- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Ecology of Ebolavirus: A Review of Current Knowledge, Speculations and Future Research Directions
Elijah Ige Ohimain1,2*
1Medical and Public Health Microbiology Research Unit, Niger Delta University, Nigeria
22Microbial Ecology Laboratory, Niger Delta University, Nigeria
Submission: October 02, 2016; Published: December 12, 2016
*Corresponding author: Elijah Ige Ohimain, Niger Delta University, Wilberforce Island, Bayelsa State, Nigeria, Tel:234-803730650; E-mail:eohimain@yahoo.com
How to cite this article: Elijah I O. Ecology of Ebolavirus: A Review of Current Knowledge, Speculations and Future Research Directions. JOJ Immuno Virology. 2016;1(3):555564. DOI: 10.19080/JOJIV.2016.01.555564
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Abstract
Ebola virus disease (EVD), which emerged in West Africa in March 2014, infected about 28,616 people resulting in the death of over 11,000 people. After the discovery of the Ebola virus in 1976, over 20 outbreaks have been reported. The 2014/2015 outbreak, started in Guinea in March 2014, spread to Liberia, Sierra Leone, with few cases in other countries including Nigeria, Senegal and Mali, and isolated cases in Europe and US. Though there have been no approved/licensed drugs or preventive vaccines, some therapies and vaccines, which have entered phase 3 clinical trials, have shown promising results. This virus emerges and re-emerges sporadically. Hence, the aim of this review is to assess the ecology of the virus with the view of understanding the ecological basis for the emergence and re-emergence of the virus. Bats are thought to be the primary/reservoir hosts of the ebolavirus, great apes the possible intermediate hosts, and humans the end hosts. But it also appears that decomposers and scavengers such as insects, rodents and other animals could possibly play a role in the spread and sustenance of ebolavirus in the forest ecosystem. Climate change and human activities such as urbanization, deforestation, agricultural intensification, hunting and consumption of wildlife, which disturb forest ecosystems, may have contributed to the sporadic emergence of the virus.
Keywords: Disturbed habitats; Emerging diseases; Forest ecology; Microbial ecology; Zoonotic infections
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Introduction
TFiloviruses particularly Ebola and Marburg viruses causes deadly hemorrhagic fevers in humans and non-human primates particularly the great apes (chimpanzees and gorillas). Ebola virus disease (EVD), which is also known as Ebola hemorrhagic fever (EHF) is caused by Ebola virus, which has a case fatality rate of up to 90% [1-3]. Ebola virus is among the most dangerous microorganisms today. It has been classified as Category A biothreat pathogen [4-6] and Biosafety Level 4 organism [4,6,7]. Ebola and Marburg virus have been linked to several sporadic outbreaks of hemorrhagic fever especially in East and Central Africa [7-9]. Ebolavirus has been described as pathogen causing emerging and re-emerging zoonotic disease outbreaks in humans [7,10,11]. There are indicators that the frequency, scale and severity of outbreaks are increasing. For nearly 40 years, the science community has been researching on Ebola virus. Recent findings suggest that outbreaks of Ebola virus might not just be sporadic as previously thought, but could be linked to changes in ecology that brought humans in close proximity to natural / primary host and immediate hosts of Ebola virus due to human exploitation of previously unoccupied forest ecosystems.
Ebola virus was first discovered in 1976 with twin simultaneous outbreaks in Nzara, south Sudan and Yambuku, Zaire now Democratic Republic of Congo [12,13], while Marburg virus was discovered in 1967 in Germany and Yogoslavia, where the virus was first isolated from African green Monkeys (Cercopethicus aethiops) imported from Uganda [14]. The 2014/2015 Ebola virus disease outbreak started in Guinea in the Gueckedon region [15-17] from where it spread to neighboring countries i.e. Sierra Leone and Liberia. The suspected index case was a 2 year old boy who possibly became infected on 6 December, 2013 [18,19], and on 22 March 2014, the World Health Organization (WHO) officially declared Ebola outbreak in Guinea. Soon the disease spread to other countries including Liberia (31 March, 2014), Sierra Leone (26 March, 2014), with minor cases in Nigeria (20 July 2014), Senegal (29 March 2014) all in West Africa and few imported cases to other countries including US (30 October, 2014), Spain (6 October, 2014) and Mali (25 October, 2014). While ebolavirus was rapidly curtailed in other countries [2] it persisted for longer periods in the three West African countries where the epidemic started.
At the end of December 2014, over 20, 000 EVD cases have been reported with nearly 50% fatality [20]. A total 27,988 persons have been infected worldwide with the following breakdown in the three main countries; Guinea (3,766 infected, 2524 dead), Liberia (10,672 infected, 4808 dead) and Sierra Leone (13,494 infected, 3,952dead) by August 19, 2015 [21]. As of 29 March 2016, when the Public Health Emergency of International Concern (PHEIC) related to EVD in West Africa was lifted, a total of 28,616 cases were recorded with 11,310 deaths in Guinea, Liberia and Sierra Leone (WHO, 2016). The WHO declared Liberia Ebola virus free on 3 September 2015 and Sierra Leone 8 November 2015 after 42 days of no new cases. To date, 4 out of 5 known species of Ebola virus cause EHF in humans. But Zaire ebolavirus (ZAIV), which is the most virulent, is the cause of EVD outbreak in West Africa [2,22,23]. Thus far, 2014 could be ranked as the worst year of filovirus outbreaks. While ZAIV was ravaging West Africa and northern DRC, Marburg virus was reported in Uganda on 29 September 2014. Feldmann [24] reported that Ebola is becoming a growing threat. Briand et al. [25] reported that the West African EVD has become an international emergency. Martina & Osterhaus [7] describe filovirus as a real pandemic threat.
The threat posed by Ebola and other filovirus is increasing due to several reasons. The current West Africa outbreak has been sustained for over one year despite all the global concerted attention. Out breaks of SUDV and MARV also occurred in African during this same period, but because of their relatively small size compared to the West African outbreak, little attention was paid to them. More worrisome, is the detection of ZAIV IgG among rural communities in some countries in Central Africa e.g. Cameroun that have never witnessed any EVD outbreak [26,27] indicating risk of possible outbreak. Pigott, et al. [26] listed at listed 22 countries in West, East and Central Africa that are potentially at risk of future EVD outbreaks. Repeated filovirus outbreaks have occurred in few countries in Africa particularly Democratic Republic of Congo (DRC), Republic of Congo (RC), Uganda and Gabon. EVD have being linked with wildlife such as non-human primates (NHP), duikers and bats, which are consumed in Africa as sources of protein commonly referred to as ‘bush meat’ [9]. In fact, index cases of EVD are often linked to contact with wildlife. These contacts appear to be increasing due to increase in population, urbanization, hunting and agricultural expansion into previously forested areas. Wittmann, et al. [27] postulated that EVD outbreak will occur episodically in certain ecological condition caused by habitat disturbances or climate change.
Also worrisome is the discovery of bats that are seropositive for ZAIV and MARV in China [28] and Bangladesh [29] and Loviu virus in Spain [30]. Nidom, et al. [31] reported the presence of Ebola antibodies in Indonesian Orangutans, Pongo pygmaeus. All these findings suggest that the risk of Ebola and other filoviruses is bigger than previously thought. EVD is characterized by fever, cold, headache and pains, cough and sore throat, muscle and joint pains, diarrhea, vomiting, general weakness, red eyes, internal and external bleeding [17,32,33]. Despite the severity of the disease and the much attention given to it, there has been no approved therapeutics or preventive vaccines. Hence, the response is limited to supportive care and palliative treatments of some of the symptoms, which involved rehydration therapy and management of blood pressure and organ failures. In response to the growing threat of EVD, global research and development efforts have yielded some experimental drugs (ZMapp, Favipiravir (or Avigan), TKM-Ebola, Brincidofovir) and vaccines (HPIV3, rVSV, cAd3, MVA, RABV, VEEV replicons, rCMV) that are undergoing clinical trials [34,35]. There is the urgent need to focus and understand the ecology of ebolavirus with the aim of quantifying the extent of the challenge and identify a weak link that can be used to control the virus. An excellent review of the ecology of the Marburg virus was recently carried out by Brauburger, et al. [22]. Following the devastating effects of the 2014/2015 EVD outbreak in West Africa, much research attention have focused on the virus. Yet many questions remain unanswered. Hence, an understanding of the ecology of the virus is crucial for prevention and control of future outbreaks. Hence, this paper is aimed at describing the ecology of ebolavirus based on current knowledge. The study also speculated in instances where limited evidences exist, but not unequivocally proven.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Ecology of Ebolavirus
By their very nature, viruses are mostly parasitic. Virus infections could be varied depending on the type of host. It could be benign i.e. asymptomatic in reservoir or primary host, amplified in secondary or intermediate host and fully parasitic in dead-end host. This situation appears to be the case of ebolavirus where recent compelling evidence suggests that bats are the reservoir hosts, while great apes and duikers serve possibly intermediate hosts and humans the end host. Hence, this subsection focused on the ecology of ebolavirus, which could help to predict future outbreak, direct monitoring efforts (location and target organisms) and focus research attention on risky or vulnerable ecosystems.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Ebola and other Filoviruses
The family Filoviridae comprises of 3 genera namely Ebola virus discovered in 1976, Marburg virus discovered in 1967 and Cueva virus that was recently discovered in 2010. Among these, the genus, Ebola virus is the most diversified having 5 distinct species namely Zaire ebolavirus (ZAIV), Sudan ebolavirus (SUDV), Tai Forest ebolavirus (TAFV), Bundibugyo ebolavirus (BDBV) and Reston ebolavirus (BDBV), which is not pathogenic to humans but only to NHP. RESTV was first discovered in Reston (Virginia, USA) from an outbreak of EHF among primates caused by cynomalgus monkeys, Macaca fascicularis, imported from Philippines in 1989 [33,36,37]. Only one species of Marburg virus is commonly reported in literature, but evidence from recent phylogentic assessment suggests that there are 2 species namely Marburg (MARV) and Ravn Marburg (RAVV) [22,38]. Apart from RESTV and LLOV, all the other filoviruses originated from Africa. Outbreaks of Ebola and Marburg virus occurred mostly in DRC, South Sudan and Uganda. In 1976, when Ebola virus was first discovered, different species of the virus caused simultaneous outbreaks, SUDV in South Sudan and ZAIV in DRC. But the simultaneous 2014 outbreaks in West Africa and DRC were caused by ZAIV. So far, there have been at least 24 EVD outbreaks in Africa, 15 caused by ZAIV, 6 by SUDV, 2 by BDBV and 1 by TAFV. The 2014 EVD outbreak in DRC is the seventh one. The frequency of EVD outbreaks is highest in DRC, South Sudan, RC, Uganda and Gabon.
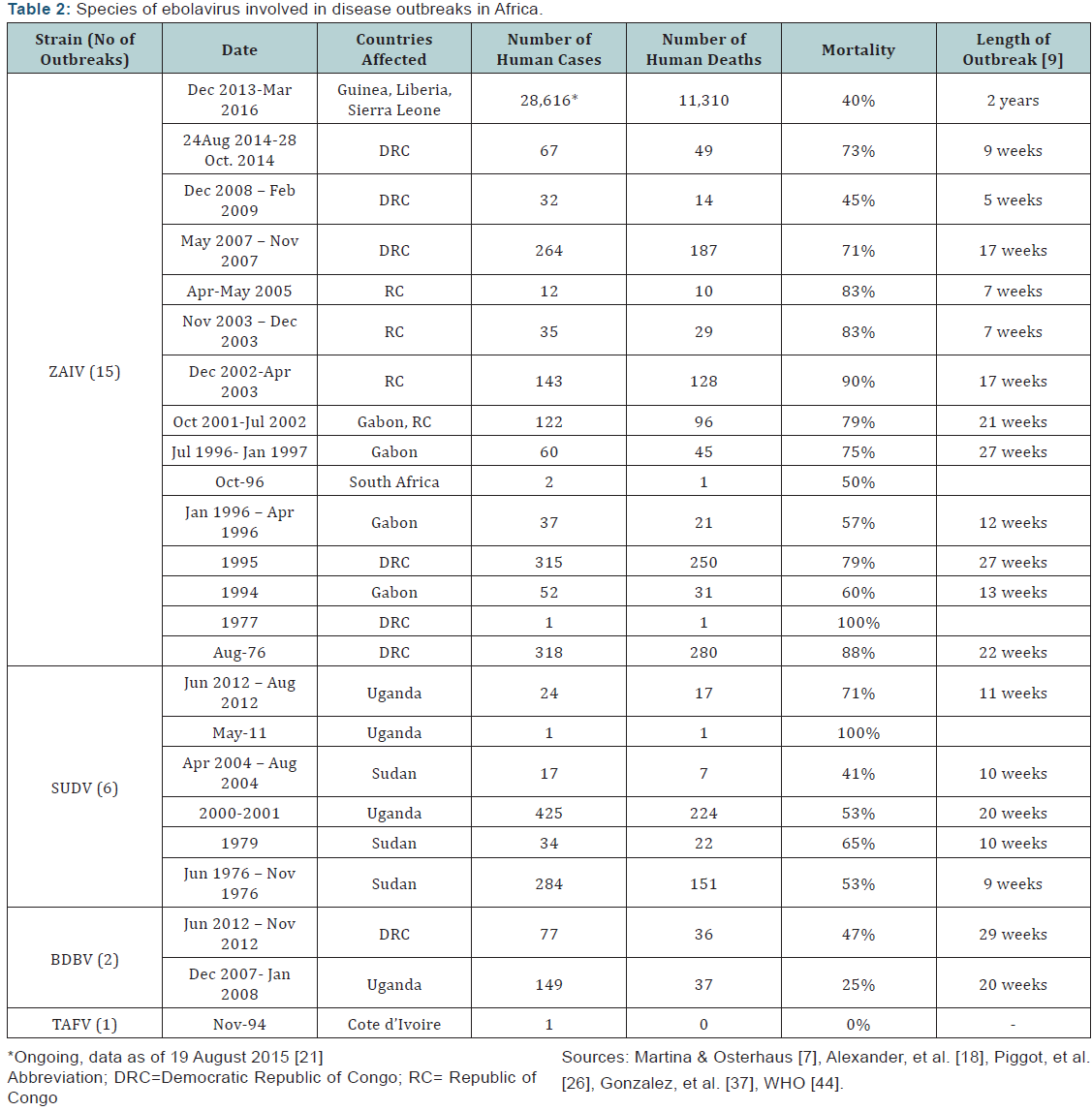
In terms of scale, severity and human casualty, the 2014 EVD outbreak is by far the largest and is bigger than all the other outbreaks combined. Though, the outbreak started in Guinea, and spread to neighboring Sierra Leone and Liberia but with minor incidents in Nigeria, Senegal and Mali and few imported case into Spain and USA. Historically, fatality from ZAIV is 45- 100% but was generally described as 90%, but the West Africa outbreak recorded 40% perhaps due to more global concerted efforts. While all the previous EVD outbreaks occurred within relatively short periods ranging from few weeks to months, the 2014/2015 EVD outbreak have been sustained for about two years despite all the global attention. The 2014/2015 EVD was the first outbreak in West Africa and the largest thus far. Carroll, et al. [39] reported that filovirus shared a most recent common ancestor approximately 10,000 years ago, but the most recent common ancestry can be traced back within the last 50 years for ZAIV and RESTV, 700 years ago for MARV and 850 years for SUDV. Other evidences suggest that filoviruses originated at least 12 million years ago. Molecular evolutionary rates in terms of nucleotide substitution rate were 0.46x10-4 substitution/site/yr for SUDV, 7.06x10-4 substitution/site/yr for ZAIV and 8.27x10-4 substitution/site/yr for BDBV [40-44]. Recent studies also show that the West African outbreak of ZAIV that spread to Mali had a nucleotide substitution rates of 1.3x10-3 substitution/site/yr, which is consistent with rates observed in Central African out breaks (Table 1). Using molecular biology tools, Gire et al. [45] traced the origin and pattern of transmission of the 2014/2015 EVD outbreaks in West Africa. These researchers found that the West African variant of ZAIV diverged from Central African lineage around 2004 and crossed from Guinea to Sierra Leone in May 2014. This observation is in agreement with the findings of Walsh et al. [46] claiming that ZAIV has recently spread across rather than being persistent at each outbreak locality. Hoenen et al. [47] also reported that the nucleotide substitution rate of the 2014/2015 West African Ebola virus to be 1.3×10-3 substitutions per site per year, which is consistent with rates observed in Central African outbreaks (Table 2).
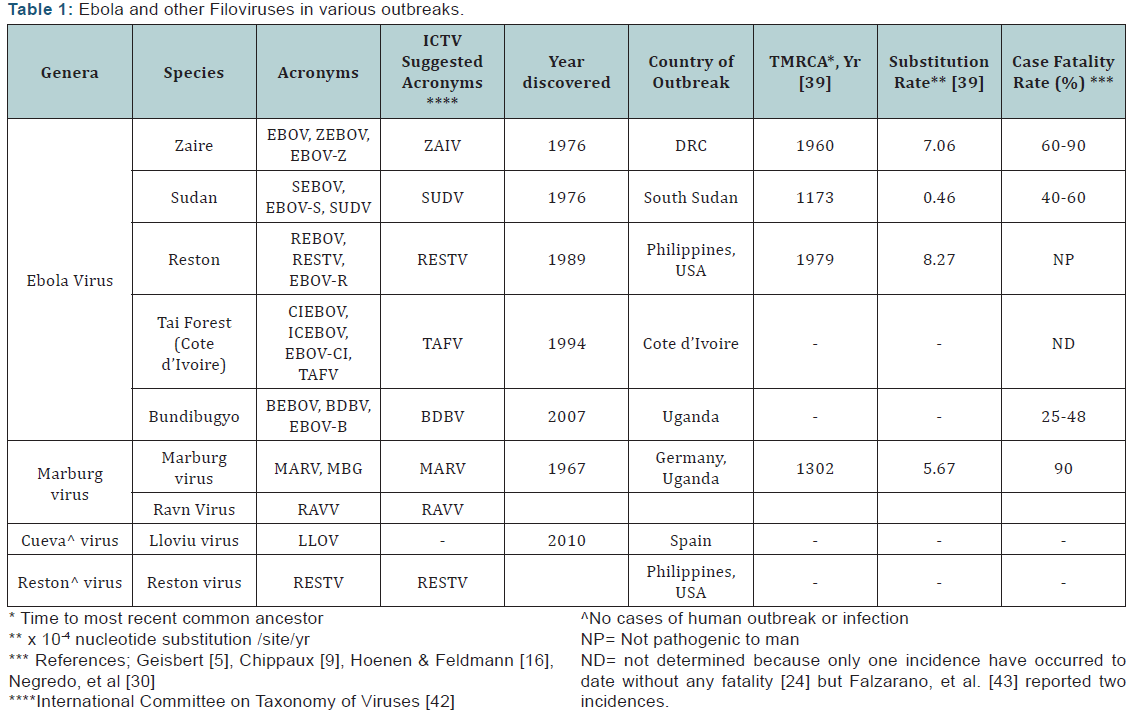
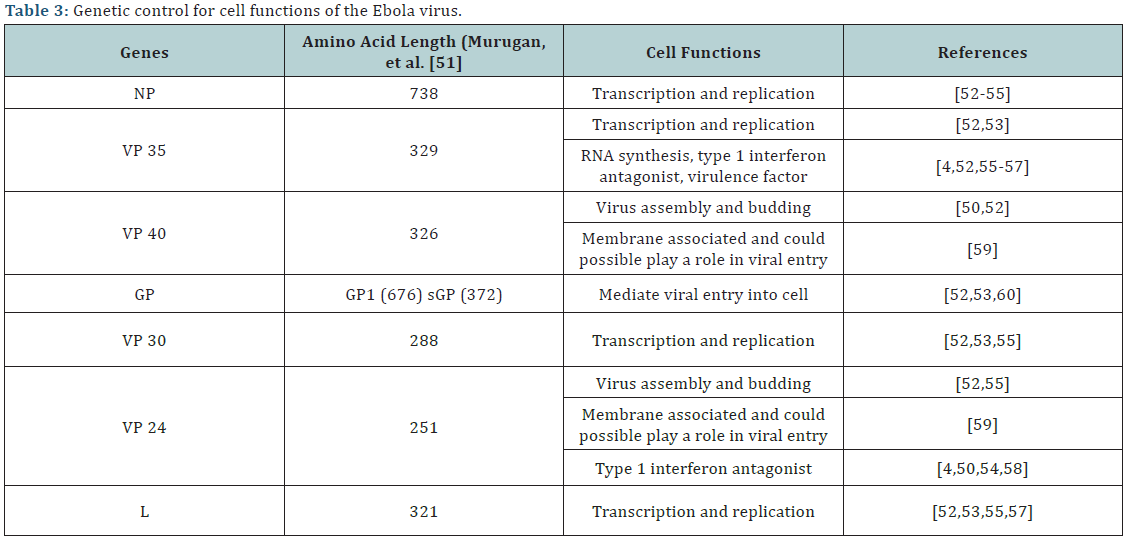
Ebolavirus and related Marburg virus have negative-sense RNA genome. The genome of Ebola virus is about 19 kb long consisting of 7 genes encoding for proteins including nucleoprotein (NP), virion matrix protein (VP35), VP 40, glycoprotein (GP), VP 30, VP 24 and the RNA dependent RNA polymerase (L). Rao et al. [48] reported that GP, NP, VP24 and VP40 are structural proteins while VP30, VP35 and L are non-structural proteins. The amino acid length and functions of each of these proteins are presented in (Table 3). Of particular importance is the GP which mediate entry into susceptible hosts, NP, V35, VP30 and L are involved in viral transcription and replication, while VP24 and VP 40 are involved in virus assembly and budding. VP35 and VP 24 are type 1 interferon antagonist. The inhibition of type 1 interferon during ebolavirus infection is strongly associated with increased virulence [49-53]. Several authors [4,54-56] reported that the ability of filovirus to interfere with the host innate immune system especially the interferons is attributed to VP 24 and VP 35. Using Cosic’s resonance recognition models for protein sequences and photo-emission of ebolavirus genes, Murugan, et al. [57-59] was able to differentiate lethal (ZAIV and SUDV) from relatively non-lethal (BDBV and TAFV) species of ebolavirus.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Bats (Suspected Reservoir of Ebolavirus)

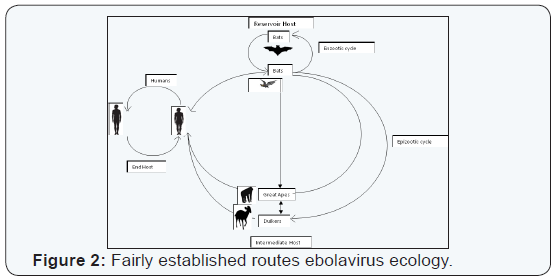
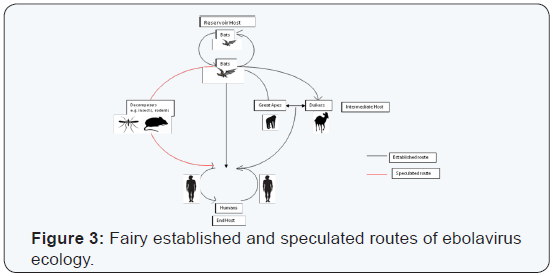
It has long been suspected that bats act as reservoir to many zoonotic diseases including viruses [60,61]. Monath [62] speculated that bats are the primary host/natural reservoirs of Ebola virus. For about 40 years that ebolavirus ravaged central Africa, the nature of this reservoir has been elusive. And because of the sporadic nature of the outbreak, it has long been suspected that the reservoir host will be an organism that has rare or infrequent contacts with humans [37,62]. Because most human outbreaks of EVD is often preceded by large scale fatalities of great apes and duikers [9,45,63,64] many researchers has speculated that apes and duiker may be the primary reservoir. But reservoirs will not succumb to infection; hence great apes and duikers are probably secondary or intermediate host of ebolavirus (Figures 1-3). While working in Gabon and RC, Leroy et al. [65] first reported evidence of asymptomatic infection by ebolavirus in three species of fruit bats (Hypsignathus monostrous, Epomops franqueti and Myonycters torquata) suggesting that bats are the reservoir of ebolavirus. As usual with reservoir hosts, there viruses cause little or no pathology in bats [66]. Moratell and Calisher [67] postulated that bat genes associated with early immune responses might permit virus replication without primary immune response which in turn allows low level viral replication over extended periods, while the host bat remained asymptomatic. Some bats roost on the edges of the forest. So that forest encroachment by humans might well be linked to increasing Ebola outbreaks. Pourrut, et al. [63] detected ZAIV IgG in the tissues of these three fruits bats, while in Gabon and RC, Leroy, et al. [68] demonstrated the role of fruit bats in the 2007 EVD outbreak in Luebo, DRC. Biek, et al. [69] reported recent common ancestry of ZAIV found in bats. Hence many authors have reported these three bats as the reservoir of Ebola virus [5,9,15,70,71]. Ebola appears to circulate within and between bat population through fighting and sexual contacts [63] & Saez, et al. [72] investigated the origin of the 2014 EVD outbreak in West Africa and found evidence implicating an insectivorous free-tailed bat (Mops condylurus) as the possible reservoir. Hayman, et al. [73] found ZAIV antibodies in the tissue of the migratory straw-coloured fruit bat (Eidolon helvum) in Ghana. The Egyptian fruit bat (Rousettus aegyptiacus) was linked to ZAIV infections in Garbon and RC [74] and Marburg virus infections in Uganada [75] & Garbon [14,76]. Ebola virus antibodies were also found among another species of Rousettus spp. bats R. lanosus in Kenya, Uganda and Zimbabwe [62] and R. leschenaultii in Bangladesh [29] and China [28]. Generally, bats are found in all continents except Antarctica [71]. Peterson, et al. [77] listed about 72 species of bat consisting potential reservoir for filoviruses.
In a large serological survey, Pourrut, et al. [73] found ZAIV specific IgG antibodies in bat species (Hypsignathus monstrosus, Epomops franqueti and Myonycters torquata, Micropteropus pusillus, Mops condylurus and Rousettus aegyptiacus) and MARV antibodies in 2 bats (H. monstrosus and R. aegyptiacus). In DRC, Swanepoel, et al. [78] reported the presence of MARV in 2 insectivorous bats (Rhinolophus eloquens and Miniopterus inflatus) and R. aegyptiacus. Lloviu virus was detected in Schreiber’s bat (Miniopterus schrebersii) in Spain [30]. Hayman, et al. [79-83] detected ZAIV and BDBV antigens in serum of bats from Ghana including Epomophorus franqueti, E. gambianus, Hypsynathus monstrosus, Nanonycteris veldkampii and Epomops buettikoferi. Although 3-6 species of bats have been mostly reported as possible reservoir of Ebola and Marburg viruses, more recently, many bat species have been reported to be the likely primary reservoir host of filoviruses (Table 4).
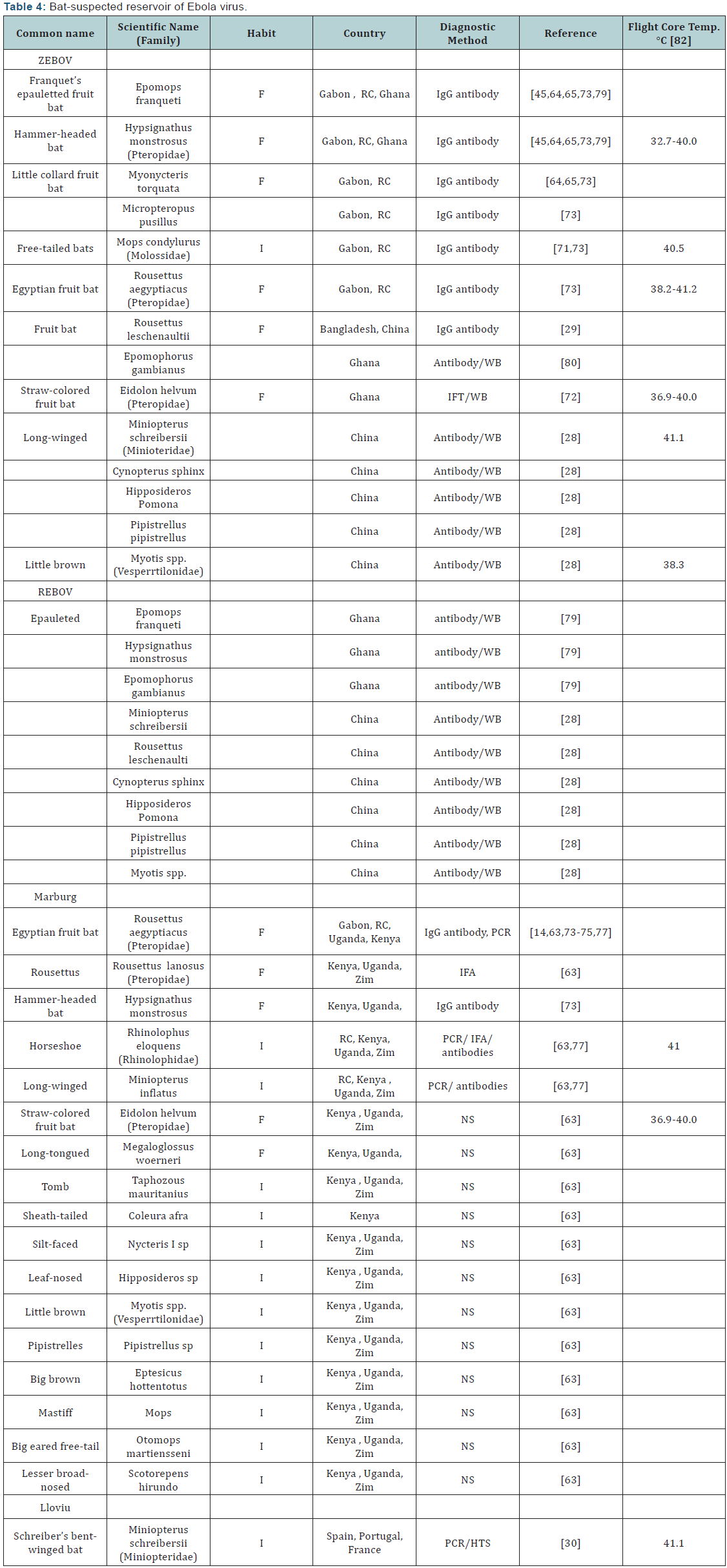
IFT= Indirect fluorescent test; WB= western blot; PCR = polymerase chain reaction; HTS = high-throughput sequencing; IgG = immunoglobulin G;RC= Republic of Congo; DRC= Democratic Republic of Congo; Zim =Zimbabwe; I = insectivorous; F = frugivorous; NS= not stated There are no currently known bat hosts for Bundibugyo, Sudan, or Tai Forest Ebolaviruses [83].
Many questions immediately come to mind. How are bats able to act as the reservoir of this disease? What other compelling evidence exists beyond the presence of Ebola antigen or antibodies in the bat? If bats are the reservoir, how does this host transmit the virus to human? Swanepoel, et al. [84] experimentally inoculated 24 species of plants and 19 species of animals with Ebola virus and found 3 species of bat (Tadarida condylura, T. pumila and Epomophorus wahlbergi) became infected, the viruses replicated without development of diseases symptoms. Bat exhibit several characteristics that made it able to serve as reservoir host of Ebola virus. The role of bats in the spread and maintenance of various viral diseases is well established [61,71,85]. Bats are natural reservoirs of emerging and reemerging zoonotic viruses such as Rhabdovirues, Coronaviruses, Paramyxoviruses, Lyssaviruses, Reoviruses, Flaviviruses, Adenoviruses etc [61,85-92]. About 75% of emerging infectious diseases are zoonosis [89] many of which are caused by bats. Bats, which belong to the order Chiroptera are among the most abundant and widely distributed non-human mammalian species in the World [93].
Bats accounted for about 20% of all mammals [71,86,93]. Bats can be divided into two suborders, the Megachiroptera (Megabat) and Microchiroptera (Microbat). The megabat comprise of 1 family Pteropodioptera, which are mostly fruit bats comprising of 42 genera belonging to 166 species, while the microbat, which are mostly insectivorous contain 16 families belonging to 135 genera and 759 species [71,86]. Morratelli & Calisher [67] reported that over 100 viruses have been detected in bats. The feeding pattern of bats is very diverse though, frugivorous and insectivorous bats are commonly cited, but there are 7 feeding habit group of bats; fruit eaters, flower feeders, insect eaters (aerial and ground foliage gleaners), carnivorous (feeding on birds, frog, and small mammals), fish eaters, blood feeders and omnivorous [67]. African straw coloured fruit bat Eidolon helvum is a reservoir to multiple viruses apart from Ebola and Marburg viruses such as several species of Paramyxoviruses [94] and Lyssaviruses particularly Lagos bat virus [73]. Similarly, Rousettus aegyptiacus is a reservoir to many viruses including Ebola, Marburg and Lyssavirus [29,71,73,92-94]. Circumstantial evidence suggests that most human and domestic pathogens of at least 4 viral families originated from bats; coronaviridae, filoviridae, paramyxoviridae and lyssaviridae [95]. Moratolli and Calisher [67] reported that over 200 viruses, some of them deadly zoonotic viruses have either been detected in bats.
Bats have morphological and physiological adaptation for powered blight, which could also be linked to the spread of zoonotic diseases. For instance, the 2014/2015 EVD outbreak in West Africa, which is caused by ZAIV was traced to a 2 year old boy (index case) who got probably infected while playing in a hollow tree housing a colony of insectivorus bats (Mops condylurus) [72]. Bats are known to be able to travel long distances, which explained how ZAIV could have been brought into West Africa from Central Africa. Fruit bats are highly migratory. Studies have variously shown that they can migrate over 2000 km [73,79,80,96]. During flight, bats are known to maintain relatively high temperatures (fevers) 38 - 41ºC [82] that help to suppress/ or control the replication of filoviruses. Such adaptations help to maintain and sustain the virus in the reservoir host. Details on the mechanisms of flight, fever, body temperature and the control of viruses by bats can be found in O’Shea, et al. [82] and Ng, et al. [97]. Using telemetry, Richter and Cumming [98-103] showed the Eidolon helvum is capable of migrating several thousand km in 5 months.
The long life span of bats is another factor that made it a suitable reservoir for viruses. Bats are reported to have life of at least 3.5 times greater than non-flying mammals of similar size [104-105]. Several authors have reported high longevity in bats. Martino, et al. [106] reported a life span of 38 years for Myotis brandti. Munshi-South & Wilkinson [104] reported 41 years for Myotis brandti while Wilkinson & South [105] listed 5 bat species that lived above 30 years including Plecotus auritus (long eared bat), Myotis lucifugus (little brown bat), Myotis brandti (Brandt’s bat), Rhinolophus ferrumequinum (horseshoe bat), and Pteropus giganteus (giant flying fox). Some of these bat genera have been reported to possibly harbor Ebola and Marburg viruses, e.g., Myotis and Rhinolophus. Wilkinson & South [105], Martino AMG, et al. [106] attributed the long life span of bats to be due to hibernation. Because of its longevity, bat appears to heighten the risk of Ebola and Marburg viruses infection using radio transmitters, Hayman, et al. [73] demonstrated the long term survival of Eidolon helvum seropositive for Ebola and Lagos bat viruses. Radio transmitter signals were transmitted for only 13 months after the release of these bats. The tagged bats might have migrated out of signal reach or the battery expired.
Bats occurs in large population [73,96]. Hayman, et al. [79] Studied colony of up to one million bats that roosts in trees in Accra, Ghana. Luis et al. [90] reported a colony of Mexican free-tailed bat (Tadarida brasiliensis) reaching a density of 3000 bats/m2 with a population of up to a million. Hayman et al. [73] reported that R. aegyptiacus typically live in very large roosts within population of over 100,000, which could facilitate persistence of infections within hosts. In Uganda, over 40,000 R. aegyptiacus was found in a cave linked to the 2007-2008 Marburg virus outbreaks.
In terms of demography and migration pattern, one of the bats that was first and most studied in Africa, is the straw coloured-fruit bat Eidolon helvum. Using stable isotopes, Ossa et al. [96] found that 22% of Eidolon helvum are migratory over 250 - 860 km with a few over 2000 km. It has been estimated that Ebola virus spread at a constant rate of 50km/year [7,46]. Using solar powered satellite telemetry, Richter and Cumming [98] estimated that Eidolon helvum can travel 29 - 90 km/day and a single bat can cover 370 km in one night. The greatest distance travelled by a single bat was estimated at 2518 km in 149 days. During migration, high intra and inter specific contacts rates increases, which can facilitates rapid transmission of pathogens [90].
Eidolon helvum are widely distributed in Africa [96,73,79]. The tropical rain forests are thought to be the primary habitats of Eidolon helvum [80] but they migrate seasonally and spatial coinciding with the availability of fruits [98]. The authors demonstrated that migration of Eidolon helvum is linked to spatial variation in rainfall, which in turn results in fruit production. Each year, from October to December an estimated 5-10 million Eidolon helvum often congregate at the Kasanka National Park Zambia [98]. Such large congregation of bats could facilitate the transmission of zoonotic diseases. Bats could also migrate during reproduction as observed in Eidolon helvum [98] and R. aegyptiacus [75]. Amman, et al. [75] using RT-PCR technique, reported season pulses of MARV circulation in juvenile of R. aegyptiacus, which coincided with periods of increased risk of human infection. Hayman et al. [79] reported that E. helvum is a seasonal breeder with copulation occurring from April to June followed by parturition from February to May the following year. Large-scale movements could cause extensive genetic mixing among wildlife populations that could cause virus diseases outbreaks [90]. Simons, et al. [23] reviewed the potential for introduction of bat-borne zoonotic viruses into Europe, which could also happen in other continents. Bats borne zoonotic diseases are becoming a global threat [66,91].
Many bat species are gregarious [90] and living/roosting in diverse places such as caves [14,75], tree tops [73,96] and have peridomestic habits, roosting in buildings and trees in urban areas [73,86,90]. Bats exploit a variety of roosts including hollows (tree trunks, caves, mines, building, tunnels), crevices and foliage [67]. For instance, E. helvum have been frequently sighted in urban areas in Africa including Lagos, Kampala, Abidjan, Accra and Dar es Salaam [91]. In Africa, bats roosts in broad range of ecosystems from tropical rainforest in the Guinea savannah to Sahel and Sudan savannah. Changes in land use and penetration into previously remote areas of rainforest bring humans in contact with bats [26]. Bats are also known to be adaptable to disturbed ecosystems [67].
Bats appears to have evolved about 50 million years ago [67,86]. Filoviruses are thought to have coevolved with bats [76], may use highly conserved cellular receptors, that enhances their ability to transmit viruses to other mammals [90]. According to Luis, et al. [90], bat have evolved traits that suited for hosting viruses, such as long life span, prolonged torpor and hibernation and powered flights. According to Moratelli & Calisher [67], the evolution of flight, which permits wide bat distribution, could be linked to some aspects of the evolution of the immune systems and metabolism of bats, which allowed them to host a variety of viruses. Bats produce antibodies against many viruses including IgG, IgM, IgE, and IgA [67]. Details of the immune system of bats can be found in Bakers, et al. [94], Moratelli & Calisher [67], Schountz [66], Calisher, et al. [70]. Most of these studies are based on serological evidences, which could be problematic sometimes due to cross-reactivity of false-positive results.
Bats, particularly the fruit bats (flying foxes) perform vital ecosystem functions particularly pollination and /or dispersal of seeds. Ossa, et al. [96] reported that the ecosystem functions of bat result in maintaining genetic connectivity of plants among fragmented landscapes and sustenance of about 450 economically important plant products. The survival of Iroko timber, Milicia excelsia is attributed to the migratory movements of E. helvum. Bats are critical to the sustainability of terrestrial ecosystems because they help to pollinate plants, control insects and reseed cut forests [71]. While performing ecosystem functions, bring bats into contact with plants, animals and humans, which often lead to the transmission of diseases, either directly or indirectly. Bats have relatively short digestive tracts [61] hence they defecate partially consumed fruits, which are often eaten by other animals particularly NHP, duiker leading to disease transmission. qRT-PCR studies have found virus in the lung, colon, kidney, reproductive organs and feces, which is consistent with oral, fecal, respiratory and sexual transmission routes to susceptible hosts [18,75]. It has been reported that when pathogens spills over from reservoir to intermediate or end host, they could become more virulent [107].
In Africa, wildlife is often consumed as source of protein commonly referred to as bush meat. Hence, bat (primary reservoir) and many secondary/intermediate hosts of Ebola virus such as NHP and duiker are often consumed by Africans, which have led to transmission of zoonotic diseases including EVD. The following subsection shall therefore discuss in more detail the role of humans and other animals in the ecology of Ebola virus.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Intermediate/ Secondary Host of Ebola Virus
Viruses are known to be relatively stable and well adapted to their reservoir host’s cellular, immunologic and ecological environments with little or no clinical disease manifestation [89]. But when the viral spills over to other host it could become pathogenic and disastrous [107]. Several factors have increased the contacts between bats and mammals such as feeding, climatic change and destruction of forest for farm and urban development and hunting. Chippaux [9] reported that bats by sharing their narrow ecological niche bringing them in contact with many mammals particularly the great apes, which facilitate the transmission of Ebola viruses.
Ecological survey shows that Ebola virus spill over to animal’s particularly great apes (Chimpanzee and Gorilla) and duiker (a type of antelope). Ebola antibodies have been found in many primates, but have been most commonly reported in great apes. (Table 5) presents the list of mammals in Africa that Ebola virus antibodies have been detected including chimpanzee, gorilla, baboons, drill, mandrill and monkeys. Ebola virus antibodies have also been found in dogs and pigs. Most of these studies were carried out in Central Africa particularly Gabon, RC and Cameroun. But Ebola virus antibodies have also been found in orangutans in Indonesia [31]. Swanepoel et al. [84] experimentally inoculated 24 species of plants and 19 species of animals with Ebola virus and found out that the virus could replicate in 3 species of bats, brown house snake (Lamprophis fuliginosus) and social spider (Stegodyphus dumicola). The presence of Ebola viruses in other animals in the food chain could increase the risk and sustenance of Ebola virus in the ecosystem.
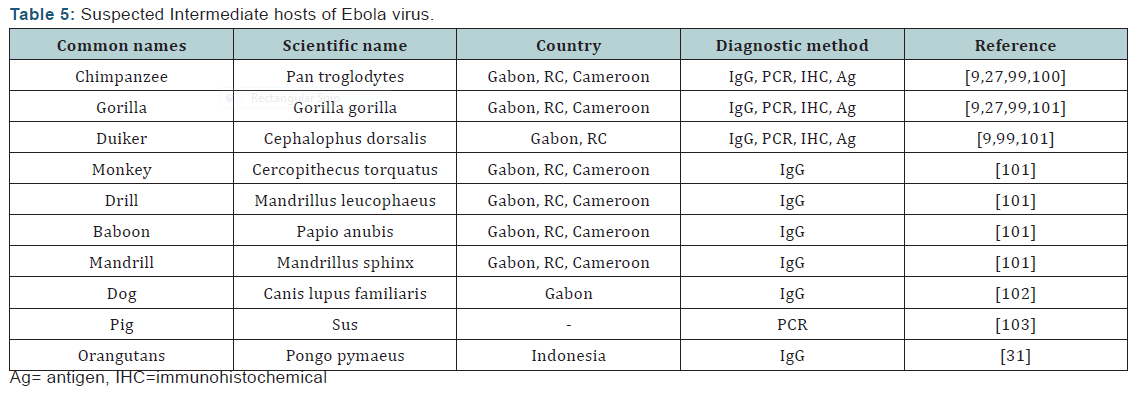
Between 1979 and 1980, a total of 1664 animals samples representing 117 species including >400 bats and 500 rodents were collected in DRC and Cameroun. All tested negative for Ebola virus [108]. A total of 3066 blood samples were collected from animals including dogs, cattle and pet primates from 10 June - 28 August 1995 from Kikwit (an area exposed to EVD) in DRC, similarly yielded negative results [109-110]. Studies carried out by Monath [62] also failed to establish the role of arthropods and plants in ebolavirus transmission but implicated bats and other wildlife primates. Pourrut, et al. [63] reviewed several studies that have been carried out to identify ebolavirus vectors. Over 7000 vertebrates and 30,000 invertebrates were sampled and the results show that mice (Mus setulosus and Praomys sp.) and shrew (Sylvisorex ollula) in CAR were positive for Ebola virus. These findings tend to agree with the view of Walsh, et al. [46] that ebolavirus has recently spread across the region rather than being persistent at each outbreak locality.
Ebolavirus infections have been very fatal on great apes, leading to the decline [46,100]. Grad, et al. [111] reported massive deaths of apes during different outbreaks of EVD and presented a trend showing >75% decline in Gabon (1983- 2000), >80% decline in NE Gabon (1994-1988) and >80% decline in Lossi (RC) from 2001-2004. During the 2001-2003 EVD outbreak in Gabon and RC, 98 wild animal carcasses were recovered including 65 great apes [12], Genton et al. [112] have attributed the death of 93% gorilla in Central Africa declining the population of 350 gorilla to <40 in RC. Leroy et al. [101] reported more than 50% decline in the great apes population of Gabon from 1983 - 2000. The authors estimate the reduction rates of gorillas, chimpanzees and duikers to be 56%, 89% and 53% respectively from 2000 - 2003. Ebola outbreak was reported to result in the death of about 5000 gorilla at the Lossi Sanctuary (Gabon) from 1995 - 2003 [113]. Carcasses of wildlife particularly gorilla, chimpanzees and to a lesser extent duikers are often associated with EVD outbreaks. Carcasses decompose very quickly under tropical conditions. For instance, Rouquet et al. [12] reported that it takes about 10 days to completely decompose the flesh of an adult male gorilla weighing 150 kg. The authors further described the fate of the carcasses within 3 - 4 days after death. Common house fly, Musa domestica colonizes the carcass laying eggs and maggots, which completely consume the flesh within 5 - 10 days, while scavengers such as mongoose take pieces of bones and disseminate them within the forest ecosystem.
The detrital ecology of the carcasses could contribute to the spread and sustenance of ebolavirus in the forest ecosystem. For instance, house fly are known vectors of many diseases including bacteria, protozoa and viruses [114]. Barreiro et al. [115] reported that due to their indiscriminate movement, ability to fly long distances and attraction to dead decaying matter, housefly greatly amplify the risk of human exposure to diseases. It is unclear whether arthropods are able to transmit Ebola virus because several studies carried out in the 1990 failed to detect Ebola among arthropods [62,109,110] & But Reiter et al. [109] cited a case of where MARV replicated in mosquito (Aedes aegypti). Mosquitoes are capable of transmitting flavivirus particularly dengue and yellow fever viruses [116] & Schurrer, et al. [117] reported an instance where flies acquired virus from pigs and spread the virus over a distance of 1.7 km. Other questions emerge such as: Can housefly transmit Ebola virus? Could insectivorous bats and other insect feeding animals exposed to Ebola virus via this route? Could mongoose contact Ebola virus by scavenging dead animals? Wong, et al. [118] reported transmission of Ebola virus from swine to NHP via respiratory route. The transmission of ebolavirus via respiratory route in humans is unlikely and has not been demonstrated. But there is the possibility of sexual transmission. Katzourakis & Gifford [119] detected endogenous viral elements of filoviruses in mammals particularly rodents, marsupials and bats. The presence of filovirus genetic elements in bats, rodents, and marsupials suggest that these mammals could be among the possible carriers of ebolavirus. Rouquet, et al. [12] reported an instance where a Swiss anthropologist became infected with Ebola virus while examining dead chimpanzees in Tai Forest without wearing any personal protective equipment (PPE). Could other animals such as duikers, rodents and arthropods become infected likewise? There is therefore the urgent need to carry out fresh ecological studies in Africa to ascertain the role of scavengers and arthropods in ebolavirus dynamics. Leroy, et al. [101] presented data showing temporal and spatial overlap between increased mortalities of wild large mammals and human outbreaks of Ebola virus. Rouquet, et al. [12] reported that epidemiological surveillance of animal mortality rates can be used to predict and prevent the emergence of the disease in humans. Citing the EVD outbreaks in Gabon (2011) and RC (2002 - 2003), the authors confirm that mortality of wild animals can reveal Ebola virus propagation in the forest ecosystem. Citing these incidences, Leroy, et al. [101] also observed that wildlife mortality often preceded and linked to human infections. Rouquet, et al. [12] had twice used fatality of wildlife as indicators of possible human outbreaks to alert the governments of Gabon and DRC.
Using molecular biology tools, Carroll, et al. [39] found that viruses similar to those found during the Luebo (DRC) outbreak may have been circulating in the forest ecosystem since 2005 i.e. 2 years before the outbreak was first recognized. But in 2007, the villagers at Luebo did not observe any unusual wildlife mortality, but massive annual fruit bat migration preceded Ebola outbreak [45]. In a study carried out by Grad, et al. [111] presented two viewpoints that the Luebo 2007 EVD outbreak (1) did not result in viral spread from previously identical loci but from an independent viral emergence, and (2) that migrating bats viral spill over into local wildlife population, which allowed local viral persistence and re-emergence from year to year.
The feeding habits of intermediate host can help to explain the spread and persistence of Ebola virus in the forest. Monkeys are strict vegetarians, but they could become exposed to Ebola virus through the consumption of fruits contaminated by bats. Chimpanzees and gorillas are omnivorous. In addition to eating fruits, they are known to hunt and eat bats, monkeys, duikers, and other mammals. Duikers have been observed to eat flesh of decomposing carcasses [12]. Most of the intermediate hosts often get infected through the consumption of fruit rejects, partially digested fruits/seeds, fibrous feces of bats. Bats swallow and pass out seeds relatively intact. Because of their short GIT, bats pass out consumed food rapidly in about 20 minutes [67]. For instance, Chivers and Hladik [120] reported that the smallest mammalian gut known is found in the insectivorous bat, Rhinopoma, with a tract of about four-fifths of its body length.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Dead End Host (Humans)
The mechanisms of how Ebola virus spill over to humans have been a topic of research and speculations. But recent scientific evidence has revealed the mechanisms. Human exposure to Ebola virus has been linked to animal vectors particularly bats, duikers, chimpanzees, gorillas and monkeys [12,69,99,101,121]. Humans could be exposed to Ebola virus by hunting, butchering and consumption of bush meat particularly bats, duikers and NHP especially monkeys, chimpanzees and gorillas. For instance, the index case of the 2014 EVD outbreak in West Africa was probably infected through contacts with a colony of insectivorous fruit bat, Mops condylurus [71]. Similarly, the 2007 and 2008 EVD outbreaks in Luebo (DRC) were possibly linked to bats. Leroy, et al. [68] reported events leading to the transmission of Ebola virus from bats to humans in the 2007 Luebo (DRC) EVD outbreak. The index case was involved in the hunting and consumption of fruit bat H. monstrous. Each year, many villagers in Africa often hunt and consume migratory bats as sources of protein. Bat hunting and consumption have been well documented. A large colony of about 25,000 - 1 million of E. helvum was documented in Accra, Ghana. It is estimated that about 128,000 E. helvum bats are sold each year in Ghana [79,122,123]. The IUCN has classified E. helvum as near threatened due to massive hunting.


Apart from bats, other wildlife are also hunted, sold and consumed in African (Figures 4 and 5) including great apes, monkeys, duikers, grass cutter, porcupine, bush pig, bush dog, potto & squirrels [124,125]. It has been estimated that nearly 1 million kg of bush meat is sold annually in the Cross-Sangana River region alone [126,127]. Bush meat contributes about 20 - 90% of the protein consumption in many parts of Africa. The bush meat sector in Ghana employs 300,000 persons, while local consumption and export of bush meat generates over $ 300 million annually [128]. This idea could be the trend in other African countries if studies are carried out. The zoological society of London (ZSL) has a bush meat research programme Swensson [129] listed the IUCN conservation status of some of the common bush meat in Africa including vulnerable (pied bat, black and white colobus, gazelle), near threatened (olive colobus, duiker) and endangered (red colobus, chimpanzee). In a serological survey of Ebola infection in NHP in central Africa (RC, Gabon and Cameroun), Leroy et al. [101] reported the seroprevalence of Ebola antibody in wild-born chimpanzee to be 12.9% and concluded the following:
- That Ebola virus circulates in the forest of a large region of Central Africa including countries like Cameroun with no previous outbreak of EVD
- Ebola virus was present in the forest prior to human outbreaks
- Chimpanzees are continually in contact with the virus and
- Non-lethal Ebola virus can also occur in chimpanzees. High seroprevalence of Ebola virus have also been reported in non-epidemic area like CAR. The prevalence was highest among hunters who handled bush meat than non-hunters [13].
A high prevalence of Ebola virus antibodies (12.4%) was found among 5070 persons randomly sampled in 6 Central African countries (Cameroun, CAR, Chad, RC, Equatorial Guinea and Gabon) between 1983-1987 [130]. But in CAR alone, Ebola virus Seroprevalence ranged 5.3%-21.3% [131-132]. Nkoghe, et al. [13] reported the prevalence of ZAIV specific IgG among rural Gabonese populations to be 15.3% (average), which increased to 32.4% in areas close to the forest and concluded that ZAIV, which is endemic in Gabon is linked to the forest ecosystem and that human positivity could be linked to exposure to contaminated fruits. On the other hand, Hefferman, et al. [133] reported low Seroprevalence of ebolavirus IgG, in an endemic zone in Northeastern Gabon, indicating low risk of EVD. Pernet, et al. [134] reported evidence of Henipavirus spillover from bats (E. helvum) into humans in Cameroun. Seropositive human samples were found also exclusively among individuals who reported butchering bats for meat and living in areas undergoing deforestation. Rasmussen, et al. [135] presented recent data showing that host genetic background determines susceptibility to Ebola virus infection. Once the index person has acquired EVD from wildlife, human transmission of Ebola virus is by direct contact. Ebola virus have been detected in almost all body fluids including blood, urine, saliva, bile, bone marrow, semen and pancreatic juice with the highest presence in blood plasma and peripheral blood lymphocytes [3].
Ebola virus can therefore be transmitted among humans through contacts with excretions and fluids such as urine, blood, excreta, sweat, saliva, tears. Ebola virus could also be transmitted through casual contacts such as hand shaking, contacts with contaminated equipment, door knob even in rest rooms. Nosocomial transmission is also common [2,7,116]. Transmission of Ebola virus via the respiratory route is a possibility, but it has not been demonstrated in humans but only in NHP. But increase in air travel is a route of transmission of EVD among different countries [18,26,97].
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
The incidence of emerging disease is increasing globally [136,137]. About 1407 - 1415 human pathogens have been identified with 58 - 75% of them of zoonotic origin out of which 177 are considered as emerging or re-emerging [138-141]. Jones, et al. [136] reported that 60.3% of emerging infectious diseases event are zoonotic out of which 71.8% originate from wildlife. The risks of zoonotic infections are higher at lower latitudes i.e. nearer the equator in area characterized by poor reporting [136,140]. Engering, et al. [142] categorized and described infections disease emergence event into 3 groups (1) pathogens showing up in a novel host including zoonosis, (2) mutant pathogens displaying novel trait in the same host including increased virulence, antibiotic resistance and host immune escape, and (3) disease complex emerging in a geographical area, either through range expansion or long distance jumps. Ebola virus appear to fall within the three categories, being zoonotic, possibly carried by migratory bats to new location (from Central Africa to West Africa) and has ability to evade the human immune system.
Bats are the natural host of a number of high impact viral zoonosis [90]. Many emerging pathogens are more likely to be viruses those other pathogens types [140]. Viruses that originate from bats are the most notorious emerging zoonosis that spill from wildlife through domestic and other animals to humans [107]. More zoonotic viruses are hosted by bats, whose distribution overlap with a good number of other species [90]. Due to their broad host ranges, viruses particularly RNA viruses are most likely to emerge [89,138,141]. Moreover, the ability of the pathogen to infect multiple hosts, particularly in other taxonomic groups of wildlife is risk factors for emergence in humans [141]. Ebolavirus like most other emerging pathogens can be transmitted through diverse pathways among humans and animals such as physical contact with infected organisms and materials (food, body fluid and contaminated objects), sexual intercourse, and via vectors such as bats and possibly insects and rodents [90,137,139]. Engering, et al. [142] presented a conceptual framework based on changes in the interplay of pathogens, host and environmental factors that lead to the formation of novel disease patterns and pathogen genetic adjustment. The emergence of zoonosis appears to be driven by socio-economic, environmental and ecological factors [136]. Jones, et al. [140] linked the emergence of zoonosis to agricultural intensification and environmental change. Ng, et al. [97] analyzed EVD outbreaks from 1976 - 2014 and found a relationship between the disease and climatic parameters such as temperature, humidity and rainfall. Many authors have also observed season changes that appear to trigger EVD [18,46,143]. In a given landscape, local and regional weather patterns acts as strong determinants of vegetation, soil and water characteristics. The nature and distribution of these resources can influence animal behavior, migration pattern, population and species distribution [18,144]. Richter and Cummings [98] reported that seasonally large bat population of 5 - 10 million congregate at the Kasanka National Park, Zambia in response to the seasonal changes in rainfall, which affect the availability of fruits. Availability of fruits will also attract other animals and humans, which could increase contact and transmission of diseases. Besides, humans increasingly hunt bats and other wildlife during fruiting periods.
Bat behaviors that could be possibly associated with Ebola virus transmission including fighting and mating occur more frequently during the rainy season [18,83,97]. Olival and Hayman [83] reported that the prevalence of many other batborne viruses such as rabies and coronaviruses show seasonal dynamics. Pinzon, et al. [145] associated EVD outbreaks with sharply drier conditions following the rainy season. Polonsky, et al. [146] reported that the increased frequency of Ebola and Marburg virus outbreaks in Uganda is caused by a combination of factors such as increased contacts between humans and bats, fluctuation in viral load and prevalence within bat and other factors such as improved surveillance and laboratory capacity. Peterson, et al. [147] used geographical features to predict outbreaks of MARV. Walsh and Haseeb [144] described the spatial relationship between zoonotic EVD transmission events/ spillovers and population density and vegetation over. Alexander, et al. [18] reported seasonal factors, which may increase forage and wildlife distribution could potentially increase their contacts with bats. Due to the combined effects of urbanization, population increase and agricultural intensification particularly in Africa, humans have encroached into the rainforest and altering the ecosystem. Changes in land use pattern and penetration into previously inaccessible areas of rainforest might have brought humans into contact with new disease reservoir [148-151]. The Guinean and Congolean forests are largely deforested due to socioeconomics conditions that linked bats to the intermediate hosts. Other drivers (human activities) include urbanization, ecotourism, cultural practices, trade and international travel. Plowright, et al. [107] described a series of connected enabling conditions necessary for spillover of emerging bat viruses to include; infection and distribution of reservoir host, pathogen shedding/survival outside the host, and spillover to susceptible host. Pigott, et al. [26] used vegetation, elevation, temperature, evapotranspiration and bat distribution to map the zoonotic niche of EVD in Africa and found 22 million people at risk in 22 countries across Central and West Africa including Nigeria, Cameroun, CAR, Ghana, Liberia, Sierra Leone, Angola, Tanzania, Togo, Ethiopia, Mozambique, Burundi, Equatorial Guinea, Madagascar and Malawi.
logging and clearing and burning for agriculture [15,140]. Some bats species are well adapted to these disturbed ecosystems [67,136]. Smith & Wang [89] discussed the drivers of zoonotic virus spill over from bats to include extrinsic factors (drought, habitat loss, bush fire, cave destruction) and intrinsic factor (age, progeny and nutritional status of bats), agricultural practices and socioeconomics conditions that linked bats to the intermediate hosts. Other drivers (human activities) include urbanization, ecotourism, cultural practices, trade and international travel. Plowright, et al. [107] described a series of connected enabling conditions necessary for spillover of emerging bat viruses to include; infection and distribution of reservoir host, pathogen shedding/survival outside the host, and spillover to susceptible host. Pigott, et al. [26] used vegetation, elevation, temperature, evapotranspiration and bat distribution to map the zoonotic niche of EVD in Africa and found 22 million people at risk in 22 countries across Central and West Africa including Nigeria, Cameroun, CAR, Ghana, Liberia, Sierra Leone, Angola, Tanzania, Togo, Ethiopia, Mozambique, Burundi, Equatorial Guinea, Madagascar and Malawi.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Future Research Directions
From the literature, it appears that Ebola virus that was restricted to the Congolean forest in Central Africa has spread to other regions on the continent in West and Southern Africa due possibly to the activities of migratory bats. About 22 million people in 22 countries across Africa are now potentially at risk of infection by Ebola. The bats could transmit the virus to other wildlife unnoticed, from where the virus could amplify and cause outbreaks in wildlife and spill over to humans sporadically. Research into ecological and other important aspects of viral transmission should therefore focus on the following research areas.
- Monitor and track the migration of bats.
- Monitor intermediate hosts particularly great apes and duikers
- Monitor other animals including birds, reptiles, rodents, NHP and invertebrates for the prevalence of Ebola virus
- Monitor domestic animals such as dogs, pigs, cattle, goat, for Ebola virus Ig.
- Develop disseminating vaccines such as recombinant Rabies-Ebola vaccine that could be used to stop the spread of Ebola among wildlife.
- Carry out continuous monitoring in the 22 countries at risk of Ebola virus emergence.
- Develop vaccines and therapeutics for response against future EVD outbreaks
- Frequently carry out routine molecular, virological and serological studies, of all organisms in the EVD outbreak chain.
- There is need to understand the route and seasonality of viral shedding in bats.
- The possibility of boosting bat immune system to suppress the replication of ebolavirus could be explored.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Conclusion
Ebolavirus emerged for the first time in West Africa causing large fatalities in Guinea, Liberia and Sierra Leone with minor cases in Nigeria, Senegal and Mali and few imported cases into US and Spain. Because of the devastating effect of the 2014/2015 West Africa EVD, attracted several research attentions, but thus far no approved vaccine or therapeutics for the disease. The epidemic has ended. But outbreaks could occur in the future because the virus is still circulating in African tropical forests, hence the need for vigilance. It may be difficult to stop the virus in the wild, but the transmission to intermediate host could be mitigated by the use of replicating vaccines. Human drivers of forest degradation could be reduced and bush meat consumption could be stopped.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Acknowledgement
The author wishes to thank Sylvester C. Izah of the Niger Delta University for the editorial work and Dr. Beth Middleton of USGS for proofreading the manuscript. The author wishes to dedicate this manuscript to all the field staff of international NGOs (listed here: http://www.cidi.org/ebola-ngos/#.VPTjsC5vTFU assessed 2 March 2015) who risked their lives while combating Ebola virus disease in West Africa, funding agencies (Bill and Melinda Gates Foundation, Facebook, Aliko Dangote Foundation, Tony Elumelu Foundation), United Nations and some her agencies such as WHO and UNICEF, banking institutions (AfDB, World Bank) and the government of nations that responded to the Ebola Crisis and c countries that funded research for the development of drugs and vaccines (USA, Canada, Japan, China, Cuba, UK, Spain).
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
Compliance with Ethical Standards:
a. Funding: This study received no external funding as it was solely funded by the author
b. Ethical approval: This article does not contain any studies with human participants or animals performed by author.
- Research Article
- Abstract
- Introduction
- Ecology of Ebolavirus
- Ebola and other Filoviruses
- Bats (Suspected Reservoir of Ebolavirus)
- Intermediate/ Secondary Host of Ebola Virus
- Dead End Host (Humans)
- Climatic and Anthropogenic Factors Possibly Triggering Ebolavirus Emergence and Re-Emergence
- Future Research Directions
- Conclusion
- Acknowledgement
- Compliance with Ethical Standards
- References
References
- Kawaoka Y (2005) How ebola virus infects cells. The New Eng J Med 352(25): 2645-2546.
- Ohimain EI (2015) How the spread of Ebola virus was curtailed in Nigeria. Inter J Med Pharm Case Reports 4 (1): 11-20.
- Narayanan R (2014) Ebola-associated genes in the human genome: implications for novel targets. MOJ Proteomics Bioinf 1(5): 00032.
- Bente D, Gren J, Strong JF, Feldmann H (2009) Disease modeling for Ebola and Marburg viruses. Dis Models Mech 2(1-2): 12-17.
- Feldmann H, Geisbert TW (2011) Ebola haemorrhagic fever. The Lancet 377(9768): 849-862.
- Bray M (2003) Defense against filoviruses used as biological weapons. Antiviral Res 57(1-2): 53-60.
- Martina BE, Osterhaus AD (2009) Filoviruses: a real pandemic threat? EMBO Molecular Med 1(1): 10-18.
- Peters CJ, LeDuc JW (1999) An introduction to Ebola: the virus and the disease. The J Infect Dis 179 (Suppl 1) 9-16.
- Chippaux JP (2014) Outbreaks of Ebola virus disease in Africa: the beginnings of a tragic saga. J Venom Anim Toxins Incl Trop Dis 20(1): 44.
- Marston HD, Folkers GF, Morens DM, Fauci AS (2014) Emerging viral diseases: confronting threats with new technologies. Sci Transl Med 6(253): 1-6.
- Peters CJ, Sanchez A, Feldmann H, Rollin PE, Nichol S, et al. (1994) Filoviruses as emerging pathogens. Seminar in Virology 5(2): 147- 154.
- Rouquet P, Froment JM, Bermejo M, Kilbourn A, Karesh W, et al. (2005) Wild animals mortality monitoring and human Ebola outbreaks, Gabon and Republic of Congo, 2001-2003. Emerg Infect Dis 11(2): 283-290.
- Nkoghe D, Padilla C, Becquart P, Wauquier N, Moussavou G, et al. (2011) Risk factors of Zaire ebolavirus-specific IgG in rural Gabonese populations. J Infect Dis 204(Suppl 3): S768-S775.
- Maganga GD, Bourgarel M, Ella GE, Drexler JF, Gonzalez JP, et al. (2011) Is Marburg virus enzootic in Gabon? J Infect Dis 204(Suppl 3): S800-S803.
- Bausch DG, Schwarz L (2014) Outbreak of Ebola virus disease in Guinea: where ecology meets economy. Plos Negl Trop Dis 8(7): e3056.
- Hoenen T, Feldmann H (2014) Ebolavirus in West Africa, and the use of experimental therapies or vaccines. BMC Biology 12: 80.
- Goeijenbier M, van Kampen JJA, Reusken CBEM, Koopmans MPG, van Gorp EC (2014) Ebola virus disease: a review on epidemiology, symptoms, treatment and pathogenesis. The J Med 72(9): 442-448.
- Alexander KA, Sanderson CE, Marathe M, Lewis BL, Rivers CM, et al. (2014) What factors might have led to the emergence of Ebola in West Africa. PLOS Negl Trop Dis In press 9(6): e0003652.
- Baize S, Pannetier D, Oestereich L, Rieger T, Koivogui L, et al. (2014) Emergence of Zaire Ebola virus Disease in Guinea. N Engl J Med 371(15): 1418-1425.
- http://resiliencesystem.com/ebola-graphics-toll-tragedy-1
- WHO (2015) Ebola situation report 19 August 2015. World Health Organization, Rome, Italy.
- Brauburger K, Hume AJ, Muhlberger E, Olejnik J (2012) Forty-five years of Marburg virus research. Viruses 4(10): 1878-1927.
- Simons RRL, Gale P, Horigan V, Snary EL, Breed AC (2014) Potential for introduction of bat-borne zoonotic viruses into the EU: A review. Viruses 6(5): 2084-2121.
- Feldmann H (2014) Ebola-a growing threat? N Engl J Med 371(15):1375-1378.
- Briand S, Bertherat E, Cox P, Formenty P, Kieny MP, et al. (2014) The international Ebola emergency. N Engl J Med 371(13): 1180-1183.
- Pigott DM, Golding N, Mylne A, Huang Z, Henry AJ, et al. (2014) Mapping the zoonotic niche of Ebola virus disease in Africa. Elife 3: e04395.
- Wittmann TJ, Biek R, Hassanin A, Rouquent P, Reed P, et al. (2007) Isolates of Zaire Ebolavirus from wild apes reveal genetic lineage and recombinants. Proc National Acad Sci United States Amer 104(43): 17123-17127.
- Yuan J, Zhang Y, Li J, Zhang Y, Wang LF, et al. (2012) Serological evidence of Ebolavirus infection in bats, China. Virol J 9: 236.
- Olival KJ, Islam A, Yu M, Anthony SJ, Epstein JH, et al. (2013) Ebola virus antibodies in fruit bats, Bangladesh. Emerg Infect Dis 19(2): 270-273.
- Negredo A, Palacios G, Vázquez-Morón S, González F, Dopazo H, et al. (2011) Discovery of an Ebolavirus-Like Filovirus in Europe. PLoS Pathog 7(10): e1002304.
- Nidom CA, Nakayama E, Nidom RV, Alamudi MY, Daulay S, et al. (2012) Serological evidence of Ebola virus infection in Indonesia orangutans. Plos One 7(7): e40740.
- Chertow DS, Kleine C, Edwards JK, Scaini R, Giuliani R, et al. (2014) Ebola virus disease in West Africa-clinical manifestations and management. The New Engl J Medicine 371(22): 2054-2057.
- Sullivan N, Yang Z-Y, Nabel GJ (2003) Ebola virus pathogensis: implications for vaccines and therapies. J Virol 77 (18): 9733-9737.
- Ohimain EI (2015) Promising therapeutics against Ebola virus disease. Inter J Trop Dis Health 10(4): 1-17.
- Ohimain EI (2015) Recent advances in the development of vaccines for Ebola virus disease. Virus Res 211: 174-85.
- Geisbert TW (2003) Towards a vaccine against Ebola virus. Expert Rev Vaccines 2(6): 777-789.
- Gonzalez JP, Herbreteau V, Morvan J, Leroy EM (2005) Ebola virus circulation in Africa: a balance between clinical expression and epidemiological silence. Bull Soc Pathol Exot 98(3): 210-217.
- Peterson AT, Holder MT (2012) Phylogentic assessment of filoviruses: how many lineage of Marburg virus? Ecol Evol 2(8): 1826-1833.
- Carroll SA, Towner JS, Sealy TK, McMullan LK, Khristova ML, et al. (2013) Molecular evolution of viruses of the family filoviridae based on 97 whole-genome sequences. J Virol 87(5): 2608-2616.
- Lukashevich IS, Shirwan H (2014) Novel Technologies for Vaccine Development. Springer-Verlag Wien, pp. 33-59.
- Hoenen T, Groseh A, Feldmann H (2012) Current Ebola vaccines. Expert Pin Biol Ther 12(7): 859-872.
- Bukreyev AA, Chandran K, Dolnik O, Dye JM, Ebihara H, et al. (2014) Discussions and decisions of the 2012-2014 International Committee on Taxonomy of Viruses (ICTV) Filoviridae Study Group, January 2012-June 2013. Arch Virol 159(4): 821-830.
- Falzarano D, Geisbert TW, Feldmann H (2011) Progress in filovirus vaccine development: evaluating the potential for clinical use. Expert Rev Vaccines 10(1): 63-77.
- WHO (2014) Ebola virus disease. World Health organization, Geneva, Switzerland.
- Gire SK, Goba A, Andersen KG, Sealfon RSG, Park DJ, et al. (2014) Genomic surveillance slucidates Ebola virus origin and transmission during the 2014 outbreak. Science 345(6202): 1369-1372.
- Walsh PD, Biek R, Real LA (2005) Wave-like spread of Ebola zaire. PLOS Biology 3(11): e371.
- Hoenen T, Safonetz D, Groseth A, Wollenberg KR, Koita OA, et al. (2015) Virology. Mutation rate and genotype variation of Ebola virus from Mali case sequences. Science 348(6230): 117-119.
- Rao M, Bray M, Alving CR, Jahrling P, Matyas GR, et al. (2002) Induction of immune responses in mice and mokeys to Ebola virus after immunization with liposome-encapsulated irradiated Ebola virus: protection in mice requires CD4+ T cells. J Virol 76(18): 9176- 9185.
- Kondratowicz AS, Maury WJ (2012) Ebola virus: a brief review of novel therapeutic targets. Future Microbiol 7(1): 1-4.
- Enterlein S, Warfield KL, Swenson DL, Stein DA, Smith JL, et al. (2006) VP 35 knockdown inhibits Ebola virus amplification and protects against lethal infection in mice. Antimicrobial Agent Chemotherapy 50(3): 984-993.
- Sobarzo A, Perelman E, Groseth A, Dolnik O, Becker S, et al. (2012) Profiling the native specific human humoral immune response to Sudan Ebola virus strain gulu by chemiluminescence enzyme-linked immunosorbent assay. Clin Vac Immunol 19(11): 1844-1852.
- Geisbert TW, Lee ACH, Robbins M, Joan B Geisbert, Honko AN, et al. (2010) Postexposure protection of non-human primates against a lethal Ebola virus challenge with RNA interference: a proof-of -concept study. The Lancet 375(9729): 1896-1905.
- Watanabe S, Noda T, Halfmann P, Jasenosky L, Kawaoka Y (2007) Ebola virus (EBOV) VP24 inhibits transcription and replication of the EBOV genome. J Infect Dis 196(Suppl 2): S284-S290.
- Leung DW, Prins KC, Basler CF, Amarasinghe GK (2010) Ebolavirus VP35 is a multifunctional virulence factor. Virulence 1(6): 526-531.
- Trunschke M, Conrad D, Enterlein S, Olejnik J, Brauburger K, et al. (2013) The L-VP35 and L-L interaction domains reside in the amino terminus of the Ebola virus L protein and are potential targets for antivirals. Virology 441(2): 135-145.
- Basler CF, Amarasinghe GK (2009) Evasion of interferon responses by Ebola and Marburg viruses. J Interferon Cytokine Res 29(9): 511- 520.
- Murugan NJ, Karbowshi LM, Persinger MA (2015) Cosi’s resonance recognition model for protein sequences and photon emission differentiates lethal and non-lethal Ebola strains: implications for treatment. OJBIPHY 5(1): 35-43.
- Wilson JA, Bray M, Barkken R, Hart MK (2001) Vaccine potential of Ebola virus VP24, VP30, VP 35, and VP40 proteins. Virology 286(2): 384-390.
- Martinez O, Tantral L, Mulherkar N, Chandran K, Basler CF (2011) Impact of Ebola mucin-like domain on antiglycoprotein antibody responses induced by Ebola virus-like particles. The J Infectious Dis 204(Suppl 3): S825-S832.
- Sulkin SE, Allen R, Sims R, Taylor SK (1965). Bats in relation to arthropod-borne viruses: An experimental approach with speculations. Am J Public Nations Health 55(9): 1376-1385.
- Halpin K, Hyatt AD, Plowright RK, Epstein JH, Peter Daszak, et al. (2007) Emerging viruses: coming in on a wrinkled wing and a prayer. Clin Infectious Dis 44(5): 711-717.
- Monath TP (1999) Ecology of Marburg and Ebola viruses: Speculations and Directions for future Research. The J Infectious Dis 179(Suppl 1): S127-S138.
- Pourrut X, Delicat A, Rollin PE, Ksiazek TG, Gonzalez JP, et al. (2007) Spatial and temporal patterns of Zaire ebolavirus antibody prevalence in the possible reservoir bat species. The J Infectious Dis 196(Suppl 2): S176-183.
- Reed PE, Mulangu S, Cameron KN, Ondzie AU, Joly D, et al. (2014) A new approach for monitoring Ebolavirus in Wild great apes. Plos Negl Trop Dis 8(9): e3143.
- Leroy EM, Kumulungui B, Pourrut X, Rouquet P, Hassanin A, et al. (2005) Fruit bats as reservoirs of Ebola virus. Nature 438(7068): 575-576.
- Schountz T (2014). Immunology of bats and their viruses: challenges and opportunities. Viruses 6(12): 4880-4901.
- Moratelli R, Calisher CH (2015) Bats and zoonotic viruses: can we confidently link bats with emerging deadly viruses? Mem Inst Oswaldo Cruz 110(1): 1-22.
- Leroy EM, Epelboin A, Mondonge V, Pourrut X, Gonzalez JP, et al.(2009) Human Ebola outbreak resulting from direct exposure to fruit bats in Luebo, Democratic Republic of Congo, 2007. Vector-Borne and Zoonotic Diseases 9(6): 723-728.
- Biek R, Walsh PD, Leroy EM, Real LA (2006) Recent common ancestry of Ebola Zaire virus found in bat reservoir. Plos Pathog 2(10): 0885- 0886.
- Kuhl A, Hoffmann M, Muller MA, Munster VJ, Gnirß K, et al. (2011) Comparative analysis of Ebola virus glycoprotein interactions with human and bat cells. The J Infectious Dis 204(Suppl 3): S840-S849.
- Calisher CH, Childs JE, Field HE, Holmes KV, Schountz T, et al. (2006) Bats: important reservoir hosts of emerging viruses. Clin Microbiol Reviews 19(3): 531-545.
- Saez AM, Weiss S, Nowak K, Lapeyre V, Zimmermann F, (2015) Investigating the zoonotic origin of the west Africa Ebola epidemic. EMBO Molecular Medicine 7(1): 17-23.
- Hayman DTS, Emmerich P, Yu M, Wang LF, Suu-Ire R, et al. (2010) Long-term survival of an urban fruit bat seropositive for Ebola and Lagos bat viruses. PLOS One 5(8): eii978.
- Pourrut X, Souris M, Towner JS, Rollin PE, Stuart T Nichol, et al. (2009) Large serological survey showing cocirculation of Ebola and Marburg viruses in Gabonese bat populations, and a high seroprevalence of both viruses in Rousettus aegyptiacus. BMC Infectious Dis 9: 159.
- Amman BR, Carroll SA, Reed ZD, Sealy TK, Balinandi S, et al. (2012) Seasonal pulses of Marburg virus circulation in juvenile Rousettus aegyptiacus bats coincide with periods of increased risk of human infection. Plos Pathogens 8(10): e1002877.
- Towner JS, Pourrut X, Albarino CG, Nkogue CN, Bird BH, et al. (2007) Marburg virus infection detected in a common African bat. Plos One 2(8): e764.
- Peterson AT, Papes M, Carroll DS, Leirs H, Karl M. Johnson (2007) Mammal taxa constituting potential coevolved reservoirs of filoviruses. J Mammalogy 88(6): 1554-1554.
- Swanepoel R, Smit SB, Rollin PE, Formenty P, Leman PA, et al. (2007). Studies of reservoir hosts of Marburg virus. Emerg Infect Dis 13(12): 1847-1851.
- Hayman DTS, Yu M, Crameri G, Wang LF, Suu-Ire R, et al. (2012) Ebolavirus antibodies in Ghanaian fruit bats, West Africa. Emerg Infectious Dis 18(7): 1207-1209.
- Hayman DTS, McCrea R, Suu-Ire R, Wood JLN, Cunningham AA, et al. (2012) Demography of straw-colored fruit bats in Ghana. J Mammal 93(5): 1393-1404.
- Hayman DTS, Fooks AR, Rowcliffe JR, Restif O, Baker K, et al. (2012) Endemic Lagos bat virus infection in Straw-coloured fruit bats. Epidemiology Infection 140(12): 2163-2171.
- O’Shea TJ, Cryan PM, Cunningham AA, Fooks AR, Hayman DTS, et al. (2014) Bat flight and zoonotic viruses. Emerg Infectious Dis 20(5): 741-745.
- Olival KJ, Hayman DTS (2014) Filoviruses in bats: current knowledge and future directions. Viruses 6(4): 1759-1788.
- Swanepoel R, Leman LA, Burt FJ, Zachariades NA, Braack LE, et al. (1996) Experimental inoculation of plants and animals with Ebola virus. Emerg Infect Dis 2(4): 321-325.
- Mackenzie JS, Field HE, Guyatt KJ (2003). Managing emerging diseases borne by fruit bats(flying foxes), with particular reference to henipaviruses and Austrian bat lysaavirus. J Appl Microbiol 94(Suppl): 59S -69S.
- Shi Z (2010) Bats and virus. Protein & Cell 1(2): 109-114.
- Shi Z (2013) Emerging infectious diseases associate with bat viruses. Science China Life Science 56(8): 678-682.
- Yadav PD, Raut CG, Shete AM, Mishra AC, Towner JS, et al. (2012) Short report: detection of Nipah virus RNA in fruit bat (Pteropus giganteus) from India. The Amer Soc Trop Med Hyg 87(3): 576-578.
- Smith I, Wang LF (2013) Bats and their virome: an important source of emerging viruses capable of infecting humans. Curr Opin Virol 3(1): 84-91.
- Luis AD, Hayman D, O’Shea TJ, Cryan PM, Gilbert AT, et al. (2013) A comparison of bats and rodents as reservoirs of zoonotic viruses: are bats special? Proc Biol Sci 280(1756): 2012-2753.
- Peel AJ, Sargan DR, Baker KS, Hayman DTS, Jennifer A. Barr, et al. (2014) Continent-wide panmixia of an African fruit bat facilitates transmission of potentially zoonotic viruses. Nature Communications 4.
- Banyard AC, Evans JS, Luo TR, Fooks AR (2014) Lyssaviruses and bats: emergence and zoonotic threat. Viruses 6(4): 2974-2990.
- Poel VDWH, Lina PHC, Kramps JA (2006) Public health awareness of emerging zoonotic viruses of bats: a european perspective. Vector- Borne and Zoonotic Diseases 6(4): 315-324.
- Baker KS, Todd S, Marsh GA, Crameri G, Barr J, et al. (2013) Novel, potentially zoonotic paramyxoviruses from the African strawcoloured fruit bat Eidolon helvum. J Virol 87(3): 1348-1358.
- Rapin N, Johns K, Martin L, Warnecke L, Turner JM, et al. (2014) Activation of innate immune-response genes in little brown bats (Myotis lucifugus) infected with the fungus Pseudogymnoascus destuctans. PloS One 9(8): e112285.
- Ossa G, Kramer-Schadt S, Peel AJ, Scharf AK, Voigt CC (2012) The movement ecology of the straw-coloured fruit bat, Eidolon helvum, in sub-sahara Africa Assessed by stable isotope ratios. Plos One 7(9): e45729.
- Ng S, Cowling BJ (2014) Association between temperature, humidity and Ebolavirus disease outbreaks in Africa, 1976 to 2014. Euro Surveill 19(35): pii:20892.
- Richter HV, Cumming GS (2008) First application of satellite telemetry to track African straw-coloured fruit bat migration. J Zoology 275(2): 172-176
- Leroy EM, Telfer P, Kumulungui B, Yaba P, Rouquet P, et al. (2004) A serological survey of Ebola virus infection in Central African Nonhuman primates. J Infect Dis 190(11): 1895-1899.
- Reed PE, Mulangu S, Cameron KN, Ondzie AU, Joly D, et al. (2014) A new approach for monitoring Ebolavirus in Wild great apes. Plos Negl Trop Dis 8(9): e3143.
- Leroy EM, Rouquent P, Formenty P, Souquiere S, Kilbourne A, et al. (2004) Multiple Ebola virus transmission events and rapid decline of Central African Wildlife. Science 303(56560: 387-390.
- Allela L, Bourry O, Pouillot R, Delicat A, Yaba P, et al. (2005) Ebola Virus Antibody Prevalence in Dogs and Human Risk. Emerg Infectious Dis 11(3): 385-390.
- Kobinger GP, Leung A, Neufeld J, Richardson JS, Falzarano D, et al. (2011). Replication, pathogencity, shedding, and transmission of Zaire ebolaviruse in pigs. J Infect Dis 204(2): 200-208.
- Munshi-South J, Wilkinson GS (2009) Bats and Birds: exceptional longevity despite high metabolic rates. Ageing Res Rev 9(1): 12-19.
- Wilkinson GS, South JM (2002) Life history, ecology and longevity in bats. Ageing Cell 1(2): 124-131.
- Martino AMG, Aranguren J, Arends A (2006) New longevity records in south American microchiropterans. Mammalia 70(1-2): 166-167.
- Plowright RK, Eby P, Hudson PJ, Smith IL, Westcott D, et al. (2014) Ecological dynamics of emerging bat virus spillover. Proc Biol Sci 282(1798): 20142124.
- Breman JG, Johnson KM, Groen GVD, Robbins CB, Szczeniowski MV, et al. (1999) A search for Ebola virus in animals in the Democratic Republic of the Congo and Cameroun: Ecologic, Virologic, and serologic surveys, 1979-1980. Ebola Virus Study Teams. J Infect Dis 179(Suppl 1): S139-S147.
- Reiter P, Turrell M, Coleman R, Miller B, Maupin G, et al. (1999) Field investigations of an outbreak of Ebola hemorrhagic fever, kikwit, Democratic Republic of the Congo, 1995: arthropod studies. J Infectious Dis 179 (Suppl 1): S148-S154.
- Leirs H, Mills JN, Krebs JW, Childs JE, Dudu Akaibe, et al. (1999) Search for the Ebola virus reservoir in Kikwit, Democratic Republic of the Congo: Reflections on a vertebrate collection. J Infectious Dis 179(Suppl 1): S155-163.
- Grad G, Biek R, Tamfum JJM, Fair J, Wolfe N, et al. (2011) Emergence of divergent Zaire Ebola virus strain in Democratic Republic of Congo in 2007 and 2008. J Infect Dis 204(Suppl 3): S776-S784.
- Genton C, Cristescu R, Gatti S, Levrero F, Bigot E, et al. (2012) Recovery potential of western lowland Gorilla population following a major Ebola outbreak: Results from a ten year study. Plos One 7(5): e37106.
- Bermejo M, Rodriguez-Teijeiro JD, Illera G, Barroso A, Vilà C, et al. (2006) Ebola outbreak killed 5000 gorillas. Science 314(5805): 1564.
- Iqbal W, Malik FM, Sarwar MK, Azam I, Nadia Iram, et al. (2014) Role of housefly (Musa domestica, Diptera; Muscidae) as a disease vector; a review. J Entomol Zool Studies 2(2): 159-163.
- Barreiro C, Albano H, Silva J, Teixeira P (2013) Role of flies as vectors of foodborne pathogens in rural areas. ISRN Microbiol 2013(2013): 7.
- Fisher-Hoch SP (2005) Lessons from nosocomial viral haemorrhagic fever outbreaks. British Med Bull 75-37: 123-137.
- Schurrer JA, Dee SA, Moon RD, Rossow KD, Mahlum C, et al. (2004) Spatial dispersal of porcine reproductive and respiratory syndrome virus-contaminated flies after contact with experimentally infected pigs. Am J Vet Res 65(9): 1284-1292.
- Wong G, Qiu X, Richardson JS, Cutts T, Collignon B, et al. (2015) Ebola virus transmission in guinea pigs. Virology 89(2): 1314-1323.
- Katzourakis A, Gifford RJ (2010) Endogenous viral elements in animal genomes. PLoS Genet 6 (11): e1001191.
- Chivers DJ, Hladik CM (1980) Morphology of the gastrointestinal tract in primates: Comparisons with other mammals in relation to diet. J Morphol 166(3): 337-386.
- Bray M, Murphy FA (2007) Filovirus research: knowledge expands to meet a growing threat. J Infect Dis 196(Suppl 2): S438-443.
- Kamins AO, Restif O, Ntiamoa-BaiduY, Suu-Iru R, Hayman DTS, et al. (2011) Uncovering the fruit bat bushment commodity chain and the true extent of fruit bat hunting in Ghana, West Africa. Biolog Conservation 144(12): 3000-3008.
- Kamins AO, Rowcliffe JM, Ntiamoa-Baidu Y, Cunningham AA, Wood JL, et al. (2015) Charcateristics and risk perceptions of Ghanaian potentially exposed to bat-borne zoonoses through bushmeat. EcoHealth 12(1): 104-120.
- Hamadina MK, Otobotekere D, Anyanwu DI (2007) Impact assessment and biodiversity considerations in Nigeria: a case study of Niger Delta University campus project on wildlife in Nun River forest reserve. Manage Environ Quality: An Intern J 18(2): 179-197.
- Martin GHG (1983) Bushmeat in Nigeria as a Natural Resource with Environmental Implications. Environ Conservation 10(2): 125-132.
- Fa JE, Seymour S, Dupain J, Amin R, Albrechtsen L, et al. (2006) Getting a grips with the magnitude of exploitation: bushmeat in the cross-sanaga Rivers, Nigeria and Cameroun. Biolog Conservation 129(4): 497-510.
- Subramanian M (2012) Zoonotic disease risk and the bushmeat trade: assessing awareness among hunters and traders in Sierra Leone. EcoHealth 9(4): 471-482.
- African Center for Economic Transformation (ACET) (2014) Bushmeat and the future of protein in West Africa. West Africa Trends Newsletter 9: 1-13.
- Swensson J (2005) Bushmeat trade in Techiman, Ghana, West Africa. Committee of tropical ecology Uppsala University, Sweden. Minor field Study 110.
- Gonzalez JP, Joss R, Johnson ED, Merlin M, Georges AJ, et al. (1989) Antibody prevalence against haemorrhagic fever viruses in randomized representative Central African populations. Res Virol 140(4): 319-331.
- Gonzalez JP, Nakoune E, Slenczka E, Vidal P, Morvan JM (2000) Ebola and Marburg virus antibody prevalence in selected populations of the Central African Republic. Microbes Infect 2(1): 39-44.
- Johnson ED, Gonzalez JP, Georges A (1993) Haemorrhagic fever virus activity in equatorial Africa: distribution and prevalence of filovirus reactive antibody in the Central African Republic. Trans Royal Soc Trop Med Hyg 87(5): 530-535.
- Heffernan RT, Pambo B, Htacett RJ, Leman PA, Swanepoel R, et al. (2005) Low seropositive of IgG antibodies to Ebola virus in an epidemic zone: Ogooue-Ivindo region, northeastern Gabon, 1997. J Infect Dis 191(6): 964-968.
- Pernet O, Schneider BS, Beaty SM, LeBreton M, Yun TE, et al. (2014) Evidence for henipavirus spillover into human population in Africa. Nat Commun 5: 5342.
- Rasmussen AL, Okumura A, Ferris MT, Green R, Friederike Feldmann, et al. (2014) Host genetic diversity enables Ebola hemorrhagic fever pathogenesis and resistance. Science 346(6212): 987-991.
- Jones KE, Patel NG, Levy MA, Storeygard A, Deborah Balk, et al. (2008) Global trends in emerging infectious diseases. Nature 451: 990-993.
- Butler CD (2012) Infectious disease emergence and global change: thinking systemically in a shrinking world. Infectious Dis Poverty 1: 5.
- Woolhouse ME J, Gowtage-Sequeria S (2005) Host range and emerging and reemerging pathogens. Emerg Infectious Dis 11 (12): 1842-1847.
- Obi RK, Orji NM, Nwanebu FC, Okangba CC (2010) Emerging and re-emerging infectious diseases: the perpertual menace. Asian J Experimental Sci 1(2): 271 - 282.
- Jones BA, Grace D, Kock R, Alonso S, Rushton J, et al. (2013) Zoonosis emergence linked to agricultural intensification and environmental change. Proc Natl Acad Sci 110(21): 8399-8404.
- Cleaveland S, Laureson MK, Taylor LH (2001) Diseases of humans and their domestic mammals: pathogens characteristics, host range and the risk of emergence. Phil Philos Trans R Soc Lond B Biol Sci 356(1411): 991-999.
- Engering A, Hogerwerf L, Slingenbergh J (2013). Pathogen-hostenvironment interplay and disease emergence. Emerging Microbes Infections 2: e5.
- Muyembe-Tamfum JJ, Mulangu S, Masumu J, Kayembe JM, Kemp A, et al. (2012) Ebola virus outbreak in Africa: past and present. Onderstepoort J Veter Res 79(2): 451.
- PWalsh MG, Haseeb MA (2015) The landscape configuration of zoonotic transmission of Ebola virus disease in West and Central Africa: interaction between population density and vegetation cover. Peer J 3: e735.
- Pinzon JE, Wilson JM, Tuncker CJ, Arthur R, Jahrling PB, et al. (2004) Trigger events: enviroclimatic coupling of Ebola hemorrhagic fever outbreaks. The Am J Trop Med Hyg 71(5): 664-674.
- Polonsky JA, Wamala JF, de Clerck H, Van Herp M, Sprecher A, et al. (2014) Emerging filovirus disease in Uganda: proposed explanations and research directions. The Amer Soc Trop Med Hyg 90(5): 790- 793.
- Peterson AT, Ryan Lash R, Carroll DS, Johnson KM (2006) Geographic potential for outbreaks of Marburg hemorrhagic fever. Am J Trop Med Hyg 75(1): 9-15.
- Mate SE, Kugelman RJ, Nyenswah TG, Ladner JT, Wiley MR, et al. (2015) Molecular Evidence of Sexual Transmission of Ebola Virus. N Engl J Med 373(25): 2448-2454.
- Taylor DJ, Ballinger MJ, ZhanJJ, Hanzly LE, Bruenn JA (2014) Evidence that ebolaviruses and cuevaviruses have been diverging from marburgviruses since the Miocene. PeerJ 2: e556.
- Taylor DJ, Dittmar K , Ballinger MJ, Bruenn JA (2011) Evolutionary maintenance of filovirus-like genes in bat genomes. BMC Evol Biol 11: 336.
- Taylor DJ, Leach RW, Bruenn J (2010) Filoviruses are ancient and integrated into mammalian genomes. BMC Evol Biol 10: 193.






























