antimalarials drugs (Hydroxy chloroquine and chloroquine) represent a first-line therapeutic option in the context of many systemic diseases in particular systemic lupus erythematosus (LES) with an excellent benefit /risk ratio, however they can be responsible of toxic retinopathy that can lead to blindness [1]. Recommendations for monitoring treatment at antimalarial drugs were the subject of updates in 2011 and 2016 by the American Academy of Ophthalmology (AAO) [2]. Macular OCT is currently considered a first-line assessment with the central visual field [3]. The initial involvement results in an alteration of the internal segments/external segments of the photoreceptors, without interrupting or modifying the thickness of the external retinal layers [4]. At this stage retinal toxicity is reversible. The disease continues with focal thinning of the external retinal layers on either side of the macula, giving a so-called “flying saucer” appearance and then at the late stage, an atrophy of the retinal pigment epithelium [5].
Conclusion
Early diagnosis of antimalarial drugs retinal toxicities involvement is crucial. The risk of retinal toxicity is no longer considered rare but as a function of the dose and the duration of treatment.
References
- Guiot A, Couturier M, Tebib JG, Abouaf L, FCoury (2018) Rétinopathie sévère aux antipaludéens de synthè La revue de médecine interne 39(5): 364-368.
- Marmor, Kellner U, Lai TY, Melles RB, Mieler WF (2016) American Academy of Ophthalmology Statement: Recommendations on screening for chloroquine and hydroxychloroquine retinopathy 123(6): 1386-1394.
- Couturier A, Giocanti-Aurégan A, Dupas B, Girmens JF, Le Mer Y, et al. (2017) Mise à jour des recommandations sur la toxicité rétinienne des antipaludéens de synthè J Fr Ophtalmol 40(9): 793-800.
- Kellner S, Weinitz S, Kellner U (2009) Spectral domain optical coherence tomography detects early stages of chloroquine retinopathy like multifocal electroretinography, fundus autofluorescence and near-infrared autofluorescence. Br J Ophtalmol 93(11): 1444-1447.
- De Sisternes L, Hu J, Rubin DL, Marmor MF (2015) Localization of damage in progressive hydroxychloroquine retinopathy on and off the drug: inner versus outer retina, parafovea versus peripheral fovea. Invest Ophtalmolo Vis Sci 56(5): 3415-3426.






























